What Is Cholesterol?
Updated: Sep. 07, 2021
Different types of cholesterol aren't inherently good or bad. But too much or too little of the wrong kind can be dangerous.
Cholesterol is a public health issue
Think of high cholesterol as one of the world’s most notorious public-health offenders. Close to 100 million Americans have unhealthy cholesterol levels, putting them at grave risk of having a heart attack, stroke, or other cardiovascular issue.
Getting and keeping cholesterol at normal levels can greatly reduce that danger.
“Cholesterol is one of the keys to good health,” says Daniel Muñoz, MD, associate professor of medicine at Vanderbilt University Medical Center. “Part of the reason we focus so much as physicians: in general, we know by identifying opportunities early we can prevent a lot of cardiovascular disease down the road.”
Here’s what you need to now about this all-important feature of good health.
What is cholesterol?
Cholesterol is typically described as a “waxy” substance found in your bloodstream and in every cell in your body. It doesn’t start out “good” or “bad.” It’s simply necessary.
“It’s a type of fat. We need it to live,” explains Michael Goyfman, MD, director of clinical cardiology at Long Island Jewish Forest Hills in Queens, New York.
The nutrient plays a specific and necessary role in the body. “It helps build cell membranes and helps make vitamin D and hormones,” says Sonya Angelone, RDN, a national spokesperson for the Academy of Nutrition and Dietetics.
Because fats are not water soluble (remember, cholesterol is waxy), they can’t mix with blood, which is watery. So they’re transported by higher-density protein molecules via the bloodstream to every cell in the body. This combination of fats, or lipids, and proteins is called lipoproteins.
Your liver is usually capable of producing all the cholesterol it needs (that in itself tells you how essential is, says Angelone). Excess cholesterol can be made by the liver usually as a result of eating animal-based foods high in saturated and trans fats, explains Dr. Muñoz.
Types of cholesterol
There are several different types of cholesterol but two, in particular, can impact your health. The first is low-density lipoprotein (LDL), which has the reputation of being bad for you. The other is high-density lipoprotein (HDL), or “good” cholesterol.
“Density” refers to how much fat the molecule has compared with protein, explains Dr. Goyfman. Fat molecules are less dense than protein, so low-density cholesterol means there’s a lot more fat than protein. On the flip side, HDL has less fat and more protein.
HDL and LDL are, in a sense, polar opposites. Yin and yang. While too much LDL can contribute to plaque and block your arteries, “HDL functions as a law enforcement officer or scavenger to mop up excess cholesterol,” explains Dr. Muñoz.
They work well in tandem but, “like with most anything, too much and the wrong kind is bad,” says Angelone.
Less-famous types of cholesterol play additional roles in transporting cholesterol throughout the body, explains Dr. Goyfman. These include:
- Very-low-density lipoprotein (VLDL), which veers towards the “bad” end of the cholesterol spectrum
- Intermediate-density lipoprotein (ILD)
- Chylomicrons, which carry cholesterol from food
- Remnant-like particles (RLP)
Doctors sometimes calculate a person’s non-HDL cholesterol, particularly if the patient’s risk for heart problems is especially high. This number is your total cholesterol level minus HDL, and it accounts for types of cholesterol like VLDL and ILD.
How too much LDL cholesterol can lead to heart disease
HDL helps protect your health by absorbing cholesterol and bringing it back to the liver, which removes it from your body. But in cardiology the spotlight is on LDL. It is, says Dr. Muñoz, “an ingredient in the recipe of blockage.”
And blockages in the arteries are what cause heart attacks, strokes, and more. After all, your arteries are essential for supplying blood to your heart.
This is how it works: Excess LDL cholesterol can bind with other substances to form a sticky substance (plaque) that coats the walls of the arteries and narrows them. This decreases blood flow to your heart.
The eventual result is atherosclerosis, a hardening of the arteries.
If a piece of the plaque breaks off and forms a blood clot, blood flow is obstructed, possibly resulting in a heart attack (if the artery supplies the heart), stroke (if the artery feeds into the brain), or problems elsewhere in the body.
Causes of high LDL cholesterol
Unhealthy lifestyle habits are the main drivers of high LDL cholesterol.
Although diet (including eggs) plays less of a role than we used to think, foods high in saturated and trans fats (such as fatty meats and dairy, baked goods, and deep-fried and processed foods) can contribute to an overload of LDL cholesterol.
Also putting you at risk:
- Smoking
- Lack of exercise
- Being overweight or obese
- Shouldering a lot of stress
- Consuming too much alcohol
These are all risk factors you can control. The ones you can’t control include:
- Genetics (including a condition called familial hypercholesterolemia), which may make you more likely to develop high cholesterol
- Age—cholesterol levels rise as you get older
- Race or ethnicity, which can influence your risk for high LDL and/or low HDL levels
Some medical conditions can also cause high LDL and/or low HDL, such as diabetes, chronic kidney disease, HIV/AIDS, pregnancy, sleep apnea, and lupus.
Medications that can contribute to unhealthy cholesterol levels include some drugs for your heart (beta blockers and diuretics), cyclosporine and other immune-suppressing drugs, steroids, and retinoids for acne.
Screening and prevention
Most people with high LDL and/or low HDL don’t show any symptoms, which is why regular screening is so important.
The American Heart Association recommends that all adults age 20 and over who have an average risk for high cholesterol get their levels tested every four to six years. Once you turn 40, your doctor may recommend more-frequent checks, depending on your risk factors for heart disease.
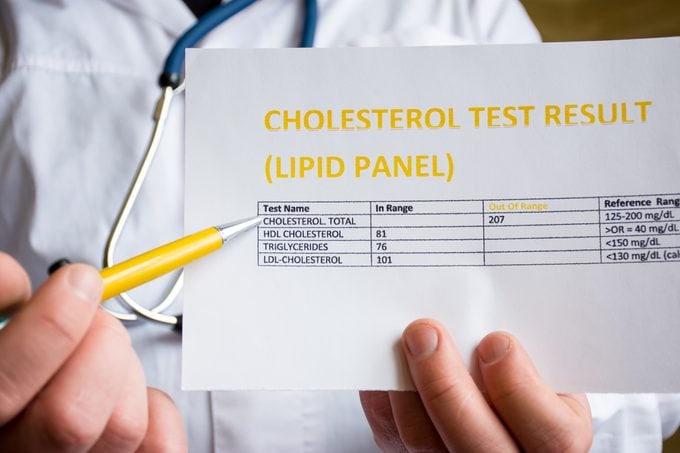
Screening is a simple blood test called a lipid panel that’s ideally done by your doctor. The results will show total cholesterol, LDL, HDL, and triglycerides (another type of fat).
There are also home tests. According to the Food and Drug Administration, some—but not all—can be as accurate as the ones done in a doctor’s office. If you go with one of these, look for tests that are “traceable” to the Centers for Disease Control and Prevention and check the label for information on accuracy.
Healthy cholesterol levels
The National Cholesterol Education Program, part of the National Heart, Lung, and Blood Institute, provides the following guidelines for healthy cholesterol levels in adults age 20 and older.
LDL cholesterol
Optimal: Less than 100 mg/dl
Near/above optimal: 100 to 129 mg/dl
Borderline high: 130 to 159 mg/dl
High: 160 to 189 mg/dl
Very high: 190 mg/dl and above
HDL cholesterol
Low: Less than 40 mg/dl
High: 60 mg/dl and above (this is protective)
Total cholesterol
Desirable: Less than 200 mg/dl
Borderline high: 200 to 239 mg/dl
High: 240 mg/dl and above
While doctors do look at total cholesterol levels, “we care as much, if not more, about LDL specifically,” says Dr. Muñoz.
Lowering your LDL cholesterol with lifestyle changes
If you need to lower your LDL levels, start with the lifestyle issues that may be contributing to your too-high cholesterol.
A good place to start is your diet. Certain foods worsen the condition, but there are also foods that can help lower your cholesterol levels.
The only diets that have proven long-term beneficial effects on heart health are the DASH and Mediterranean diets, says Dr. Goyfman. Both are low in saturated fat and focus on unsaturated fats, lean proteins, fruits, vegetables, and whole grains.
Try to exercise for 30 minutes, most days of the week. And get enough quality sleep.
All of these actions will help you maintain a healthy weight, which is also critical for keeping cholesterol levels low. Losing as little as 3 to 5 percent of your body weight can alter your cholesterol levels for the better.
Lowering your LDL cholesterol with medication
You may need medication if you’ve had a previous heart attack or stroke, have diabetes, or have an LDL level above 190 mg/dl. Doctors usually first turn to statins, drugs that prevent your liver from making cholesterol.
“Most patients are easily enough controlled with statins,” says Dr. Goyfman. “That’s really the cornerstone.”
If statins don’t do the trick, your doctor may turn to non-statin cholesterol-lowering medications. Ezetimibe (Zetia) is the top option, followed by newer, injectable PCSK9 inhibitors. The PCSK9 inhibitors, Dr. Goyfman adds, “are considered game-changers. They can control cholesterol in most patients.”
Is there such a thing as too-low LDL or too-high HDL?
Technically, yes. But it hardly ever happens.
In fact, no one really knows what too-low LDL means, although some say it’s probably less than 40 mg/dl.
“Since we know that cholesterol is a component of cell membranes, you’re definitely going to have problems if it gets too low, but it’s not a problem for most people,” says Dr. Goyfman.
Levels of HDL beyond target ranges could theoretically add some benefit, but, says Dr. Muñoz, “we very rarely get to that person.”