
Sure, I can give you some meds to dampen the pain
We spoke to some of the top pain specialists around the country (see the “Sources” below for more info). And they all agreed that the best doctors will talk to you about the possible causes of your pain, whether it’s your lack of activity, your stress level, a condition like arthritis, your mattress, or one of these surprising back pain causes.

Heat or ice?
Use an ice pack for acute injuries, to minimize blood flow and reduce swelling and pain. Use heat to loosen muscles and stiff joints and help you feel more mobile. (Heat or ice? Here’s a guide to injury treatment.)

Any doctor can hang a shingle that says ‘I treat pain’
Look for doctors who are board-certified in pain medicine or who did a fellowship in something pain-related. (Here’s what you should know about pain management.)
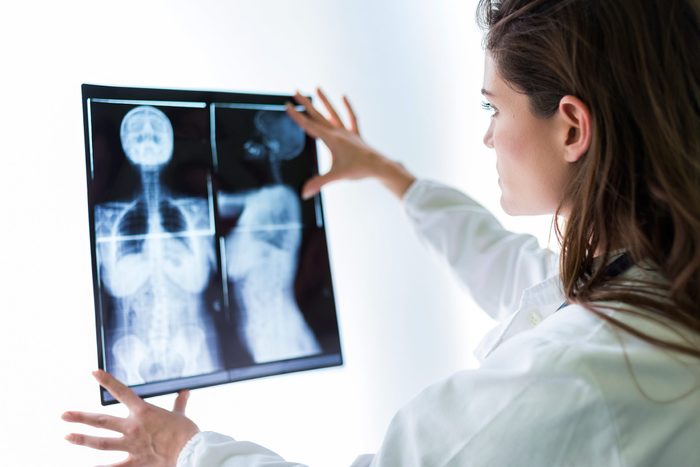
Your back and neck (and often shoulder) pain may have little or nothing to do with your abnormal MRI
Studies show that if you perform an MRI on any 100 people, you’ll find an abnormality in about 90 percent of them, even if they’re not experiencing any pain. (These are the sciatica symptoms you should know.)
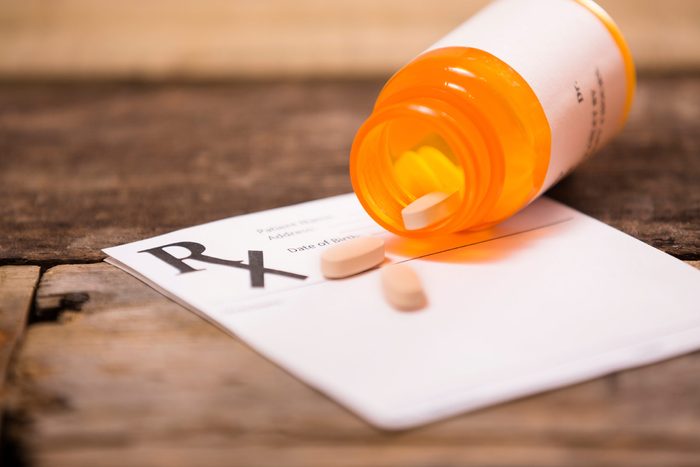
Reconsider before asking for a prescription
The latest research shows that taking opioid pain meds (like Vicodin and OxyContin) for chronic pain can change the brain, damaging its ability to feel pleasure and leading to a craving for more drugs. A few studies found that long-term use can actually lead to increased pain. There are many other options to treat pain, including non-opioid medications.

In mild pain? Play word games or another favorite challenging puzzle
When you distract your brain, you don’t hurt as much. Another activity that helps: watching a funny TV show.
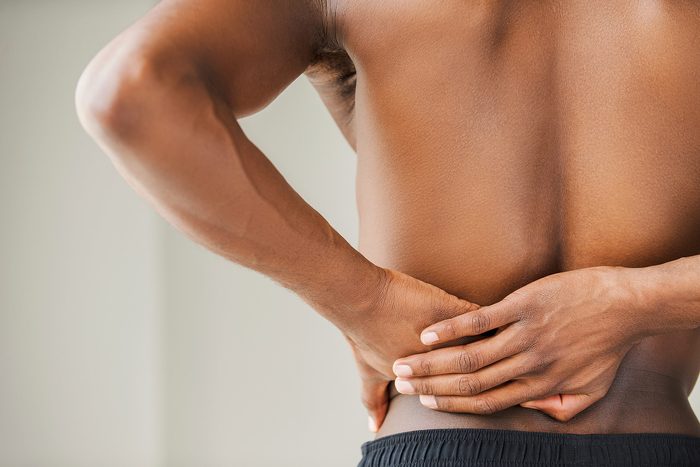
Before you praise me for curing your back pain, remember this
It may have gone away on its own. Approximately 90 percent of low-back pain subsides within 12 weeks without medical intervention.

If you have chronic pain, consider experimenting with dietary changes
Eliminate dairy for a few weeks, then reintroduce it and see how you feel. Do the same with wheat, red meat, shellfish, citrus, peanuts, caffeine, and alcohol, one at a time. If your pain gets worse when you add back a food, it may be contributing to your problem. Here are anti-inflammatory foods you can eat to help reduce pain.
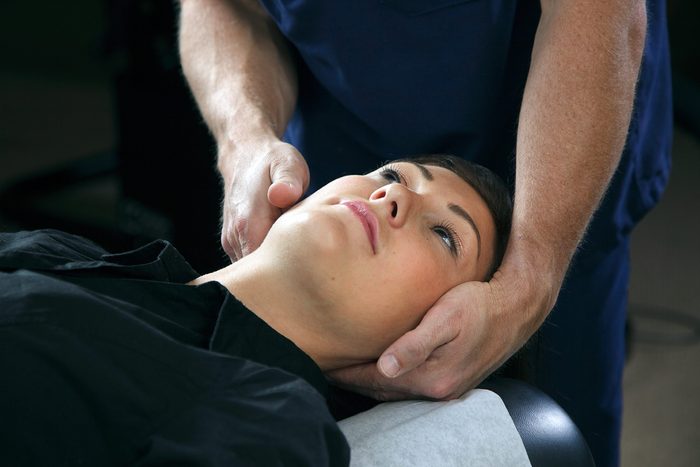
If I specialize in prescribing narcotics, giving injections, or doing surgery, that’s probably what I’m going to recommend
But there are dozens of other options to try like massage, physical therapy, chiropractic, acupuncture, spinal cord stimulators, and behavioral therapy. If you want to explore these options, work with an integrative medicine doctor to explore different natural and conventional methods of treating pain. And don’t forget nutrition, sleep, exercise and stress reduction.

Think twice about having surgery, especially on your back or spine
I’m in a practice with only three doctors, and between us, we have over 1,000 patients who had back surgery who wish they never had. In a Consumer Reports survey, just 60 percent of those who had back surgery were completely or very satisfied with the results. (Here’s how one woman with a herniated disc healed through mind-body exercises.)

Pain is mental too
Your brain can make your pain feel worse. So you may want to explore psychotherapy, cognitive behavioral therapy, meditation, and even self-hypnosis. (Here’s how to trick your brain into feeling less pain.)
If the doctor takes only cash (not insurance) and hands you a prescription after just a few minutes, you may be at a pill mill, not a full-service pain clinic
Most legitimate pain clinics take insurance and offer treatments beyond medication.

Your pain may improve with the right kind of exercise
Specifically, aerobic exercise fives times a week and regular practice of yoga and t’ai chi have been shown to help. Pain will also feel worse if you don’t get a good night’s sleep. (Here are sleep doctors’ tips for deeper sleep.)

Pain medications are known for causing severe constipation
Always ask about a stool softener, or try one of these constipation home remedies.
Before you come to me, try taking Tylenol or Advil for a few days
Simple, but it may work. And in some cases, the may be just as effective as opioid painkillers. Be aware, though, that overuse can result in rebound pain, liver issues, bleeding and ulcers.

Surgeons and orthopedic doctors who prescribe narcotics after surgery tend to under-dose
That’s because they’re worried about creating an addiction. If you’re still in pain after a procedure, it’s OK to ask for more. Social support can actually cut down on the need for pain meds.

To many insurance companies, the treatment of pain is an elective procedure, not a medical emergency
Be prepared to fight to get your treatment covered.
Diagnosed with spinal stenosis?
If you’ve been diagnosed with spinal stenosis, a narrowing of the spinal canal, and your doctor says you could be paralyzed if you don’t have surgery, find another doctor. Studies have shown that’s not true, and surgery should be a last resort only after you’ve tried other options.

Try injections for carpal tunnel
Injections for carpal tunnel syndrome have the highest success rate of any procedure. It should definitely be something you try before you resort to surgery. Here are some home remedies to try for carpal tunnel syndrome, too.
Please don’t take it personally when I ask you to take a drug test
We want to believe that you’re not addicted, but 3.3 million people in the U.S. are abusing prescription pain relievers, and we don’t want to be responsible.

You may never be 100 percent pain-free
Especially if you’re experiencing chronic back or knee pain. In many cases, we consider your treatment a success if we get rid of 50 percent of your pain and help you to be more functional.
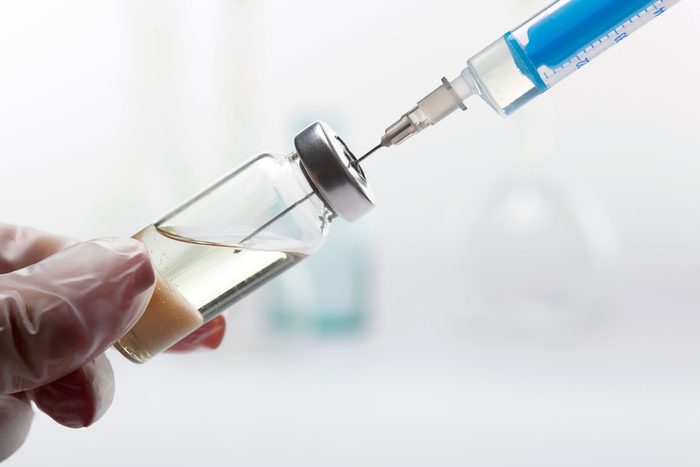
Steroid injections are now a top treatment for back pain in America
But critics say there is little evidence of any long-term benefit compared to their risks, especially for back pain that doesn’t radiate down the legs.

We’re incentivized to find ways to treat you
Pain doctors are paid about five to 10 times more for doing a procedure on you than for counseling you about how to prevent pain. Nerve blocks and injections are very lucrative, especially if you do them assembly-line-style all day long.

Get out of bed!
For every day you’re lying there, you lose 1 to 3 percent of your muscle strength, and then you start to feel stiff simply because you’re not moving. Your pain will get better faster if you stay active. Make sure you avoid these things that only make pain worse.
