Subtle signs of skin cancer you shouldn’t ignore
When the weather gets warmer and daylight hours longer, people are more likely to spend time outdoors in the sun. This also means there’s an increased risk for skin cancer. It’s the most common form of cancer in the U.S., with at least 1 in 5 Americans projected to develop it by age 70, according to the Skin Cancer Foundation.
Although it’s common, it’s also the most preventable and curable cancer if caught early. It’s recommended that you do monthly self-check exams from head to toe to look at moles and any other abnormalities on the skin. But aside from monitoring spots throughout your body, there are other subtle signs of skin cancer you may be ignoring.
We asked dermatologists to tell us what skin cancer symptoms people might miss.
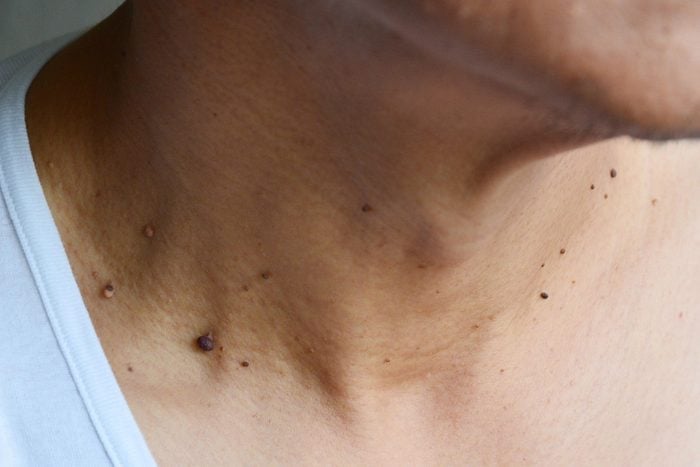
Skin growths or moles that aren’t brown or black
While you might focus on brown or dark moles when you think of skin cancer, there are actually several types of skin growths to keep an eye on. The major types of skin cancer are basal cell carcinoma, squamous cell carcinoma, and melanoma. Basal cell carcinoma is the most common type of skin cancer—there are 4.3 million cases in the United States each year, according to the Skin Cancer Foundation. Squamous cell carcinoma is the second most common, hitting another million Americans yearly.
Melanoma is the rarest—but the deadliest—type of skin cancer; one in 19 people who get a diagnosis of melanoma will eventually die of the disease. (By comparison, one in roughly 300 people will die of basal cell or squamous cancers.)
The tricky part is recognizing trouble, says surgical and cosmetic dermatologist Adele Haimovic, MD, an associate at the office of Lance H. Brown, MD, in New York City. Some melanoma moles can actually be skin-colored or pink—they’re known as amelanotic melanomas. This kind of melanoma is a challenge to recognize because we’re inclined to think it’s just a harmless bump. That’s why it’s important to have regular skin checks by a dermatologist to look at any skin growths or abnormalities.

Shaving nicks
If you find yourself bleeding after shaving, it may not be due to clumsiness: “Basal cell carcinoma and squamous cell carcinoma can bleed after shaving or other minor trauma, and sometimes spontaneously bleed with no known inciting event,” says Dr. Haimovic. “This is because skin cancer leaves the skin more fragile than healthy skin.” If you find yourself bleeding in the same spot, get it checked out. (Read about the 8 ways your body changes after just one sunburn.)
Your family tree
About one in ten people who are diagnosed with melanoma have a family member with a history of melanoma, according to the Skin Cancer Foundation. Familial malignant melanoma refers to families in which two or more first-degree relatives, such as a mother, father, siblings, or children, have melanoma. Familial malignant melanoma increases melanoma risk by 50 percent.
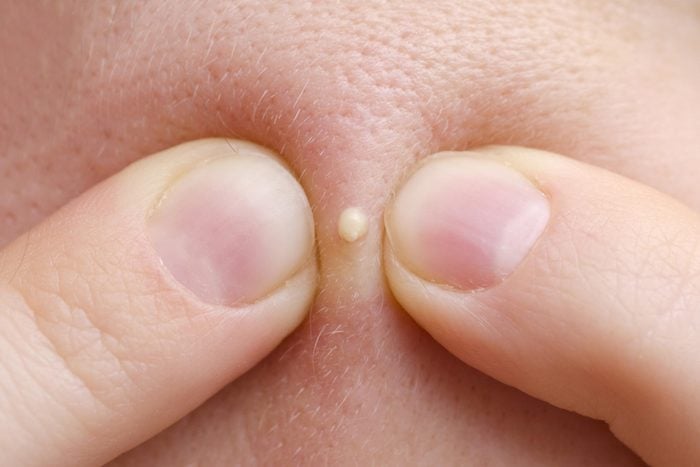
A pimple that doesn’t go away
“Basal cell carcinoma may look like a translucent, skin-colored, or pink pimple that does not resolve or recurs in the same spot,” says Dr. Haimovic. Usually, pimples go away on their own in two to three weeks; if one sticks around longer than that, it should be evaluated by a dermatologist. (Make sure you know the skin cancer myths you need to stop believing.)
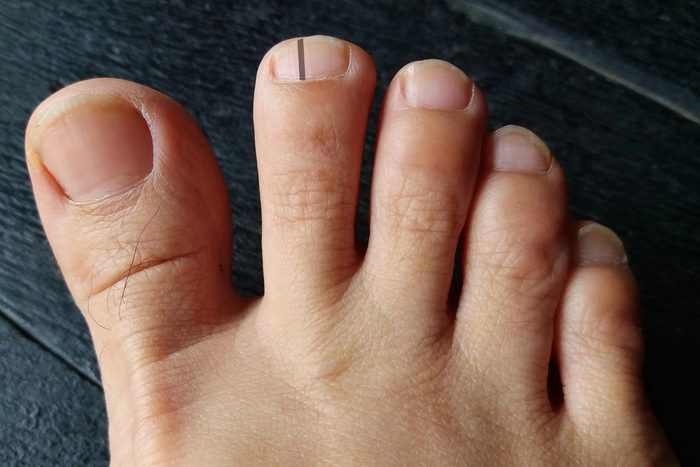
A dark band on your nail
If you notice a fairly defined, dark vertical line on your fingernail or toenail, you might think you banged the nail. Take a closer look: “If the band has multiple different shades of brown and black, that is a concern. Also, if the width of the band is greater than three millimeters, that is another concerning feature,” says dermatologist Steven Wang, MD, founder of Dr. Wang Herbal Skincare. Although there are other causes (such as an injury), a dark vertical line can sometimes be a sign of a melanoma, so make sure to ask your doctor to take a look.
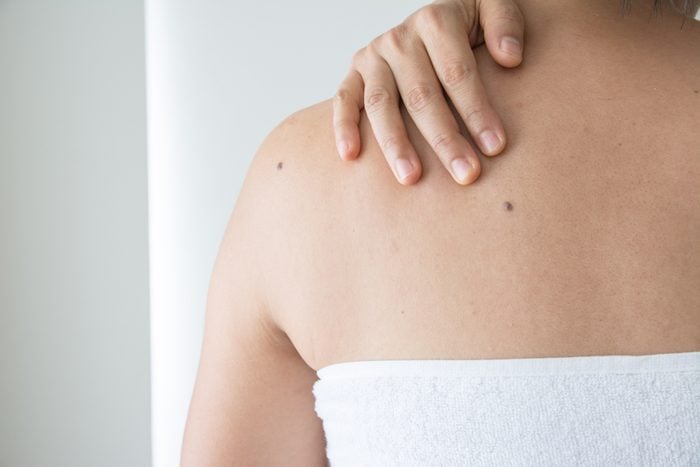
One of your moles is not like the others
“A reddish-colored or light-brown-colored mole in a sea of dark moles is what dermatologists call ‘the ugly duckling sign,'” says Dr. Wang. Basically, one of the moles doesn’t belong in the group or doesn’t look like the others, so it could be a sign of melanoma. If you have a dominant mole pattern on your back and it’s disrupted by a darker, larger mole, it could be an ugly duckling sign. Another example: You have two patterns of small and dark moles on your back, but there’s a smaller, pale mole. The only way to confirm if this is malignant melanoma is to have it checked by a dermatologist. Here’s what you need to know about mole mapping.

You’ve had PUVA treatments
Psoralen and UV-light treatments (PUVA) are a type of ultraviolet radiation treatment for severe skin conditions such as psoriasis and dermatitis. A previous study published in the Journal of the American Academy of Dermatology found an increased risk of malignant melanomas 15 years after a patient’s first PUVA treatment. In fact, patients who had 250 or more treatments had five times the risk of people who had never gotten PUVA. The American Osteopathic College of Dermatology acknowledges that PUVA may increase a person’s risk of developing melanoma, but the likelihood may occur after undergoing at least 150 treatments.
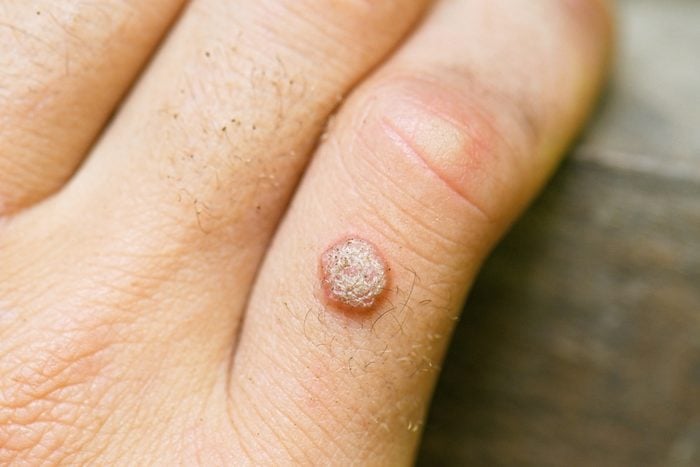
You’ve had an HPV infection
Some forms of human papillomavirus (HPV) are known to infect the genitals and anus, increasing the risk of cervical and other types of cancers. Other kinds of HPV (there are more than 100 in this family of viruses) can cause warts on the skin, often the hands or feet.
It’s thought that these skin wart-causing viruses may also increase the risk of nonmelanoma skin cancers. In a 2012 study published in the American Journal of Epidemiology, the participants with antibodies against certain types of HPV had a higher risk of developing nonmelanoma skin cancer. (Make sure you know the things that dermatologists want you to know about skin cancer.)

Your immune system is weak
People with weakened immune systems because of disease or certain types of treatment can have a higher risk of skin cancer. HIV/AIDS and lymphoma patients may have an elevated risk, for example, according to the American Cancer Society. This is also true of people who get chemotherapy or other medications that suppress immunity.

You have the XP gene
Xeroderma pigmentosum (XP) is a rare inherited disorder. According to the Genetics Home Reference, it’s estimated that about one in one million people in the United States and Europe have it. People with the disorder have an extreme sensitivity to ultraviolet rays from the sun. The gene limits skin cells’ ability to repair damage to their DNA. According to the American Cancer Society, people with XP have a high risk of developing melanoma and other skin cancers when they are young—when the condition usually reveals itself—especially on the eyes and sun-exposed areas. (Take a look at these sneaky places skin cancer may be lurking that aren’t on your skin.)

You work with industrial chemicals
People who work in the fields growing produce, in steel and iron foundries, or in coal and aluminum production plants have a higher risk of skin cancer, according to a 2014 study published in BioMed Research International. Also at risk are people who work with industrial carcinogens. These include arsenic—used in pesticides—and polycyclic aromatic hydrocarbons—which are in raw paraffin, creosote, chimney soot, asphalt, shale oil, tar and pitch, and even diesel-engine exhaust fumes.
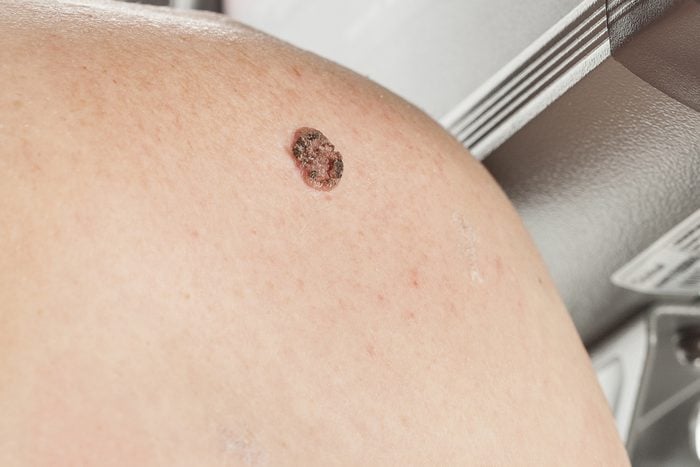
You already had skin cancer
Just because you’ve had a squamous cell carcinoma or another type of skin cancer emoved doesn’t mean you can relax—if anything, you should be more concerned. Squamous cell carcinoma recurrence is relatively common on the ears, nose, and lips; it typically occurs during the first two years following surgery. In fact, having any type of skin cancer makes it more likely that you will develop another type of skin cancer. “During your regular skin check, your dermatologist will examine old scars to make sure there is no evidence of the cancer returning,” says Dr. Haimovic. (Be aware of these 9 surprising skin cancer risks.)
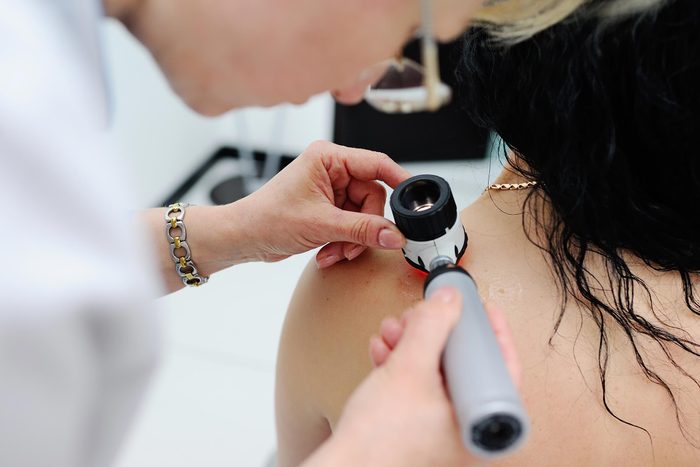
Stay vigilant
Dermatologists recommend that you do a monthly self-check of your moles and any other skin abnormalities to help catch trouble early. This will help you keep tabs on any changes. Be on the lookout for moles or lesions that changed in color (including fading), shape, or size, or if you’re experiencing pain, itching, or bleeding in these areas, Dr. Wang advises.
If you do have a growth, use the guideline called ABCDE to evaluate it. That stands for asymmetry (melanomas are less likely to be symmetrical), border (melanoma borders tend to be uneven), color (multiple colors aren’t good), diameter (if it’s the size of pencil eraser or bigger, that’s a red flag), and evolving (a change in size or behavior, such as bleeding, itching, or crusting).
The good news is that although skin cancer is the most common form of cancer in the U.S, it is usually curable if detected early. (Here are some other places you may be ignoring when you check for signs of skin cancer.)

