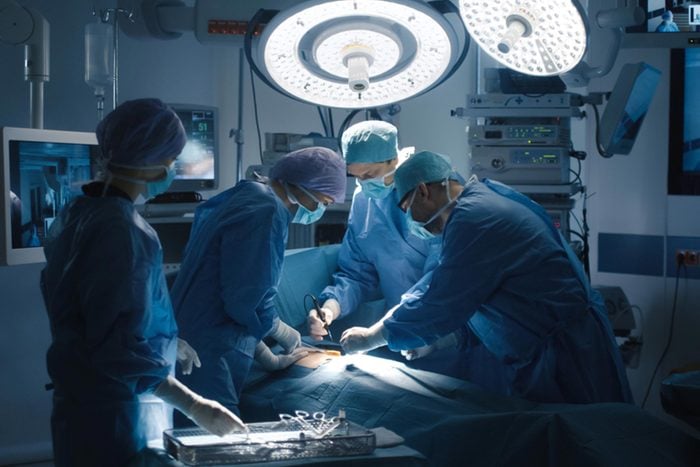
What happens under anesthesia?
If you’ve ever had a medical procedure where you’ve been asleep during surgery, you’ve been under general anesthesia. Anesthesia helps prevent pain, relax muscles, and keep you unconscious so that doctors can easily perform the procedure. But what really happens once you’re under? Here’s what anesthesiologists have to say.

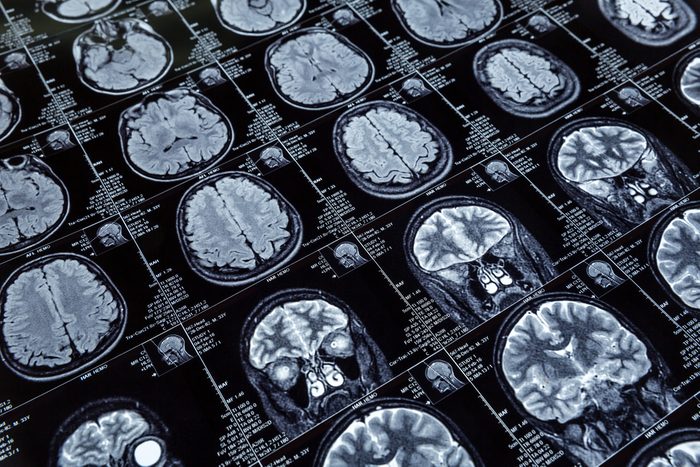
Your brain quiets down like it’s getting deep sleep
As the anesthesiologist asks you to count down from 100 in the operating room, here’s what’s taking place in your head: “A hypnotic agent is given to quiet the thinking part of the brain, the cerebral cortex, and areas of the brain stem associated with awareness,” explains Jennifer Kollman, MD, director of anesthesia at UCHealth Memorial Hospital Central in Colorado Springs, Colorado. You can expect your breathing to slow and your body to relax. “When you awaken, it’s almost like you’ve time-traveled, feeling like you only fell asleep moments ago,” says Dr. Kollman. “Some people even report dreams afterward.”
You might not fall completely asleep, though
Rarely—in about one or two out of 1,000 cases—a person might become aware during anesthesia, but they won’t usually feel pain, says James D. Grant, MD, president of the American Society of Anesthesiologists and chair of the department of anesthesiology at Beaumont Hospital-Royal Oak in Royal Oak, Michigan. “Anesthesia awareness can occur for a few reasons. There are some procedures, because of either urgency or unstable patient conditions, that warrant using lower doses of drugs that could place patients at a higher risk for awareness,” he says. These higher-risk procedures may include trauma, cardiac surgery, and emergency C-section delivery.

Your blood pressure could dip if you don’t know your correct weight
If you’re unsure how much you weigh, request a scale at the hospital so you can give the anesthesiologist an accurate number. “Initial dosing is often based on weight,” says Nitin Sekhri, MD, medical director of pain management at Westchester Medical Center in Valhalla, New York. “Giving a falsely low weight may lead to underdosing of both anesthetics and antibiotics. And giving a falsely elevated weight may lead to a higher-than-needed anesthetic dose, which could dangerously drop one’s blood pressure.” A too-low dose of antibiotics could increase your risk of infection.
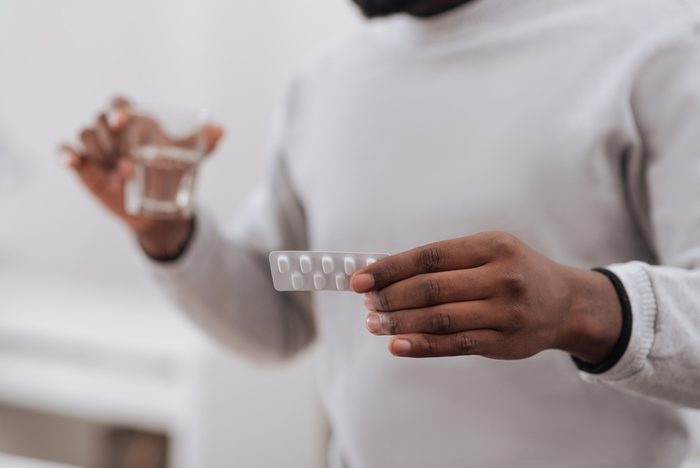
You could bleed too much if you didn’t stop taking your meds
Before surgery, your doctor will give you a list of medications you’ll need to stop taking prior to surgery. This typically includes blood thinners, ibuprofen, and supplements like omega-3s and ginkgo biloba; they all can increase the risk of excessive bleeding during surgery. But if you didn’t follow instructions, tell your anesthesiologist. “If you were told to stop your blood thinner on Friday and you forgot and did not do it until Monday, say something,” says Steven L. Mandel, MD, an anesthesiologist at the Ketamine Clinics of Los Angeles in California. Also discuss any medications and supplements you’re taking, including any recreational substances. “We are scientists, not DEA agents!” says Dr. Kollman. “Every drug with an action has a reaction, and those reactions require us to modify our medications to provide the best care for you. Help us help you.”

Your heart will work better without tobacco
“If you use tobacco products, seriously consider stopping them before surgery,” says Dr. Kollman. The ideal time to quit: three to four weeks before your surgery date. But, “even one day is enough to see improved heart and lung function,” she says. “The carbon monoxide clears from the red blood cells, allowing them to carry more oxygen to your tissues, which improves healing and decreases the risk of infection. It is, quite possibly, the biggest thing you can do to help yourself heal.” (Need help? Here are 22 ways to quit smoking for good.)

You could have problems breathing if your stomach isn’t empty
There’s a really good reason surgeons warn you not to eat several hours before an operation. While under anesthesia, “a person loses their ability to cough and protect their airway from having stomach contents enter the lungs,” says Dr. Sekhri. “While often a nuisance, not eating before a general anesthetic is crucial. If your stomach has contents inside of it at the start of the procedure, stomach contents can enter into the lungs causing severe, possibly life-threatening pneumonia.” If you did eat or drink something later than instructed, tell your anesthesiologist so they can come up with a plan of action.
You can still be uncomfortable
Be sure to talk to your anesthesiologist about any other conditions or issues that might cause pain, says Dr. Sekhri. “During your procedure, the anesthesiologist is the physician that is in charge of you outside of the surgical field,” he explains. So if you suffer from back pain, ask for a cushion to be placed under your back before you go to sleep. Shoulder discomfort? Request that your arm is positioned by your side during the surgery. You also can ask the anesthesiologist to put the intravenous catheter in your non-dominant hand.
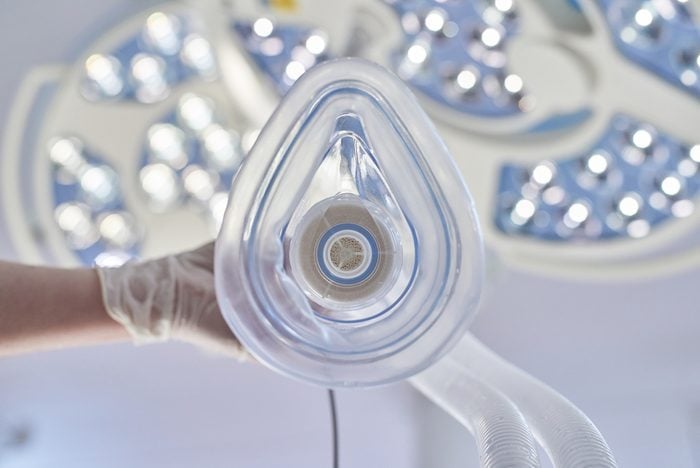
You might not need general anesthesia
General anesthesia has the advantage of keeping you unconscious and unable to move, according to the National Institute of General Medical Sciences. But many procedures only require local or regional anesthesia in which only certain parts of the body are numbed. Surgeons will typically offer these in procedures such as C-section delivery and some arm or leg surgeries. With these types of anesthesia, the patient stays conscious through the procedure. “We are big advocates of regional techniques due to their many advantages, good pain relief with fewer side effects, better safety, and fewer complications,” says Stanley Chang, MD, an anesthesiologist at Torrance Memorial Medical Center in Torrance, California.

You’ll be dehydrated
Because patients are typically instructed to refrain from eating and drinking before surgery, keeping well-hydrated for several days before the procedure is important. Carry a water bottle with you to remind yourself to drink. “Appropriate hydration prior to surgery may help with many side effects, including low blood pressure and nausea,” says Dr. Sekhri. (Check out these other ways to recover faster from surgery.)

You might become nauseated
But there are ways to minimize this risk. “Post-operative nausea and vomiting is a very common problem that is not only uncomfortable for the patient but can also keep a patient in the hospital longer,” says Dr. Sekhi. He suggests letting the anesthesiologist know if you have risk factors such as motion sickness or if you’ve experienced feelings of nausea after anesthesia in the past. “The anesthesiologist may elect to use less or no inhaled anesthetic, which tends to be more nauseating, or even to perform acupuncture on the wrist.” (This alternative therapy can effectively reduce nausea.) Post-operative nausea occurs more often with certain types of surgery, such as abdominal, pelvic, or inner ear surgery, notes Dr. Kollman.

You may have odd side effects
“Just as your anesthesia plan is tailored specifically for you, side effects can be personal as well,” says Dr. Kollman. “Some people are prone to postoperative nausea or headaches. Others may be slow to wake.” Shivering is another possible strange side effect. It happens because of the way anesthetics affect the brain, says Dr. Sekhri. Shivering typically happens a few hours post-surgery, and you can ask for medication to limit the effect. Also, men with prostate problems may experience a temporary inability to urinate following anesthesia. Make sure to discuss any potential issues with your anesthesiologist ahead of time.
Next, don’t miss these secrets hospitals won’t tell you, but every patient should know.
