
Myth: Breast cancer is the biggest cancer killer of women
“Lung cancer is the leading cancer killer in both men and women. So if you light up, quit smoking! Smoking is the leading cause of preventable cancer deaths.” —Colleen Doyle, RD, director of active living for The American Cancer Society in Atlanta. These are 13 things your breasts aren’t telling you.

Myth: You don’t need to do self-exams
“While self-exams don’t replace yearly checkups with your doctor, they’re still a good tool. The wisest thing is to know your body well. Don’t be afraid to examine yourself; embarrassment is a dangerous barrier. Notice if your breasts change in any way. Don’t hesitate to talk to your doctor about any concerns.” —Elizabeth Chabner Thompson, MD, founder of Best Friends For Life (BFFL)-Co in Scarsdale, New York. Breast self-exams are necessary. Here’s what to look out for.
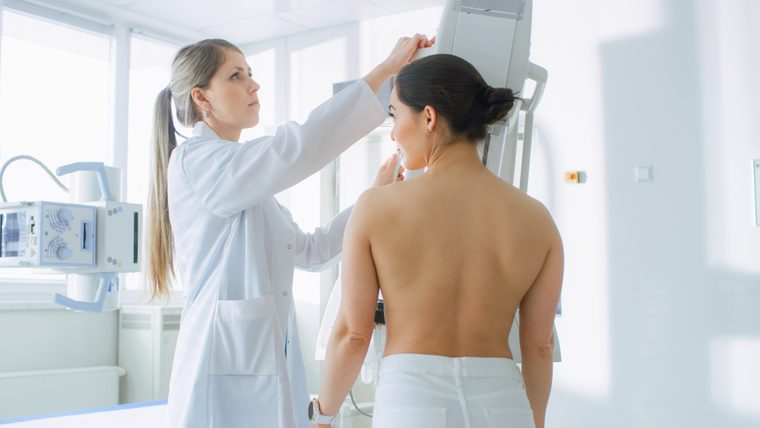
Myth: Mammograms can cause cancer
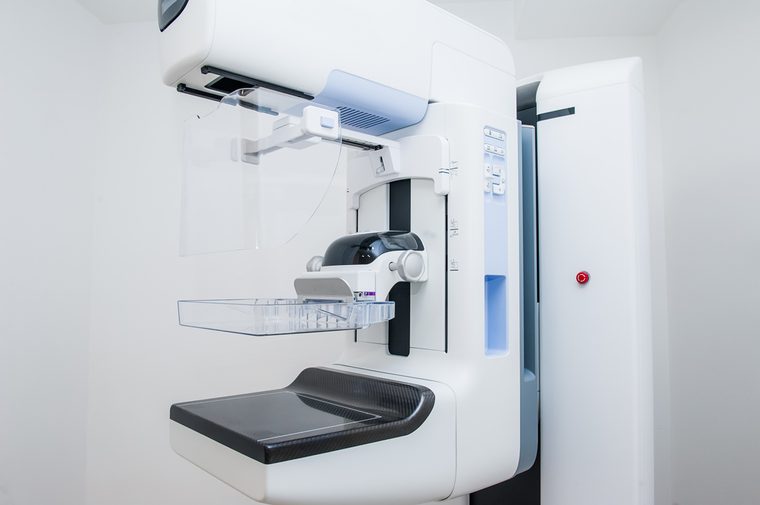
“It is true that women who receive large doses of radiation, especially when they are younger, have an increased risk of breast cancer but routine breast cancer screening with mammography uses a very small dose of radiation and poses very little risk for future breast cancer development. Mammography allows us to detect early-stage breast cancer, which in turn allows for early intervention and improvement in outcomes. This significantly outweighs the potential harm.” —Sean Fischer, MD, medical oncologist at Providence Saint John’s Health Center in Santa Monica.
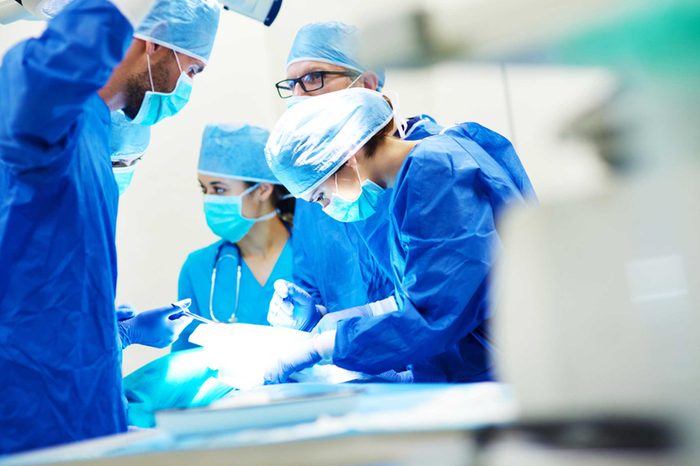
Myth: Removing a tumor spreads cancer
“There is no data that exposing a tumor to air or removing it spreads cancer to other places. If this were the case no one would undergo surgical procedures.” —Anton Bilchik, MD, chief of medicine and chief of gastrointestinal research at John Wayne Cancer Institute at Providence Saint John’s Health Center in Santa Monica, California.
Myth: A close family history of breast cancer means you’ll get it too
“Women who have a family history of breast cancer are placed into a higher risk category, but 90 percent of women diagnosed with breast cancer have no family history of breast cancer. If you have a first-degree relative (a mother, daughter, or sister) with breast cancer who developed breast cancer before the age of 50, you should start some form of regular diagnostic breast imaging 10 years before you become the age your relative was. If you have a second-degree relative with breast cancer (a grandmother or aunt) your risk increases only slightly.” —Sean Fischer, MD. These are common breast cancer symptoms that many women often ignore.

Myth: No family history? No need to worry
“Fewer than 10 percent of women have a genetic mutation causing their cancer, while the other 90 percent are considered to be sporadic, or not due to a gene mutation. In sporadic cases there often is no clear cause. Anyone can get breast cancer, regardless of family history, so make note of any changes and discuss them with your physician in a timely fashion.” —Preya Ananthakrishnan, MD, director of breast surgery at White Plains Hospital in New York.
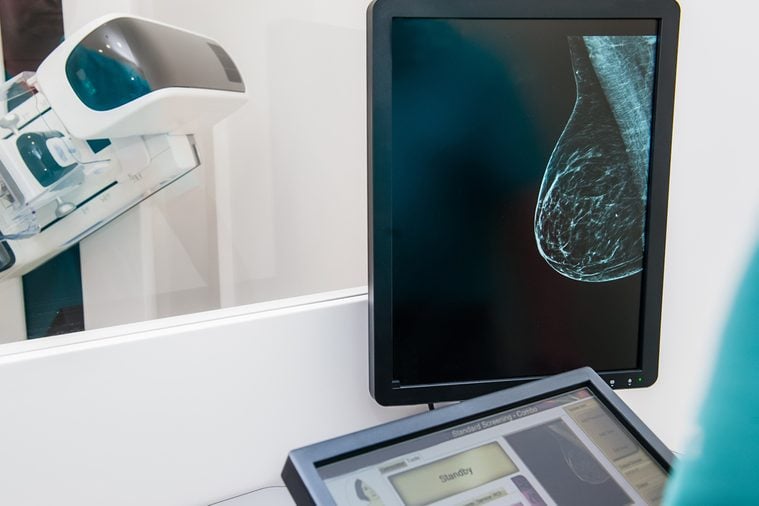
Myth: If you have breast cancer, symptoms will be obvious
“A breast mass is often not found by an exam. That is why mammography is very important in addition to what a woman may see or feel.” —Neelima Denduluri, MD, an oncologist at Virginia Cancer Specialists, with offices throughout Virginia.

Myth: Sugar can cause breast cancer
“The bottom line is sugar fuels all our cells, including cancer cells. So there’s nothing really specific about sugar directly causing breast cancer or if you already have breast cancer, sugar causing those cells to grow more or faster. But the issue is we eat a lot of sugar in this country and that is contributing to the overweight/obesity epidemic we’re seeing today, which does impact cancer risk.” —Colleen Doyle, MS, Boost breast health with these cancer-fighting foods.

Myth: Your bra can cause cancer
“This myth is primarily based on the notion that bras that are ill-fitting or tight-fitting or bras with an underwire decrease circulation of lymphatic fluid and may trap toxins in the breast tissue that can cause cancer. This correlation is false. Wearing an underwire bra does not increase your risk for breast cancer.” —Caroline Coombs-Skiles, MD, breast surgeon at the Austin Cancer Center in Texas.
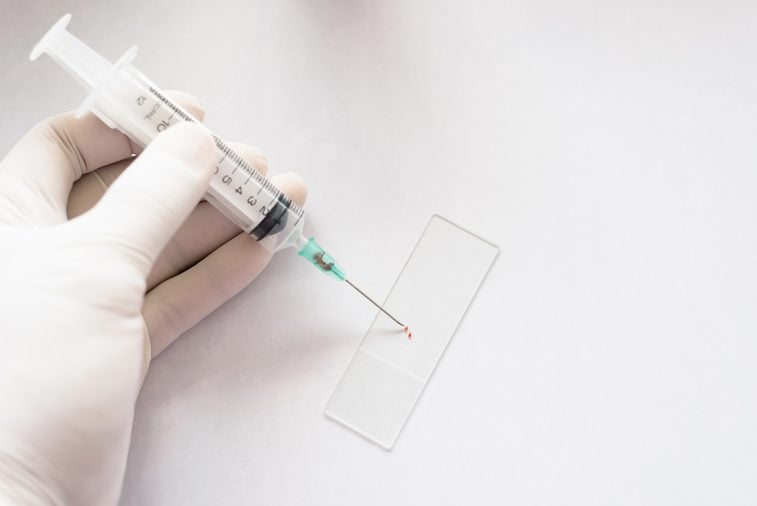
Myth: A biopsy can spread cancer
“This has been studied extensively. There is no evidence that a biopsy can spread cancer cells. In fact, it is very important to start with a needle biopsy of a lump or mass to determine if a lump is cancerous. If a diagnosis of cancer is made, the tumor is removed surgically with a surrounding margin of normal tissue and lymph node sampling may be performed at the same time. Although many patients come in asking for a lump to be removed with surgery instead of a needle biopsy, in fact the needle biopsy is an essential guide for further treatment and helps to avoid multiple unnecessary trips to the operating room.” —Preya Ananthakrishnan, MD

Myth: Dad’s breast cancer family history isn’t an issue
“Your father’s family history of breast cancer is just as important as your mother’s in understanding your risk. The medical history of women on your father’s side of the family impact your chances of getting breast cancer just as much as the family members on your mother’s side.” —Caroline Coombs-Skiles, MD
Myth: Weird nipples are always a cancer symptom
“You can’t tell someone has cancer just by looking at them. If your nipples have always been inverted, that is just how your breasts are shaped. However, if the nipples change suddenly, like invert or change color, that is a concern you should address with your doctor to rule out cancer. Hairy nipples on women have nothing to do with cancer and are totally normal.” —Neelima Denduluri, MD. Be aware of these breast cancer symptoms that aren’t lumps that every woman should know about.
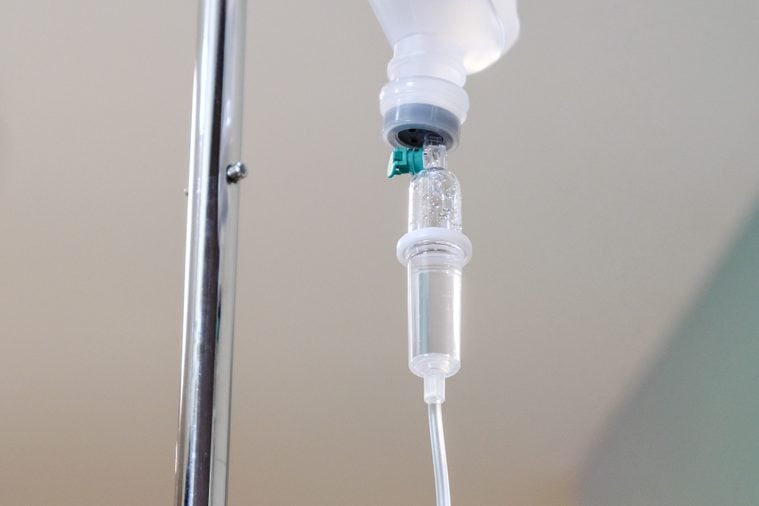
Myth: It’s safe to delay chemo
“More and more women are delaying chemotherapy as a treatment for their breast cancer in order to try alternative therapies like supplements or diets first. This may not be a good idea. Timely initiation of breast cancer chemotherapy is associated with better breast cancer survival.” —Heather Greenlee, PhD, an assistant professor of epidemiology at Columbia University’s Mailman School of Public Health in New York City.