Botox for TMJ: Does It Work and Is It Safe?
Updated: Mar. 14, 2022
Feeling jaw pain? It's possible it could be due to "temporomandibular joint" (TMJ) disorder. Some experts now say Botox may be a solution worth considering to treat TMJ.
The pain in your jaw
We’ve all experienced occasional jaw pain, which sometimes goes away on its own. But what causes jaw pain that persists, especially when it’s accompanied by clicking sounds or grating sensations when you chew or yawn? One possible answer is that it’s temporomandibular joint disorder—better known as TMJ.
TMJ is a condition that affects more than 10 million Americans, according to the National Institutes of Health (NIH).
Botox for TMJ is one possible avenue for relief that some dental and medical professional now recommend. Here’s what experts suggest you should know about how Botox for TMJ works.
How the jaw works
Your jaw is one of the few joints in your body that can move in all directions—up, down, side to side, forward, and even backward. This flexibility comes from the temporomandibular joint and its connecting masseter muscle, which acts as a “hinge” for your jaw. If you put your fingers near your ears and move your mouth, you’ll feel the joints in action.
According to the American Dental Association, the jaw is the only joint in your body that purposely dislocates, then re-locates after use. These cool but complex mechanics can make it difficult to treat when problems like TMJ occur.
Symptoms of TMJ disorder

The most common symptom of TMJ disorder is frequent, radiating pain in the jaw joints or masseter muscle that won’t go away on its own. TMJ disorder is often to blame when the pain is recurring and does not respond to typical pain medication or therapeutics.
The TMJ Association, a national patient advocacy group, says TMJ disorder can also cause neck and shoulder pain, chronic headaches, limited jaw movement, ringing in the ears, and even dizziness or vision problems.
What causes TMJ?
The exact cause of TMJ disorder is unknown. For many people, symptoms come on suddenly without any detectable reason, but the explanations may include genetics, jaw injuries, teeth grinding from stress, and even arthritis.
Research suggests women are much more likely to have TMJ disorder than men. Kids are also susceptible, with adolescent girls reportedly at greater risk than boys.
Standard treatment to relieve the pain of TMJ
Diagnosing and treating TMJ disorder may start with your dentist. Some professionals may follow a “less is more” type of strategy, as outlined by the National Institute of Dental and Craniofacial Research.
The organization recommends some minor interventions (along the lines of these at-home TMJ remedies) before a patient pursues more invasive modes of treatment. TMJ treatment options may start with a dental pro’s recommendation to eat softer foods, avoid chewing gum, apply cold packs and warm packs when pain flares, use relaxation techniques to ease tension (such as meditation), and specific exercises to strengthen jaw muscles.
If these techniques don’t work, a dentist or other healthcare provider may prescribe medications such as muscle relaxants, anti-anxiety drugs, or anti-inflammatory medications. You may wear a night guard or bite plate to prevent clenching or grinding your teeth.
In extreme cases, surgery may be the only option for relief. The NIH advises that surgical treatments are controversial and often irreversible. The NIH recommends avoiding this, if possible, as the long-term effectiveness is currently unknown.
However, if you’re suffering from TMJ symptoms, there’s been some progress in research for a different kind of solution.
Botox as a breakthrough for TMJ disorder
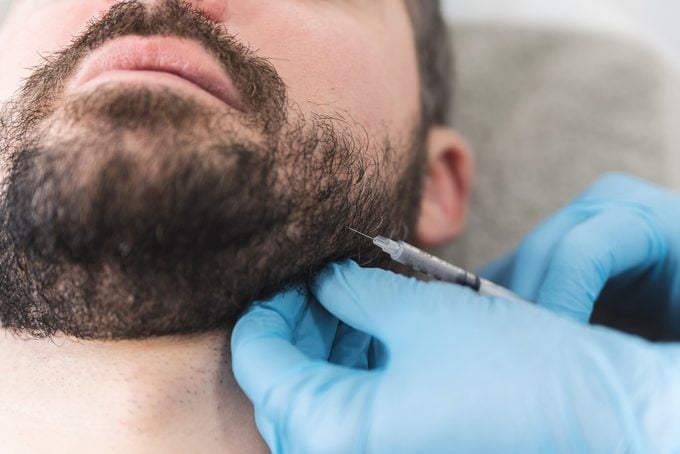
Lately, some healthcare providers have been turning to Botox for TMJ treatment. Botox—or onabotulinumtoxinA—was first approved in 1989 by the U.S. Food and Drug Administration (FDA) for cosmetic use, then later for chronic migraines and eye disorders.
Botox is derived from the same toxin (Clostridium botulinum) that causes botulism, a deadly food poisoning that paralyzes muscles. But this muscle-relaxing trait also helps tame the hyperactive muscles in the temporomandibular joint, alleviating pain and discomfort.
Although there is no FDA-approval for Botox to treat TMJ disorder, licensed healthcare providers can still use it “off label” when their clinical judgment suggests it’s appropriate.
Louis Malcmacher, DDS, president of the American Academy of Facial Esthetics, says Botox is a “game changer” for patients struggling to deal with chronic pain and discomfort from TMJ disorder.
Of Botox for TMJ, Dr. Malcmacher says: “[…It] has worked where nothing else had worked before.”
The science behind Botox and TMJ
Despite many studies on Botox and TMJ disorders over the past two decades, the National Institutes of Health deems clinical studies “inconclusive” on the effectiveness of Botox for treatment of chronic TMJ disorders.
“Studies have looked at injecting [Botox] into the chewing muscles to reduce muscle spasm and pain,” said J.D. Ventura, a spokesman for the NIH. “However, the information from these studies is limited, and it is not clear whether this medication works to relieve symptoms.”
Allergan, the pharmaceutical company that manufactures Botox, is currently conducting a clinical trial on the use of Botox to treat TMJ disorder. This is the final testing phase before the FDA considers official approval for use. It’s been reported that in the past, the FDA’s approval of Botox for TMJ disorder traces back to early studies that linked Botox to loss of bone density in animals.
However, more recent research suggests this may not be the case among humans. In 2020, a study published in the peer-reviewed Journal of Oral Rehabilitation by researchers at the NYU College of Dentistry concluded that low levels of Botox did not result in “significant bone-related changes” when used to manage pain in humans with TMJ disorder.
The study did, however, recommend continued research. Karen Raphael, PhD, the study’s lead author, stated: “Given the concerning findings from animal studies, and the limited findings from clinical studies, more research on the safety of Botox for jaw muscles and bones is critically important.”
How Botox for TMJ works to stop pain
Dr. Malcmacher says about 85 percent of “orofacial” pain is from misfires in the head and neck muscles. This is why Botox has helped some patients with chronic TMJ disorder. “Botox directly treats the muscles by relaxing them and reducing the intensity of the muscle contraction,” Dr. Malcmacher explains.
A professional determines how much Botox is necessary, and then may inject the product into the patient’s forehead, temple, and jaw muscles. Improvement typically occurs within days, with the effect lasting several months before another treatment may be needed.
“In my experience, Botox has a much higher success rate than any of the other [treatments] currently available for at least partial relief,” Dr. Malcmacher says, adding that “full relief is quite common.”
To ensure the best outcomes, Dr. Malcmacher says it is essential for a patient to turn to a licensed healthcare professional such as a dentist, physician, or nurse, who is specifically trained to administer Botox for TMJ.
The most common side effect of Botox, according to Allergan, is pain or swelling at the injection site. Occasionally, patients report drooping eyes or drooling. If these effects continue for more than a few days, a followup consult may be necessary.
The cost of Botox treatments
Since Botox is not FDA-approved for TMJ disorder treatment, most insurance companies will not cover the cost… and unfortunately, out-of-pocket can be expensive. A doctor may recommend 40 units of Botox per side, per treatment, at an average industry cost of $10 to $15 per unit. Then consider the provider’s administration fee and other potential costs, and Botox for TMJ maintenance can add up fast.
However, some insurance companies may cover Botox treatment as a therapeutic for TMJ disorder. Additionally, since Botox is FDA-approved for chronic migraines, insurance may cover a diagnosis of migraines related to TMJ disorder.