Do you need genetic testing for breast cancer?
Certain gene mutations increase the risk of breast cancer. That’s why your doctor might refer you to a genetic counselor to see if genetic testing is a good option for you as it might not be a fit for everyone. Here’s everything doctors wish you knew.
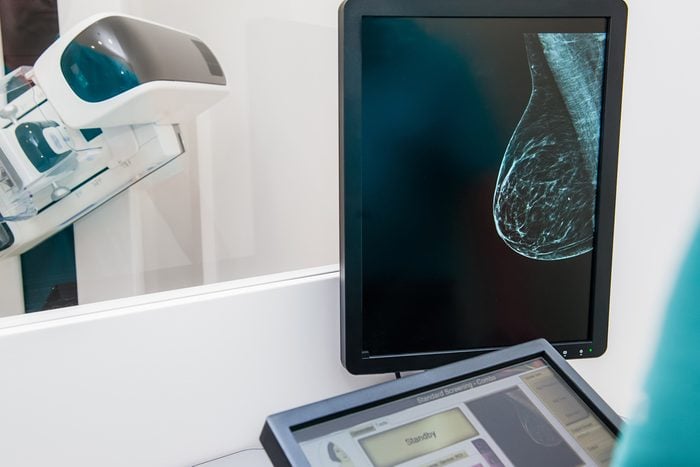
Most breast cancer isn’t inherited
Most cases of breast cancer don’t have a genetic link, according to surgeon Ali Cheaito, MD. As far as researchers can tell, only 5 to 10 percent of breast cancers fall into the inherited category. Another thing to keep in mind is that a positive genetic test doesn’t mean you will get breast cancer; likewise, a negative result doesn’t mean you won’t get it. That’s why it’s a good idea to take precautions to reduce your risk of breast cancer. Genetic testing can only reveal whether you are at an elevated risk for certain kinds of cancer.

The genetic links are growing
Genetic testing for breast cancer used to mean looking for mutations on the BRCA genes, but researchers have identified many more genes in the last couple of decades, and mutations in any of them could raise your risk of breast cancer, according to Susan G. Komen Breast Cancer Foundation. These include:
- ATM
- BARD1
- CDH1
- CHEK2
- NBN
- NF1
- PALB2
- PTEN
- RAD51D
- STK11
- TP53 (p53)
And researchers expect to discover even more.

Testing can identify other cancers, as well
Since the mid-1990s, cancer doctors have known that women who test positive for a mutation to a BRCA gene are at a higher risk of developing breast cancer. But it’s not just breast cancer. Ovarian cancer is also associated with mutations to the BRCA genes. And over the years, scientists have come to understand that genetic mutations are also associated with a higher risk for developing certain other kinds of cancers, explains genetic counselor Maggie McDuffee. These include prostate, fallopian tube, colorectal, peritoneal, and pancreatic cancers.

“Hereditary cancers” are different from “sporadic cancers”
When cancer occurs because of a known inherited gene mutation, it’s referred to as “hereditary cancer,” according to Facing Our Risk Of Cancer Empowered (FORCE). Other cases are called “sporadic cancer.” The distinction matters because statistically hereditary cancers present differently from sporadic cancers. For example, some hereditary cancers tend to present at younger ages than sporadic cancers. Some tend to be more aggressive, and some are more (or less) responsive to certain types of therapies. And having had one hereditary cancer may put you at a greater risk for certain other types of cancers that are also inherited. (That’s why you should learn the signs of breast cancer you might not recognize.)

Certain groups are more likely to carry a mutation
The mutations that cause inherited breast cancer turn up in about 1 in every 40 Ashkenazi Jewish women, according to the Centers for Disease Control and Prevention (CDC). That makes these women about 10 times more likely to carry a mutation than the general population, and those with the mutation have a 75 percent greater risk of developing breast cancer. But you don’t have to be Jewish to carry the mutation. The cancer-predisposing mutations are present in other ethnic groups, including people with Latin American and Caribbean heritage.

Who should get tested
“Having cancer predisposition testing can be very empowering, as there are a lot of actions we can take to prevent cancer if we learn that we are at high risk for it,” McDuffee says. “For instance, we can pursue earlier and/or more frequent screenings, take medications that reduce risk, make lifestyle changes, and even consider preventive surgeries in certain situations.” Some research, including a clinical trial in Breast Cancer Research and Treatment, indicates that women who undergo genetic testing for breast cancer report a high level of satisfaction—and few regrets.

Who can skip genetic testing
Since hereditary breast cancer tends to be rare, genetic testing for breast cancer isn’t recommended for everyone. Genetic counselors like McDuffee can help you decide if you’re someone who could benefit from it. But generally speaking, you probably wouldn’t even consider testing unless you’ve already been diagnosed with cancer, you have a family history of breast, ovarian, pancreatic or high-grade prostate cancer, or you have a family member who has tested positive for a mutation, notes Roshni Rao, MD, chief of the division of breast surgery at New-York Presbyterian Hospital and Columbia University Medical Center.

More doctors believe diagnosed patients should be tested
In recent years, more doctors have been recommending that breast cancer patients get genetic testing, according to Dr. Rao. The American Society of Breast Surgeons issued “consensus guidelines” in 2019 recommending that genetic testing be offered to all patients newly diagnosed with breast cancer. The goal of testing is to help determine treatment as well as future screening tests. Another advantage to testing: If a patient has a mutation, his or her relatives may want to be tested, according to surgical oncologist, Peter Beitsch, MD.

You can inherit a mutation from your father
Many of the doctors and genetic specialists we consulted shared their concern that there’s a misconception that only the mother’s side matters. You have to take into account both sides of the family when considering family history, says Dr. Rao. (Here are 15 other breast cancer myths and misconceptions.)

Men can get breast and other inherited cancers
Men also can benefit from genetic testing for cancer predisposition, McDuffee points out. Some of the gene mutations mean you have an increased risk of prostate, pancreatic, and other types of cancer that are common in men. They also can mean an increased risk of breast cancer for men. Breast cancer in men isn’t common, but it occurs.

Testing positive doesn’t mean you’ll get cancer
McDuffee and other experts emphasize that just because you test positive for a mutation doesn’t mean you will get cancer. “Based on the specific test result, the patient is often able to be given a risk percentage to develop breast cancer during his or her lifetime.”
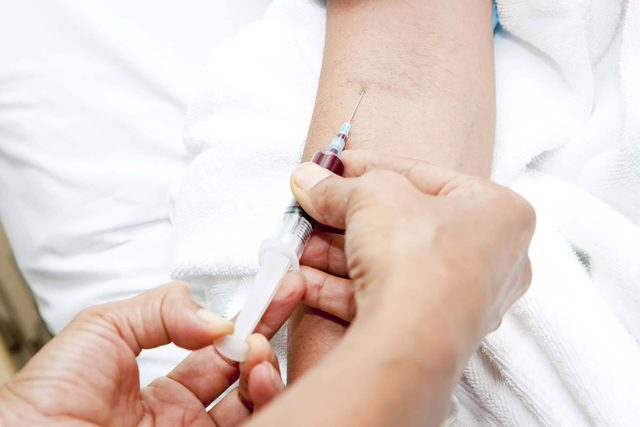
Genetic testing is a blood test
Genetic test is done through a simple blood draw. From there, you usually receive results in two to three weeks. But it’s important to have testing done through a genetic counselor or similarly qualified professional—for example, an oncologist who works directly with a genetic counselor—instead of a home DNA test. A positive result is an opportunity to make decisions, and only a genetic counselor or similarly qualified professional can help with that.
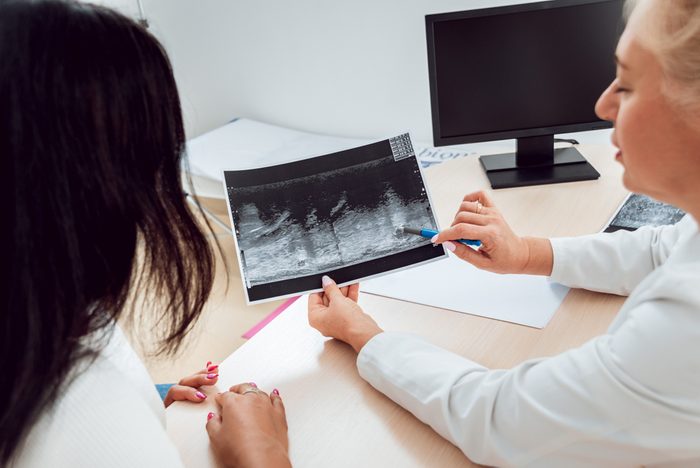
What genetic counselors do
Genetic counselors have earned an advanced degree or are certified in providing patients with customized cancer risk assessments, explains McDuffee. What they do includes:
- Gathering a complete personal and family health history
- Discussing the suitability of genetic testing
- Guiding the patient through testing options to make sure that they have the most appropriate and up-to-date testing available
- Explaining the risks, benefits, and limitations of genetic testing
- Making screening and other risk-reducing recommendations for patients and their families, based on national guidelines and current research.

Legal and financial cost
Some misconceptions around genetic testing for breast cancer are that the testing is expensive, insurance won’t cover it, and you’ll be denied insurance in the future based on the results. None of that is true. The price is about $300 (from $3,000 when it first began), and insurance will cover it if it’s considered medically necessary for people who meet certain criteria. A federal nondiscrimination law passed in 2008 stipulates that people can’t use the information gathered against you.

How to get started
If you’re interested in genetic testing for breast cancer and other cancers, start by asking your doctor for a referral to a genetic counselor. You can also visit the National Society of Genetic Counselors website to find a certified genetic counselor. You’re better off using a genetic counselor rather than testing at home, says immunologist, Tsvetelina Velikova, MD, because you’ll need to process and fully understand the results.

If you tested negative years ago, consider retesting
The medical and scientific knowledge about hereditary breast cancer and other hereditary cancers has grown dramatically over the past several decades. Genetic testing for breast cancer in the mid-1990s through the early 2000s only sought mutations of the BRCA genes. Now, the testing is much broader and can be far more informative. (To help with some of the uncertainty, learn these 25 things you think cause cancer but don’t.)
