How allergists manage their allergies
Allergy season is here. How do you know? Your runny nose, non-stop sneezing, and itchy red eyes remind you it’s one of the worst times of the year.
According to the American College of Allergy, Asthma & Immunology, over 50 million Americans experience allergies each year. Pollens that come from trees, grasses, or weeds are among the most common causes of allergies. So, how do you treat your allergies? Typically, avoiding or reducing your exposure can help alleviate your symptoms. However, what do you do if your symptoms don’t seem to be getting better?
We spoke with allergists who reveal how they keep their own allergies under control to reduce the severity of their allergy symptoms.

Stock up on meds before allergy season begins
There’s no place for procrastination during allergy season. Call your doctor’s office for new prescriptions before you’re stuck with a bad case of the sniffles, sneezing, and itchy, watery eyes. “Be proactive and start a daily antihistamine or nasal steroid before the season begins,” says Mitchell H. Grayson, MD, chief of the Division of Allergy and Immunology at Nationwide Children’s Hospital in Columbus, Ohio, (who happens to be allergic to cats, dust mites, tree, grass, and weed pollen). You can take antihistamines year-round, if necessary. However, nasal steroids need between a week and 10 days to become fully effective, so be sure to take it well before allergy season rolls around. Try an antihistamine like Allegra, Claritin, or Zyrtec; but steer clear of brands that contain chemicals like diphenhydramine that cause sedation and other side effects like depression. Waiting till the last minute to get your allergy meds isn’t the only thing that may make your allergies worse, your contact lenses do too.

Don’t overdo it on the nasal decongestants
Nasal decongestant sprays work like a charm because they shrink the swollen tissues in your nasal passages that cause congestion. Unfortunately, these drugs are not for long-term use. If you go overboard and use the spray for more than five days in a row, you can actually exacerbate your allergy symptoms and become addicted from overuse. “I avoid nasal decongestants, like oxymetazoline because it could worsen congestion over time or so-called rebound phenomenon,” says Dr. Grayson. In a 2014 study published in The Journal of Allergy & Clinical Immunology, 895 people with moderate to severe rhinitis (a runny or stuffy nose) completed a questionnaire about the allergy medication they use. Despite the fact that 80 percent of patients knew there was a time limit they shouldn’t exceed for their nasal decongestant spray use, nearly 49 percent still reported overusing it. ((Find out the truth behind the big myths about allergies.)

Steroid nose sprays are the way to go
Unlike nasal decongestant sprays, steroid nose sprays are safe to use for longer periods of time and clear up your sinuses. “The steroid sprays do the most benefit for the most number of people,” says Warren V. Filley, MD, staff allergist at the Oklahoma Allergy & Asthma Clinic and clinical professor of medicine at the University of Oklahoma Health Sciences Center, who is allergic to pollen, grass pollen, weeds, and dust mites. “I think people should use an antihistamine, a steroid nose spray, and saltwater rinses.” Nasal steroid sprays decrease the inflammation in your nasal passages caused by allergens, which helps treat sneezing, runny nose, congestion, and post-nasal drip. Nasacort, a nasal steroid spray, works best for Dr. Filley because it lasts up to 24 hours and contains triamcinolone, a chemical well-known for its non-sedating effects and fewer side effects like depression. Another viable nasal steroid spray is Flonase, which contains fluticasone, a chemical similar to triamcinolone. Check out these other allergy nasal sprays that doctors recommend.
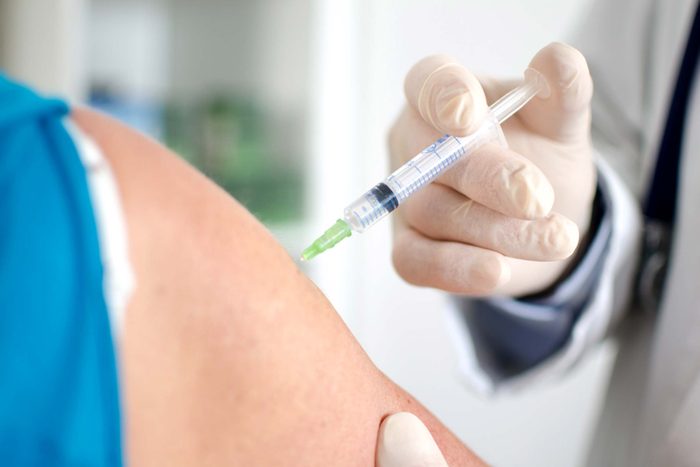
Consider allergy shots
If you’re sick of popping pills every day and aren’t afraid of needles, allergy shots may be right for you. The shot works like a vaccine, and it injects your body with gradually increased amounts of the allergen to build up your body’s immunity to the irritant. “I take allergy shots and they’ve made a huge difference in the way I feel,” says Dr. Filley. “Now I don’t need medicines every day. I use the medications on more of an ‘as needed’ basis.” He gets an allergy shot every two to three weeks, depending on the severity of his allergies. Initially, you receive increasing amounts of the allergen once or twice a week for three to six months. This will help build up your tolerance. Once the effective dose has been reached, the doctor will wean you off weekly injections and switch you to a biweekly or monthly regimen depending on your body’s reaction. One time you should skip the shots: If your asthma or allergies are acting up, as they make those symptoms harder to treat.

Always rinse your nose
After being outside or in another environment where you’re exposed to allergens, it’s always best to rinse your nose with saltwater. “If I’ve been outside working or in dusty areas, I go in as soon as I can and do the rinse,” says Dr. Filley. “Then I use the steroid spray. [The rinse] quiets things down and gets rid of the allergens and the steroid has a better chance of spraying into the nose.” Use a squeeze bottle or a Neti pot and make sure that the saline wash you choose doesn’t contain iodine, as that irritates the nasal passages. You should rinse your nose once to twice daily. (Don’t miss these other natural remedies for allergies.)

Wash your bedding on a weekly basis
Your bed’s warm, humid environment is dust mite heaven, so you better throw those bedsheets in the washer regularly. Both Dr. Filley and Dr. Grayson wash their bedding in hot water on a weekly basis. Hot water and drying your sheets on high heat kills those pesky dust mites for good. For an added layer of protection, buy dust mite-proof covers for your bedding that you don’t have to wash frequently like your pillows, mattress, and comforter. The tight weave on these allergen covers keeps dust mites from crawling into bed with you each night. Check out these other tips for getting rid of dust mites.

Invest in a dehumidifier
A humid home means unwanted houseguests like dust mites and mold. Dehumidifiers reduce the dampness in your home and lessen the risk of it becoming an allergen cesspool. Use a vacuum cleaner with a HEPA (high-efficiency particulate air) filter, which throws less dirt and fewer dust mites back into the room as you vacuum. They also get rid of allergens and irritants in your home.

Hire help to do your outdoor chores
During high pollination season, working around the yard may be the bane of your existence. Do yourself a favor and hire a neighbor to do the yard work for you. “I have a neighborhood kid who mows my yard,” says Dr. Filley. “He enjoys the money.” If you prefer doing things yourself, cover your body from head to toe with a mouth and nose mask, long sleeves, pants, and gloves to keep your allergies at bay. A quick nose rinse and shower after an afternoon of manual labor is also a good idea.

Filter the air in your home
There’s nothing more satisfying than a fresh spring breeze blowing through your home in the springtime. Unfortunately, that fresh air is detrimental to your health during allergy season. Keep your windows and doors closed as the first step to controlling your allergies inside. Air conditioners with filters are another item to consider. “I buy a standard 3-inch filter that you replace every two months,” says Dr. Filley. “It gets quite a bit of dust and debris.” The same habits apply to your car. “When driving, I keep my windows closed and run the air conditioner so the air passes through a filter,” says Dr. Grayson. Adding plants like the fig tree and the Boston fern to your living room may also help clean up the air inside your house and quell those allergies.