Myth: You either have a mild or severe food allergy
The truth: There are no mild or severe allergies, only mild or severe reactions. “Reactions are somewhat unpredictable,” explains Joshua Dorn, MD, allergy/immunology fellow at the Mayo Clinic in Rochester, MN. That means you can eat a food a few times and have nothing more than a couple of hives, then boom, you might have anaphylaxis—a severe systemic reaction that requires immediate medical treatment. “There have been many reports of people having severe reactions after mild ones,” Dr. Dorn confirms. And anaphylaxis is on the rise: Visits to the ER for a severe allergic reaction shot up a staggering 124 percent from 2005 to 2014, according to a 2017 study published in the Journal of Allergy and Clinical Immunology: In Practice.
Reactions are tricky to predict because other variables can be in play. Are you sick? Were you exercising? Overheated? Drinking alcohol? Do you have active asthma? Other allergies? They’re all considered “co-factors” that can contribute to a more extreme immune response.
The bottom line: “Any reaction can range from mild to severe so it’s best to be prepared for a severe one,” says Dr. Dorn. And when allergists say “be prepared,” they mean carry two EpiPens or other epinephrine auto-injectors.

Myth: You don’t need epinephrine if you’re not going to be eating
This is one of the most common mistakes allergists see. You think, “My child is just going to lacrosse practice. She won’t be eating—no need to bother with the EpiPen.”
You’re taking a serious risk, warns Dr. Dorn. What happens if your child’s coach hands out surprise snacks on the sidelines? Research shows that about half of fatal food allergy reactions happen away from home. Perhaps the bigger worry, though, is that reactions sometimes strike an hour or more after eating. If you don’t have epinephrine on hand, it could set in motion a terrible turn of events. “Most severe reactions happen when people don’t have their EpiPen with them,” notes Dr. Dorn. Deaths from food allergy often involve delayed epinephrine or not getting it at all, according to a 2017 review of research. “If you always carry it, it becomes a habit,” he says. This is some of the worst advice allergy doctors have heard.

Myth: Adults can’t develop new food allergies
While kids are more prone to food allergies, you can absolutely develop them at any age. One surprising study presented at the American Academy of Allergy, Asthma and Immunology Conference in 2017 found that 45 percent of adults with food allergy got them after age 18.
The most common adult food allergy, according to this research, is shellfish allergy: 3.6 percent of adults have one, which is up 44 percent from 2014. Next up: tree nut allergies. If you’re seeing hives or noticing other allergic symptoms after eating, be sure to see an allergist, who can test you and prescribe an EpiPen. Then bring it everywhere. (Here are the other most common food allergies to be aware of.)
Does your mouth feel itchy when you bite into an apple or other fruit or veggie? You may have a common condition called oral allergy syndrome—OAS. Related to pollen allergy, OAS is an immune response to certain fruits or vegetables, but it almost never leads to anaphylaxis, explains Dr. Dorn. “About 90 percent of the time, symptoms are just in the mouth.” The other good news about OAS: People can generally tolerate the food cooked (which means apple pie is back on the menu.). Find out more about OAS.

Myth: Nobody outgrows nut allergies
OK, there is a kernel of truth here: A child is less likely to outgrow a peanut or tree nut allergy than an allergy to, say, milk or eggs. But they definitely can shed nut allergies. Experts believe that roughly one in five kids will lose their peanut allergies, Dr. Dorn reports, and about the same amount or slightly less will one day be able to safely enjoy tree nuts.
Most allergists test patients yearly and, if there is evidence that the food allergy is waning, they may propose you try a food challenge. Conducted in the allergist’s office or at a hospital, a food challenge means you’ll keep eating the problem food in increasing amounts while a medical team monitors you. If you pass, you can safely reintroduce the food at home—after a 24-hour waiting period to make sure there’s no delayed reaction.

Myth: Blood tests reveal how bad your reactions will be
About that bloodwork at the allergist’s office: The IgE test shows the levels of immunoglobulin E antibodies circulating in your blood in response to an allergen. Keep in mind that it’s a probability test, Dr. Dorn stresses. “People think higher results mean severe, lower mean less severe,” he says. “All it does is provide one piece of information to help decide whether or not someone is allergic to food.” A person with an 80 result to cashews, say, is more prone to be allergic to them than someone with a 5, but it doesn’t necessarily mean that they’ll have more severe reactions.
These tests are often used in tandem with skin prick tests: An allergist uses a needle with a diluted allergen to prick your skin and see if you develop a wheal (a hive).
Since both blood and skin prick tests can have false positives, the new thinking on testing is that allergist should only use them to confirm suspected allergies, not to search for possible sensitivities. Don’t miss these weird things you can be allergic to.

Myth: Feeling tired or weird after eating means you’re allergic
Nope, and here’s why: A food allergy is a reproducible immune response to proteins in food. Food allergy symptoms may include some or all of the following: hives, a rash, itching or swelling of the mouth, vomiting, diarrhea, stomach cramps, breathing difficulty, or low blood pressure. “When it comes to non-specific symptoms like fatigue or symptoms that occur daily, food allergy is unlikely,” Dr. Dorn says.
That’s not to say your symptoms aren’t real. If you suspect your diet is making you feel blah, bloated, or otherwise off, keep a food diary and check in with your doc. Developing headaches after eating foods like red wine, aged cheese, and deli meats can signal you’re susceptible to migraines. If you have the autoimmune disorder celiac disease, simply eating gluten (a protein found in wheat, barley, and rye) triggers the body to attack the lining of the small intestines. Many people have an intolerance to gluten, lactose, or other foods. So if food is making you feel bad, Dr. Dorn says it’s normal to ask yourself, “What am I eating and can I change it to feel better?”

Myth: Kids who are allergic to peanuts just need to start eating them
Not on your—or their—life. Feeding an allergic child a peanut could be deadly. Why do some people believe this myth? In 2015 the LEAP study grabbed headlines with its findings that peanut exposure decreased rates of peanut allergy by more than 70 percent. However, some people mixed up the takeaway of the study. “LEAP is about prevention, not treatment,” Dr. Dorn says. “Kids who are allergic to peanuts should never be fed a peanut at home.”
The real message of the LEAP findings is that we’ve been introducing foods like peanuts to babies all wrong. “What the study showed is that consuming peanuts earlier seems to prevent the development of a peanut allergy in those at high risk of a peanut allergy—which the guidelines define as having an egg allergy or moderate to severe eczema.” Infants who are in that high-risk group should be tested by an allergist to make sure they’re not already allergic, and if they aren’t, then introduced them to peanuts at four to six months.

Myth: But doctors are giving peanuts to kids with allergies
Actually, they’re not, but it is easy to confuse LEAP with something called “peanut oral immunotherapy.” Oral immunotherapy research tests whether allergists can treat food allergies by exposing kids to incredibly tiny amounts of the allergen—peanut proteins. The researchers gradually increase exposure over a period of years until they reach a maintenance dose. The goal is to see if it’s possible to retrain the immune system so it won’t react to peanuts as a dangerous substance and trigger a severe reaction. “The peanut trials are farther along than tree nut, eggs, and milk, and have had some success,” says Dr. Dorn.
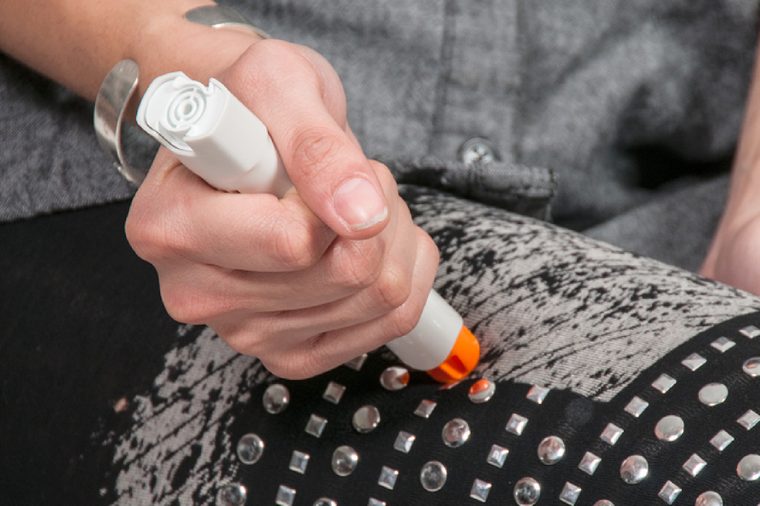
Myth: Epinephrine is a dangerous drug, try an antihistamine first
This can have devastating consequences. “Epinephrine is the only treatment for anaphylaxis and it works better when it’s given earlier in a reaction,” Dr. Dorn says. Plus: “It’s very safe.”
How do you know when to use it? That’s a great question to talk through with an allergy doctor, who will take your past reactions and test results into account. The standard advice is to use the EpiPen or Auvi-Q if two of your body systems—skin, gastrointestinal, respiratory, cardiovascular—are reacting. One example could be that you break out in hives and then vomit. But some allergists will recommend using it as soon as you have any symptoms at all, or even as soon as you know you’ve been exposed.
Every year, the news reports tragic stories about people who waited too long to use their epinephrine. Remember: You’re safer using an EpiPen when you didn’t need it, as opposed to waiting too long.

Myth: Airborne reactions are a huge problem
Growing up allergic to tree nuts and peanuts, Dr. Dorn felt anxiety about having a bad reaction because someone was eating nuts near him. He now knows better: “You’re very unlikely to have anaphylaxis from casual contact or inhalation,” he says. Since peanut protein isn’t airborne, a child sitting across the room from a friend who is eating peanut butter should be fine (as long as the pal washes their hands with soap and water after). But if you are sitting right next to a guy shucking peanuts, you could have a mild reaction such as “hayfever type symptoms like itchy eyes and a stuffy nose,” Dr. Dorn says.

Myth: An allergy always happens within minutes of eating something
It may—or it may not. So just because a food doesn’t give you immediate hives doesn’t mean you’re in the clear. The typical window is minutes to two hours—and symptoms can progress fast. (The timeframe is longer—six to eight hours—with alpha-gal allergy, a sensitivity to meat that is spread by the Lone Star Tick.)
You should also watch out for a bi-phasic reaction, a second wave of anaphylaxis after the initial round seems to clear up. This dangerous recurrence can come hours or days later. It’s more likely to happen to children, people who needed more than one dose of epinephrine, and folks who didn’t get epinephrine promptly. These reactions are prone to getting life-and-death serious, fast, so if you notice a flare after you’re home from the ER, use another EpiPen and call 911. Here are some signs your child may be developing a food sensitivity.

Myth: Companies have to list every single ingredient in foods
You would think so, but no. In fact, the only rule that food manufacturers have to follow—as a result of the Food Allergen and Consumer Protection Law, passed in 2004—is listing on the label if a food contains any of the top eight allergens: peanuts, tree nuts, soy, milk, eggs, shellfish, fish, and wheat. They have to use plain English and tell the consumer exactly which type of tree nut, shellfish, or fish is present (meaning a label would state “shrimp” rather than using a generic term like “shellfish”).
These foods are responsible for 90 percent of food allergies, according to the FDA, but plenty of people are allergic to other foods. And if you are and want to make sure your food is safe? You’re on your own, as crazy as that seems. Your allergen might be listed, or it might not. Terms like “spices” and “natural flavorings” are particularly vexing to people trying to manage food allergies. What do they even mean? Your only recourse is to call each company and try to get that essential information from them.

Myth: Food companies must reveal if their products are made on the same lines as top allergens
You’ve probably seen warning words on labels: “made in a factory with…, may contain…., made on shared equipment with… If you believe this means manufacturers will always warn you about the potential for cross-contamination, you’re mistaken. This precautionary labeling is completely voluntary, which means it’s completely unreliable.
Dr. Dorn’s advice: You can always contact the manufacturer to see if they will share specifics about their manufacturing process, but it’s safest to avoid foods marked as “may contain” or “made in a factory with” your allergen. Next, find out about these medical conditions that could be mistaken for allergies.

