New allergy treatments
Allergies may feel like an old curse, especially when they come back season after season, but people with allergies have more options than ever to help clear up their symptoms, says Murray Grossan, MD, an ear, nose, and throat doctor in Los Angeles and author of The Whole Body Approach to Allergy and Sinus Relief. You’re not limited to the two over-the-counter pills that are widely available, in fact you have many options besides medications, he says.
“There are so many different allergy treatments with new ones coming out all the time. There are different classes of medications, types within each class, and ways to take them like pills, capsules, nasal sprays, liquids and even injections,” says Jennifer Caudle, DO, a board-certified family medicine physician and associate professor at Rowan University. “This is great but it can feel overwhelming trying to figure out what will work best for your particular allergies and symptoms which is why it’s so important to talk to your doctor.” Check out the 7 best allergy nasal sprays that doctors recommend.

The importance of prevention
“Prevention is everything when it comes to allergies,” Dr. Caudle says. “Medication and other medical treatments can help but they’ll work so much better if you take some steps to help yourself.” One of the best ways to prevent allergies before they start is to figure out your allergy triggers—through testing or trial and error—and set up your environment to minimize them. For instance, she suggests that people who are allergic to pollen should check the National Allergy Map each morning to see the pollen count in their area and make plans accordingly. “Limit activities that put you in contact with your allergen,” she says, adding that it may sound simple but many people suffer more because they don’t plan ahead. Here’s how to allergy-proof your home this season.

Keep your windows closed
One of the best things you can do to stop allergies before they start is to keep your doors and windows closed, especially when you’re sleeping, Dr. Caudle says. “Closing doors and windows in the car and home can limit pollen exposure and reduce the severity of your response,” she says. (Here’s what else doctors do to allergy-proof their homes.)

Up your laundry game
Your clothing can be a major source of irritating pollen and mold spores, Dr. Grossan says. It’s crucial to get them off your clothes so you don’t contaminate your house. Start by removing your outer clothing outside and vigorously shaking it out. Then launder your clothing with an anti-allergy, hypoallergenic detergent, followed a hot trip through the dryer. Avoid the temptation to let clothing, towels, or bedding air-dry outside; while you get points for eco-friendliness, this makes them pollen magnets.

Allergy-proof your room
You spend a lot of time in your living spaces, like your bedroom and TV room, so it makes sense to minimize allergens in those areas, Dr. Caudle says. She recommends using a mite-proof mattress cover and anti-allergenic bedding in addition to regular laundering. A HEPA air filter can also go a long way in detoxing your air and reducing your symptoms.

Check your fruit bowl
Oral allergy syndrome (OAS) is where airborne allergens may sensitize you to those in food and affects 50 to 75 percent of seasonal allergy sufferers, says Dr. Grossan. For example, the proteins in certain fruits such as peaches and apples are similar to the proteins from birch tree pollen so you may have a reaction to both the tree pollen and eating raw peaches and apples, although the symptoms differ. Those with OAS may experience a tingling or itchy throat, or swollen lips.

Try a nasal steroid spray
If you’ve done everything you can and you’re still stuck with itching, wheezing, coughing, watery eyes or a runny nose, try a steroid spray, Dr. Caudle says. In 2017 guidelines, the Joint Task Force (a coalition from the American Academy of Allergy, Asthma & Immunology and the American College of Allergy, Asthma, and Immunology) recommends that people start with a nasal steroid spray because it’s best for quelling symptoms. However, if your symptoms don’t respond, check out the options below—and chat with your doctor—to come up with the best allergy-fighting cocktail for you.

Try a dry spray
If you can’t tolerate traditional liquid nasal sprays, chat with your doctor about the dry aerosol nasal steroid spray Qnasl, says Derrick Ward, MD, of Kansas City Allergy & Asthma Associates. This prescription med targets seasonal and year-round allergies when used once daily. One hitch, Dr. Ward points out, is that many insurance companies require patients to try over-the-counter meds first; it can be a challenge to get a Qnasl prescription covered. Still, if you’re avoiding using liquid sprays because of the comfort factor, talk to your doctor about this option.

Check out newer medications
Though the FDA approved the indoor-outdoor allergy treating medication Xyzal in 2007, it’s only been available without a prescription since fall of 2017. The oral antihistamine is designed to provide 24-hour coverage for symptoms such as a runny nose, sneezing, itchy watery eyes, and nose or throat itching seasonally or year-round. “Xyzal is the first drug I recommend to my patients because it is over-the-counter and is a powerful, all-night and all-day allergy relief that is just as effective at hour 24 as it is at hour one,” Dr. Caudle says.

Take meds in advance
Don’t wait until you’re sneezing up a storm to take allergy medication. New York City allergist and immunologist Clifford Bassett, MD, author of The New Allergy Solution, recommends beginning allergy medication up to two weeks prior to the season kicking in. He puts his patients on allergy alert; your doctor can inform you more specifically about when you should start. (Try these tricks to keep your summer sneeze-free.)

Consider immunotherapy
Allergy shots have been around for a century and can work well for many types of allergens (some better than others). However, allergists can now offer sublingual therapy: You place a tablet under your tongue daily that contains small amounts of the allergen. It builds tolerance so that your body no longer reacts to it. You can get sublingual pills for both ragweed and grass pollen allergies, and there’s a relatively new sublingual treatment for dust mites called Odactra. (It was approved by the Food and Drug Administration (FDA) in 2017.) “This is nice for patients who don’t want to do allergy shots or don’t have time to come in and get them,” says Dr. Ward. For grass and ragweed allergies, you’ll need to start treatment three to four months prior to the onset of the season, so plan ahead.

Ask your doctor about drops
Some doctors are using sublingual drops (they contain the same active ingredients as allergy shots) for allergy immunotherapy, explains Dr. Ward. The drops allow docs to treat a broader range of allergies than they could with the sublingual pills, he says, but the treatment is off-label—it hasn’t yet been approved by the FDA. If you want to try this approach, you’ll need to see an ear, nose, and throat specialist or your general practitioner; also note that insurance is unlikely to cover the cost. (Here are 17 ways to help keep allergies from ruining your life.)

Think about alternative treatments
There are some natural therapies out there that may help you get relief from symptoms, though even the promising ones have very little data to back their use. One treatment you may want to try is acupuncture: A trial found a small improvement in the quality of life for seasonal sufferers, says Dr. Bassett. He also recommends eating more quercetin-rich foods (like apples, onions), an antioxidant that “studies show may provide a small benefit to eye and nasal symptoms,” he says. Another natural approach Dr. Bassett suggests is applying a petrolatum-based ointment (like Vaseline) near your nostrils a few times a day to block pollen from entering your nose. (Here are some more alternative allergy remedies.)
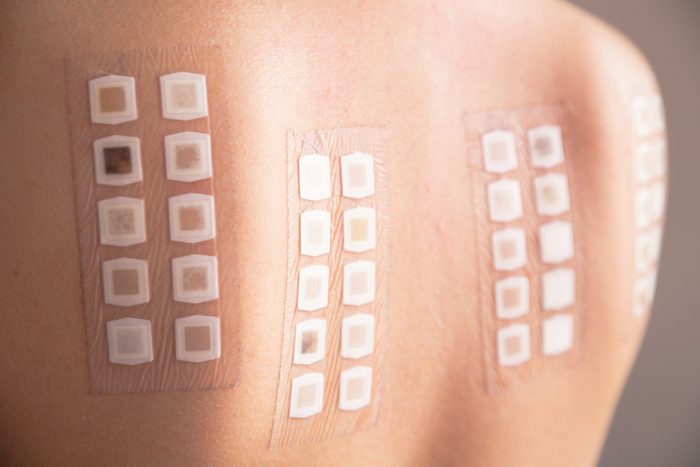
Get allergy tested
You may know you’re allergic to something—but not know exactly what. Is it pollen? Grass? Mold? Dust mites? That’s why getting tested to pinpoint exactly what’s bothering you is so important, says Dr. Ward. With that info, you can tailor your treatments to deal with the exact culprit, which is far more effective than guessing. Skip the at-home tests though as they are not accurate or reliable.
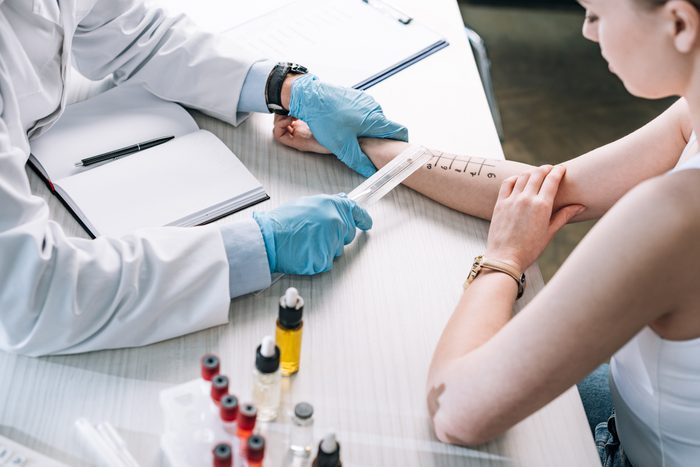
The need for testing, part two
Even with the advancements in sublingual therapy, it doesn’t guarantee you can go shot-free. The other benefit of allergy testing is that it will help you choose between sublingual therapy and allergy shots. “If I test someone and they’re allergic to multiple things, giving them a tablet for ragweed isn’t really beneficial. But if they also have allergies to animals or dust mites, that’s where allergy shots shine—I can put all of that in a shot,” says Dr. Ward.
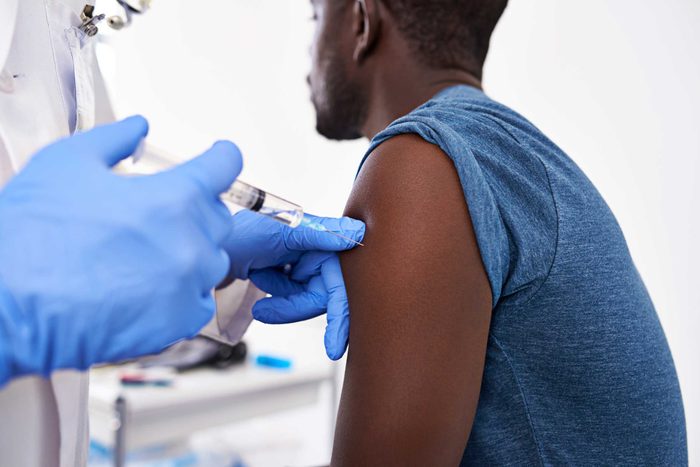
Personalized treatment approach
Sometimes, it can feel as if you’re throwing everything you have at those spring allergies and getting nowhere. That’s why an allergist’s personalized treatment approach can be a game-changer: “There are many, many strategies that are helpful, cost-effective, and will get the job done. It takes an extra few minutes to see an allergist who can create an individualized pollen calendar for you, which you can use to reduce and prevent symptoms,” says Dr. Bassett. Ask your doctor how you can best prepare for the season ahead. Next, check out the surprising triggers of spring allergy symptoms that aren’t pollen.
