I Was Diagnosed With Colon Cancer at Age 34
Updated: Oct. 10, 2022
Before a stage 4 colon cancer diagnosis, a young mother dismissed early symptoms, like fatigue. Here's how she found out she had cancer, and the surgery, chemotherapy, and other treatments that helped.
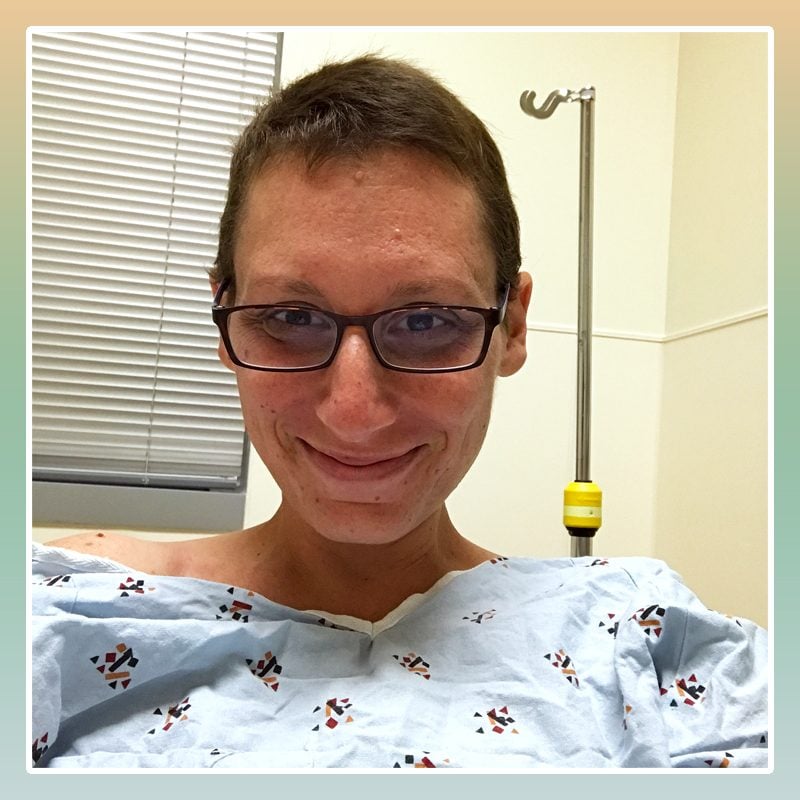
While blood in the toilet bowl may be one sign that something is going on with your health, other colon cancer symptoms include constipation, bloating, diarrhea, anemia, and other stool changes that last longer than a few days. When spotted early, colorectal cancer can be prevented or more easily treated. But if it’s caught late, as it is in many younger people, it can mean a more difficult path. Here, Jenessa Schwartz, 37, shares her symptoms, diagnosis, and treatment for stage 4 colon cancer.
Overlooking common symptoms
When you’re pregnant or a mom of young children, you tend to overlook a lot. And while I used to consider myself quite healthy, I was pregnant and/or breastfeeding almost nonstop from 2009 to 2015. I had my two children less than two years apart, and then I carried twins in a surrogate pregnancy when my youngest child was two.
Looking back, I began having subtle symptoms after the twins were born in 2015: chronic fatigue, inconsistent bowel movements, and occasional mild nausea. All were things that I could easily ignore or explain away. I thought to myself, what mother of young children isn’t tired all the time? What busy woman runs to the doctor for a little bit of constipation or diarrhea?
(These are the signs of colon cancer in women you should know.)
A bowl of bloody stool
On a regular day in March 2017, when I was 34 years old, I had a terrible bout of bloody diarrhea. It came out of nowhere. It was not just a little bit of blood in my stool—it was toilet bowls full of blood.
Even so, I was ready to explain it away. I happened to mention it to a friend, who said bloody stool really wasn’t good. She convinced me to call my doctor.
I reluctantly made an appointment and had a somewhat humiliating—but totally painless—rectal exam. My doctor didn’t see anything that would have caused so much bleeding, but he decided to order labs and a colonoscopy just to be safe.
“It’s likely nothing,” he said casually as the appointment was ending. “But I can’t promise it’s not colon cancer.”
An interrupted colonoscopy, a CT scan, and a diagnosis
His comment didn’t register with me until a few weeks later, when I woke up after my colonoscopy to a somewhat panicked gastroenterologist (GI doctor) telling me she was sending me down for a CT scan right away.
She said that she hadn’t been able to finish the procedure because she had encountered a large tumor nearly blocking my entire colon at the splenic flexure, the sharp bend between the bottom part of the colon and the transverse colon, the long, middle part.
I had the CT scan, then spent the next few days in a daze, unable to really process what was happening. I went to see a GI surgeon first, who showed me the scans and pointed out the primary tumor in my colon as well as some lesions on my liver.
I went through some more testing, which revealed the cancer had spread to my lymph nodes, my omentum (the tissue that surrounds the abdominal organs), and my peritoneum (the thin membrane that lines the abdominal cavity).
At my first visit to the oncologist, he told me I had stage 4 colon cancer. “People with your diagnosis used to only live about a year, but with current treatments, you may get twice that,” he said to me.
I remember staring at him, completely numb. “Twice one year is…two years,” I said.
It took weeks for what he said to really sink in. Even so, I was determined to fight. I was determined to continue raising my children, who were four and six at the time, for as long as I possibly could.
Starting chemo
Things happened very quickly after my diagnosis. My doctor said that because of the extent of my disease, surgery was not an option. Chemotherapy was my only route for treatment.
I had a port put into my chest and began chemo right away. I suffered from pretty bad nausea and peripheral neuropathy (nerve-related pain and other symptoms in the arms, legs, feet, and hands), but I teach middle school language arts and managed to finish out the last couple of months of the school year.
A few months into my treatment, I got some good news: Scans showed that my disease had shrunk significantly from the chemo, which made me a candidate for a procedure called HIPEC (hyperthermic intraperitoneal chemotherapy), which is performed during surgery (called cytoreduction surgery, or CRS).
Surgeons would open up my abdomen, remove any visible disease and then pump heated chemotherapy into my abdominal cavity with the goal of killing any other microscopic cancer cells.
Among patients, CRS/HIPEC is known as the “mother of all surgeries.” It is extensive, carries major risks, and can come with a brutal recovery. Even so, I knew it was my best chance at getting rid of the cancer, so I decided to do it.
The mother of all surgeries
During the procedure, my doctors ended up removing the primary tumor and a foot of my colon. But they didn’t stop there. The surgery also removed my appendix, gallbladder, some of my liver, 26 lymph nodes, my falciform ligament (the ligament that separates the liver into two lobes), and three clusters of cancer on my peritoneum.
To give my colon time to heal, I received a temporary ileostomy, a procedure that connects the small intestine to the abdomen. That meant I would excrete waste into an external ostomy bag.
Colon cancer tends to spread to the liver, lungs, and ovaries, so I knew there was a chance they would need to remove my ovaries as well. But when my surgeon looked at them during the procedure, she was extra concerned and ended up paging a gynecological oncologist to the operating room.
This new surgeon performed a hysterectomy to remove my uterus and a sliver of my cervix, and a bilateral salpingo-oophorectomy to take out my ovaries and fallopian tubes.
My surgeon’s concern ended up being spot-on. When the pathology report came back later, I learned that there was more cancerous tissue than normal tissue in both of my ovaries.
A healing colon and reversing the ileostomy
Recovery from surgery was long, slow, and just as challenging mentally as it was physically. Learning to live with the ileostomy would have been challenging enough, but it turned out that I am allergic to nearly every medical adhesive, which is how they normally attach the bag to your body. Every single one destroyed my skin.
I spent a lot of time in bed feeling sorry for myself. Even so, my family and friends were a never-ending source of comfort and support, pushing me to get out of bed, eat food, and take walks outside.
Slowly, I regained my strength. Once my colon had healed, I had a second surgery to reverse the ileostomy.

The long road to “no evidence of disease”
In early 2018, I restarted chemotherapy. When a scan shortly after restarting treatment showed an early recurrence in my liver, I was pretty devastated.
My frustration was compounded by the fact that several surgeons said they would not operate on me. One even compared me to an old car, saying, “If a car has no tires, you’re not going to replace the carburetor.” At that point, my original surgeon stepped in and said she would operate on my liver—I could practically hear her rolling her eyes at all the men who had refused.
She did an open liver resection to remove the recurrence, after which I did six more rounds of chemo. Then, in October 2018, I was finally declared NED—no evidence of disease.
I knew that as a stage 4 colorectal cancer patient, NED is as good as it gets. My chance of recurrence was nearly 100 percent, but NED for any length of time was something to celebrate.
I had 10 glorious months of no treatments and no surgeries. Every three months, I would go in for a scan and hold my breath, expecting the worst but hoping for the best.
Colon cancer recurrence
In August 2019, my scans revealed a startlingly abrupt and extensive recurrence. The disease was back in my liver, peritoneum, and pelvis. I took my family on a last-minute, whirlwind trip to Disneyland, then we came back and I restarted treatment in September.
I began a protocol of chemotherapy every other week, which quickly became the rhythm of our lives. Thankfully, I could tolerate this treatment fairly well and was able to parent, work, and generally live life to my fullest.
I had to tweak my treatment this past September when a scan revealed cancer in my lungs, and that new therapy wiped me out for a while. But eventually, I regained my rhythm.
Extending my colon cancer prognosis
I’m not sure if I will achieve NED again, but I do think I will remain stable for a long time. During most 14-day cycles, I have more good days than bad days, and the kids provide all the motivation I need to keep going.
On March 27 of this year, I will reach my four-year cancer-versary—that’s twice as long as my original prognosis, and I fully intend to keep on doubling!
If there is a moral to my story, it’s to listen to your body and not try to explain away symptoms. Early-onset colorectal cancer is on the rise, and the young people that are diagnosed tend to be diagnosed with late-stage disease. Don’t hesitate to get checked out.
—As told to Alyssa Sybertz