A new way to think about health
Could the final frontier of medicine actually be inside us already? New research like that presented at the recent Gut Microbiota for Health World Summit, organized in part by the American Gastroenterological Association (AGA), is illuminating how the gut microbiome may be the secret key to unlocking better health and disease prevention. But what exactly is the microbiome? “The gut microbiota is a vast community of bacteria and other microscopic organisms, including fungi and viruses, that live in our intestines,” says pediatric gastroenterologist Geoffrey A. Preidis, MD, PhD, an assistant professor at Baylor College of Medicine and Texas Children’s Hospital and a scientific advisory board member for the American Gastroenterological Association Center for Gut Microbiome Research & Education. “There are more microbes in our gut than there are human cells in our body! Each of these microbes carries genetic material in the form of DNA, and the whole collection of this community’s DNA is called the microbiome.”
Is the gut our disease control center?
Responding to signals from us and the outside environment, the gut microbes produce substances that affect our health throughout our body, Dr. Preidis says. “Only recently have we begun to understand just how important the microbiome is to human health and well-being,” he says. “Dozens of diseases, including obesity, undernutrition, diabetes, cardiovascular diseases, cancer, and allergy, have been linked to alterations in the gut microbiome.” But in a chicken-or-egg conundrum, it’s often hard to say if gut changes are the cause or the effect of these diseases. “We still have much to learn,” he says. One thing is clear: “When we eat, we are not just feeding ourselves—gut microbes start feasting even before our meal can be absorbed by our intestines,” Dr. Preidis says. “Different types of gut microbes prefer different foods, and changes in our diet can have rapid and dramatic effects on the gut microbiome and its function.” Here are some of the most groundbreaking recent discoveries. And keep an eye out for 13 signs that your gut microbiome might be in trouble.

Diet may help prevent infection
One of the most notable studies from the World Summit showed how a low-fat, high-fiber diet, compared to a high-fat diet, may help prevent the dangerous infection C. difficile. “Antibiotics are typically prescribed to eliminate harmful bacteria that make us sick, but antibiotics cause collateral damage, eliminating beneficial bacteria at the same time,” Dr. Preidis says. “Sometimes, this creates an opportunity for dangerous bacteria like C. difficile to flourish.” The new study suggests a healthy diet may help counteract this effect. Other microbiome research has shown how a stool transplant procedure called fecal microbiota transplantation (FMT) is effective in treating C. diff, but altering the diet of high-risk people may be an even easier option to prevent the infection. Start with these best probiotic foods for your gut.

Prebiotics may prevent the side effects of radiation treatment
Another noteworthy study from the World Summit found that a prebiotic supplement may help patients with blood cancer avoid some side effects of radiation, such as weight loss and reduced nutrition, by helping to maintain a healthier intestinal environment. “Prebiotics are non-living products that influence the gut microbiota, either by causing beneficial populations of microbes to flourish or by helping these good microbes perform their healthy tasks,” Dr. Preidis says. “There is currently much less clinical data to support the use of prebiotics [than probiotics, which are living bacteria], but this is likely to change as more research is completed.” Learn more about the difference between probiotics and prebiotics.

MS may be caused by gut bacteria
The neurodegenerative autoimmune disease multiple sclerosis (MS) currently has no cure—but scientists are closer to figuring out its cause, and that discovery could lead to new treatment options. “Studies are linking dysbiosis—the wrong types of bacterial species in the gut—with autoimmune conditions like multiple sclerosis as well as neurodegenerative diseases,” says biochemist Erika Angle, PhD, CEO of the gut microbiome testing company Ixcela. One recent study from Switzerland revealed how certain gut microbes in MS patients form a protein that ramps up immune cells; these aggressive cells may migrate to the brain and begin attacking healthy nerves. Targeting this protein may be the key to halting MS’s effects.

Lupus linked to unhealthy guts
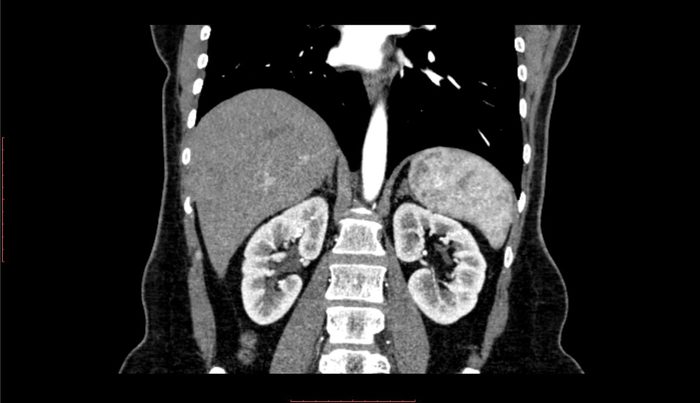
Turns out, the autoimmune disorder lupus may start in the gut: A recent small study from NYU has found the first link between altered gut bacteria and lupus, a condition in which the immune system damages various parts of the body including the skin, joints, kidneys, or heart. “Our study strongly suggests that in some patients, bacterial imbalances may be driving lupus and its associated disease flares,” study author and immunologist Gregg Silverman, MD, said in a statement. “Our results also point to leakages of bacteria from the gut as a possible immune system trigger of the disease.” If larger studies confirm the results, new treatments using probiotics and dietary changes could bring hope for lupus patients. Make sure you know about these lupus symptoms you should never ignore.

Gut bacteria and depression
Although scientists have been researching a potential link between mental health and gut health for years, the first population study has recently been published, and it sheds light on the specific bacteria present in humans with depression. Furthermore, the study investigated how gut bacteria produce neurotransmitters that affect mood. “The production of brain chemicals, such as serotonin, by human cells can be amplified or diminished by gut microbes,” Dr. Preidis says. “The more we learn about the connection between the brain and gut microbiome, the closer we will come to managing mental health disorders with microbiome-targeting therapies.” Depression isn’t alone—here are 11 more conditions that can start with gut bacteria. With the rise of popularity in gut health, at-home gut health tests are also becoming more popular.

Childhood trauma linked to gut problems
Even more disturbingly, recent research from Columbia University has linked childhood trauma to gut issues and the potential for future mental health problems. Children with “caregiver disruptions,” such as placement in an orphanage or foster care, had different gut microbiomes and different brain activity patterns than children without such trauma. The children also had more GI symptoms like stomach aches, constipation, and vomiting. “Our study is among the first to link disruption of a child’s gastrointestinal microbiome triggered by early-life adversity with brain activity in regions associated with emotional health,” lead study author Bridget Callaghan said in a statement. Again, if the study’s results are replicated, diet and probiotics may have a role to play in the treatment of childhood trauma.

New understanding of the “second brain”
Did you know your gut contains another brain? Scientists refer to the enteric nervous system (ENS)—a collection of cells lining the GI tract—as the “second brain” because it acts independently from your actual brain and spinal cord to sense, respond to, and “feel” what’s going on in the gut. For the first time, researchers were able to observe the unique neural activity of the ENS, which could help further our understanding of the brain-gut connection. “The ENS and microbiome are critically intertwined and affect each other; aggravation in the gut can create symptoms of anxiety and depression—or vice versa,” Dr. Angle says. “The communication between these two systems can be greatly challenged when each triggers the other, leading to the exacerbation of conditions like IBS, IBD, depression, and anxiety.”

Red meat may be bad for your gut
You’ve probably heard that too much red meat isn’t great for your heart. Now, a study has highlighted the negative effects of red meat on your gut. “Among the more striking recent discoveries is what happens when certain gut bacteria consume nutrients that are found in red meat and other animal products,” Dr. Preidis says. “These gut bacteria produce a substance called TMAO [trimethylamine N-oxide], which can be detected in the bloodstream and can lead to cardiovascular diseases such as heart attacks and strokes.” Dr. Angle also stresses that the ways diet affects the gut microbiome are critical to overall health. “The organisms living in the gut use the nutritional byproducts of the food to produce digested materials that then go and play other roles in the body,” she says. Always keep an eye out for these health symptoms your gut is trying to tell you.

A healthy gut may help fight cancer
Research also suggests a good diet may help battle other diseases, including cancer. In a study recently presented at the American Association for Cancer Research meeting, scientists found that melanoma patients who ate a high-fiber diet were five times more likely to respond to an immunotherapy treatment. Other research previously suggested that a diverse gut microbiome would lead to a more favorable response to the treatment. “Imagine if you could increase the number of patients who benefit from immunotherapy through something as simple as dietary changes—that would be remarkable,” study author Christine Spencer, PhD, said in a statement. “This study does point to diet playing a role in immunotherapy response via the gut microbiome, and we hope these findings will spur more studies on this topic in the cancer research community.”
Gut bacteria could help stroke victims
The gut doesn’t just impact the brain: It appears the brain impacts the gut as well. A recent study in mice showed that strokes unfavorably altered their gut bacteria and intestinal tissue even a month after the event, which could weaken nutrition and compromise stroke recovery. The unbalanced gut bacteria could also have negative effects on the recovering brain’s function and behavior. “If it ends up being that the gut has an influence on the repair of the brain, maybe our stroke treatments shouldn’t just be focused on what we can do for the brain—maybe we need to think about what can we do for the gut,” said study author and graduate student Allison Brichacek of the West Virginia University School of Medicine in a statement.

Diet may treat diabetes
Is there anything the gut microbiome can’t treat? As Dr. Preidis explains, gut microbes produce beneficial short-chain fatty acids (SFCA) when they break down certain fibers, which might help people with diabetes. “Recently, a study enrolling diabetic patients found that consuming a specially designed fiber-containing diet increased numbers of SCFA-producing gut bacteria and improved signs of diabetes,” he says. On the flip side, “studies are linking low levels of certain molecules generated by bacteria in the gut to be risk factors for conditions like type 2 diabetes,” Dr. Angle says. “Meaning if you don’t have the right types of bacteria in the gut, you could be at elevated risk for serious conditions.”

Gut bacteria could treat PCOS
No one’s sure what causes polycystic ovarian syndrome (PCOS), a female endocrine condition marked by altered hormones and reproductive issues—and there is no cure. Previous research has found that the gut microbiome is less diverse in women with the condition; a new study suggests that mice with PCOS who were exposed to healthy gut microbes displayed a reduction in symptoms. “Our new results suggest that altering the gut microbiome via prebiotic or probiotic therapies may be a potential treatment option for PCOS,” study author Varykina Thackray, PhD, of the University of California San Diego School of Medicine, said in a statement. “Additional research is needed to understand how specific gut bacteria contribute to PCOS.” Diagnosing the condition can be tricky—these are the 8 signs of PCOS that every woman should know.
Antibiotics could change gut bacteria permanently
Although antibiotics are sometimes necessary to fight against infection, doctors know they can wipe out good bacteria, too. But a recent study from the UK found that this state of unbalance in the microbiome, called “dysbiosis,” could last for at least a year—or maybe even permanently. “It is important that the microbiome be balanced and not in a state of dysbiosis,” Dr. Angle says. “Dysbiosis can further skew the balance of healthy microbes, pushing people to a state of unhealthiness.” Although the exact effects of antibiotics on the gut microbiome aren’t yet known, the study authors note that these results do raise concerns about their use.

Gut bacteria may protect against food allergies
Certain gut bacteria may also aid in preventing or treating food allergies. A recent study found that mice given gut microbes from healthy infants were protected against an allergic reaction to cow’s milk; however, those given microbes from allergic infants had a bad reaction to the milk. “This study allows us to define a causal relationship and shows that the microbiota itself can dictate whether or not you get an allergic response,” study author Cathryn Nagler, PhD, of the University of Chicago, told UChicago Medicine’s website. The results could pave the way for new food allergy treatments utilizing certain gut bacteria. In addition, probiotics could be your best defense against spring allergies.

A healthy microbiome could calm inflammation
Another World Summit study found a pathway to explain how “good” gut bacteria helps control inflammation and fight inflammatory bowel disease (IBD): Healthy bacteria support proteins that block overactive immune cells—these cells attack healthy tissues and set up the inflammation that triggers symptoms. Also: “Clinical trials using probiotics have reported a variety of beneficial effects for individuals with various gut disorders, including inflammatory bowel disease,” Dr. Preidis says. But, “despite a growing body of research, defining a precise role for probiotics remains challenging. Nonetheless, it is likely that one day probiotics might have a well-defined role in the management of certain gut disorders.” If you’re looking to start a probiotics regimen now, here are the 13 probiotics brands nutritionists trust most.
