Why Are Kidney Stones So Painful? Two Women Share Their Journeys
Updated: Apr. 26, 2021
Two women share their painful ordeals dealing with kidney stones. Doctors discuss causes, possible prevention, and treatments.

When Yolanda Alonso, 49, of El Escorial, Madrid, first felt the twinge in her right side, she assumed she was ovulating. Over the next couple of days, though, the pain escalated, reminding her of the excruciating contractions she experienced when giving birth to her now teenaged daughter. But labor pains wax and wane. These were unrelenting.
Soon, Alonso could barely function. Frightened, she had her husband take her to the nearest hospital emergency department. After X-rays and other tests, doctors returned their diagnosis: She had a kidney stone.
Passing a kidney stone
Alonso was given IV painkillers and sent home with pain pills to take while she waited for the kidney stone to work its way out of her system. The pills helped for a few days “until I had another severe attack, and I went back to hospital and had intravenous medication again.” Finally, her agony abruptly ended. The stone passed on its own.
Kidney stones are one of the most painful conditions known. Considering their tiny size—typically just a couple of millimeters (about half the length of a grain of rice)—it’s surprising that they can cause such debilitating symptoms. And for so many people.
“One out of 10 [people] will develop a stone,” says Thomas Knoll, MD, PhD, an associate professor of urology at Mannheim University Hospital, Germany, and head of the department of urology at Sindelfingen Medical Center, University of Tuebingen, Germany. In the United States, the prevalence of kidney stones is 8.8 percent as of the late 2000s—an increase from 3.8 percent in the late 1970s—according to the National Kidney Foundation. Men have about a 19 percent lifetime risk of developing kidney stones, compared to a 9 percent risk in women.
How kidney stones form
Various substances circulate through your body all the time; any excess is sent to the kidneys for disposal. The more urine you produce, the more likely your body is to flush away this excess. But when minerals and other substances clump together before they can be expelled, kidney stones can form.
The typical kidney stone is usually a combination of calcium and an organic acid called oxalate. A kidney stone also can develop from uric acid, the culprit in gout. (Not surprisingly, gout predisposes people to produce kidney stones.) Calcium can also combine with phosphate to form stones. Other minerals also can be responsible for people with a genetic propensity towards kidney stones, according to the National Kidney Foundation.
A kidney stone usually only makes its presence known after it leaves the kidney. If it gets stuck in the ureter (the tube that carries urine from the kidney to the bladder) and blocks the flow of urine, the pain can be extreme. It’s the body’s unsuccessful attempts to push through the blockage that causes the pain.
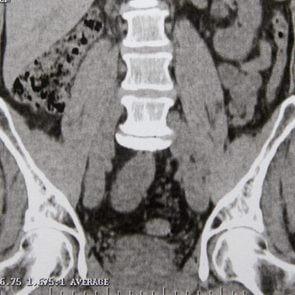
To confirm that pain is due to a kidney stone, doctors first use X-rays and sometimes CT scans, which can be helpful in detecting tiny stones. Blood and urine analysis can show whether abnormal levels of stone-forming substances are circulating through your system.
What are the main causes of kidney stones?
Dehydration is a major risk factor. “If people don’t drink enough, they have a higher risk of stone formation,” says Dr. Knoll.
But dehydration isn’t the only cause. As we grow in bulk, becoming a more overweight population, we also grow more prone to kidney stones. It’s not just how much we eat, but what we eat.
“A diet that is rich in meat, primarily red meat, contributes to the stone formation risk,” says Hendrik Heers, MD, a urologist at Oxford University Hospitals in the U.K. “Vegetarian patients have a much lower risk of kidney stones compared to the meat-eating population.”
A diet heavily reliant on processed food, such as canned, frozen, and other packaged fare, also can increase the risk of stone problems, according to the National Institute of Diabetes and Digestive and Kidney Diseases. Processed foods tend to be high in sodium (salt), and excess salt increases the amount of calcium you excrete in your urine.
While kidney stones are most often a problem for the middle-aged and older, according to a study published in The Journal of Urology, children too, especially adolescents, are susceptible. The incidence of kidney stones in those younger than 18 has increased dramatically in the past 25 years. “That is absolutely, from my point of view, related to the diet,” says Palle J.S. Osther, MD, PhD, professor of urology at Lillebaelt Hospital in Fredericia, Denmark.
No one is immune to kidney stones

When she was 18, Rushka Robert was stunned by a sudden agonizing pain in her right side. Writhing and vomiting, the young Amsterdam native barely managed to make it to bed. Her mother, a former nurse, assumed it was appendicitis. When they called their doctor, however, he immediately suspected kidney stones. The ambulance crew gave Robert a fast-acting shot of painkillers, and at the hospital, her doctor’s diagnosis was confirmed.
The next day, after more painkillers, Robert was sent home to wait for the stone to pass. But it didn’t, and the pain worsened. She couldn’t urinate at all. Back in the hospital, Robert was told that they had to operate. Surgery was successful—but that wasn’t the end of her battle.
How to prevent kidney stones (again)
If you’ve had one bout with kidney stones, you have as high as a 50 percent chance of having another. “And you have about a 20 percent risk of having three or more stone episodes,” says Dr. Heers.
Watch your fluids
New problems often can be prevented with a few simple lifestyle changes. “Drink a lot to reduce the risk of getting a new stone,” says Dr. Osther. Aim for two liters (about 8.5 cups) of urine production a day, he says. To hit that target, you should drink at least two and a half liters (10.5 cups). “And when the weather’s warm, you should drink even more.” Those with a genetic propensity to form stones should double those amounts.
Although water is an obvious choice, other fluids might be even more effective. Coffee drinkers tend to have lower risks of kidney stones. But citrus juices take the prize, says Dr. Knoll, especially lemon and grapefruit. “They elevate the pH level of the urine,” he says. In other words, citrus makes your urine more alkaline, in which case “you reduce the risk of almost all stone formation.”
Avoid citrus drinks with sugar though, as the sweetener can increase your risk, undoing the good the juice by itself does. Find out if cranberry juice is good for kidney stones.
Limit certain foods
Depending on the chemical makeup of kidney stones, your doctor might advise you to limit certain foods. Meat and eggs are high on the list, as is shellfish, but plant-based foods with a high oxalate content such as peanuts, rhubarb, spinach, beetroot, chocolate, and sweet potatoes can also cause problems for some.
Sometimes, however, changing your diet just isn’t enough. For those with uric acid stones, a gout medication called allopurinol is often prescribed to reduce their incidence.
Diuretics in the thiazide family (hydrochlorothiazide, chlorthalidone, and indapamide) can reduce the amount of calcium excreted by the kidneys and help prevent calcium-based stones.
When kidney stone prevention isn’t enough
But for some, like Robert, prevention is not so straightforward. Just two years after her surgery for her first kidney stone, she experienced many of the same symptoms again. This time, she was completely disheartened.
She had done everything her doctors had recommended, including cutting back on dairy and sugar and avoiding spinach altogether. Yet X-rays showed almost two dozen stones sitting in her kidneys. Although she was able to avert another surgery, Robert experienced three more stone-related ordeals before a new doctor offered the most promising preventive medication: potassium citrate pills.
Now 26, Robert is taking 12 potassium citrate pills a day. “After six months, a new count showed just two stones on the left and one on the right,” she says. She’s hopeful that the medication will keep her stone-free.
Kidney stones treatment
Until relatively recently, medications that treat high blood pressure (nifedipine) and enlarged prostate (tamsulosin) were routinely given to hurry the expulsion of stones. But a large study published in The Lancet showed that these medications are no better than placebo at speeding passage. The current thinking is to treat only for pain while waiting for stones to make their own way out. Of course, not everyone does.
“The bigger the stone, the more unlikely is a spontaneous passage,” says Dr. Heers. Occasionally, even a small stone will get stuck in the ureter. Surgery is then the answer, but it’s almost always minimally invasive.
The three most common types of surgical treatment are:
Shockwave lithotripsy: Sound waves are focused on the stone from outside the body, breaking it into smaller pieces that can be passed in the urine. Pros: Least invasive. Usually an outpatient procedure. Cons: If the stone has a very hard composition more than one treatment is often needed.
Ureteroscopy: A small tube is inserted into the urinary tract and the stone is either pulled out or a laser is used to break it up. Pros: The most successful method for removing small to medium stones. Often an outpatient procedure. Cons: There is a slight risk of damage to the ureter. Sometimes a catheter must be left in place until the stone passes.
Percutaneous nephrolithotripsy: A small incision is made in the back directly into the kidney so that stones can be accessed and removed. Pros: Most successful method for removing larger stones. Cons: More invasive than the alternatives, requires a hospital stay and longer recovery time.
Remember, seek immediate medical help if you experience sudden, severe kidney pain, whether or not blood appears in your urine.
Next up, learn about the warning signs of kidney disease.