
They’re supposed to have a lengthy chat with you
A recent study revealed that many doctors don’t discuss prostate cancer screening pros and cons with their patients, which is pretty worrying, as we rely on our docs to keep us in the loop, right? Researchers at Brown University found that only one in three men screened with the PSA test discussed the advantages and disadvantages of the test with their doctor. The men who were more likely to undergo testing without being aware of all the pros and cons had low incomes, lacked a high school diploma, were uninsured or were Hispanic. “The most vulnerable men are getting less counseling,” said study co-author Annie Gjelsvik, an assistant professor of epidemiology at Brown’s School of Public Health. The findings, published online in the journal Urology, have been described as “alarming” by the study authors. This type of cancer in men is more common than breast cancer in women, so it’s an illness we need to be talking about. Here are 10 prostate cancer facts you might not know.

Prostate cancer is really common
“It’s the second most common cancer in men, and the third leading cause of cancer death behind lung and colon cancer,” says Timothy Wilson, MD, Professor and Chair of Urology and Director of the Urologic Oncology Research Program and at the John Wayne Cancer Institute at Providence Saint John’s Health Center in Santa Monica, CA. According to Cancer Treatments Centers of America, in most cases symptoms are not apparent in the early stages of the disease. The symptoms may be different for each man, and any one of them may be caused by other conditions. As a result, consulting with your doctor about anything odd down there is important. Common symptoms include burning or pain during urination, difficulty urinating, or trouble starting and stopping while urinating, more frequent urges to urinate at night, loss of bladder control, decreased flow or velocity of urine stream, and blood in urine. If the cancer has spread to nearby tissues or bones, men may experience blood in their semen, difficulty getting an erection, painful ejaculation, swelling in their legs or pelvic area, numbness or pain in the hips, legs or feet, or bone pain that doesn’t go away, or leads to fractures.
Screening and treatment isn’t for every man
There is a lot of controversy behind the prostate-specific antigen (PSA) blood test, and it stems from large scale studies in Europe and the US. The screen measures the level of PSA protein, which is made by cells in the prostate. When levels of the protein are elevated, cancer may be present. However, researchers found that men who skipped the test (or biopsy and treatment if they had a suspicious score on the test) lived as long as men who were screened regularly. Why? Prostate cancer can be very slow to advance, and men who avoided testing and treatment were more likely to die of something else before the cancer could become dangerous. The men who got yearly screens were more likely to get a cancer diagnosis and undergo treatment—but that didn’t mean they lived longer. And they were risking a significant decline in quality of life; prostate cancer surgery and treatment carry serious side effects like urinary incontinence, impotence, and loss of bowel control. Learn the 7 common habits that lead to prostate cancer.
The PSA continues to be problematic
Once hailed as one of the most important tests a man can have, it suffered a setback in 2012 when the U.S. Preventative Services Task Force (USPSTF) recommended against routine screening for otherwise healthy men. The recommendations were based on a growing body of evidence that suggested the benefits of PSA screening may not outweigh the potential harm of unnecessary treatment. One study estimated over-diagnosis to rise with age, from 27 percent at age 55 to 56 percent by age 75.
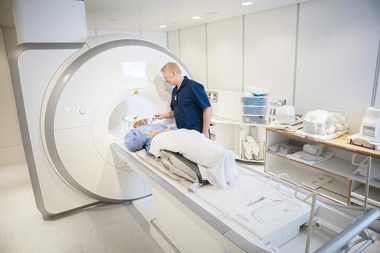
Screening exams are improving
“Common sense approaches to screening along with multi-parametric MRI, leads to more accurate biopsies and can find those men with more aggressive cancers and allow us to treat them earlier and more effectively,” explains Wilson. “In addition, new genetic tests (Prolaris and oncotype Dx) are now FDA approved that can help experts counsel patients more precisely as to whether or not treatment is really necessary.” S. Adam Ramin, MD, urologic surgeon and medical director of Urology Cancer Specialists in Los Angeles, says all men aged 55 to 69 (younger if there is a family history) should know about the Digital Rectal Exam (DRE) in addition to the PSA. “Though the DRE exam would not be the first choice for most men, it is safe and easy, and the possible benefits far outweigh the temporary discomfort,” he says. “It is important to note that there are many factors to consider with these screenings, and the decision to be tested is one that can be made with the educated advice of a knowledgeable and trusted urologist. Simply being aware of the test, and making it a priority to schedule a visit with a healthcare provider is the most important first step.” Learn the 13 signs of cancer men are likely to ignore.

New guidelines are encouraging
Recently, the U.S. Preventive Services Task Force (USPSTF) revised its 2012 recommendations against routine prostate cancer screening for otherwise healthy men: Now the USPSTF gives the screen a Grade C for men aged 55 to 69, which means you should have a detailed conversation with your doctor about the potential pros and cons. For men 70 and over, the test still gets a Grade D—it’s not recommended for this age group because the harms outweigh the risks. “The revamped 2017 guidelines now encourage conversation between patient and doctor—including discussion on whether or not the benefit of testing will outweigh the potential risk,” says Ramin. “This is a decision that has many urological specialists, including me, encouraged.” Here are the 5 signs of prostate cancer you should never ignore.