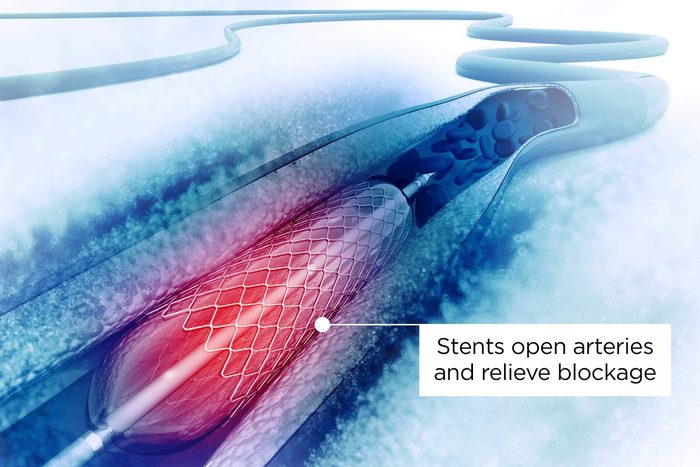
Are heart stents effective?
Heart stents have been quite popular, and they may be a lifesaving treatment in preventing heart damage during and after a heart attack. The procedure opens arteries and relieves blockage that’s causing pain. However, before getting stents in your heart, you’ll want to consider the risks of heart stent treatment and the level of effectiveness.
For instance, a small 2018 study of 200 patients with a severely blocked artery and chest pain, published in The Lancet, suggests that heart stents might not be as helpful in treating more mild heart issues, such as difficulty breathing and chest pain. The researchers noted patients who received the heart stents did see an improvement in chest pain and physical activity via treadmill tests. However, there were no notable differences between them and those who had a fake stent insertion.
If you’re on the fence about getting a heart stent or want to learn more about the treatment, here’s what you need to know.
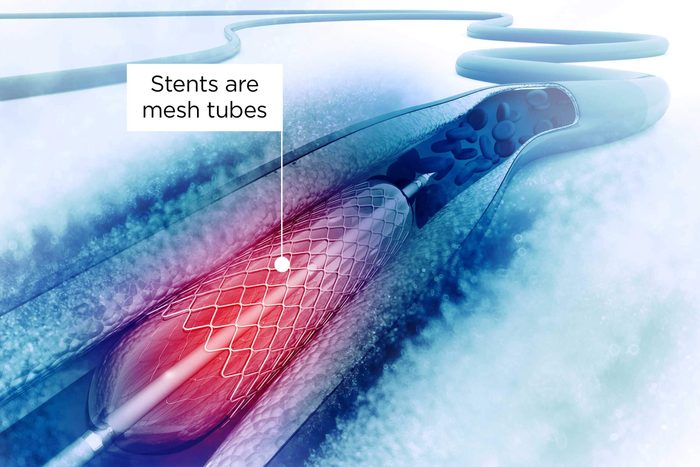
How a heart stent works
Patients are mildly sedated: They’re still awake and arousable but in a bit of a “twilight” state. The doctor then numbs an artery in the wrist or the groin and inserts a small hollow tube that allows access for catheters, says Sameer K. Mehta, MD, a cardiologist with Denver Heart: Rose Medical Center in Colorado. The physician then performs an angiogram (where dye is inserted through the catheter into the heart arteries and is seen through X-ray equipment). The physician will then determine if there is enough blockage in the arteries where the stents are needed, he says. The heart stent—a mesh tube—expands arteries to keep blood flowing. It all sounds straightforward, but stents are considered one of many risky medical procedures that don’t always pay off.
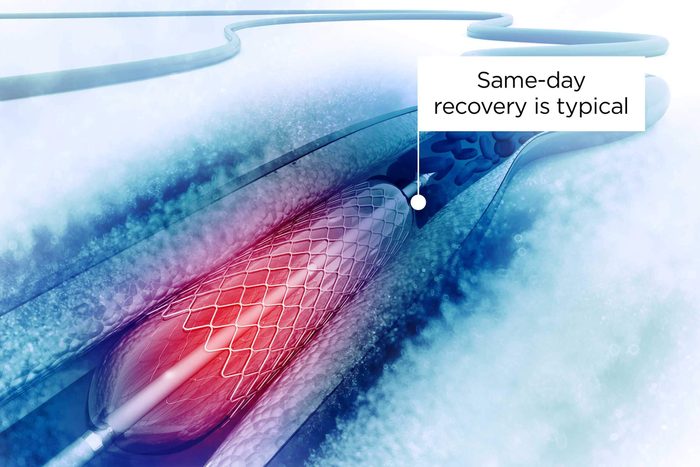
How long does it take to recover from having a stent?
Following surgery, the patient can usually recover the same day, says Dr. Mehta. Usually, if the stent was placed via the artery in the wrist, the patient won’t require much bed rest, he says. However, “if the femoral artery is utilized, the patient may require anywhere from two to six hours of bed rest,” Dr. Mehta explains. (Beware of the worst heart foods.)
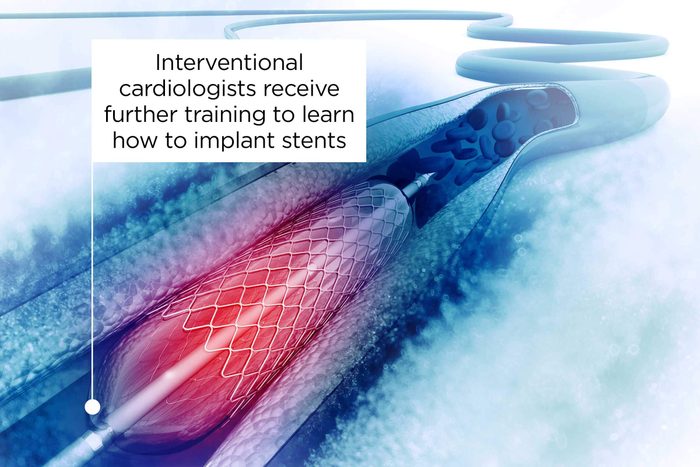
Choose an interventional cardiologist
Most cardiologists can do the procedure; however, you’ll want to make sure you’re in the best hands possible. That means you’ll want a doctor who is up-to-date on the procedure, reliable, and trustworthy, Dr. Mehta says. “All cardiologists are well-versed at the discussion regarding stents, as are the vast majority of primary care providers,” he says. However, “an interventional cardiologist is a cardiologist who received further training to learn how to implant stents. As such, interventional cardiologists, in general, would be the foremost experts in the field,” Dr. Mehta explains. (Learn the things heart doctors do to protect their own heart.)
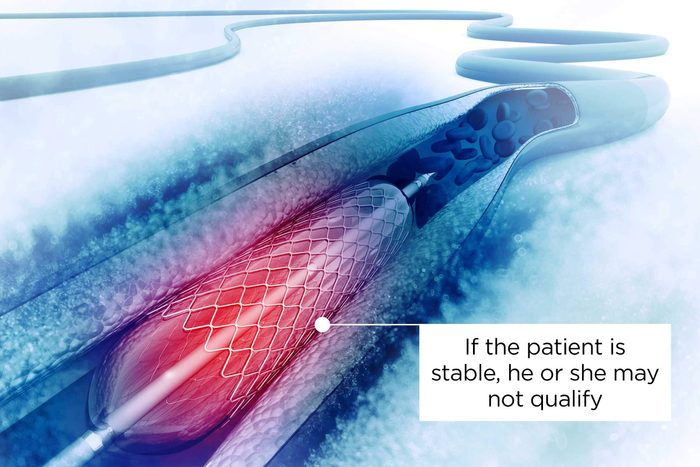
Verify if you qualify for a stent
The bottom line is that the procedure is performed too often in people who won’t benefit, according to the experts. The Lancet study found that for mild chest pain and breathing trouble, the stents don’t make sense at all. According to Dr. Mehta, “In patients who are stable, the doctor and patient will make a collaborative decision on when to progress to stenting (depending on the angiogram),” he says. They’ll look at how positive—or high risk—their stress test is, if one was done, he explains. The patient’s health will also come into play—would the surgery be dangerous for them? For people who have sudden or unstable heart symptoms, the decision will be more obvious, says Dr. Mehta: A heart stent may be a life-saving option, at that point.
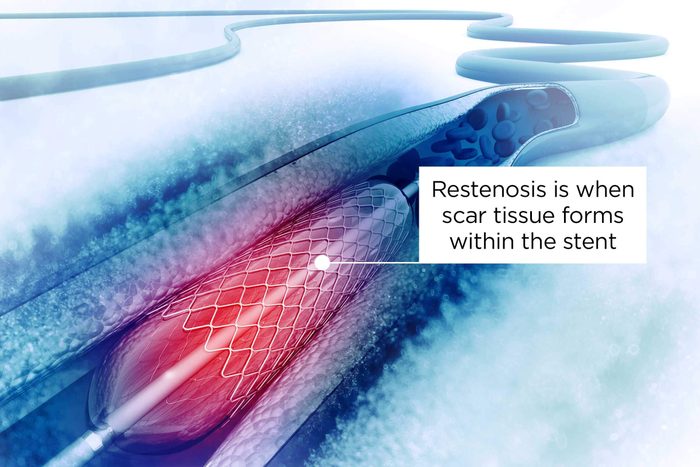
You could develop restenosis
It’s important to note that you may restenosis may be a side effect of heart stents. This is when scar tissue forms within the stent, says Dr. Mehta. “Basically, stents heal when the body’s own cells, known as endothelial cells, line the inside of the stent. This process occurs normally. However, occasionally the body lays down an excessive amount of cells known as fibroblasts within the inside of the stent,” says Dr. Mehta. When this occurs, the artery within the stent basically becomes “blocked” again due to scar tissue, and restenosis can result. Symptoms of restenosis are usually chest pain or shortness of breath, he says.
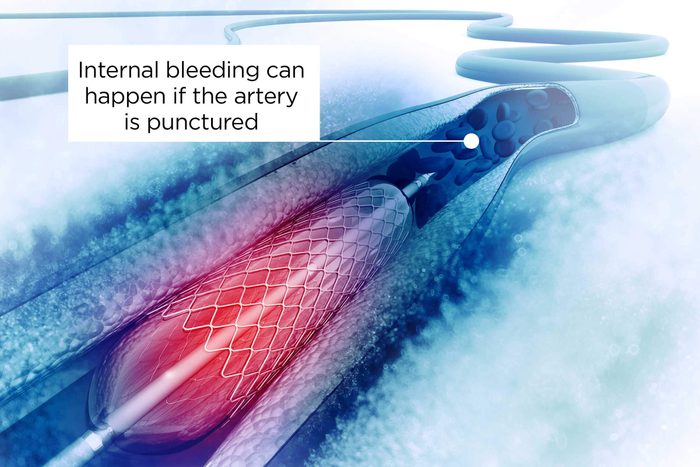
There’s a risk of internal bleeding
This happens if the artery is punctured during the procedure. Because patients are often placed on blood thinners, such as heparin, during the procedure, the bleeding can be problematic and can happen anywhere within the body, says Dr. Mehta. You may also be at risk for a blood clot. “Stent placement is not without risk. Between 1 to 2 percent of patients may develop a blood clot at the site of the stent, with the greatest risk in the first several months after placement. This may further elevate the risk for a heart attack or stroke,” says Robert Glatter, MD, an assistant professor of emergency medicine at Northwell Health and attending emergency physician at Lenox Hill Hospital in New York City.
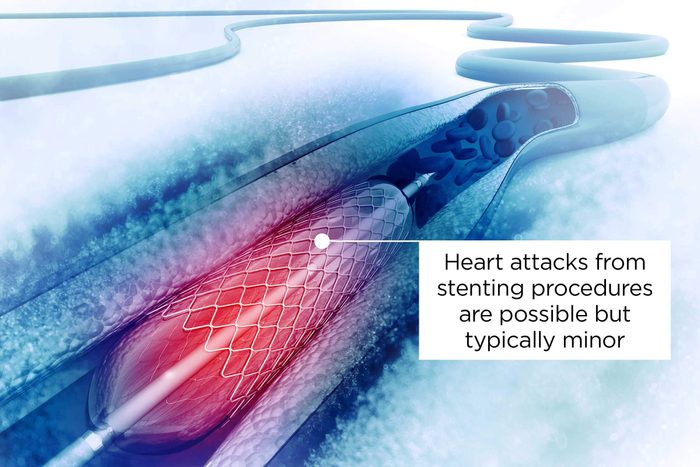
You could have a heart attack
Heart attacks can occur during the stenting procedure as plaque breaks off from the artery, warns Dr. Mehta. As this plaque moves toward the heart, or the artery tears (though rare), a heart attack can be a risk, he explains. “However, most heart attacks from stenting procedures are minor in nature,” he says. (Find out about the countries with the lowest heart disease rates.)
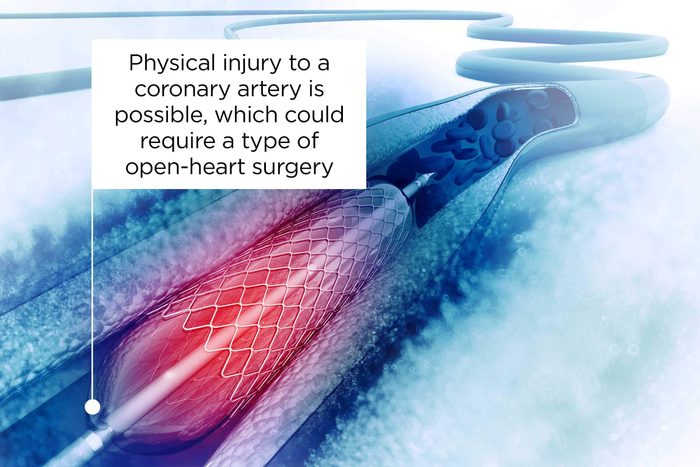
You might end up with open-heart surgery
In a very small percentage of cases, there can also be physical injury to a coronary artery from the catheter, requiring a type of open-heart surgery called a coronary artery bypass grafting or a minimally invasive direct coronary artery bypass (mid-CAB) procedure, says Dr. Glatter. Though rare, your kidney could suffer damage: “The risk of kidney injury from the dye used during heart stent placement remains an ever-present risk, albeit a small one,” Dr. Glatter says.
With some patients, a stent may trigger an irregular heartbeat. “If arrhythmias occur, we may need to administer special medications or electricity to restore the normal cardiac rhythm,” he adds.
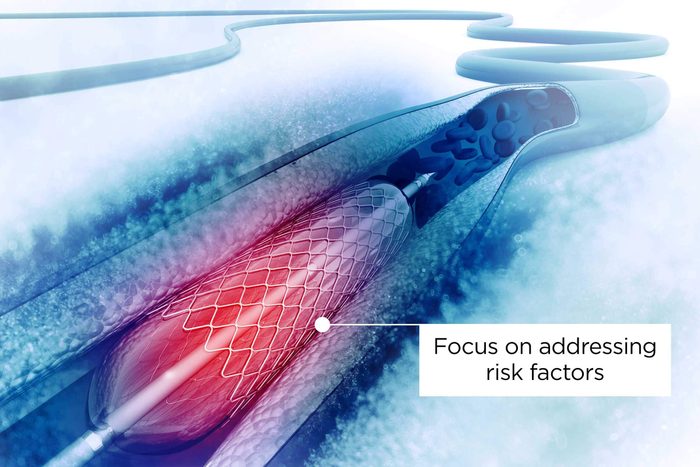
Stents aren’t always needed
Before booking an appointment, make sure you’re up-to-date on stent information and that you’re following all the healthy habits to prevent heart disease and stroke to protect your heart. “The bottom line is that doctors should approach the treatment of patients with stable coronary artery disease using optimal medical therapy—not stents—and maintain a focus on addressing risk factors, such as not smoking and improving dietary habits, while encouraging ongoing and regular aerobic exercise and physical activity,” says Dr. Glatter.