Birth defects affect 1 in 33 babies
Parents will commonly tell you that all that matters is that their baby is born healthy. Hearing that yours has a birth defect can rock your world. About three percent of all babies in the U.S. are born with a birth defect—that’s 1 in 33 babies, according to the Centers for Disease Control and Prevention (CDC). Many are not life-threatening, but some are devastating. Birth defects are responsible for 20 percent of infant deaths, per the CDC. Here are 7 ways to prevent birth defects before and during pregnancy.
More treatments are available
Despite the statistics, “there’s no question that we’re getting better at treating major birth defects,” says Michael Belfort, MD, PhD, obstetrician/gynecologist-in-chief and fetal surgeon at Texas Children’s Hospital in Houston, Texas. Major defects include brain or heart defects and spinal defects, such as spina bifida.
Folic acid isn’t only for neural tube defects
Before getting pregnant—and throughout pregnancy—the American College of Obstetricians and Gynecologists (ACOG) recommends taking a folic acid supplement to help prevent neural tube defects (birth defects of the brain and spine). Plus, experts have found that folic acid also helps prevent heart defects, too. A study in PLoS One in 2017 revealed that women who did not take a supplement and who got little folate in their diet (the nutrient is in foods like leafy greens, avocado, and legumes) had nearly twice the risk of their babies developing a heart defect than women who had an adequate intake. (This is the difference between folate and folic acid.) Note that many grain-based foods—think breakfast cereals and bread—are now fortified with folic acid to help prevent birth defects. Here are 7 foods high in folic acid and folate.

Treating mom’s health can help the baby
If you have diabetes, managing your blood sugar throughout pregnancy is important for a healthy mom—and baby. A recent study in the American Journal of Obstetrics and Gynecology concluded that having diabetes—type 1 or type 2—before pregnancy was associated with an increased risk for 46 out of 50 of the birth defects analyzed, including abnormal brain development, congenital limb defects, and heterotaxy (where internal organs develop in the wrong places). Working with your doctor to get blood sugar under control before conceiving improves the odds of having a healthy baby, the study says. (Check out these symptoms of type 2 diabetes).
Prenatal care in general is critical during pregnancy. With prenatal care, healthcare providers can check for gestational diabetes, a type of diabetes that occurs in 2-5% of pregnancies. Gestational diabetes typically develops in the middle or later in pregnancy and is not associated with birth defects in the same way as pre-pregnancy diabetes. However, it does require special treatment and can affect the baby’s and mother’s health in other ways.

Genetic help for family planning
Right now, doctors can do genetic testing during pregnancy to determine if the mother or father is a carrier for certain diseases, like cystic fibrosis. These conditions aren’t considered birth defects, but these types of tests may be used in the future to look for risks of birth defects. “We know that people who have a family history of congenital heart defects are more likely to have children with these defects,” says Dr. Belfort. In fact, one study in the Journal of the American College of Cardiology found that among couples with a strong family history, a gene panel could identify the cause of congenital heart disease in nearly one-third of families. In the future, this technology could help improve family planning efforts.
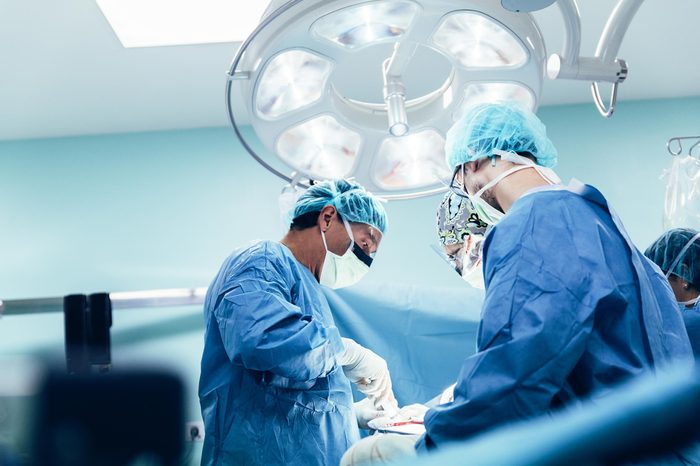
In-utero open fetal surgery is an option
Spina bifida is a birth defect that may not always be life-threatening—but it’s potentially devastating, and can lead to paralysis and a condition called hydrocephalus (accumulation of fluid in the brain), among other problems. For some moms and their fetuses, in-utero surgery can repair spinal cord defects to prevent and reverse some nerve damage, says N. Scott Adzick, MD, the surgeon-in-chief of Children’s Hospital of Philadelphia (CHOP) and founder and director of the Center for Fetal Diagnosis and Treatment. At CHOP, surgeons can perform this surgery for the most severe form of spina bifida, myelomeningocele, by opening the uterus and operating on the baby’s back. (The uterus is then closed and the fetus remains in the womb until delivery.)
“The techniques for fetal surgery for spina bifida are getting better, and there are fewer complications,” he says. While not a cure, children can grow up to have “much better motor function of the legs and arms with less hydrocephalus. These kids who would have otherwise died or become severely disabled are now running around and living normal or near-normal lives. We are saving many lifetimes with this surgery,” he says.
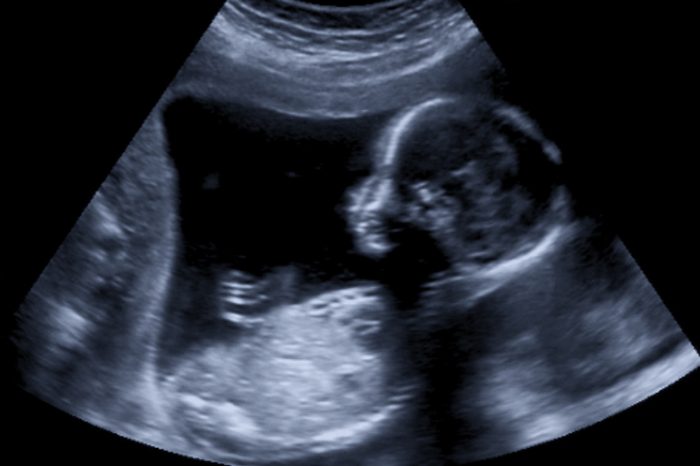
Minimally invasive treatments can be done in-utero, too
In some instances of myelomeningocele, doctors can perform minimally invasive surgery for the repair. This is called a fetoscopic procedure, where small instruments go through the wall of the uterus, fill the uterus with carbon dioxide gas to create room for an operation using minimally invasive techniques such as laparoscopic surgery, explains Dr. Belfort (he developed the technique). “This is safer for the mother, and she can have a vaginal delivery if she wants, as there is low or no risk of rupturing the uterus [during delivery],” he says.

Modified c-sections save lives
There are cases where a baby may be born unable to breathe. Dr. Belfort gives the example of a neck mass that obstructs the baby’s windpipe. “We can perform an exit procedure, which is basically a modified C-section,” he says. The baby’s head is delivered and put on life support while the medical team works to get an airway, either by intubating through the mouth or performing a tracheostomy, before disconnecting the baby from the mother’s placenta. “Once baby can breathe, the cord is cut and the baby is handed off,” says Dr. Belfort. These are the c-section myths pregnant women should know.

Babies are now being born after in-utero stem cell transplants
Stem cell transplants from the mother to the fetus offer the hope of treating inherited blood conditions that can be difficult to deadly for the baby. Sickle cell disease—a group of blood disorders—causes extreme fatigue, anemia, and swollen hands and feet; sickle cell can also delay growth and damage organs. Alan Flake, MD, a fetal surgeon at CHOP has designed an in-utero stem cell transplant, which involves injecting the mother’s stem cells into the bloodstream of the fetus. He’s tested it in animals with the aim of preventing babies from developing blood cell disorders in the first place.
A trial in babies is underway in the Bay Area: In 2018, UC San Francisco announced that an infant with the blood disorder alpha thalassemia was born after receiving blood transfusions and a stem cell transplant in utero. The condition—a defect in red blood cells that leads to severe and sometimes deadly anemia—requires a lifetime of monitoring and difficult treatment; because a baby in utero has an underdeveloped immune system and a greater tolerance for a mother’s cells, the transplantation has a greater chance of success, note the doctors involved with the trial.
Artificial wombs for premature babies
There may be hope for babies born extremely early. “One of the most exciting things on the horizon is the full support of a very preterm baby in a new type of incubator,” says Dr. Belfort. An artificial womb could allow a fetus to be delivered and survive by connecting the cord to a type of heart and lung machine, says Dr. Belfort. “This is a lung machine that uses the baby’s own heart to pump blood. That blood goes to a device that acts like a placenta to some extent. It can keep a baby alive until it can support its life,” he says. The wombs have already been tested on fetal lambs.

And the future is one with fewer birth defects
Whether an artificial womb is five or 10 years away, experts aren’t sure, but it’s a promising and exciting new technology. “A lot of birth defects could be corrected early with that system, and the baby could grow as a fetus as opposed to delivering early and then get surgery to save its life,” says Dr. Belfort. If you’re pregnant, don’t fall for these 9 pregnancy myths—and 3 that are actually true.
