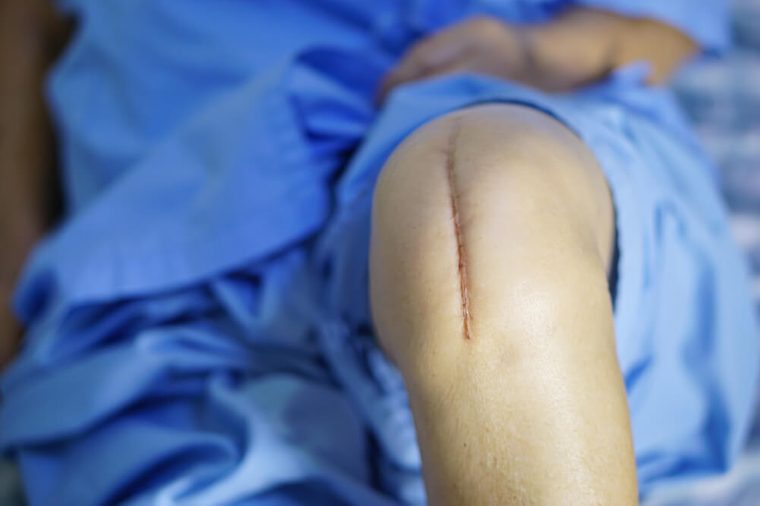
What is knee replacement?
Knee replacement means you’ve opted to replace your joint with an artificial one. It’s only an option when all other treatments—physical therapy, pain meds, injections, etc.—can no longer relieve your pain.
Why do joints fail? The pain results from lost or damaged cartilage that cushions the bones of the knee, says orthopedic surgeon, John V. Tiberi, MD. Risk factors include age and obesity.
The surgery, itself, involves replacing some of the damaged bone and cartilage in the joint with a smooth gliding surface made of metal and plastic, says Nashville orthopedic surgeon, Jeffrey Hodrick, MD.

Who is a candidate?
Typically, people get knee replacements because of arthritis: especially osteoarthritis, but also post-traumatic arthritis, rheumatoid arthritis, and other inflammatory arthritis such as gout, explains Jeffrey I. Peretz, MD, chief of orthopedic surgery at Emory St. Joseph’s hospital in Atlanta. (If your knees are aching due to rheumatoid arthritis, try eating this food.)
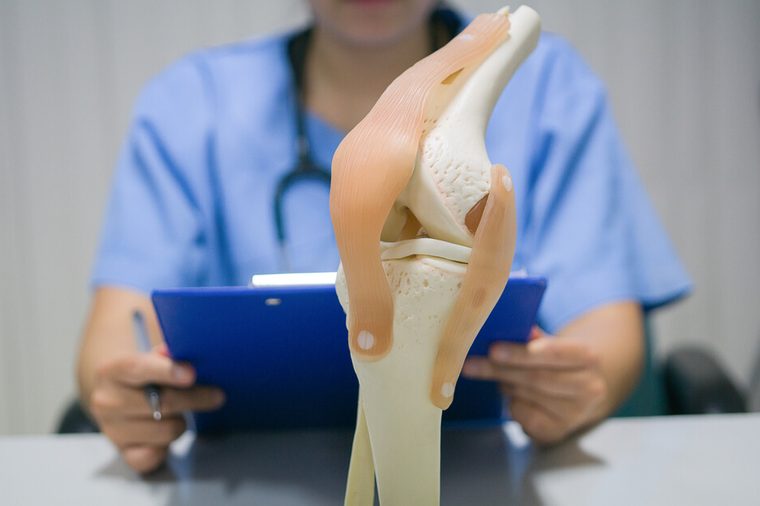
Types of replacement
Knee replacements can be either partial or total. The knee is divided into three compartments, explains Austin-based orthopedic surgeon, Barbara Bergin, MD.
- medial (inside)
- lateral (outside)
- anterior (kneecap)
Patients can get opt for partial replacement when only one part of the knee’s cartilage is damaged (usually the medial), according to Bradford Waddell, MD, an orthopedic surgeon at The Hospital for Special Surgery, who makes an evaluation based on listening to and examining the person and reviewing their imaging. That said, most replacements are total because arthritis tends to affect the entire knee, says orthopedic surgeon, Miho J. Tanaka MD, director of the Women’s Sports Medicine Program at The Johns Hopkins Hospital.
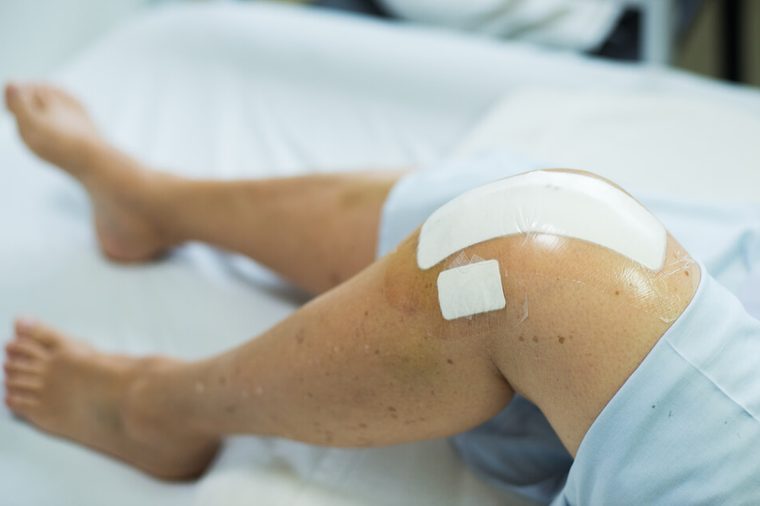
Preparing for surgery
When it comes to picking a surgeon, “research shows that the more of these surgeries the surgeon performs, the better the outcomes,” says Nakul Karkare, MD, a New York joint replacement surgeon. Once you’ve chosen your doctor, the best way to prepare is to follow the doctor’s orders to optimize your health, advises Dr. Peretz.
Since diabetes and obesity can negatively influence the outcome, according to Dr. Bergin, if you have these conditions, it’s best to get them under control. Another way of improving your odds of a good outcome, according to Dr. Hodrick, is to engage in “prehab,” a pre-surgery protocol involving exercises to strengthen the muscles around the knee. Keep in mind, you may need to fast and only drink water closer to your operation.

How long does the surgery take?
While the surgery itself can be accomplished between 30 to 60 minutes, with prep time and anesthesia the patient’s time comes out closer to two hours, according to Dr. Peretz. (Here are 50 secrets your surgeon won’t tell you.)
Anesthesia
California orthopedic surgeon, Timothy Gibson, MD says that, for a total knee replacement, surgical anesthesia will include:
- a spinal anesthetic (this numbs the legs during the surgery and for several hours after)
- a local anesthetic (at the knee)
A significant new advance, according to Dr. Gibson, is the use of a “nerve block,” which can extend pain relief into the days that follow. Pain after a partial knee replacement is much less severe, and a nerve block may not be given. (Here’s why you should never schedule an evening surgery.)
Managing pain after surgery
The severity of post-surgical pain depends upon the individual. The best way to manage it, according to Oregon orthopedic surgeon, James Van Horne, MD, is to prevent it from starting. Typically, opioid pain medication is used to ease the immediate, and more severe, post-operative pain. But patients are encouraged to switch to non-narcotic medication as soon as possible. “During my surgeries, I inject a non-opioid option called Exparel, which provides relief with decreased opioid consumption for 48 to 72 hours after surgery, in combination with other anti-inflammatories,” Dr. Horne says.

Do I have to be hospitalized?
Most total replacements require one to two nights in the hospital, says Russell G. Cohen, MD, an orthopedic surgeon at Tucson Orthopaedic Institute. However, other surgeons may choose to do it as an outpatient procedure, depending on their training and the hospital protocols. Partial replacements are more likely to be an outpatient operation. (Don’t miss these tips for improving your hospital stay.)

How long is the recovery?
Dr. Cohen describes the recovery as a year-long process that occurs in three phases:
- First six weeks: Heal, reduce swelling, and regain movement.
- Next three to five months: Build endurance and muscle strength through regular-life activity and exercise.
- Final six months: Continue to gain strength and mobility.
The first six to eight weeks
Starting the day of surgery, you should begin moving the joint and see a physical therapist (plan to go three times per week). In the first few weeks, you may need a walker or cane, says Dr. Peretz; some surgeons recommend patients not flex their knee beyond 90 degrees. People who like shopping can be walking in the mall in three weeks, says Eugene S. Krauss, MD, chair of Orthopedics at Northwell Health’s Syosset Hospital in New York. “Golfers should be hitting golf balls by six weeks.”

The next five months
At twelve weeks most patients are extremely active, says Dr. Krauss. Within the first six months, most people feel fully recovered. Within two to three months, many patients report feeling better than they did before surgery. Dr. Bergin adds that once the surgical incision is fully healed, patients should be encouraged to progress as aggressively as possible with rehabilitation. That said, doctors recommend holding off on high impact activities like running and doing squats.

Long-term recovery
Depending on how you feel, you should be able to return to all normal activities within six to 12 months, according to Dr. Krauss. Barring infection in the incision or other complications, says Dr. Bergin, patients should be as aggressive as possible with rehabilitation in order to get back their range of motion and strength. “The long-term outcome depends on their motivation and ability to continue to strengthen the knee and muscles around the knee for the first year after surgery,” says Dr. Peretz.

What are the best-case scenario results?
Knee replacement is one of the most satisfying surgeries in orthopedics, says Dr. Karkare. The best-case scenario involves a functional joint that remains pain-free for upwards of 30 years, according to Timothy Bollom, MD, a sports medicine specialist and orthopedic surgeon at The Center Orthopedic & Neurosurgical Care & Research in Bend, Oregon. Dr. Hodrick likes to see his patients “forget” they’ve had the surgery. Dr. Krauss says that many of his patients have returned to very active lifestyles, including playing racquetball and engaging in extreme hiking. For the more sedentary patients, it’s enough to go back to whatever they were doing before, be it shopping, dancing, or walking.
When and why do some knee replacements fail?
The most common reason for early failure is an infection, says Dr. Tiberi. Other causes include instability, loosening, and wear and tear. Most later failures are the result of persistent pain or mechanical symptoms (the joint locks or gives out), according to Dr. Bergin. “These factors are difficult to analyze because there are really no good studies to help us decide why a patient still has pain or dysfunction,” she says.

How long before you know if it was a success?
Most patients will know that their surgery was a success in the first two to three months after surgery, but sometimes it takes longer to recognize a failed replacement, according to Armin Tehrany, MD, founder of Manhattan Orthopedic Care. “When a patient feels increasing pain and/or decreasing function at least six months after surgery, the initial surgeon should be seen for evaluation.” (While you’re waiting to see if your surgery was a success, here are some ways to develop a positive outlook.)

How to avoid knee replacement
For some, knee replacements are inevitable due to genetic predisposition to arthritis. “It isn’t possible to prevent arthritis or slow down the progression,” says Dr. Tiberi. But you can help prevent an arthritic knee from being so painful that you require surgery, he says, by maintaining a healthy body weight (here are the signs you’re already at a healthy weight) and an active lifestyle. Try low impact exercise to keep leg muscles strong. In addition, studies indicate there may be hope for using stem cells to treat knee pain in the future, according to Dr. Tehrany. Next, check out some natural remedies to try before you start thinking about knee replacement.

