What You Need to Know About Ulcerative Colitis
Updated: Mar. 16, 2021
Ulcerative colitis, an inflammatory bowel disease, can cause cramping, abdominal pain, and other symptoms. Here's what doctors want you to know about this condition that affects the digestive tract.
Our editors and experts handpick every product we feature. We may earn a commission from your purchases.
On This Page
What is ulcerative colitis?
Ulcerative colitis is a chronic inflammatory bowel disease that causes irritation and ulcers, or open sores, in the intestine. This can result in painful symptoms, such as severe belly pain, cramping, and urgent bowel movements, that often leave you on the sidelines.
In the United States, the number of individuals with ulcerative colitis is estimated to be 900,000, says Kelly Cushing, MD, a clinical lecturer and gastroenterologist at Michigan Medicine in Ann Arbor. That’s much less frequent than common diseases like type 2 diabetes and heart disease.
“However, it is also not a rare disease, and individuals should be aware of common signs and symptoms,” says Dr. Cushing.
Where does ulcerative colitis start?
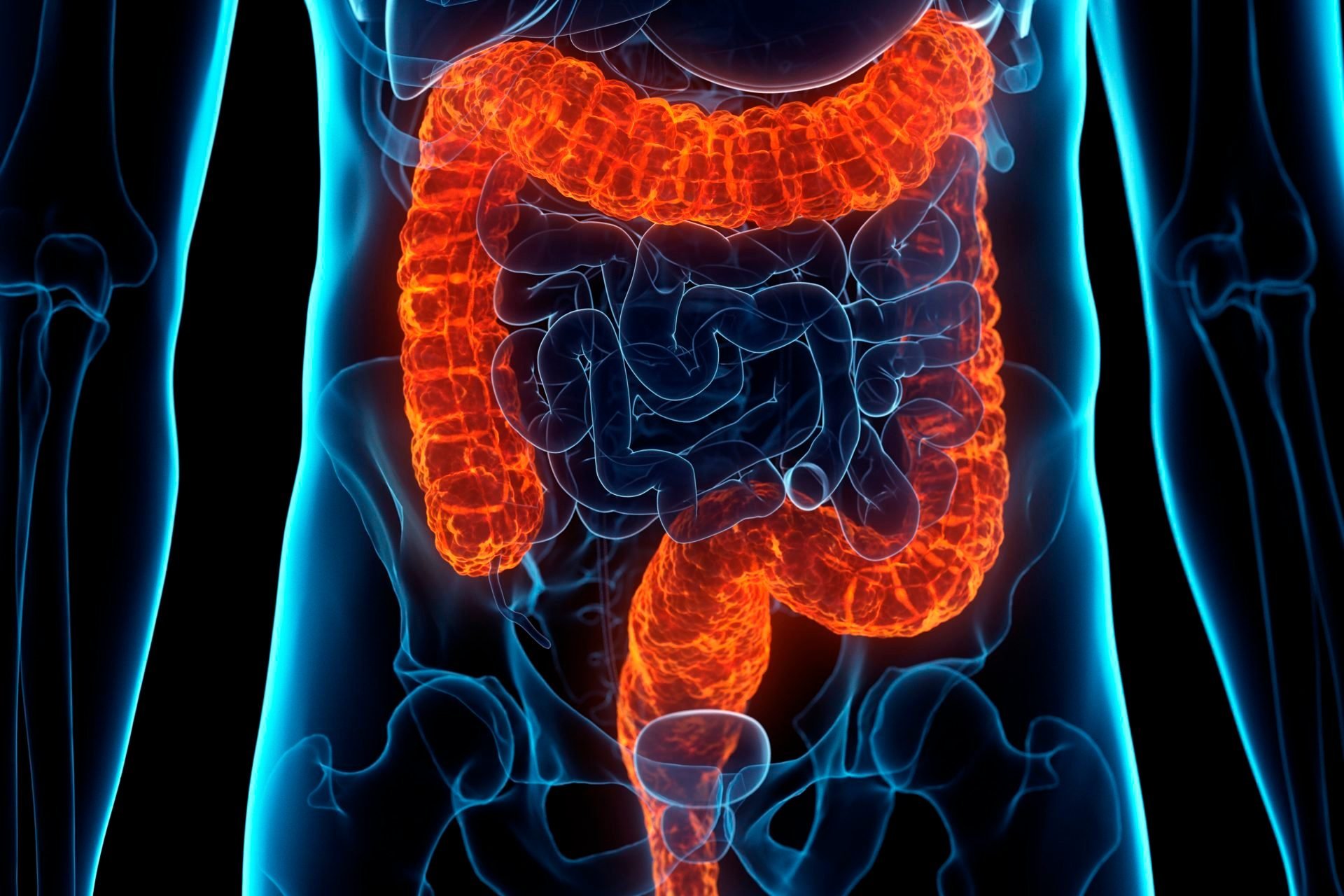
Ulcerative colitis occurs in the large intestine, also called the colon, and can include the rectum, but the painful inflammation occurs only in the innermost lining of the intestine, or mucosa.
The condition usually begins in the rectum and the lower part of the colon, but the inflammation can spread to the entire colon. The inflammation causes diarrhea and the cells in the mucosa to die, causing ulcers to form. These ulcers may cause pus, mucus, and bleeding.
Ulcerative colitis usually starts slow and gets worse, and it’s unpredictable—you may have months or even years of remission, when symptoms are very mild or not present at all, or you may have flare-ups when symptoms get worse or return more often. This is not an unusual pattern for autoimmune diseases, which includes inflammatory bowel diseases like ulcerative colitis.
Ulcerative colitis can happen at any age, even in children, but is more commonly diagnosed in young adulthood, such as in the teens or 20s, and late adulthood, in people in their 50s or 60s, Dr. Cushings says.
“Infections can trigger the onset of ulcerative colitis or a flare of ulcerative colitis. However, the disease can also occur or flare in the absence of infections,” she says. There’s no cure for ulcerative colitis, but medication, diet, and other therapies can treat it. (Here are the gut digestive symptoms to pay attention to.)
Types of ulcerative colitis
It’s important to know which part of the intestine is affected, as the symptoms and extent of inflammation vary. The three most common types of ulcerative colitis are:
Ulcerative proctitis: The inflammation is restricted to the rectum—usually less than 6 inches of the rectum. Symptoms include urgent bowel movements, rectal pain, and rectal bleeding.
Left-sided colitis: The inflammation in left-sided colitis stretches from the rectum up to the splenic flexure, a part of the colon near the spleen in the upper left abdomen. Proctosigmoiditis is a form of left-sided colitis as well. People with this type have pain on the left side of the abdomen, diarrhea, loss of appetite, and weight loss.
Extensive colitis: As the name implies, the inflammation is extensive—affecting the entire colon. Symptoms include bloody diarrhea, abdominal pain, lack of appetite, and weight loss.
How is ulcerative colitis different from Crohn’s disease?
It’s easy to confuse ulcerative colitis with Crohn’s disease. Both are inflammatory bowel diseases with similar symptoms, and both are autoimmune diseases that affect the digestive tract. But the main difference between the two is the location of the damage.
Inflammation in Crohn’s disease can target any part of the digestive tract, from the mouth to the anus, and extend through the intestinal wall. Yet there may be spaces where the digestive tract is healthy.
In contrast, inflammation in ulcerative colitis is confined to the colon, tends to be continuous (without healthy patches), and affects the inner lining only.
Neither condition is related to irritable bowel syndrome, a different type of digestive ailment that causes diarrhea and constipation but doesn’t have the same type of intestinal damage seen with inflammatory bowel diseases.
According to the Centers for Disease Control and Prevention’s latest statistics, an estimated 3 million people reported having either Crohn’s or ulcerative colitis.
(Learn more about the difference between ulcerative colitis vs. Crohn’s disease.)
Ulcerative colitis symptoms
Symptoms of ulcerative colitis can vary from person to person, as can their severity. “The symptoms of ulcerative colitis can be nondescript, such as abdominal discomfort and diarrhea.
Therefore, some patients may mistake symptoms for a transient illness or infection and have a delay in diagnosis,” says Dr. Cushing. Don’t procrastinate. Call your doctor if diarrhea persists for more than two days.
Here are the most common symptoms to look for:
- Diarrhea
- Stomach pain
- Rectal bleeding
- Urgent need to move bowels
- Fatigue
- A sensation of incomplete bowel movement
The inflammation can cause problems in other parts of the body including fever and joint pain, as well as cause eye, skin, liver, and bone problems.
Do certain foods cause ulcerative colitis?
When you have a belly ache or diarrhea, you might blame it on something you ate. But when it comes to ulcerative colitis, food is not the culprit.
While the exact causes of the disease are unknown, we do know that it involves an interaction between the immune system, genes, and environmental factors.
The immune system is set up to attack and kill viruses, bacteria, fungi, and other microorganisms. But for people who have ulcerative colitis (or Crohn’s), the immune system doesn’t retreat. Instead, it keeps firing away, resulting in inflammation.
People who have inherited genes for inflammatory bowel diseases are more susceptible to this. Additionally, unknown environmental factors can trigger and ignite this harmful immune response.
Treatment for ulcerative colitis
Treatment is tailored to each individual based on what type of ulcerative colitis is present, the severity of symptoms, and other factors, such as other existing medical conditions. Taming the inflammation is key.
“We see our medications as the first line and use diet more of an adjunct,” says Nimah Ather, MD, a gastroenterologist at the Ronald Reagan UCLA Medical Center in Los Angeles.
Once inflammation is subdued, the goal becomes achieving and then maintaining remission. If you don’t accomplish remission, the focus is to decrease the severity of your symptoms.
Traditional medications
These medications are often used to treat ulcerative colitis:
- Aminosalicylates (anti-inflammatories)
- Corticosteroids (reduce immune system activity)
- Immunomodulators (modifies and decreases activity in the immune system)
- Janus kinase inhibitors (suppresses the immune system)
Biologic medications
Biologic therapy is relatively new and approved for moderate to severe ulcerative colitis. Unlike other medications, biologics are protein-based drugs that mimic naturally-occurring growth factors and molecules. They’re produced via a biological—as opposed to chemical—process.
“For those that continue to have symptoms such as diarrhea and blood in their stool, stronger medications such as biologics should be considered,” says Dr. Ather.
Another reason a doctor may turn to biologic drugs: You’re dependent on powerful steroid drugs, such as prednisone, that reduce symptoms by suppressing the immune system.
“Although steroids are effective for the treatment of ulcerative colitis, long-term use can lead to osteoporosis, poor wound healing, increased risk of infections, and elevated blood sugars,” Dr. Ather says. He believes that biologics are a better long-term options than steroids.
Diet
While there is no specific diet that’s recommended for all people with ulcerative colitis, certain foods can exacerbate symptoms. Keep in mind: There is no one-size-fits-all diet for ulcerative colitis.
“Diet is used more when we know their ulcerative colitis looks to be under control but they are still having symptoms,” Dr. Ather says. “We work with dietitians more to figure out what foods are aggravating their GI [gastrointestinal] symptoms since a specific diet hasn’t been shown to cause ulcerative colitis.”
An essential tool to identify foods that aggravate your ulcerative colitis is a food diary. Use it to spot the connection between what you eat and the symptoms that may follow. Your doctor may also suggest an elimination diet, in which certain foods are removed from your diet to find which ones you may not tolerate.
Here’s some bowel-friendly diet tips:
- Eat smaller meals at more frequent intervals throughout the day.
- Soft, bland foods might be easier on your digestive tract.
- Stay away from foods that can cause diarrhea, like greasy and fatty foods.
- If you’re particularly gassy, don’t use a straw or drink carbonated beverages.
- When diarrhea is in full swing, curb your caffeine intake, as it acts as act as a laxative. But be sure to drink plenty of water because diarrhea can cause dehydration.
- If you’re lactose intolerant, limit dairy foods.
- Boil, steam, poach, or grill foods.
- Limit insoluble fiber (foods that contain this promote bowel movement and are harder to digest). You’ll find it in raw veggies, fruits with skin and seeds, whole nuts, whole grains, and cruciferous vegetables such as broccoli and cauliflower. Peel and cook other veggies before eating.
Surgery
When medications no longer work to keep ulcerative colitis under control, surgery may be an option. There’s more than one type of ulcerative colitis surgery. Some remove only portions of the colon, while others remove the full colon.
Certain types of surgery redirect stool to an ostomy bag, which must be worn at all times to collect waste that would normally exit the body in a bowel movement.
“The good thing about surgery is that it can be curative for ulcerative colitis,” says Dr. Ather. “Most patients who go the surgery route will be able to have regular bowel movements and not have to wear an ostomy bag to remove their waste.”
(These are the secrets your surgeon won’t tell you.)
Flare-ups
After the initial diagnosis and treatment, you may feel fine for weeks or months, or you might suddenly be affected by mild to severe symptoms, otherwise known as a flare.
“Flares can range from mild to severe,” says Dr. Cushing. ” Mild flares may only last a few days and resolve with minimal intervention. Severe flares may last for several weeks and require more intensive medical therapy changes.”
The exact cause of flare-ups in ulcerative colitis is still not entirely known.
Dr. Cushing says gastrointestinal infections are a common trigger, although not all infections will cause a flare-up. Other potential triggers are missed doses of ulcerative colitis medicines and the use of nonsteroidal anti-inflammatory drugs (NSAIDs) and antibiotics, both of which provoke disease activity.
Treating ulcerative colitis flare-ups
“If a patient experiences a flare of ulcerative colitis, their provider will often ask several questions about the severity of their symptoms as well as try to identify potential triggers,” says Dr. Cushing.
That’s why it’s good to keep a diary. Include a timeline of how long you have had symptoms, the progression, stool frequency, blood in the stool, and other symptoms, such as weight loss.
Your doctor may order tests to get to the bottom of your flares. “Testing often includes ruling out infection and assessing disease activity through the use of stool studies,” says Dr. Cushing.
Next, you and your doctor will devise a treatment plan. “We manage flare-ups with medications, change in diets, and control of stress,” Dr. Ather says.
(Here’s what to know about the different types of poop.)
Comfort tips for flare-ups
Sources of comfort are essential to coping with a flare. Here are some home remedies you can use to feel better:
- Use moist towelettes or wipes instead of dry toilet paper. Even better, consider installing a bidet attachment for your toilet.
- Use Vitamin A&D ointment or Desitin to the area around the anus before going to sleep.
- If your doctor says it’s okay, take Imodium or Pepto-Bismol to help relieve diarrhea.
- When bathing, use Balneol to clean and soothe a sore bottom.
- You can also calm an irritated bottom by relaxing in a warm sitz bath.
Complications
Good news: For most people, ulcerative colitis is not life-threatening.
Sometimes the disease leads to more serious conditions, however. “If a patient has severe disease, they could develop toxic megacolon,” says Dr. Ather. If you develop this rare but severe swelling of the colon, you’d need to be closely monitored in an intensive care unit and may require emergency surgery.
“Other life-threatening complications that may develop due to ulcerative colitis include tears in the colon, severe bleeding, and blood clots,” says Dr. Ather.
Symptoms beyond the intestine
When ulcerative colitis is raging, it can take its toll on more than just the GI tract.
“The inflammation from ulcerative colitis can make patients feel very fatigued; lead to blood loss, causing anemia; and cause weight loss due to difficulty absorbing nutrients,” says Dr. Ather.
Symptoms beyond the intestine affect mental health and quality of sleep, too. A study published in 2018 in the International Journal of Behavioral Medicine found higher rates of mental health and sleep disorders in people with ulcerative colitis.
“It is important for us to screen for these issues and refer our patients to get the help they need,” Dr. Ather says.
What about colon cancer risk?
“Anyone with ulcerative colitis that involves more than one-third of the colon has a higher risk of colon cancer,” says Dr. Ather. The risk of colon cancer is higher in left-sided and extensive colitis. However, in ulcerative proctitis, only a small amount of the colon is involved, so it doesn’t carry a higher risk of colon cancer, he says.
He recommends people get a colonoscopy to screen for cancer starting eight years after their ulcerative colitis diagnosis and then every one to three years, depending on what other risk factors they have. (Consult your doctor for specific advice on cancer screenings.) Have a colonoscopy coming up? Here are some colonoscopy prep tips to make it more tolerable—and comfortable.
What is ulcerative colitis remission?
Remission is the ultimate goal. In a given year, 1 to 2 percent of people with ulcerative colitis have severe disease activity, 20 percent have moderate activity, 30 percent have mild activity, and 48 percent are in remission, according to the Crohn’s and Colitis Foundation of America.
But what exactly is remission? There are two ways to know: symptoms and testing. “Bowel movements should average one to three per day, none at night,” says Fernando Velayos, MD, a gastroenterologist and director of the Inflammatory Bowel Disease Program at Kaiser Permanente in San Francisco. “There should be no urgency, no blood in the stool, and the person should also subjectively feel well.”
(Here are your pooping habits, explained.)
As symptoms vary among people, your doctor may elect to check objective tests of inflammation to determine if ulcerative colitis is in remission. These can include a stool test, a blood test, a flexible sigmoidoscopy, or a colonoscopy.
Remission is cause for celebration, but that doesn’t necessarily mean you can toss out your medications for good.
“Ulcerative colitis is a chronic condition characterized by periods of flares and remission, and most people will require some type of maintenance medication. It is important to continue maintenance medications to keep inflammation under control,” Dr. Velayos says. “Typically, over half of people in remission will relapse within a year if they do not continue with maintenance medication.”
Take care of your mental health
Living with the unpredictability of ulcerative colitis can be challenging both physically and mentally. There may be days when symptoms may cause you to miss out on the things you love to do. Or you might not be able to get quality sleep or enough nutrients because of frequent diarrhea.
It’s no wonder the symptoms of ulcerative colitis cause emotional stress. It’s normal to feel depressed and discouraged, but don’t suffer alone. Be sure to reach out to a therapist to talk about your feelings. Even better, find a therapist that specializes in chronic illnesses.