Sometimes you need the strongest meds
Any doctor will tell you they must use the right tool for the job: If a patient’s pain is overwhelming, a doctor will have to bring out the most powerful solution—and that can mean opioids, despite the addiction risk of this class of painkillers. But there are safe and sensible ways to use opioids, as the Centers for Disease Control and Prevention (CDC) outlines. First, opioids are no longer a first-line—or routine—therapy for chronic pain. If someone isn’t responding to other medications, opioids can help—but it’s important for people to work with their doctor to establish treatment goals. Doctors and patients also need to check in regularly to review the goals and the patient’s progress—and consider alternatives, if necessary. Here’s how doctors feel about the various pain medications they use—and don’t use.
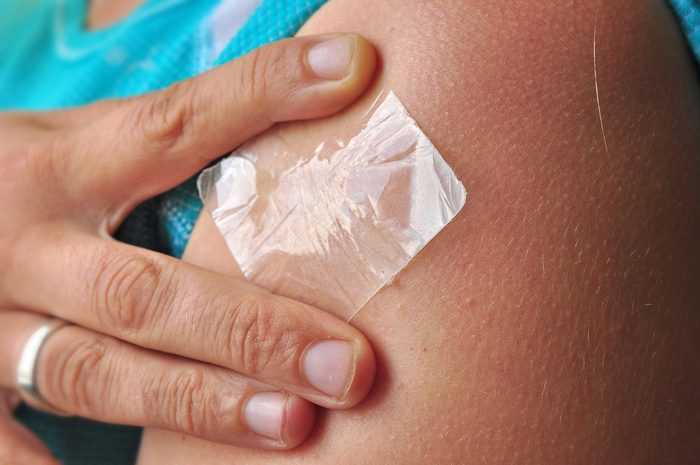
Fentanyl patches
“Fentanyl patches are extremely potent, addictive, and deadly. Fentanyl is a synthetic opioid that is similar to morphine; however, it is 50 to 100 times more potent than morphine! Very often, fentanyl patches are employed to treat patients in severe pain, and sometimes quite early in the process of pain management. This is dangerous, and I would not want any part of it as a patient. Among the more than 72,000 drug overdose deaths estimated in 2017, the sharpest increase occurred among deaths related to fentanyl and fentanyl analogs, with nearly 30,000 overdose deaths. In my professional opinion, fentanyl patches should generally be restricted to cases of cancer and palliative care.” —James Petros, MD, CEO/president of the Allied Pain & Spine Institute and clinical instructor at Stanford University. (Don’t miss these 24 secrets pain doctors won’t tell you.)

Aspirin and Advil
“I personally would never take any medication in the nonsteroidal anti-inflammatory drug (NSAID) family—particularly aspirin or Advil. I have suffered from irritable bowel syndrome in the past, and NSAIDs have been closely linked with the development of intestinal permeability (leaky gut). Being that I am also a relatively young male still looking to have more children in the future, I have extra reason to stay away from Advil, as it has been shown to decrease sperm count and testosterone levels at higher doses. This class of over-the-counter medication is extremely common globally, and it may be the right choice for many people; I just caution those with digestive or reproductive issues to stay away. My alternative is a daily high-dose fish oil. At doses of 2–3 grams a day, fish oil has strong anti-inflammatory properties and has the added benefits of reducing pain, improving your cholesterol numbers, and potentially lowering your risk of heart disease.” —Elroy Vojdani, MD, IFMCP, functional medicine practitioner
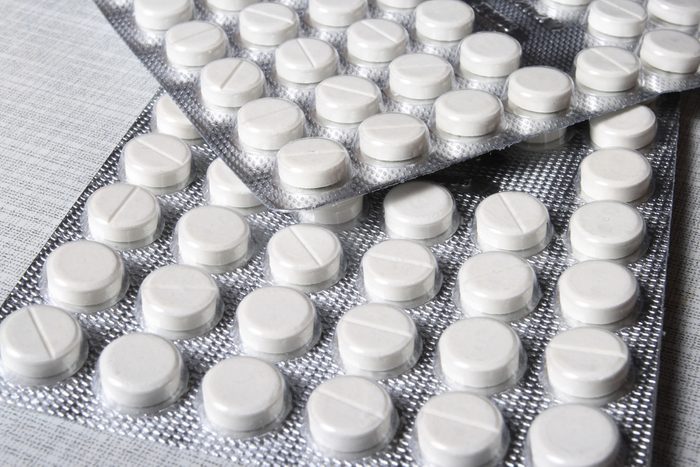
Oxycodone
“The pain med I would never take again is oxycodone. I took it once after a C-section—gave me nightmares. I rarely, if ever, prescribe oxycodone and not just because it gave me problems. I haven’t found that patients need it. Most patients, if they need something stronger for pain than over-the-counter meds, get prescription-strength naproxen. Rarely, [I’ll prescribe] hydrocodone. I mainly use hydrocodone and tramadol (another narcotic) in patients who have kidney problems and need something stronger than Tylenol. Now that lidocaine is available over the counter, I have been recommending it.” —Cynthia Jones-Nosacek, MD, a Milwaukee-based family physician who cares for chronic/acute-pain patients. (These are the 12 things your doctor might not tell you about pain meds.)
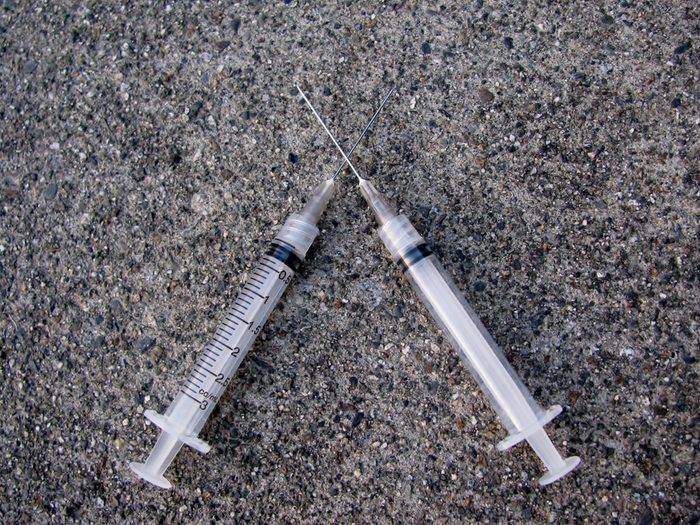
Opioids
“The misuse of opioids—codeine, oxycodone, fentanyl, hydromorphone, and morphine, to name a few—has resulted in the taking of approximately 115 American lives every day, quadrupling since 1999. Not only do opioid medications have addictive potential, but they also have significant side effects, such as drowsiness, depressed cognitive function, constipation, suppressed sexual drive, and suppression of one’s immune system. Although in some cases using opioid medications may be appropriate, I always emphasize the usage of the newer, safer non-medication treatments for pain. I have found PEMF (pulsed electromagnetic field) therapy to be extremely effective. It works at the cellular level to accelerate the body’s ability to repair injured cells. One device that possesses PEMF, which I recommend to patients, is called Oska Pulse. It’s a drug-free pain-relief device that reduces inflammation, increases circulation, improves mobility, and, ultimately, alleviates pain. [It] has no known side effects and can be used on-the-go as often as needed.” —Jonathan Kost, MD, medical director of the Hartford Hospital Pain Treatment Center and the Spine and Pain Institute at Midstate Medical Center, and a member of the Oska Wellness medical advisory board

Ambien and Lunesta
“Patients with chronic pain often experience significant difficulty falling or staying asleep. Some estimate this overlap to occur in 60 to 80 percent of pain patients. Therefore, sleep medication is commonly prescribed. But I would never take—and I never prescribe—prescription sleep medication like Ambien or Lunesta. These medications have been linked to a higher risk of Alzheimer’s disease. My alternative is using high-dose magnesium threonate, up to 1 gram, to help induce restful sleep before bed. This form of magnesium also has the added benefit of improving brain health and function in the long run and can even mildly boost mood. If my patients need some extra help with sleep, I will prescribe 200–400 mg of theanine, a calming amino acid that can help reduce anxiety and induce restful sleep when taken right before bedtime.” —Dr. Vojdani. Here are 20 things you do before bed that sabotage your sleep.

Steroids
“This is controversial and case dependent, and I, of course, commonly use steroids in my practice as a very strong anti-inflammatory. Steroids can be prescribed as an injection or pills, and can rapidly reduce inflammation and be very helpful with extreme inflammation, as in cases of pinched nerves and arthritis. However, this is a heavy-duty drug that should not be overused. Repeated usage of steroid injections can lead to a weakening of the tissue, and oral steroid usage has been associated with cases of reduced blood supply that can damage the bones…so I would try to avoid them, though I would consider a short-term dose if I had a severe problem. While there are some conditions that require long-term steroid usage—such as autoimmune disorders like lupus—patients should always inform their doctors if they have had steroid injections or treatments in the past to avoid multiple uses for minor sprains and strains.” —Miho J. Tanaka, MD, director of the Women’s Sports Medicine Program and associate professor, Department of Orthopaedic Surgery, at the Johns Hopkins Hospital
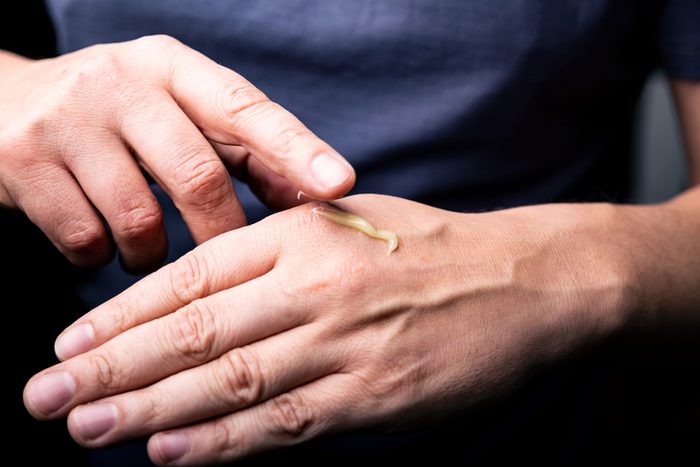
Topical anti-inflammatories
“I would not use topical anti-inflammatory ointments and creams for joint pain and arthritis. They are effective for some people and a good alternative for those who cannot ingest pills due to stomach ulcers, but I have seen a lot of patients with rashes and skin irritations. They are also not as effective [as other options]. Instead, try icing the area, wearing a brace, physical therapy, and acetaminophen (Tylenol).” —Janette Nesheiwat, MD, a New York City-based family and emergency doctor. (Learn more about 8 proven ways to manage chronic pain without medication.)

Ketamine
“There are no particular medications I would ‘never’ take. [But] there are a number of medications that I would be very reluctant to take except perhaps as a last resort in an awful situation. One of these drugs is ketamine (Ketalar), which is sometimes used in anesthesia as a dissociative anesthetic. Its effects can be much like that of the street drug PCP. In recent years, ketamine has been used by pain-management physicians to treat certain disorders that cause pain, such as complex regional pain syndrome. It depends what type of pain is being treated: Alternatives to pain medications may not even be medications at all. Most pain issues are treated with a multifaceted approach that can include physical therapy, acupuncture, cognitive behavioral therapy, diet, exercise and medically treating the underlying disorder causing the pain.” —Jeffrey B. Glaser, MD, interventional pain management physician

Marijuana
“I will not use marijuana for pain relief. Marijuana has been used for chronic pain, cancer pain, and neuropathic pain caused by nerve damage, but as more states are making medical and recreational use of marijuana legal, it’s also gaining popularity as a painkiller. There is some data to support its use in pain, but not much scientific literature is available. I will not use it because of its short-term and long-term effects, [including] impaired thinking and memory; more frequent chronic bronchitis episodes and worse respiratory symptoms; and an increase in the risk of developing schizophrenia, other psychoses, social anxiety disorders, and addiction. Addiction with marijuana is real, especially with heavy use. For moderate to severe pain not controlled by acetaminophen alone, the drug that I would prefer is Norco, which is a combo of hydrocodone and Tylenol. If used properly and according to guidelines, it is a very potent pain medication [that] acts on the central nervous system to relieve pain.” —Adil Akhtar, MD, associate professor, Department of Medical Oncology & Hematology, Oakland University’s William Beaumont School of Medicine, and director of Inpatient Clinical Operations at Karmanos-McLaren Oakland Cancer Center in Michigan

Aleve
“Whereas one dose of fentanyl in the wrong hands can lead to death, the other medication I lose sleep over may surprise you: Aleve. Nonsteroidal anti-inflammatory drugs (NSAIDs) provide substantial pain relief for many people. What most people don’t realize is the great risk when you take this medication long term. It is responsible for over 40,000 hospitalizations and more than 3,000 deaths per year as a result of gastrointestinal complications, including ulcers, hemorrhage, and perforation—which can lead to death. NSAIDs are still helpful, but I will often take a break from this class of medication and use acetaminophen for a period of time. Other medications such as Neurontin—which was originally used as an anti-seizure medication—work to dull hypersensitive nerves. There are also non-medication options to treat common musculoskeletal disorders, such as APOS therapy—it helps with chronic knee, hip, and lower back pain by adjusting gait biomechanics with special shoes. Another treatment for severe neuropathic pain from peripheral nerves is the Bioness StimRouter. Both of these treatments have been proven as safe and effective, and have reduced oral pain medication requirements.” —David A. Spinner, DO, RMSK, CIPS, FAAPMR, assistant professor at the Icahn School of Medicine and Director of Pain Management for the Department of Rehabilitation and Human Performance at Mount Sinai

Ultram
“I would not take Ultram, aka tramadol. It’s used to treat mild to moderate back pain, joint pain, sprains, post-op pain, muscle pain, etc. Many patients benefit from it, but I have also had many patients become dizzy, light-headed, and nauseated from it. Try acetaminophen or ibuprofen instead. I have also seen a lot of surgeons switch to gabapentin as an alternative for pain because it is less addictive.” —Dr. Nesheiwat. (Check out these treatments for lower-back pain that really work.)

Any over-the-counter pain meds used too frequently
“Combination analgesics, such as Excedrin Migraine and acetaminophen and NSAIDs (ibuprofen, naproxen, etc.) are some over-the-counter medications that can contribute to medication-overuse headaches if used too frequently. I tell my patients to limit the use of ‘as needed’ pain and headache medications to 10 days/month of use or less. I use naratriptan and simple analgesics such as ibuprofen for my migraines, 10 days/month of use or less.” —Kevin Weber, MD, neurologist at the Ohio State University Wexner Medical Center’s Neurological Institute

Nothing is off the table
“I actually do not believe there is any pain medication that I would never take, as all pain medications serve a useful purpose if prescribed appropriately. To me, it’s more important to ensure pain medication is used with an intended objective, appropriate time frame and vigilant consideration of side effects…[and] is prescribed with the purpose of targeting the underlying disease or illness causing the pain. For example, neuropathic pain medications such as gabapentin are excellent for burning/tingling pain related to nerves, as in sciatica. Muscle relaxers are excellent for stiffness and spasms. Certain medications, such as medical marijuana, have multiple mechanisms of action and can provide additional therapeutic benefits for easing pain.” —Tanuj Palvia, MD, spine and sports interventional pain specialist and anesthesiologist at Physio Logic. (Don’t miss these home back-pain remedies with science on their side.)