When your body begins ignoring signals from the hormone insulin to process the glucose in your blood, you have insulin resistance. This can result in blood sugar (glucose) levels that are too high, and over time, can lead to prediabetes (and eventually type 2 diabetes). Insulin resistance can also increase your risk of heart disease and other conditions, which is why doctors recommend you catch it—and treat it—as soon as possible.
Keep in mind that the most common symptom of insulin resistance is no symptom at all. You can develop it without any obvious outward signs. That said, here are eight potential signs of insulin resistance.

Abdominal obesity
Obesity, especially too much fat in the abdomen and around the organs is one of the main causes of insulin resistance, according to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). Here’s why: “Abdominal fat, or fat around your waistline, has a more negative effect on your metabolism than fat that accumulates in other areas of the body,” says Kellie Rodriguez, a registered nurse, a certified diabetes educator and director of the Global Diabetes Program at Parkland Health & Hospital System in Dallas. “Abdominal fat increases your risk for type 2 diabetes, insulin resistance, and heart disease. Therefore measuring your waistline is important–with a goal of fewer than 35 inches for women and 40 inches for men.”
For people at high risk for type 2 diabetes, losing just five to seven percent of your starting weight can help reduce your chance of developing the condition. (Avoid these worst habits for belly fat.)

Elevated blood sugar
Elevated blood sugar level is a key sign of insulin resistance. High blood sugar—hyperglycemia—can translate to excessive thirst, lethargy, frequent urination, and more serious symptoms if left unchecked, according to the American Diabetes Association. Blood sugar is considered too high if it’s more than 180 mg/dL or any reading above your target range; a blood sugar reading of 300 mg/dL or more can be dangerous, according to Michigan Medicine. If your blood sugar is elevated, you won’t necessarily know it. (Only at higher levels will it cause obvious symptoms.) A blood test at the doctor’s office can determine if your blood sugar is elevated.
People with insulin resistance may need to monitor their blood sugar, maintain a healthy eating pattern, and use exercise and/or medication to keep their blood glucose in a healthy range. (These sneaky things can also raise your blood sugar.)
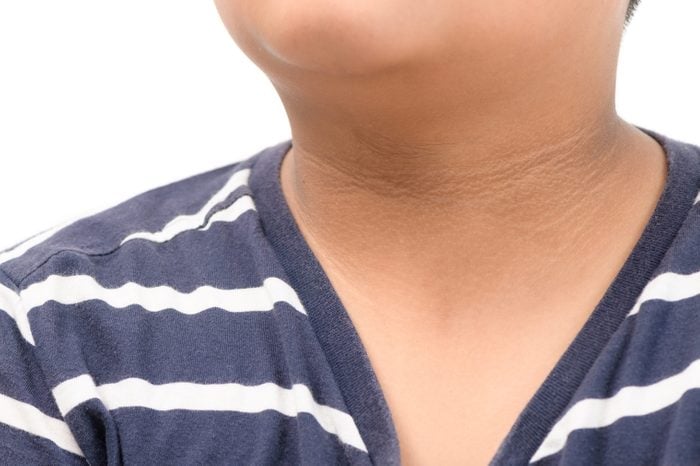
Dark skin patches
High levels of insulin in the blood can sometimes trigger the appearance of dark, velvety patches on the body, which is a skin condition known as acanthosis nigricans. The patches are typically found in body folds, such as the neck, groin, and under the arms. These patches start to appear when normal skin cells reproduce rapidly. If you have dark skin, the cells will have more melanin and manifest as a darker patch compared to the rest of the surrounding skin. Sometimes these patches are not related to any medical condition, the American Academy of Dermatology says, therefore, it’s best to consult a dermatologist that can help you find out the direct cause behind your discolored skin.

Large pores and acne
Sebum, the oil that lubricates the skin, is overproduced in those who have insulin resistance. A diet rich in carbohydrates may promote the overproduction of sebum, causing acne, according to a 2016 study published in the Journal of the American Academy of Dermatology. Eating more fresh vegetables and lean meats may help combat this and reduce your risk of insulin resistance. Here are some myths and truths you should know about large pores.

Polycystic ovarian syndrome
Women who have polycystic ovarian syndrome (PCOS) are also more likely to be insulin resistant, according to the Centers for Disease Control and Prevention. The condition is characterized by having high levels of male hormones, and an increased risk for irregular menstrual cycles, infertility, obesity, ovarian cysts, heart disease, and type 2 diabetes. If a woman with PCOS has high insulin levels, this can cause the ovaries to make more testosterone. This can lead some women to exhibit symptoms of excess androgens, such as dark hairs on the face and belly. (Here are some symptoms of PCOS.)

Hair loss in women
In addition to fat storage and regulating sugar levels, insulin helps regulates hair growth. Women who are insulin resistant may be at greater risk of female pattern baldness, suggests a 2015 study published in the Australasian Journal of Dermatology. Women who lose more than the typical amount of hair per day, estimated at about 250 strands, should be checked for insulin resistance as this may be the cause.

Swollen ankles
If you’re noticing swelling in your ankles or other parts of your body it can be one of the symptoms of insulin resistance. Swelling tends to be indicative of insulin resistance, as insulin tells the kidneys when to hold on to sodium and water. When fluid is retained unnecessarily, swelling and bloating can result. Here are some other reasons you might be bloated—and when it could signal a health problem.

Carbohydrate cravings
Unstable blood sugar levels can lead to sugar and carbohydrate cravings. This is because the body is unable to regulate blood sugar levels properly, and therefore, leaves body cells unable to absorb the available glucose. Therefore, the cells are left “starved” and signal that they need more carbohydrates to convert to energy. However, the cells’ inability to absorb blood sugar can lead levels to remain high in the bloodstream, according to Harvard T.H. Chan School of Public Health.
The good news: Unlike other insulin-related conditions, insulin resistance can improve with lifestyle changes like getting plenty of physical activity and losing weight if necessary. Rodriguez suggests the following to help your body respond better to insulin. “Eat healthy, balanced meals; take medications, such as metformin if prescribed; and get plenty of sleep,” she says. You should also watch out for these type 2 diabetes symptoms you might be missing.

