How to Use an Inhaler According to Breathing Experts
Updated: Jun. 22, 2021
Inhalers are commonly used to treat asthma and other lung conditions, but you need to use them correctly for them to be effective.
A breath of fresh air
Inhalers are one way to get medication to your lungs so your airways stay open and you can breathe easier. The devices are most commonly used for asthma, but can also be helpful for people with chronic obstructive pulmonary disease (COPD), emphysema, chronic bronchitis, and other lung conditions.
Some inhalers help nip an asthma attack (or other symptoms) in the bud, while others help control your condition and prevent problems over the long-term.
This is what you need to know about these small, life-saving devices.

What is an inhaler?
The inhaler itself is a handheld device with a mouthpiece, and can usually fit into your pocket or purse. The contents (the medication) are pressurized so the canister emits a spray of medicine through the mouthpiece when you press it.
Metered-dose inhalers (MDIs), also called “puffers,” are a common type of inhaler.
While using an inhaler may seem like a simple matter, they actually require some skill to operate.
“The inhaler is only as good as the technique,” says Gary Stadtmauer, MD, an allergy and asthma specialist in New York City who is affiliated with Mount Sinai Medical Center. “You have to be sure you’re using it correctly.”
Types of inhalers
Not only are there different types of inhalers, but there are also different types of asthmatics, Dr. Stadtmauer says. Picking the right inhaler for the person has a lot to do with lung function and the frequency and severity of symptoms, he adds.
“Rescue” inhalers deliver the medication quickly, but the effects don’t last very long. “They are purely for as-needed use,” Dr. Stadtmauer says. “All they do is temporarily open up the airways. It’s a temporary fix.” These can be helpful for someone who has mild asthma with occasional flare-ups—for example, asthma that is only triggered by exercise or cold air.
Most people with asthma need additional medications in the form of controller inhalers. These are used daily to help control asthma, and each dose lasts longer. “Controller devices have gotten so good that you can now take a single puff of medication of an inhaler and that will last for a whole 24 hours,” Dr. Stadtmauer says.
Medications
A rescue inhaler typically contains a bronchodilator. “They dilate the bronchial tubes, which are the fine branches that go into the deepest areas of the lung,” Dr. Stadtmauer explains. Albuterol is one well-known bronchodilator.
Controller or maintenance inhalers typically contain a low-dose anti-inflammatory steroid and sometimes a long-acting form of a bronchial dilator, he adds.
One advantage of inhalers over, say, nebulizers (which can deliver medications for asthma and other conditions via a mist) is that you can combine two and sometimes even three medications in one device.
Types of devices
The most common inhaler device is the MDI, which sprays a pre-set amount of medicine through the mouth to the airways.
The mechanism is simple: You depress the device and it issues a spray. “There is a manual component so patients have to coordinate the spray with the breath,” Dr. Stadtmauer says. Not everyone does that well.
There are also dry powder inhalers, which deliver the medication in powdered form. The medication gets to your airways when you take in a deep, fast breath from the inhaler.
“The medication is released when the person starts to take a deep breath,” Dr. Stadtmauer says. “There are many reasons that is a better choice for people because there’s no concern about coordination.”
How to use an inhaler
Inhalers can be tricky to use correctly, so always check the instructions for the particular model you have. Even better, since directions can be cumbersome, don’t be afraid to ask your health care provider for guidance. Getting the right technique is important.
“You have to coordinate your inhalation with the spritz,” says Len Horovitz, MD, a pulmonary specialist at Lenox Hill Hospital in New York City. “If you just open your mouth and spray, it’s mouthwash. It requires a little bit of coordination.”
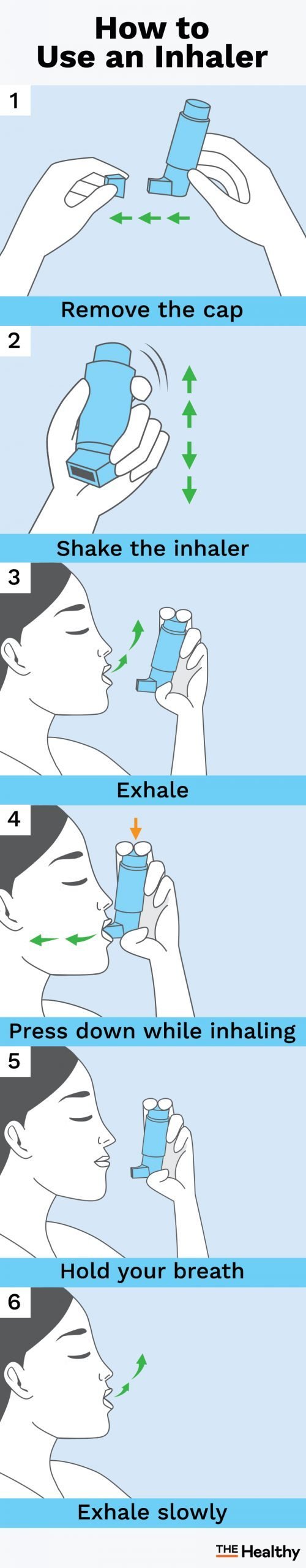
Here are the general steps for using an inhaler. You should be standing up or sitting straight.
- Remove the cap and make sure there’s nothing blocking the mouthpiece.
- Shake the inhaler several times.
- If you haven’t used it in the last three days, “prime” the inhaler by depressing once to make sure it sprays.
- Exhale out as much as you can then, with the mouthpiece pointed down, close your lips around it.
- Press down on the inhaler once while you inhale.
- If you can, hold your breath while counting to 10.
- Breathe out slowly.
Put the cap back on, then rinse your mouth with water and spit it out. There’s no specific way you’re supposed to feel after using the inhaler, Dr. Stadtmauer says. And don’t share inhalers—especially in the age of Covid-19.
If your prescription calls for two puffs (and many do), wait a minute between each. A 2019 study in the Journal of Allergy and Clinical Immunology reported that two-thirds of patients only separated their inhalations by 15 seconds or less, and only 16 percent reached the acceptable time of 30 seconds and above.
Small children, seniors, and anyone who is frail or has muscle issues may have trouble with an inhaler. Nebulizers, which also deliver medication to your lungs, can be easier.
(These fun nebulizers for kids can make treatment a little easier.)
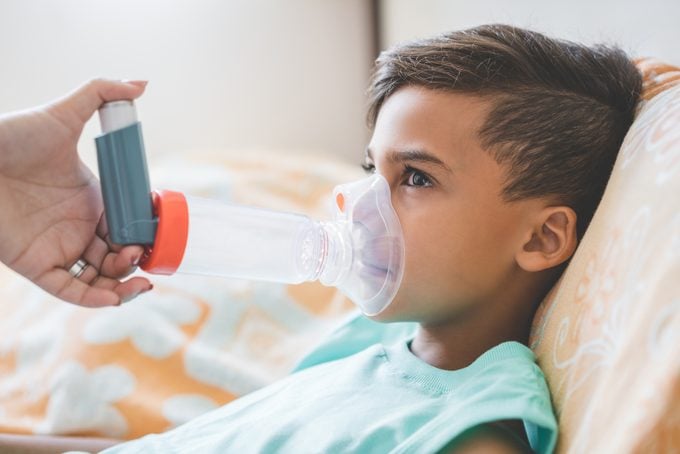
Spacers
A spacer can make it easier to use an MDI, and many doctors recommend them. This is an attachment that helps ensure the medication gets to your lungs, where it’s needed, rather than being waylaid in your mouth or throat. The spacer is a longish tube that holds the medication before it goes into your mouth. It’s larger than the actual inhaler.
Connect your inhaler with the opening in the spacer, then shake the inhaler for 10 seconds. Once your mouth is closed around the spacer, depress the inhaler once. This moves the medication from the inhaler into the spacer and then your lungs. Many hospitals also have good videos demonstrating how to use both inhalers and spacers.

Dry powder inhalers
Dry powder inhalers (DPIs) are easier to use than MDIs because, rather than timing the release of medication from the inhaler with your inhalation, a DPI automatically releases the medication in powder form when you take a sudden, deep breath. In this case, it’s less the coordination than the correct inhalation technique to activate the mechanism.
“The medication is released when a person starts to take a deep breath,” Dr. Stadtmauer says. “There are many reasons that is a better choice for people because there’s no concern about coordination.”
The basic technique is similar to that for an MDI, except you have to load the medicine yourself (read the manufacturer’s instructions). After that, take a deep breath in and out, put the mouthpiece in your mouth, sealing your lips around it. Hold your breath while counting to 10. If you need a second dose, wait one minute in between. Rinse and spit after, and wipe the mouthpiece weekly with a dry cloth. Avoid putting the device in water.
How long do inhalers last?
That depends on the specific product and on what you’re using it for.
Metered-dose inhalers come with a preset number of puffs, which is usually indicated on the label. Often these inhalers have a counter on the packaging that will tell you how much is left, but you can also keep track yourself. Just divide the total number of puffs in the canister by how many puffs you take during an average day.
Predicting when an inhaler will run out is easier for controller medications, which have a more predictable prescribing pattern, than for rescue inhalers.
Maintain your MDI by rinsing the mouthpiece and cap every week then air-drying it. Different models have different instructions, so check the directions for specific information.
Dry powder inhalers can last from weeks to years, depending on the make. Check the packaging for correct storage information.



