
Consider your options
Modern medicine isn’t perfect. Sometimes doctors prescribe medical interventions out of habit even though new evidence shows they’re not effective, too dangerous, or don’t always work. From scans and surgery to injections and medication, some treatments might not always be the best options. Ask questions and do your research before you consider these medical procedures.
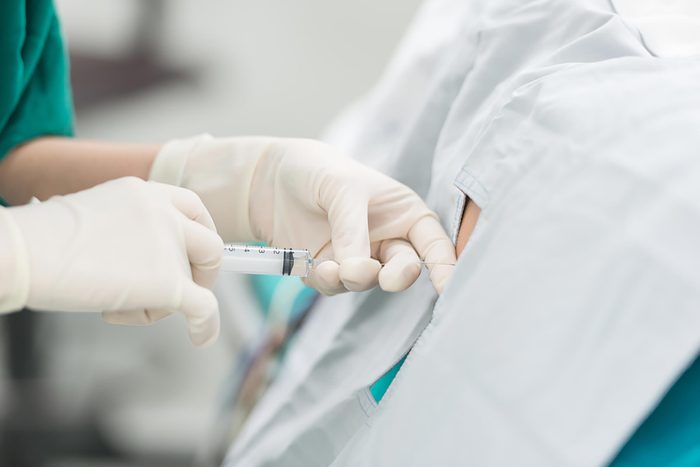
Epidural steroid injections for back pain
Epidural steroid injections for back pain may work short-term, but they have risky potential complications like neurological problems or paralysis. “Generally, epidural steroid injection isn’t very useful for treatment of chronic back or neck pain,” says Steven Severyn, MD, an anesthesiologist at the Ohio State University Wexner Medical Center. In addition, research has shown the injections haven’t reduced the number of back surgeries.
If the pain is caused by nerve issues (sciatica) instead of arthritis, “it will often relieve nerve inflammation causing the limb pain and allow time for naturally occurring improvement to take place,” Dr. Severyn says. However, the injection’s usefulness is still only short-term. Other treatments for back pain, such as physical therapy, can be a better plan for long-term improvement. (Don’t miss these medical procedures and treatments you can do at home.)
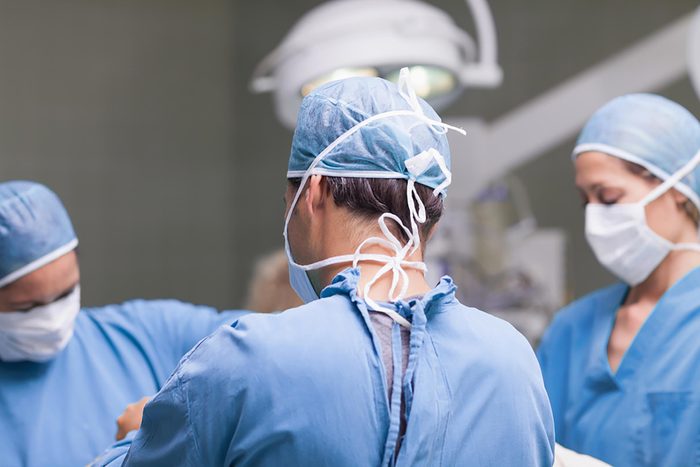
Back surgery
Unfortunately, surgery for back pain isn’t always a good option either. For some conditions, says Dr. Severyn, it can be helpful: spinal instability; loss of limb, bowel, or bladder motor functions; spinal infection; and other severe issues. But, back surgery shouldn’t be an option for chronic lower back pain, he says. And even when surgery is indicated, surgeons are using unnecessarily complicated procedures, suggests a 2016 study published in The New England Journal of Medicine. In the randomized trial, patients with spinal stenosis got either a simple procedure called decompression, which relieved pressure on the nerves, or they underwent decompression with spinal fusion, in which adjacent vertebrae are screwed together to give the spine more stability. (Spinal stenosis is a narrowing of the spinal canal that can put pressure on nerves and cause severe pain.) The study found that the outcomes in both patients were the same, but the spinal fusion patients had a greater risk of bleeding.
Before rushing to surgery, Dr. Severyn says, “find a physician who has experience, a broad comprehensive perspective, and a lot of treatment resources.” And unless it’s an emergency, get a second opinion before saying yes to back surgery.
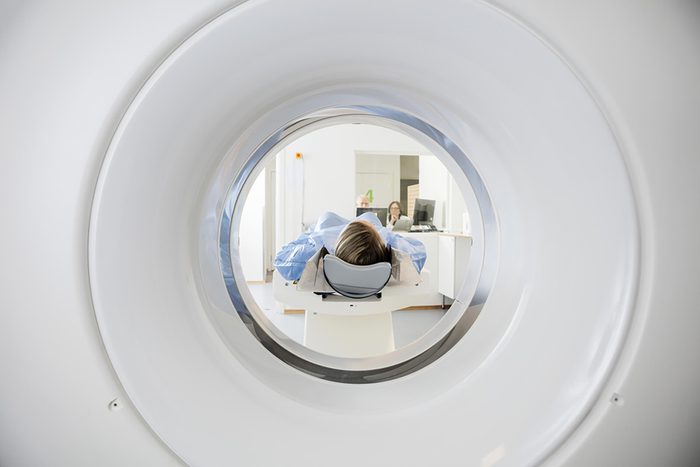
CT scans
If a doctor says you need a CT scan, ask questions before rushing to radiology. Studies have shown that radiation from CT scans could be responsible for as many as 2 percent of all cancers in the U.S. The procedure may contain as much radiation as 100 to 800 chest x-rays, according to the Environmental Protection Agency (EPA). The Food and Drug Administration (FDA) notes that between 10 and 30 percent of pediatric CT scans, and up to 50 percent of all imaging tests, are unnecessary.
Although they don’t always look for the same thing, could the much safer MRI be a better choice when appropriate? “CT scans are much quicker and tend to be less costly than an MRI, but does have the added radiation that MRI’s lack,” says Todd Sontag, DO, a family medicine physician with Orlando Health. “Ultimately, what’s ordered should be based on what will give the provider the most information on what pathology they suspect. Many times, the question is, does any imaging even need to be ordered?” Here are some of the medical tests and procedures doctors never waste money on.
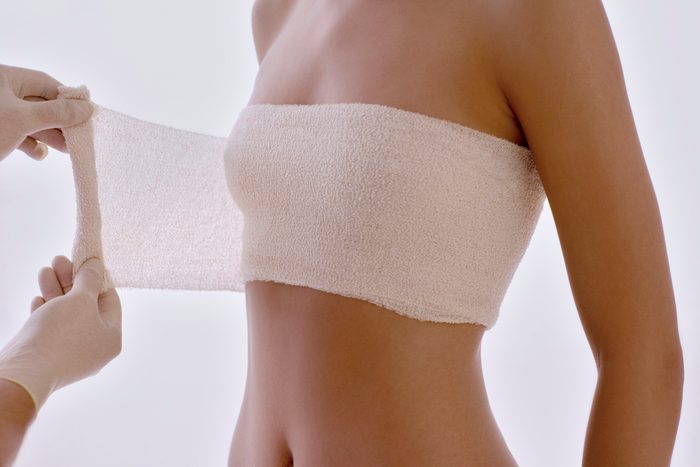
Breast reconstruction
Reconstruction after a mastectomy is a wonderful option for some women, but a small study published in JAMA Surgery indicates that many don’t fully understand the procedure before they have it—leading the researchers to suspect over-treatment. “We found that only 43 percent of patients had treatment that was consistent with their preferences and had adequate knowledge [about the procedure], which we found concerning,” study author Clara Lee, MD, a breast reconstruction surgeon at The Ohio State University Comprehensive Cancer Center—Arthur G. James Cancer Hospital and Richard J. Solove Research Institute, said in a statement. “I think this means that patients and doctors aren’t making ideal decisions about breast reconstruction.” Patients need to be fully informed about the risks, the recovery time, and the number of procedures before they can make an accurate decision about reconstruction, she says. Learn more about the 45 secrets surgeons won’t tell you.

Circumcision
In years past, it was common practice in the U.S. for a pediatrician to snip off the foreskin of penises in male babies. But recently, parents are questioning whether the practice is done more out of tradition than for medical reasons. Because of this, “there is no widespread recommendation for universal circumcision,” Dr. Sontag says. Although certain benefits, such as the prevention of urinary tract infections, sexually transmitted infections, and penile cancer, have been linked to the procedure, the risks are relatively low. “To put this in perspective of how effective it is at prevention, about 200 circumcisions are needed to be performed to prevent one hospitalized infant due to a urinary infection; and to prevent one case of penile cancer, approximately 300,000 circumcisions need to be performed,” Dr. Sontag says.
On the other hand, babies may experience some pain and bleeding during the surgery, but major complications, including infection and surgical error, are also rare. As the topic continues to be hotly debated among the medical community, just remember it isn’t a necessary procedure, but a personal choice. “There are enough benefits to warrant the circumcision for some [parents], and not enough benefits to warrant the circumcision for others,” Dr. Sontag says.
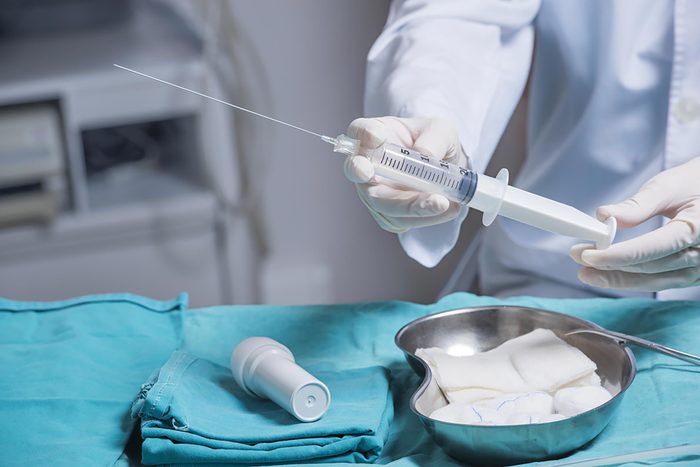
Amniocentesis
Although amnios aren’t routinely given to pregnant women, you may be offered one if blood tests or ultrasounds show worrying results. “Amniocentesis is still the only way to know 100 percent the information on the baby’s chromosomes and to detect smaller gene changes that may lead to disease,” says Clara Ward, MD, a maternal-fetal medicine specialist at McGovern Medical School at UTHealth and Children’s Memorial Hermann Hospital in Houston. In the procedure, a needle is inserted into the amniotic sac and fluid is withdrawn to test for genetic issues. Although reports of miscarriage rates vary, studies estimate the risk to be 1 in 300 to 500. “While amniocentesis may be safer than you think, it is not a necessary procedure,” Dr. Ward says. There are other, less invasive tests that help avoid amnios today, she says, so it’s important to remember that you can refuse the procedure if it’s offered to you.

Antibiotics
When they get a cold, the first thing some people do is ask the doctor for antibiotics—but that is likely a mistake. “Most patients that are prescribed antibiotics typically don’t even need them,” says Dr. Sontag. The reason is that most colds, sinus, and upper respiratory infections are caused by viruses, and antibiotics only works against bacteria. “About 95 percent of sinus infections are viral—therefore only about one in 20 will typically need an antibiotic,” Dr. Sontag says. The Centers for Disease Control and Prevention (CDC) estimates nearly a third of antibiotics aren’t necessary for all causes. Doctors end up giving patients what they ask for in order to keep them satisfied, and then when the cold clears up in a few days people think the meds worked—when in reality the cold simply ran its course.
Overprescribing these drugs is having major consequences. “Because antibiotics have been so widely used unnecessarily, now we are faced with bacteria that have become resistant to many antibiotics,” Dr. Sontag says. “As resistance builds, we are faced with less and less options to treat infections when they genuinely need antibiotics.” In addition, unnecessary antibiotics can wipe out the good bacteria in your gut, causing a serious infection called Clostridium difficile colitis, or C. diff. Here are the medical tips doctors and nurses wish you knew.
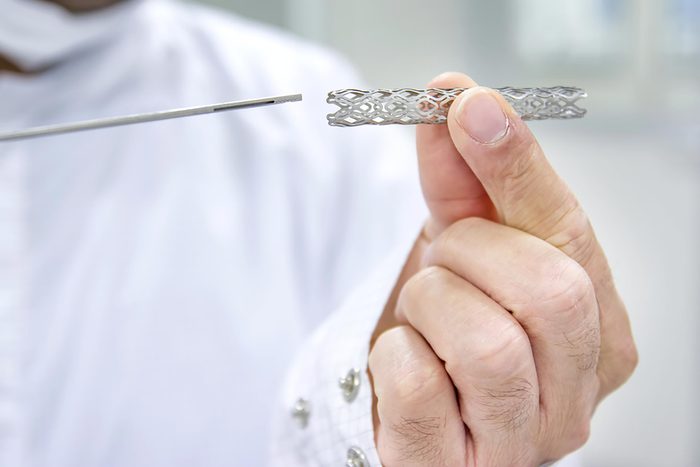
Stents
In emergency situations, putting in a stent to open up a person’s clogged artery can save a life. But they may be overused in preventative ways. “It can be hard to believe if you find a severely blocked artery in a patient’s heart that the patient is better off with the artery remaining blocked,” says Quinn Capers, IV, MD, a specialist in cardiovascular medicine at The Ohio State University Wexner Medical Center. “Studies show that, in stable coronary artery disease in patients without strong evidence that the blockage is slowing blood flow to the heart, medication can be just as effective.”
Research has found that stents aren’t effective at preventing future heart attacks and death in stable patients, because where the stent is placed might not be the spot that causes the problem down the line. Plus, the surgery carries risks. But, Dr. Capers notes that stents do provide patients with relief of daily chest pain, and if used, should be part of a broad treatment plan that also includes medications, exercise, healthy diet, and reduced stress levels.
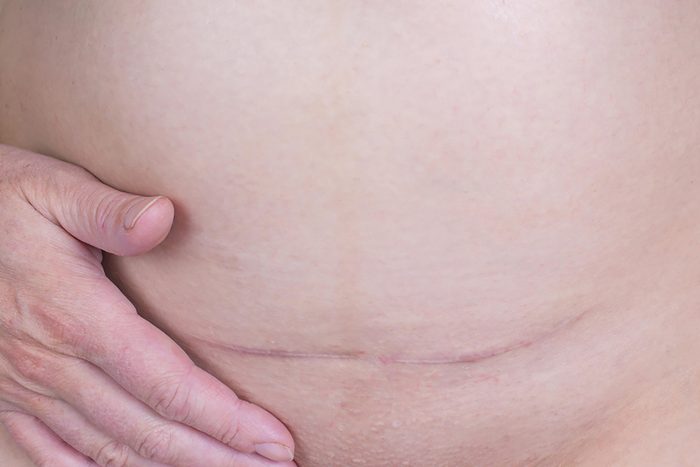
C-sections
The C-section rate in the U.S. is around 32 percent according to the CDC, much higher than the 15 percent the World Health Organization recommends. Although it is a common procedure, it is major surgery that can lead to serious maternal complications like infection, hemorrhage, sepsis, and death—so it’s not a good idea to have one if you don’t need one. Recommendations from the American College of Obstetricians and Gynecologists (ACOG) aim to curb the C-section rate, and ACOG also suggests a more hands-off approach during labor to help avoid unnecessary surgery.
“Part of this trend has included doctors researching the way labor progresses, and allowing more time for the cervix to change,” Dr. Ward says. Also, try to avoid being induced, which produces intense contractions that may put baby in distress, leading to a C-section. Don’t believe that you need one because of the baby’s weight, which is often overestimated. And if your baby is breech, ask about a manipulation to move the baby called an external cephalic version (this has its own risks, but they are minimal, Dr. Ward says). And if you’ve had a C-section before, don’t assume you need one again. “If you have had a C-section before, you may be a good candidate for VBAC—vaginal birth after cesarean,” she says.
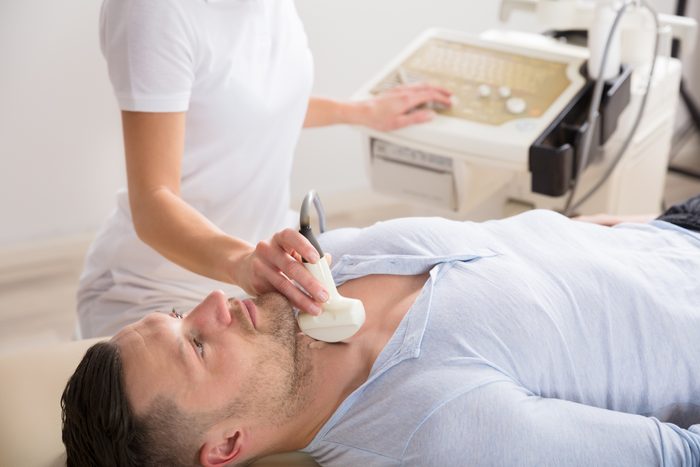
Thyroid screening and surgery
If you’ve heard some groups calling for routine thyroid cancer screening, don’t listen to them. These ultrasounds can lead to unnecessary biopsies and even thyroid removal—all for small cancerous nodules that probably wouldn’t have grown at all. “We have learned a lot from both the Japanese experience and the South Korean experience,” says Jennifer Sipos, MD, a thyroid cancer specialist at The Ohio State University Wexner Medical Center. South Korea made routine thyroid screenings part of their national healthcare. They found and removed a lot of cancers, but the mortality rate from thyroid cancer didn’t decrease. In Japan, doctors biopsied many thyroid tumors, but didn’t operate—and discovered they didn’t grow over time. Plus, “as many as 10 to 15 percent of people may have small thyroid cancers that are diagnosed at autopsy [when thyroid cancer was not the cause of death],” Dr. Sipos says.
Much of this information appears to indicate these tumors don’t need surgery. “This suggests we shouldn’t be looking for these small cancers, because if we do, we’re going to find them,” Dr. Sipos says. Research has shown that complication rates from thyroid cancer are high, and include potential damage to your voice, she says. And even if removing your thyroid goes well, you’ll still need to take thyroid hormones for the rest of your life—all for a “cancer” that wasn’t causing any harm to begin with.
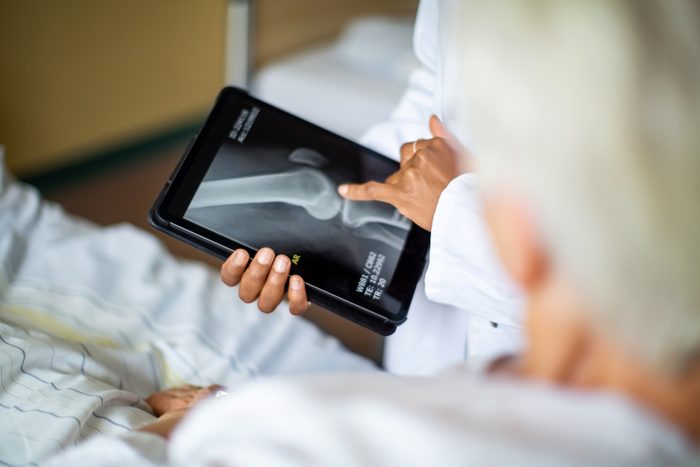
Arthroscopic knee surgery
Researchers now think that a common knee surgery is being performed more frequently than it should be on patients who aren’t going to benefit. “An area of concern recently is performing meniscus resection on arthritic knees,” says Christopher Kaeding, MD, orthopedic surgeon at The Ohio State University Wexner Medical Center. The procedure is performed arthroscopically in which small incisions are used to repair the torn meniscus. It isn’t effective on people whose tears develop from wear and aging, common in patients with arthritis.
A Finnish study published in The New England Journal of Medicine found that this surgery was just as effective as “fake” surgery (a placebo group in which an incision was made, but no surgery performed) in helping people’s knees feel better. Other research has shown that surgery for arthritis is no more effective than physical therapy and medication. “Doing arthroscopy on a knee with significant arthritis and a meniscus tear to address the meniscus tear is likely to not be effective, if it is the arthritic process that is causing the pain and disability,” Dr. Keading says. (Don’t miss these secrets hospitals aren’t telling you.)

Prostate cancer screening and surgery
Another hotly debated medical decision is whether and when to routinely screen men for prostate cancer, which could lead to invasive biopsies and surgery. As with thyroid cancer, some prostate cancers are non-aggressive and slow-growing, and surgery to remove them could cause unwanted side effects. “I personally recommend screening with PSA [blood test] and digital rectal exam starting at age 50, and earlier for men at risk due to symptoms or a strong family history of prostate cancer,” says Steven Clinton, MD, PhD, a genitourinary medical oncologist and researcher with the Ohio State University Comprehensive Cancer Center—Arthur G. James Cancer Hospital and Richard J. Solove Research Institute. The problem is the “inconsistency regarding how doctors use the laboratory tests and physical findings to advise the patient,” he says. “Our for-profit health cancer system incentivizes aggressive and lucrative treatment plans that for many men may not be necessary.” Instead, he says, “active surveillance” can be used to monitor the cancer, avoiding unnecessary surgery that has risks of incontinence and sexual dysfunction.
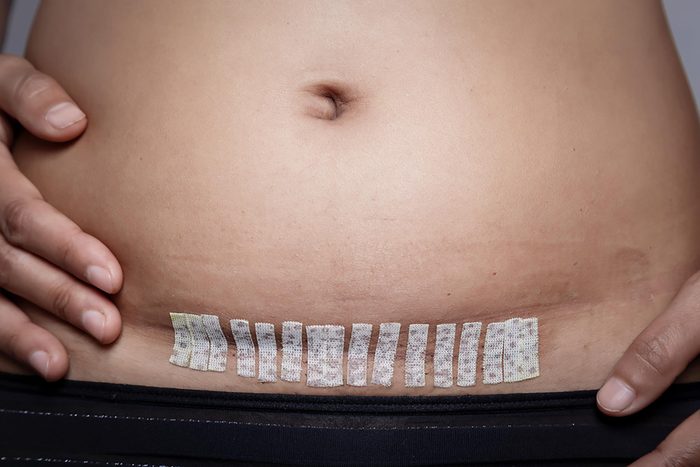
Hysterectomy
It used to be that the only treatment for painful fibroids and the heavy vaginal bleeding they bring was hysterectomy, but that’s not the case anymore. “While the only way to ensure that they don’t cause any problems is to take out the uterus, a procedure known as a hysterectomy, there are medications and less invasive procedures that may offer substantial improvement in symptoms and quality of life without the risk of a big surgery,” Dr. Ward says. “Uterine artery embolization is a newer technique which blocks the blood supply to the fibroids causing them to break down, thus relieving the symptoms.”
A study in the American Journal of Obstetrics and Gynecology found that two-thirds of embolization patients can avoid a hysterectomy. Not everyone is a candidate for this simpler procedure depending on how many fibroids you have and where they are. It’s also been associated with pregnancy complications, so women of child-bearing age should discuss options with their doctor. Of course, hysterectomy is a permanent removal of fertility and a major operation—and if the ovaries are removed, too, a woman will need to take hormones until the age of natural menopause in order to prevent risks to her heart and bones.

HRT in post-menopausal women
Speaking of hormone replacement therapy (HRT), prescribing hormones used to be common for women in order to avoid the unpleasant side effects of menopause: hot flashes, vaginal dryness, irritability, and trouble sleeping—not to mention possible benefits of estrogen for the heart and bones. But a review of research published in Mayo Clinic Proceedings found HRT intended to improved cardiovascular health in postmenopausal women actually made it worse. There is also a link to stroke and some cancers, although HRT isn’t quite as dangerous as the 2002 Women’s Health Initiative found. But it’s still a good idea to take it for the shortest amount of time possible. “Depending on your personal and family health history, the risks may outweigh the potential benefits,” Dr. Ward says. She suggests some alternative therapies, like topical creams and even antidepressants. Next up: Here’s what your doctor is really thinking—but isn’t saying to your face.
