How to Use a Nebulizer Correctly—and Safely
Updated: Jun. 22, 2021
A nebulizer can be a better alternative to an inhaler for people with asthma and other respiratory conditions. Learn how to use one, plus how to care for the machine.
What does a nebulizer do?
A nebulizer is one of several ways to get respiratory medication into your airways. The machine works by vaporizing liquid medication into a steady stream of mist, which you then breathe into your lungs.
Nebulizers aren’t as convenient as inhalers (which you can tuck in your pocket), but they tend to be easier to use. While medication delivered by inhalers sometimes miss their mark, nebulizers are more reliable.
“It’s almost a guaranteed delivery,” says Len Horovitz, MD, a pulmonary specialist with Lenox Hill Hospital in New York City.

What is a nebulizer used for?
Anyone with a chronic or acute respiratory condition can benefit from a nebulizer, says Dr. Horovitz.
Asthma and chronic obstructive pulmonary disease (COPD) are common conditions that require nebulizers. Others are chronic bronchitis, emphysema, the flu, and other viruses, even Covid-19—any illnesses that impact the lungs.
“It’s often used with albuterol or an inhaled corticosteroid to open up the lungs when people are having shortness of breath or wheezing,” says Juanita Mora, MD, national volunteer medical spokesperson for the American Lung Association.
You can use it to deliver drugs that are given regularly or even to prevent symptoms for folks who have trouble using an inhaler.
“It’s really nice. All the patient has to do is breathe it in,” she adds.
Who are nebulizers for?
Theoretically, nebulizers are interchangeable with inhalers, meaning they deliver the same medication to the same place in people with respiratory conditions, says Dr. Horovitz.
In reality, nebulizers may be best suited for people who have trouble using an inhaler.
“A study came out that said an inhaler works as well as a nebulizer, but sometimes when people are tired of coughing or don’t have a good inspiratory capacity, a nebulizer is a better choice,” says Dr. Mora.
People with muscular issues or other physical limitations may not be able to depress the inhaler enough to actually release medication. Coordination also plays a role, says Gary Stadtmauer, MD, an allergy and asthma specialist in New York City who is also affiliated with Mount Sinai Medical Center.
In both of those cases, a nebulizer is a more effective solution.
“Everyone breathes,” he explains. “A parent could hold a nebulizer to a child’s face. The same thing goes for someone who’s elderly.”
(If you need a nebulizer for a kid, these come recommended by experts.)
Types of nebulizers
All nebulizers work the same basic way—by turning liquid medication into a mist that you can inhale.
Some machines use air compressors, which use airflow to convert the liquid medication into mist, while ultrasonic nebulizers use sound waves to create that transformation.
Nebulizers also come in portable and larger, less-portable models.
“The portable ones are nice because you can travel with them,” says Dr. Mora. “The bigger ones are a bit more high grade and are usually used at home. They’re more stationary but more potent.”
There are even small nebulizers that can be powered by the cigarette lighter in your car, says Dr. Horovitz.
The equipment
Most nebulizers have the same basic components. The nebulizer is a small bowl that holds the medicine. There’s also a compressor that breaks up the liquid into an aerosol, tubing, and a mouthpiece (or mask).
“They all work to provide the same sort of action,” says Dr. Horovitz.
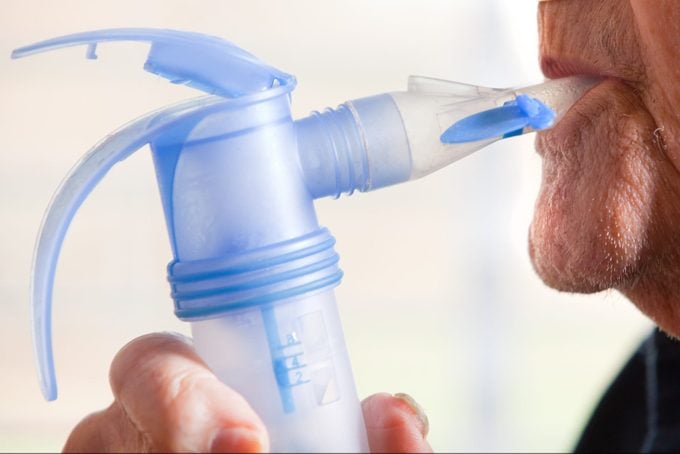
How to use a nebulizer
Before turning on the machine, wash your hands to avoid getting any nasty elements into your lungs. You just want to inhale the medication and nothing else. And start with a clean nebulizer (more on this below).
Place the right amount of medication into the nebulizer (we’ll get to that soon) and make sure the lid is secure.
Connect the tube from the compressor to the nebulizer section, then attach the mouthpiece. Some folks, including children under the age of 6 will need to use a clear mask.
Close your lips around the mouthpiece and breathe normally until the medication is gone, about 10 to 15 minutes.
The nebulizer takes less effort than an inhaler. “There’s no coordination needed to press and inhale like an inhaler,” notes Dr. Horovitz. “Just sit with it in your mouth closed, and the medication will be delivered to you.”
If you cough, stop the machine until your breathing stabilizes, then start again. You should also stop if the medication starts foaming or bubbling.
(Add these healthy lung foods to your diet to breathe better.)
The medications
The most common medications used in a nebulizer are albuterol and an inhaled corticosteroid like budesonide.
To be used in a nebulizer, medications must come in liquid form. Not all do.
“Anything that can’t be aerosolized, we can’t use,” says Dr. Mora. “There are a lot of drugs that can’t be aerosolized.”
Typically, the medications are premixed, so it’s simple to add them to the nebulizer, but medications aren’t combined for a nebulizer.
Caring for your nebulizer
Dr. Mora recommends rinsing out the tube from the compressor to the nebulizer after each use.
If you’re using the machine for an infection like Covid-19 or the flu, “you want to make sure to completely change the tubing and masks,” she says. Even better, don’t reuse it.
If you’re using the nebulizer daily for asthma exacerbations, COPD, or emphysema, rinse it with water after using it. Air dry it then store it where it won’t collect dust.
Insurance matters
For the most part, nebulizers and the medications that go in them are covered by insurance, says Dr. Mora. That’s as long as you have a prescription, not just for the medication but also for the machine, she says.
While you can buy the nebulizer machines over the counter at pharmacies or online, the medication is always prescription only.
Next, try these exercises to build stronger lungs.














