Answers to your most common heart attack questions
Every 43 seconds, someone has a heart attack. Could that someone—someday—be you? Long thought of as an “old man’s disease,” heart attacks don’t really discriminate, affecting young and old, women and men. In a study published in 2018, in the journal Circulation, researchers looked at more than 28,000 people hospitalized for heart attacks between 1995 and 2014. They found that 30 percent were young (specifically, ages 35 to 54) and the proportion was especially pronounced among women. But knowledge, of course, is power. Here’s what you need to know about heart attacks.

How will I know if I’m having a heart attack?
The number one rule: don’t diagnose yourself. If you have the slightest suspicion that you may be having a heart attack, call 911. Since about half of heart attack deaths happen within the first hour following an attack, waiting several hours before calling for help could be deadly. If you have any of the following symptoms, dial 911.
Chest discomfort: Most heart attacks involve discomfort in the center of the chest that lasts for more than a few minutes, or goes away and then comes back. It may feel like an uncomfortable level of pressure, squeezing, fullness, or pain.
Upper body discomfort: Pain in one or both arms, the back, neck, jaw, or stomach could signal a problem.
Shortness of breath: This symptom may occur with or without chest discomfort.
Other signals: Pay attention to body symptoms you don’t normally experience, such as breaking out in a cold sweat, nausea, lightheadedness, overwhelming fatigue, or a feeling of impending doom. (Don’t miss these 15 lifesaving tips to prevent heart disease, according to a holistic heart doctor.)

Will I get that “elephant on the chest” feeling I’ve heard about?
Maybe, maybe not. “A heart attack may occur without the sensation of an ‘elephant sitting on your chest,’ ” says Prashant Vaishnava, MD, a cardiologist at the Mount Sinai Hospital and assistant professor of medicine at the Icahn School of Medicine at Mount Sinai in New York City. In a heart attack, blood supply to the heart muscle is interrupted and heart muscle cells start to die, which may cause chest pain—but sometimes it doesn’t, especially in women. Most heart attacks build up slowly, with mild pain or discomfort.
“People may experience symptoms distinct from chest pain that could still suggest there is a compromise in blood flow to the heart,” says Dr. Vaishnava. “These symptoms could include shortness of breath, chest burning, stomach pain, trouble swallowing, arm pain. It is important to know that a heart attack could manifest with a range of symptoms; it is also useful to keep in mind that these symptoms usually represent something else and not a heart attack.” Here are 11 signs you might be headed for a heart attack.

Can I have a heart attack and not know it?
Surprisingly, yes. In a study of middle-age and older people who’d experienced a heart attack, published in 2015 in JAMA, almost 80 percent showed no signs of a heart attack during medical follow-ups. What’s known as a “silent heart attack” can happen to anyone, but people with diabetes are more likely to have one that those without the disease. You may not experience any of the well-known symptoms, like chest pain, but you may feel nauseous, short of breath, or even faint. Here are the 7 signs of a silent heart attack.

Is there any time of day when I’m more likely to have a heart attack?
A heart attack can strike at any time, but it occurs most frequently in the early hours of the morning. Research, including a study published in 2018 in Circulation Research, suggests that’s because people with cardiovascular disease have lower levels of protective molecules in their blood in the morning, which could be increasing their risk of blood clots and heart attacks in the a.m. hours. A review of research, published in 2015 in Circulation Research, found that sudden cardiac death peaks from 6 a.m. to noon, and is highest on Monday and lowest over the weekend.

What should I do if I think I’m having a heart attack?
Call for an ambulance immediately, and stay calm. “Stay on the phone with the 911 operator, if possible,” says Dr. Vaishnava. “If your doctor has prescribed nitroglycerin, you should consider taking it. Try to gather your ID and insurance card, but don’t stress yourself or exert yourself physically in any way.”
While you wait for the paramedics, sit or lie still, and slowly chew and swallow an aspirin—aspirin helps minimize heart damage or development of a dangerous blood clot by reducing the “stickiness” of the platelets that play an important part in blood clotting. Also, make sure your door is unlocked so emergency responders can get into your home. Don’t eat or drink anything, and phone a relative, neighbor, or friend to come wait with you.
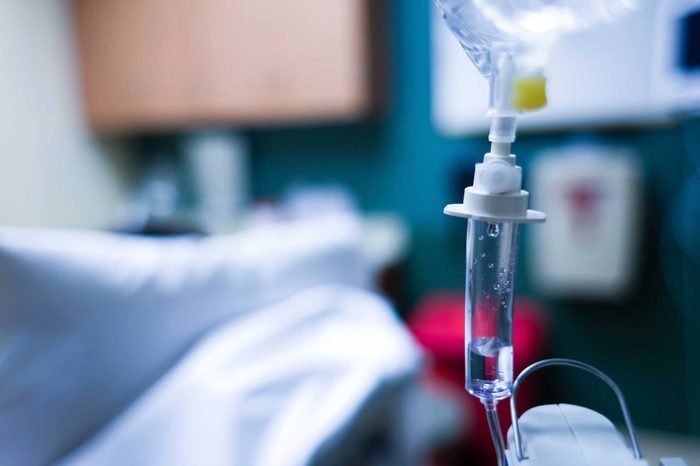
What can I expect once I get to the hospital?
First, the staff will hook you up to a cardiac monitor and intravenous drip. “If the paramedics didn’t perform an electrocardiogram (EKG), that will be performed immediately” to detect any irregular rhythm or other abnormalities that indicate a heart attack, says Dr. Vaishnava. This painless test records your heart’s electrical activity through 12 small electrodes placed on your chest, arms, and legs. “The results of the EKG dictate the next step.”
If they reveal you’re having a major heart attack, in which an artery feeding your heart is blocked, choking off the blood supply to part of your heart muscle, you’ll quickly receive treatment to open the blocked artery. If that isn’t the case, “you’ll be stabilized in the emergency department,” says Dr. Vaishnava. “You may receive a blood thinner called heparin and lab tests called cardiac enzymes which guide further decision making.”
Depending on your condition or the severity of your attack, doctors may keep you in the hospital until the best treatment is determined. These are the 16 heart-health secrets cardiologists want you to know.
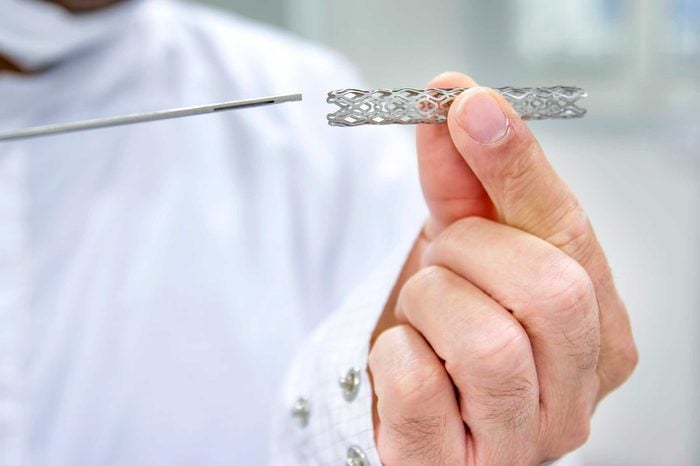
Will I have to have surgery?
If you reach the hospital quickly, doctors may try to open up your coronary arteries mechanically in a procedure known as angioplasty. A thin tube with a balloon at the tip is threaded up from your groin to your coronary artery, and a small amount of dye is injected so that the site of the blockage can be seen using an x-ray video. The balloon is inflated to widen the artery, and when the tube is withdrawn, a small metal coil known as a stent is usually left in place to keep the artery open and prevent further blockages. Some stents can also release medication to keep the artery clear.

Can I exercise after a heart attack?
Research, including a study published in 2018 in the Journal of the American Heart Association, shows that people who increase their physical activity in the year following a heart attack reduce their risk for early death, as compared to those who stay physically inactive. Exercise actually lowers your risk of suffering a second heart attack, but first talk to your doctor to find a routine–whether it’s walking, jogging, cycling, or swimming–that is safe for you. Never start training until the doctor gives you the all-clear. (This is the one thing at the gym that could save your life.)

Will I be able to have sex after a heart attack?
Once your doctor gives you the green light to engage in moderate exercise, it’s safe to be intimate. Most people are able to start having sex again within two or three weeks of having a heart attack, but always check with your doctor first. A study published in 2015 in Journal of the American College of Cardiology found no relevant risks to resuming sex among participants who were able to engage in mild to moderate physical activity, such as climbing two staircases or taking a brisk walk, so long as you can do these things without experiencing chest or neck discomfort, fatigue, or shortness of breath, says cardiologist Michael Miller, MD, professor of medicine at the University of Maryland School of Medicine in Baltimore, Maryland, and the author of Heal Your Heart. Don’t miss the 45 heart health tips cardiologists follow.