What causes hypoglycemia?
Taking certain diabetes medications, skipping meals, not consuming enough carbs, and even too much exercise can throw your blood sugar off balance and cause low blood sugar. Insomnia and excessive alcohol consumption have also been linked to low glucose levels. When blood sugar dips to a level that’s too low to sustain normal functioning—in most people, that’s below 70 mg/dl—it results in a hypoglycemic attack with varying symptoms depending on its severity. People who have recurring bouts of low blood sugar have hypoglycemia, and they may have no warning signs at all, explains Michael Bergman, MD, endocrinologist and clinical professor of medicine at NYU Langone Medical Center. This is known as hypoglycemia unawareness; the longer you’ve had diabetes, the more common it is. (Here’s the difference between hypoglycemia and hyperglycemia.)
On the milder end of the low blood sugar spectrum, you may feel hungry, nauseated, jittery, nervous, and have cold and clammy-feeling skin. Many people also describe the feeling that their heart is racing or pounding. Low blood sugar can happen at night, too, causing nightmares and night sweats. Moderate low blood sugar can cause behavioral changes, making you fearful, confused, or angry. It can also trigger blurry vision, slurred speech, and problems with balance and walking. Observers may mistake you for being drunk. If you don’t get treatment and you suffer severely low blood sugar, you could lose consciousness and possibly experience seizures, irreversible brain or heart damage, coma, or even death. (Here are first aid tips to handle a diabetic emergency.)

What to eat during a hypoglycemic attack
It goes like this: If your blood sugar reading is low (below 70 mg/dl), eat or drink something equal to 15 grams of fast-acting carbohydrate (4 ounces of juice). Even if you feel okay, don’t wait for the symptoms of hypoglycemia to kick in when you have low blood sugar. Rest for 15 minutes and re-check your blood glucose. Still low? Repeat the process until your blood sugar reaches a healthy range. Make sure your blood sugar has returned to normal before then eating a meal, warns Elizabeth Halprin, MD, clinical director of the Adult Diabetes Section at Joslin Diabetes Center and instructor of medicine at Harvard Medical School. If your next meal is more than an hour away, snack on one carbohydrate choice (an option in a diabetic eating plan that’s roughly equal to 80 calories and 15 grams of carbohydrates) to keep your blood sugar from dipping again. (Here are some other helpful hints for keeping stable blood sugar levels.)

Stock up on the right snacks
A mild case of hypoglycemia can be treated quickly by eating or drinking a small portion of glucose-rich food, or food equal to one carbohydrate choice (15 grams of carb). “As hard as it might be, try not to over-treat the low sugar,” says Dr. Halprin. “Keep in mind that the symptoms last much longer than the actual low.” Don’t leave home without the following fast-acting carbs to combat low blood sugar, equivalent to 15 to 20 grams: three or four glucose tablets; four or five saltine crackers; five or six pieces of hard candy; two tablespoons of raisins; one serving of glucose gel; a half cup of fruit juice or regular soda; a cup of milk; or one tablespoon of honey.

Treat your low blood sugar before you drive
If you have hypoglycemic unawareness—and won’t notice the symptoms before it’s too late—the National Highway Traffic Safety Administration advises letting someone else do the driving. Just as you shouldn’t drive when you’re sleep-deprived, if you have diabetes, you should never hit the road hungry. Test your blood sugar before you start the engine. If it’s not in the target range, treat it, then wait 15 minutes and recheck to make sure you’re good to go. For extra protection, eat a protein-rich snack (like a small apple and quarter cup of trail mix) before your trip. If you experience any low blood sugar symptoms while driving, pull over immediately.
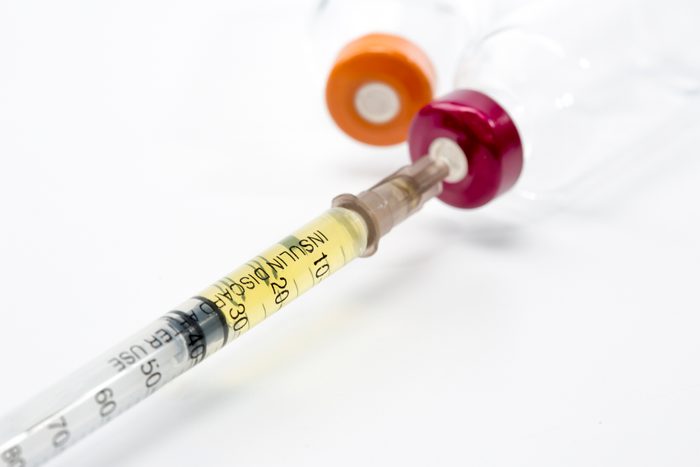
Get a glucagon kit
If you have hypoglycemia, and your blood sugar levels dip dangerously low, you may not be awake enough to eat or drink something to get them back up. If this occurs, you’ll need a glucagon shot, explains Dr. Bergman. Glucagon is a hormone that helps raise blood sugar levels quickly. Your doctor can prescribe a glucagon kit—and you should keep it in a place where your loved ones can easily access it for when you have dangerously low blood sugar.
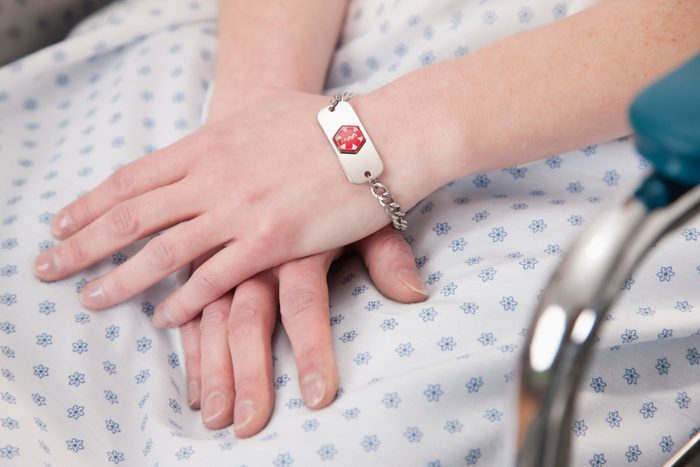
Rock a medical ID
It’s important for people who have hypoglycemia to keep a medical alert device in case of a severe hypoglycemic episode—and it doesn’t have to be in the form of a boring, clunky bracelet or necklace. The medical alert market now boasts everything from super-stylish jewelry designs (for women and men) to tattoos people design themselves. Just be sure that whichever style you choose is etched with your key health information. Some IDs even include compact USB drives that can carry a person’s full medical record for use in an emergency, according to the American Diabetes Association.

Become a self-test pro
The only way to know for sure if your blood sugar is getting too low is to test your glucose levels. To get the most accurate results, be sure to keep your meter at room temperature, check the expiration date of all your testing supplies, and wash your hands with warm, soapy water (and dry them well) before pricking your finger. Humidity, outdated test strips, and wet fingers can make your test results unreliable. Track your results and take them to your next doctor’s appointment. Together you can figure out any low blood sugar patterns.