Are Measles Coming Back? What You Need to Know
Updated: Mar. 17, 2023
Measles are so last century, right? You might think no one actually gets them anymore, but recent outbreaks suggest otherwise.
 It’s been 17 years since measles were officially eliminated from the U.S., but the term “measles outbreak” has just recently gained steam. With cases spiking in Minnesota, Nebraska, and Michigan, it seems the once ubiquitous disease—a virus that causes rash, pneumonia, dehydration, and occasional encephalitis (infection of the brain)—is making a comeback. But how?
It’s been 17 years since measles were officially eliminated from the U.S., but the term “measles outbreak” has just recently gained steam. With cases spiking in Minnesota, Nebraska, and Michigan, it seems the once ubiquitous disease—a virus that causes rash, pneumonia, dehydration, and occasional encephalitis (infection of the brain)—is making a comeback. But how?
Paul A. Offit, an American pediatrician specializing in infectious diseases and an expert on vaccines, immunology, and virology, points a finger at the growing anti-vaccination movement. “We eliminated measles from the U.S. in 2000, so the reason we’re seeing outbreaks now is that a critical number of parents have chosen not to vaccinate their children. We can protect ourselves and our children by making sure that our vaccines are up to date.” (These are the vaccine myths you can safely ignore.)
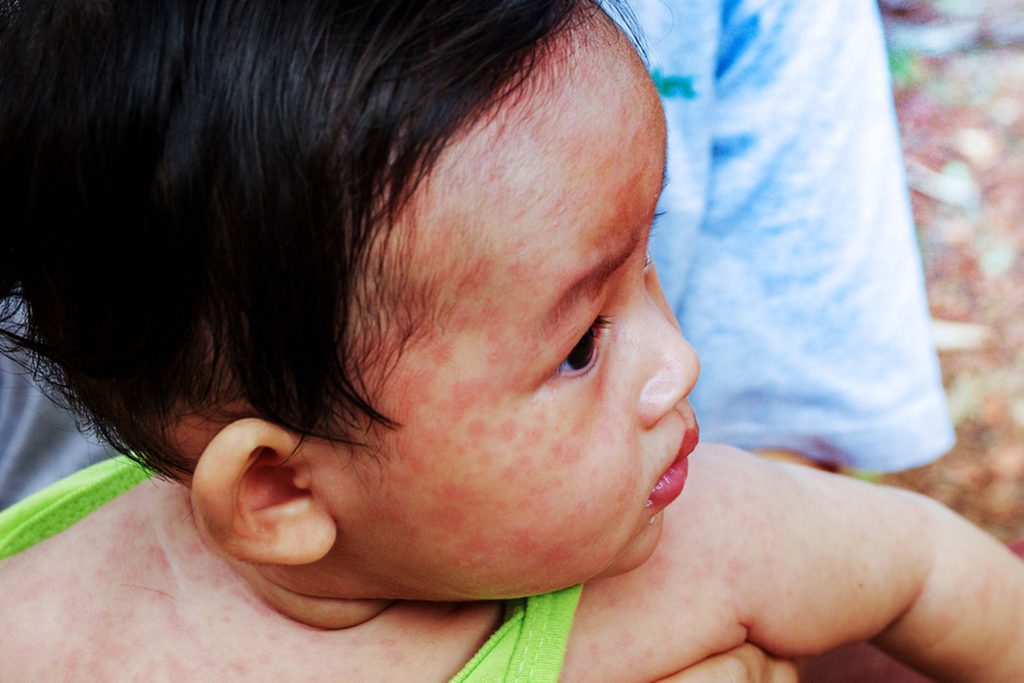
It may be strange to even consider measles making a comeback, especially if you were born after 1968, when there were essentially no signs of it. But now that it’s reappeared, it’s spreading fast. That’s because measles is an extremely contagious disease, caused by a virus from the paramyxovirus family, that spreads by air. Symptoms include fever and coughing and an infamous rash of small red dots. Most people recover within two to three weeks, with symptoms peaking one to two weeks after infection. But approximately 30 percent of measles patients suffer additional complications, including diarrhea, pneumonia, brain inflammation, and permanent blindness.
A vaccine to protect against measles was developed in the 1960s, and widespread vaccinations soon followed. In 2001, the Measles Initiative was launched by the American Red Cross, the United Nations Foundation, the U.S. Centers for Disease Control and Prevention, UNICEF and the World Health Organization, which led to a global decrease in measles cases. In 2008 and on, however, vaccination campaigns took a hit due to funding cutbacks, which has enabled the extremely contagious disease to resurface.
Getting measles may not sound like the biggest disease epidemic to worry about, but look at it this way: From 1989 to 1991, measles made a massive comeback due to people not getting vaccinated enough, and from 2000 to 2012, the measles vaccine saved about 13.8 million lives.
The measles vaccine prevents 97 percent of cases if you get the recommended two doses, and one dose covers you 93 percent of the time. However, you can lose your immunity over time, or the vaccine may simply not be strong enough the first time around. Getting a vaccine doesn’t guarantee immunity, which is why, if you’re concerned, you should get your blood checked for antibodies against the measles vaccine to ensure that it worked. A vaccine not being perfect is certainly no reason not to get it, though. It’s will cut your risk dramatically, which, in turn, will cut others’ risk as well.














