What are antibiotics?
Antibiotics fight bacterial infections including everything from strep throat to UTIs, and more. Although they’re helpful, taking them more often than needed can cause side effects, according to the U.S. National Library of Medicine. Just make sure to have a conversation with your doctor and ask the following questions before filling your antibiotic prescription.

Why am I taking this medication?
Every patient should verify and understand the rationale as to why they’re being prescribed an antibiotic, says Norman Tomaka, American Pharmacists Association spokesman and clinical consultant pharmacist in Melbourne, Florida. A JAMA study found that nearly a third of oral antibiotic treatments in the United States between 2010 and 2011 were inappropriately prescribed. Taking unnecessary antibiotics can make bacteria resistant to the drugs, so have an open discussion with your doctor to confirm your prescription is the best option.

When should I take this?
“There’s a difference between taking three times a day versus every eight hours,” says Barbara Young, an American Society of Health-System Pharmacists Consumer Medication Information editor. Antibiotics work best when taken at a consistent time between doses by keeping the right amount of the medication in your bloodstream. Instead of taking a pill with every meal, for instance, you and your doctor might find that a better time frame would be as soon as you wake up, during a midday snack, and right before bed.

Should my antibiotic be taken with food?
Eating when you take medication could affect how the drug is absorbed in your system. Taking an antibiotic with food could prevent nausea from a drug that might irritate the stomach, says Vincent Hartzell, American Pharmacists Association spokesman and president of Hartzell’s Pharmacy in Catasauqua, Pennsylvania. But it’s even more important to follow directions if a medication is meant to be taken with an empty stomach, because the food might block the drug from being absorbed in the bloodstream, he says.

Are there any foods I should avoid while on this medication?
Some medications may react badly with certain foods. For instance, dairy products make tetracycline and fluoroquinolones less effective because the calcium in the food binds with the antibiotic so your body doesn’t absorb as much, Young says. Make sure you’re aware of any foods that might get in the way of your healing.

Should I drink a full glass of water with my medication?
A glass of water can dilute stomach contents and help get an antibiotic through before your belly can get irritated, Tomaka says. While drinking enough water can help prevent nausea from most medications, other drugs need a full glass for proper absorption, he says. “A capsule prevents dissolution until it gets into the stomach, and taking it with water makes the difference between a good and bad experience,” Tomaka says.

Should I take a probiotic, too?
Not all the bacteria make you sick; some in your body are essential to a healthy bowel or reproductive system. But antibiotics don’t recognize which are which. “Most antibiotics aren’t specific to just kill the bacteria causing your infection,” Hartzell says. “They kill a variety of bacteria, including the ones you don’t want to kill.” When medications attack good bacteria, you might end up with an upset stomach, UTI, or yeast infection, Hartzell says. To prevent those side effects, your doctor might recommend eating probiotic-rich yogurt or taking a probiotic supplement. (Want to learn more? Read whether you really need to take probiotics after antibiotics.)
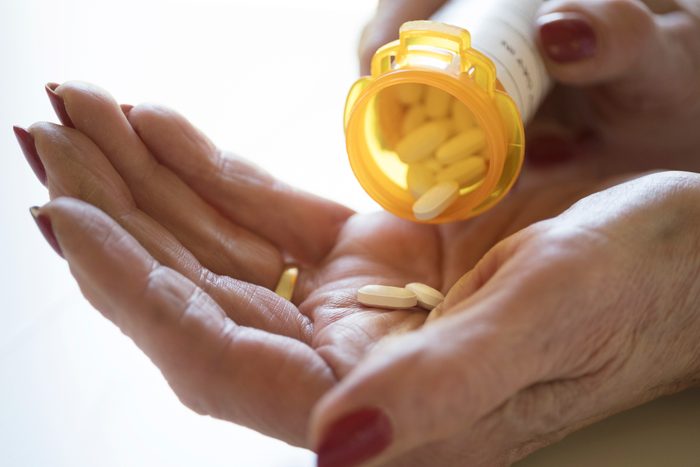
What should I do if I miss a dose?
In theory, you’ll take every pill at the right time. In reality, there’s a good chance you’ll forget and take one a bit too late. “It’s important to know ahead of time what to do if you miss a dose so you’re not scrambling for information when it’s late at night,” Young says. Some medications will work best if you take the medicine as soon as you remember, while others should wait until it’s time for your next dose.

When should I start to feel better?
You should always finish a prescription instead of quitting once your symptoms go away, because the bacteria in your body might still be at unsafe levels, Tomaka says. Still, it’s a good idea to know how soon you might start to feel healthy again, Hartzell says. “Usually if it’s been two to three days and you’re not feeling better, you need to call the doctor and go back because it’s either not the right choice of medication or something else is going on,” he says. Note that stopping an antibiotic before the infection is gone increases the likelihood of bacteria developing resistance.

What antibiotic side effects might I expect?
Side effects typically only occur in a very small percentage of those who take antibiotics, but it’s important to be aware of any possible reactions your body could have. Some medications could cause nausea, bloating, and diarrhea. “There are medication-specific things to watch for,” Young says. “Depending on the severity, a discussion with your provider would decide whether to continue or switch to another therapy.” Find out in advance what symptoms to look out for, and have a plan if those side effects happen. If you have an allergic reaction, however, you may have shortness of breath, while others might make you break out in hives. Seek medical attention for a possible drug allergy. (More on this below.)

Am I able to crush the pill?
If you have trouble swallowing pills, check with a doctor or pharmacist before crushing it, because it might not absorb the same way a whole capsule would, Young says. Many antibiotics also have a liquid form available, which could be a better option, she says.

Is this antibiotic safe with other medications I take?
Your doctor will likely ask what other medications you take to avoid a reaction, but don’t leave out easily forgotten drugs like birth control pills or over-the-counter supplements and vitamins. Some antibiotics might make birth control less effective, meaning you might need an alternative form of contraception, Hartzell says. Plus, iron from supplements binds to some antibiotics so they don’t absorb, he says. “It’s especially important to ask if you don’t get every prescription filled at that pharmacy,” he says. Your pharmacist or doctor might not be aware of every medicine you take, so make sure you provide an updated list before starting an antibiotic.
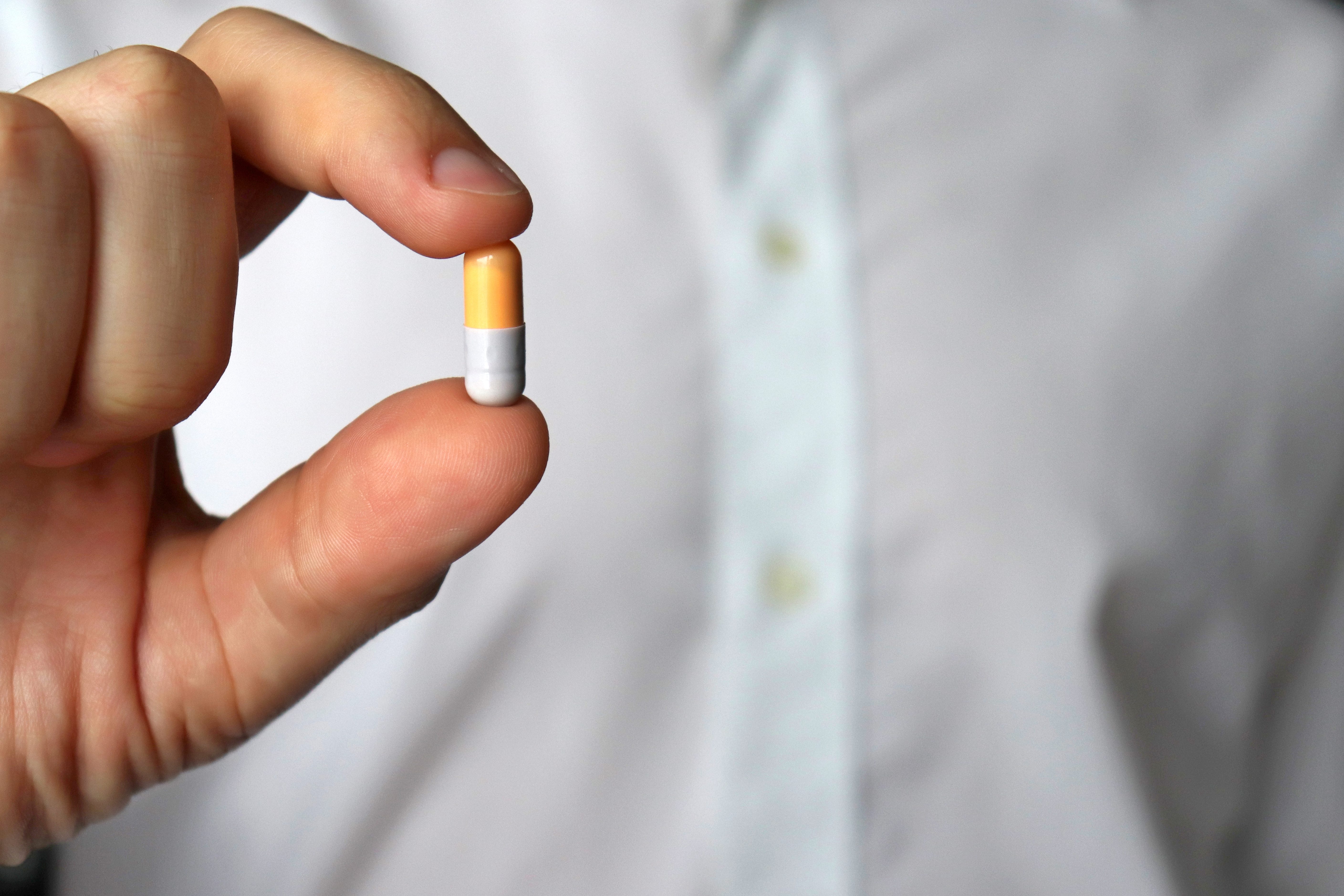
If I had a reaction in the past, am I allergic to this medication?
An allergy to an antibiotic means not only do you have to avoid that medicine, but you may also need to avoid other antibiotics in the same drug family, Tomaka says. But just because you had a reaction when you were younger doesn’t necessarily mean you need to avoid it now. Your system might be able to tolerate a type of penicillin that’s less similar to one that gave you a reaction, for instance. Plus, your reaction might not have been allergies after all—ampicillin, for example, can cause rashes in children related to histamine release, rather than an allergy. Note that side effects like nausea and vomiting are normal, and not signs of an allergy. You should still stick with a medication you know you feel comfortable with, but it might be worth a future visit to test whether you’re truly allergic. “An outpatient with an infection is not going to go through all this,” Tomaka says. “Pick the safest, most conservative route if you’re not going to be monitored. The value of finding out about an allergy is to get the most updated information.”
Next, check out the important questions to ask before taking any prescription medications.