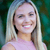What is endometriosis?
There’s a lot of confusion surrounding endometriosis—a debilitating, painful condition that affects one in 10 women during their reproductive years. In endometriosis, a type of tissue that is similar to the lining of the uterus begins growing elsewhere in the body—the ovaries, fallopian tubes, and even the intestines—where it can cause ongoing pain and even infertility. The pain can be excruciating, explains Piraye Yurttas Beim, PhD, CEO and founder of Celmatix and a board member for the Endometriosis Foundation of America.

Endometriosis is more common than people realize
The condition is distressingly common: Around the world, approximately 200 million women of reproductive age suffers from endometriosis to some degree. That’s about 10 million women in the United States alone, Beim points out. (For a glimpse of what it’s like to have this condition read this woman’s harrowing battle with endometriosis.)

Doctors may not understand it
“Despite being among the most prevalent of diseases, the condition remains under-addressed and inadequately treated at every level of our healthcare system,” explains Heather C. Guidone, surgical program director at the Center for Endometriosis Care. “A legacy of inaccuracies about endometriosis continues to be shared by doctors to patients, parents to adolescents, and media to the public, contributing significantly towards continued diagnostic delays, high treatment failures, and limited access to specialty care.”

OB-GYNs aren’t necessarily endometriosis specialists
An OB-GYN physician is considered a primary care physician rather than a specialist, explains Andrew Cook, MD, founder and medical director at Vital Health Endometriosis Center. These doctors don’t always have expertise in treating endometriosis or pelvic pain, says Dr. Cook.
If you feel your OB-GYN is meeting your needs and you’re comfortable with your doctor’s care, that’s great, he says. If, however, you feel that your concerns are not being addressed, you may want to make an appointment with another doctor—preferably a surgeon—who specializes in treating endometriosis, advises Harry Reich, MD, the Senior Medical Advisor of the Endometriosis Foundation of America.
“Find someone who does a lot of surgery for endometriosis,” their site advises. At your initial exam, Dr. Reich suggests keeping a mental checklist: The gynecologist should perform a rectal exam and schedule laparoscopy with a biopsy for analysis. If not, “then the patient should look for another doctor, immediately,” Dr. Reich says.

It targets women of all ages
The condition can be found in adolescents and even in girls as young as 8 years old, explains Ken Sinervo, MD, OB-GYN, of the Center for Endometriosis.
“Around 70 percent of girls and teens who exhibit pelvic pain will later go on to be diagnosed with endometriosis, which is why so many patients indicate that their symptoms began in adolescence, only to be dismissed for years,” he says. There seems to be a genetic component to condition—women who have a close relative with the endometriosis are up to 7 times more likely to develop it themselves, according to the Endometriosis Foundation of America.
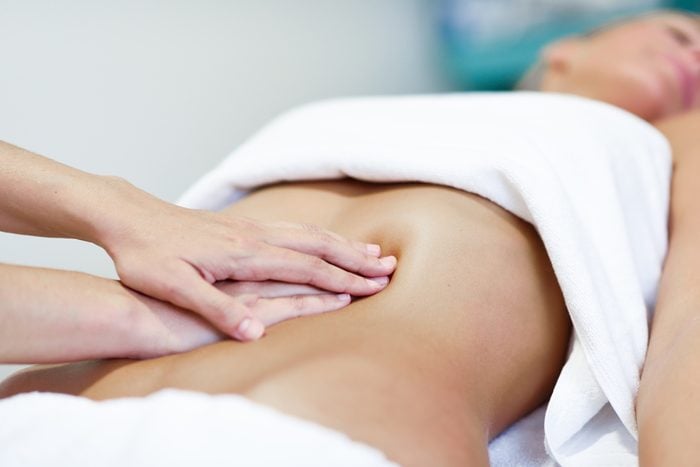
Endometriosis can spread
Despite what many doctors believe, the condition isn’t solely limited to the pelvic area in women. There are numerous reports of what is known as extrapelvic endometriosis—including rare cases involving the brain, says Dr. Sinervo. “In our own Center, for example, we routinely treat diaphragmatic, lung, and sciatic endometriosis,” he says. “It is imperative that clinicians become familiar with the various presentations of the disease, including those that are non-classical in nature.”

Doctors used to think pregnancy could relieve symptoms
This was a mistaken assumption, according to Dr. Sinervo. “In truth, many women with endometriosis can continue to experience pain and, in some cases, even progressive disease during pregnancy,” he says. “Moreover, current research has demonstrated a link between endometriosis and a higher risk of adverse obstetric outcomes and complications.” In addition, it can affect fertility. (Here are several reasons why you might not be getting pregnant.)
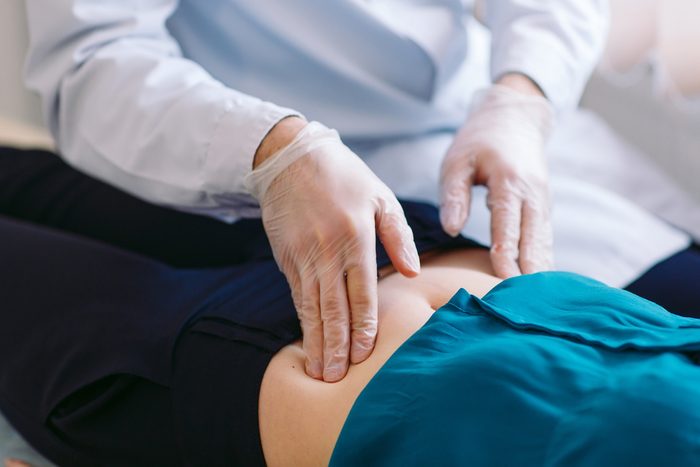
Diagnosis is tricky
Most people assume that signs of endometriosis can be spotted during a pelvic exam or during an ultrasound, but this is hardly ever the case, explains Dr. Sinervo. Another mistake many doctors make is to rule out endometriosis as a diagnosis when a patient doesn’t respond to the drugs prescribed for the condition (oral contraceptives, for example, or GnRH agonists).
“Approximately 85 percent of women who ‘fail’ medical suppression are found to have endometriosis at operation,” says Dr. Sinervo. “In other words, the absence of evidence is not evidence of absence.”
Right now, the best bet for diagnosis is surgical, he explains. Using minimally invasive techniques, a surgeon will view and even biopsy tissue to confirm endometriosis. “This is why the development of a noninvasive, accurate marker for the disease is a highly prioritized research target.”

There are ways to treat endometriosis
Some doctors still believe that a hysterectomy—complete removal of the uterus and potentially other female sex organs such as the cervix, ovaries, and fallopian tubes—can cure endometriosis. However, Dr. Sinervo points out that endometriosis is not always confined to these organs.
“The pain and symptoms arising from the disease are often not confined just to menstruation, in which case simply removing the uterus and stopping periods are not effective treatments,” he explains. “In fact, there have been many reports of endometriosis persisting after hysterectomy—even worsening. And we routinely treat patients who have had removal of their reproductive organs only to have significant disease left behind.”
In other words, it’s a myth that removing a woman’s reproductive organs can cure endometriosis. The options available for women suffering from endometriosis range from drug and hormonal therapies to specific types of minimally invasive operations, such as excision surgery.
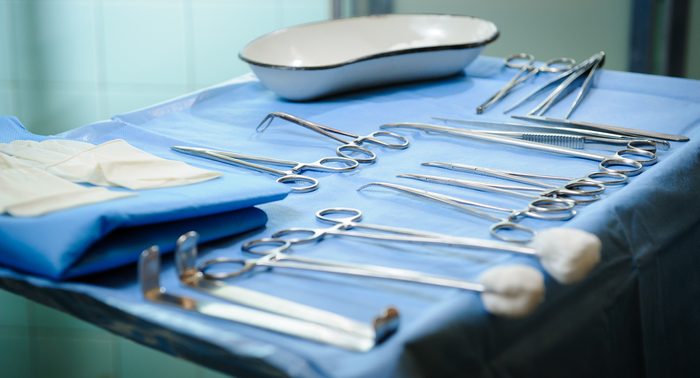
Less extreme methods can offer long-term benefits
“It is not always obvious how deep infiltration of endometriosis may be,” explains Steve Vasilev, MD, gynecologic oncologist and medical director of Integrative Gynecologic Oncology at Providence Saint John’s Health Center and a professor at John Wayne Cancer Institute in Santa Monica, California. With a technique known as excision surgery, the surgeon makes a small incision and then removes endometriotic tissue; Dr. Vasilev explains that this gives a properly trained surgeon a better chance of getting all the problematic growth. He points out that some studies suggest excisional surgery may reduce pain associated with intercourse and bowel movements, as well as chronic pelvic pain.
Unfortunately, insurance coverage can be an issue: “Insurance carriers may be reticent to pay,” Dr. Vasilev explains. However, if a surgeon finds a suspicious pelvic mass, insurers may cover the cost. (Here are 50 more secrets most surgeons won’t tell you.)

Endometriosis isn’t a guarantee of infertility
Many patients are afraid they will never be able to carry a child—but this isn’t always true, according to Dr. Cook. “If a surgery is done properly, it will help increase the chances of getting pregnant for many years following the surgery,” he says. “Once the endometriosis is removed, a woman will be more likely to become pregnant once she tries, assuming no other factors are affecting her fertility.”

Endometriosis doesn’t always go away with menopause
While women may find relief from endometriosis after going through menopause, the condition does not go away completely, according to Dr. Cook. In fact, endometriosis has been diagnosed in women in their nineties. He points out that although menopause slows the flow of estrogen that feeds the endometrial tissue, the already existing scarring and masses can still cause symptoms. “Menopause will most likely not stop the pain,” he says.

The condition needs more funding
According to patient advocate Meghan Cleary, a huge patient and clinician movement is underway: “Endometriosis organizations around the world are taking direct action to bring the definitions and treatment standards into line with current evidence-based research and medicine.”
But more funding is necessary, explains Dr. Beim: “Federal research dollars for endometriosis amount to approximately $1 per year for each woman affected by the disease. Worldwide, the average cost of endometriosis is about $10,000 per woman, per year, primarily due to lost work productivity and direct health care costs, which translates to an overall yearly cost of about $3.7 trillion, roughly equivalent to the GDP of Germany.” Learn more about why doctors often miss this crippling disease.