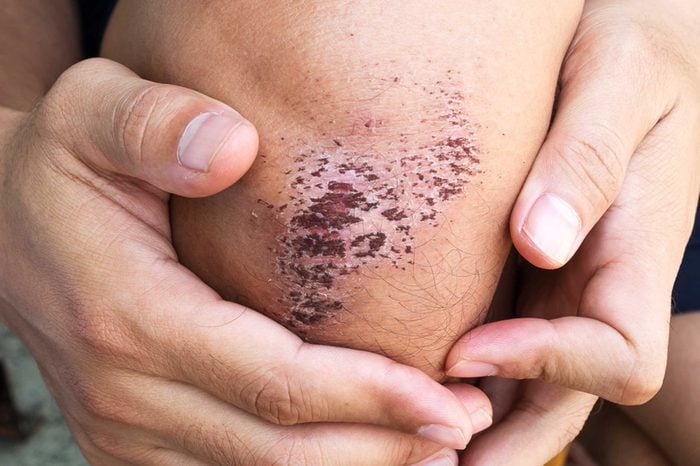
Stave off scabbing
Scabs. So annoying. Sitting there announcing to the world that you have a boo-boo and flirting with infection. “It is such a common misperception that ‘scabs’ indicate good wound healing, ” says Adam Friedman, MD, associate professor of dermatology and director of the Supportive Oncodermatology Clinic at George Washington School of Medicine and Health Sciences in Washington, DC. “A scab comprises dried blood, serum, dead skin cells, and dead bacteria that is actually a roadblock to new migrating skin cells which must now take a detour around that annoying scab to close the break in the skin,” he says. Try keeping the wound moist (with a thick moisturizer like petrolatum, for example) to allow new skin cells direct access.

Slap on a bandage
You might want to resist bandaging due to the ouch-factor when it’s time to peel it off. First, there’s a pain-free trick to removing bandages; second, you’ll speed healing with a little cover. “Keeping the area occluded will also prevent the risk for infection, as a scab is like an Old Homestead filet to bacteria,” says Dr. Friedman. Yes, this means that a bandage is your friend and won’t upset the healing process. In the future, smart bandages may be able to detect how well a wound is healing and send a report to the doctor. This research is now being conducted at several institutions, including Swansea University in Swansea Wales, United Kingdom.
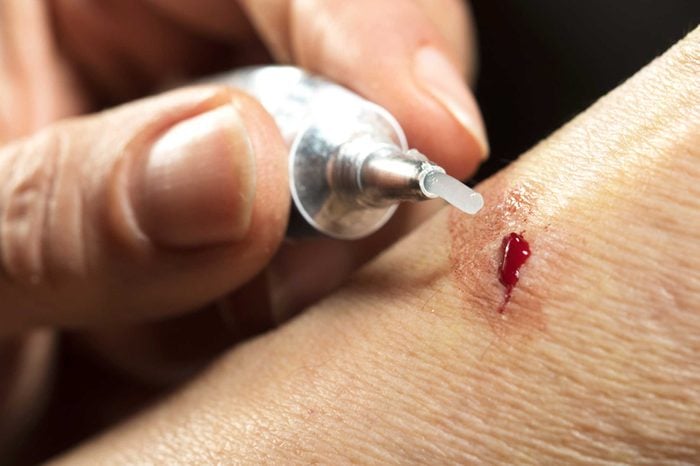
Sub out the Neosporin
Patients frequently ask Dr. Friedman if this favorite OTC spread can help healing. Simply putting any thick ointment on a wound has been shown to accelerate healing, but it’s good counsel to skip Neosporin or another antibiotic ointment unless there is an infection. The American Academy of Dermatology states that appropriate use of antibiotics, including topical ones, is paramount to preventing the rise of nasty antimicrobial-resistant bugs. (Do you know when to say no to antibiotics?) “Also, Neosporin is a well-known contact allergen which means for a good number of folks, its use can cause a really itchy and oozy rash,” Dr. Friedman says.

Make healthy choices
“Wound healing requires numerous cells, signals, and resources to mobilize over an extended period of time,” Dr. Friedman says. A “scar is not fully formed until one year after the actual injury, so how you take care of both the wound and yourself matters. This includes eating a diet high in Vitamins A and Z and zinc (especially coming from whole vegetables and fruit), avoiding sun exposure, limiting alcohol consumption and not smoking.” (Here are some other ways to strengthen your immune system.) Of note, exposure to smoke from just one cigarette impairs blood flow to chronic wounds and compromises healing—yet doctors rarely discuss this with patients who have chronic wounds, according to 2014 findings published in the Journal of Wound, Ostomy and Continence Nursing.

Take the right vitamins and supplements
Did you know that the herb arnica can help clear up bruises? And that’s not all it can do: “I provide all of my surgical patients with a supply of Arnica Montana pre- and post-op, both the pellets and the Arnica gel,” says New York City facial plastic surgeon Sam Rizk, MD. “It helps if they start on it the pellets a few days before any surgical intervention.” He also recommends 2,000 mg daily of Vitamin C (from food, if possible), which helps the body build tissues like skin, hair, and nails. “It also works to minimize bleeding into the skin and swelling.” This advice may help with non-surgical wounds too. Another surprising antidote: medical-grade Manuka honey on the wound may also aid healing.
Follow the cutting edge
Some of the most exciting innovation taking place in wound healing today is in the area of nanotechnology—the science of making things really, really, really small so they are more likely to get to where they need to go, which in this case is a wound. “Nano-wound care includes nano-silver dressings are really good are killing off scary bacteria, fungi, and viruses,” says Dr. Friedman. (Some bandages and creams already use silver to help reduce bacteria in wounds and cuts, including Curad’s Germ Shield.)
Another huge step will be the advancement of nitric oxide-generating nanoparticles. “Nitric oxide is involved in every step of the wound healing process and in many chronic wounds, nitric oxide production is damaged,” Dr. Friedman says. Nanotechnology that facilitates the production of nitric oxide from its precursor nitrite is in the works.
There’s more: Curcumin—the yellow polyphenol that gives turmeric its brilliant orange color—has been used to heal wounds for centuries, but it turns everything orange if applied topically. But “when you shrink down something in size, we can make orange/yellow curcumin invisible, thereby enabling its use,” he says. “We showed that nano-curcumin can accelerate wound healing in both burn wounds and MRSA-infected wounds.” Stay tuned.
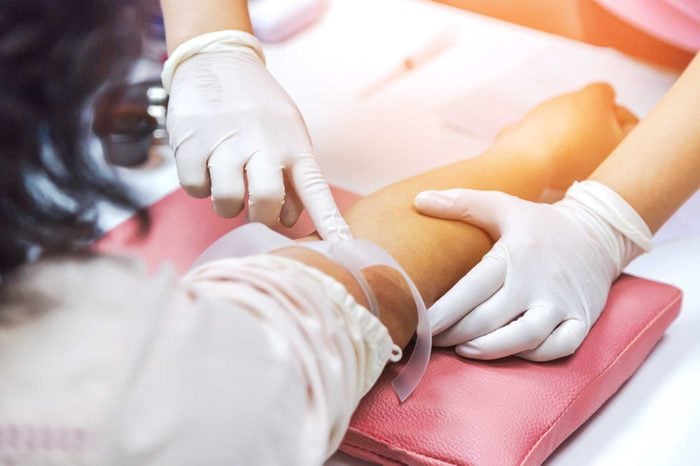
Tap into PRP
You’re probably doing everything you can to keep your bones healthy, right? What if you could heal a broken one faster? There’s a whole lot of buzz about the use of platelet-rich plasma (PRP) to heal injured tendons, ligaments, muscles, bones and joints, says Allan Mishra, MD, an orthopedic surgeon at Stanford Medical Center in Menlo Park, California. “It is becoming much more mainstream to consider using components of your own blood or bone marrow to treat a host of conditions. The power to heal comes from within.” PRP therapy involves taking some blood (about as much as would be drawn for a cholesterol screen), spinning it to isolate the plasma and all of the growth factors and proteins it contains, and then re-injecting it to the injured area. This can also be done with surgery to accelerate healing and decrease complications. “First and foremost, it is safe as we are using your own blood.” Still, more research is needed to identify ideal formulations for specific injuries, and this work will also encourage insurers to cover the cost of the therapy, which can be high. This evolving field of medicine is called regenerative medicine, and PRP is likely just the tip of the iceberg, he says. “Researchers including those at Replicel are actively trying to isolate the most important growth factors in the blood that can trigger and sustain and healing process.”
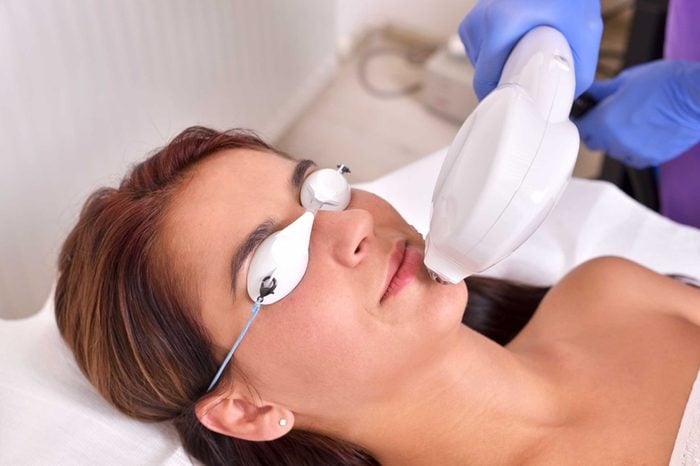
Take on scars
Sometimes the wound repair process ends with a scar, but that doesn’t mean you have to accept this outcome. “A scar may be itchy or painful, have discoloration, redness, textural changes—such as excessive thickening, depression, or ‘railroad track’ marks,” explains Estee Williams, MD, a board-certified dermatologist at Madfes Aesthetic in New York City. “Laser therapy is used to address each of these issues and is extremely important when optimizing the outcome of any scar, be it from trauma, surgery, or a burn.” For example, if the scar is from surgery, a vascular laser such as the Lumenis IPL (intense pulsed light) will selectively target the red part. “It is desirable to treat scars with lasers at this early point, not only for cosmetic reasons but also to facilitate proper wound healing. “By clamping down on the blood vessels ‘feeding’ the scar, IPL has the ability to prevent overgrowth of scar tissue. I recommend continuing monthly treatments until the redness has faded.” Some topical products such as Mederma Advanced Scar Gel or the Biocorneum line of products can also help.

