
Anosmia?
Smell is crucial to the way we experience the world, whether it’s the garlic in that sauce simmering on the stove, fresh cut grass, or the familiar scent of your first love’s perfume. That’s why anosmia, the loss of your sense of smell, can be such a blow. The condition can sneak up on you more gradually than hearing or vision loss. Because sense of smell is controlled by sensors in the nose that connect to your brain, there are a variety of conditions that could be triggering a reduced sense of smell—some temporary, others permanent.

Nasal congestion
“The most common cause is sinus blockage and congestion due to the accumulation of inflammation and toxins in the sinuses,” says Kulreet Chaudhary, MD, an integrative neurologist and author of Sound Medicine: How to Use the Ancient Science of Sound to Heal the Body and Mind. “Causes of poor digestion are multifold and involve excess stress, overworking, poor eating habits, imbalanced microbiome, and overconsumption of processed foods.”
If your congestion and subsequent loss of smell aren’t the result of a cold or allergy, they may be the result of digestive issues or stress. “The best treatments involve improving digestion to relieve the accumulation of inflammation in the sinuses,” says Dr. Chaudhary. (Here are some tips for dealing with loss of smell from allergies.)
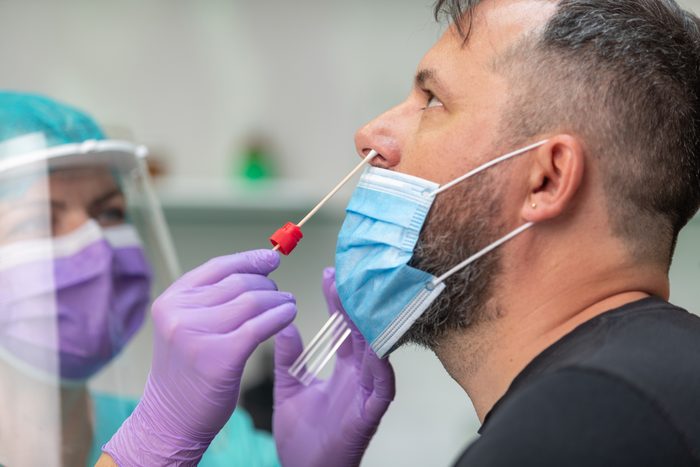
Covid-19
Since the early days of the pandemic, a loss of smell was recognized as a hallmark symptom of a Covid-19 infection. Research, including a study published in April 2020 in International Forum of Allergy & Rhinology, found that 68 percent of Covid-19 patients reported losing their sense of smell.
“The reason is because the coronavirus attacks the olfactory nerve,” says Jordan Teitelbaum, DO, an otolaryngologist and head and neck surgeon in Chicago. “This loss of smell is sudden, and it indicates an early sign of Covid-19 infection. That’s why it’s important for people who have loss of smell to seek coronavirus testing and to self-isolate until they get results.”
On a positive note: A loss of smell in someone diagnosed with Covid-19 may indicate a milder form of the disease, as compared with someone who has shortness of breath, says Dr. Teitelbaum. “This loss of smell typically returns within two to three weeks.” Read how this sommelier is fighting to regain her loss of smell from Covid-19.

Smoking
Pollution in general is an anosmia culprit, and tobacco smoke is the most concentrated form of pollution most people are exposed to. It impairs the ability to identify odors and lessens your sense of taste.
“Studies show that both the heat of cigarette smoke and its chemicals can [destroy] the neurons responsible for smell,” says Dr. Teitelbaum.
The good news? It isn’t permanent, so long as you quit smoking. “Within 48 hours, nerve endings will start repairing themselves,” adds Dr. Teitelbaum. “Sense of smell should return strongly in two to three months and other supporting cells may help return full function within a year.”

Chemicals
Exposure to toxic chemicals, such as pesticides or solvents can wreak havoc on your sense of smell by burning the inside of your nose. “Unfortunately, damage can be permanent after repeated exposure,” says Dr. Teitelbaum. “There is much we do not know yet about how nerves regenerate. Research into figuring out these pathways and how to stimulate regrowth is ongoing. For now, we know enough to tell people to protect themselves against harmful odorants.”
Check the labels of any chemical spray before you use it. And be sure to wear a respiratory device that covers your nose when handling strong-smelling chemicals at home or at work.
Medications

Head trauma

Alzheimer’s disease
Research, including a review of studies published 2018 in Biosensors, shows that a failing sense of smell can be an early sign of Alzheimer’s. In fact, this symptom may show up long before you meet the diagnostic criteria for the degenerative brain disease. “In Alzheimer’s, abnormal proteins damage the central cortex of the brain responsible for smell early on in the disease process,” says Dr. Teitelbaum.

Parkinson’s disease
Like Alzheimer’s, Parkinson’s disease is a degenerative brain disorder. And like Alzheimer’s, there are early signs of Parkinson’s that are easy to miss. An impaired sense of smell is one, says Dr. Teitelbaum. While most people with anosmia won’t develop these diseases, the majority of patients with Parkinson’s do experience anosmia.
“In Parkinson’s, a loss of neurotransmitters is responsible,” says Dr. Teitelbaum. “What’s fascinating is that loss of smell can actually present before cognitive symptoms. Creating awareness of the association between smell dysfunction and progressive neural diseases may help secure earlier diagnosis and treatment.”

Aging
As you get older, your sense of smell, like your vision and hearing, will decline. “About half of people between 65 and 80 have a measurable loss of smell,” says Dr. Teitelbaum. “At age 85, the number increases to about 75 percent. Changes in enzyme production, accumulative environmental damage to the olfactory nerve, and a natural decline in neural circuitry all contribute to this gradual loss in the sense of smell.”
