What Causes Hives? Everything You Need to Know About Urticaria
Updated: Mar. 07, 2022
Hives, or urticaria, are a common allergic reaction. Here are pictures of hives, what triggers them, and how to treat them.
On This Page
What are hives?
Nearly everyone experiences a skin rash at some point in life. It could have bumps, be itchy or painful, and pop up anywhere on your body. Hives, or urticaria, however, are not the same thing as an everyday rash.
Hives are a relatively common allergic reaction that affects approximately one out five people at some point in their lives, according to the American Academy of Dermatology Association (AAD). These welts often come and go, and they can also be chronic.
“Hives are raised red or pink areas on the skin that last less than 24 hours,” says Jeffrey Cohen, MD, a Yale Medicine dermatologist and assistant professor at Yale School of Medicine.
If you have darker skin, the area may be raised but not necessarily red or pink, it could be the same color as surrounding skin.
Urticaria is extremely itchy and bothersome, according to Dr. Cohen. Sometimes they appear as a reaction to something, but in some cases, they form for no apparent reason.
What causes hives?
Hives happen because your body recognizes something—a food or medication, for instance—as foreign and reacts by fending off the foreign invader.
This allergic reaction is your immune system’s way of protecting your body by recognizing danger, Dr. Cohen states. But in some cases, reactions occur when there is no danger.
“Sometimes, the immune system responds to something as though it is dangerous even when it is not dangerous, such as a food or medication,” he says. “This response is an allergic reaction, and hives are one type of allergic reaction.”
And before you start to worry about coming into contact with another person while you (or they) have hives, rest assured urticaria isn’t contagious. It’s a reaction, or symptom. It doesn’t spread from person-to-person contact.
That said, it is possible to catch or spread some conditions that may cause hives. (More on those below.)
Pictures of hives
Pretty much anyone can get urticaria.
“They can occur in children or adults,” Dr. Cohen says. “There is no gender difference in children, but in adults, they are more common in women.”
There have also been a few medical conditions, such as hypothyroidism, that are associated with hives.
Here are what hives look like:
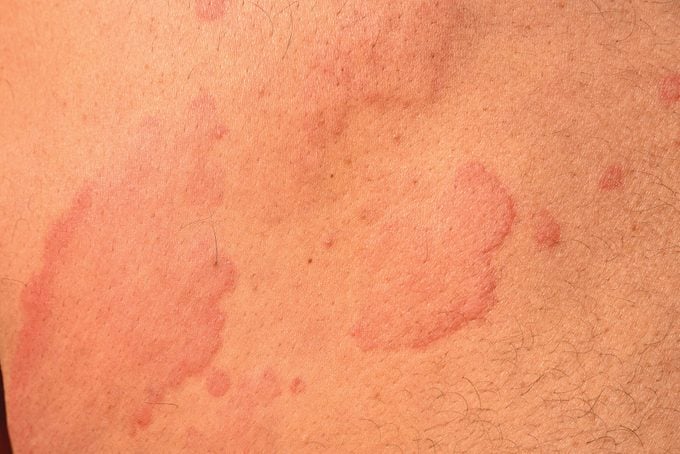
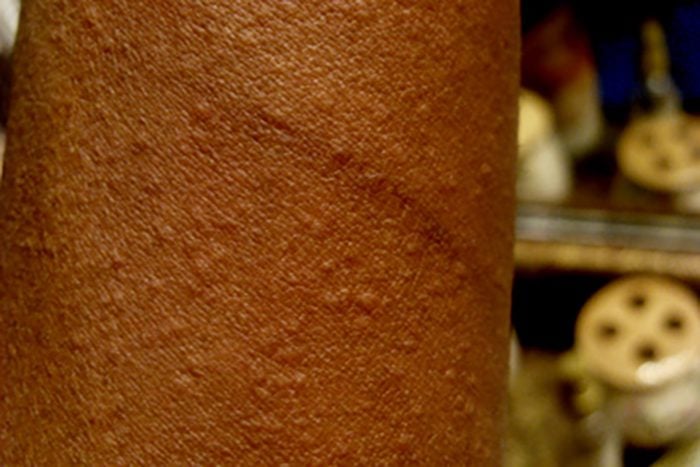
What triggers hives?
There’s no single cause of hives, and often what triggers your reaction will depend on the allergies you have. Sometimes there’s no identifiable reason for a breakout.
“There are lots of triggers for hives, but foods and medications are two of the most common,” Dr. Cohen says.
Food
What you eat might stir up an allergic reaction that results in hives, Dr. Cohen explains. Citrus fruits are a common trigger, as are milk, eggs, peanuts, tree nuts, and shellfish, according to the AAD.
Medications
Dr. Cohen explains that certain medications can be behind a breakout. For example, some antibiotics (especially penicillin and sulfa drugs), aspirin, and ibuprofen are known to induce hives, per the American College of Allergy, Asthma, and Immunology (ACAAI).
Infections and illnesses
The AAD says some illnesses, such as lupus and thyroid disease, can provoke hives. So can colds, bacterial infections, and viruses. So while hives aren’t contagious, some infections that may cause hives are contagious.
Other triggers
Other common triggers include:
- Insect bites and stings, known as papular urticaria
- Pet dander
- Pollen allergies
- Touching something to which you are allergic (like latex)
- Allergy shots
- Sun exposure
- Change in temperature, known as cold urtucaria
- Exercise
- Stress
- Contact with chemicals
- Scratching or pressure to the skin, known as dermatographic urticaria, or skin writing
Symptoms of hives
Hives can appear as slightly raised pink or red swellings or welts on lighter skin, and on darker skin the raised area may be the same color as surrounding skin. The raised areas can be extremely small or very large and may also connect together to form larger welts.
And, of course, hives are extremely itchy, says Dr. Cohen.
Hives may change shape and can appear suddenly then disappear quickly (within a day), only to reappear elsewhere on the body.
Another sign of hives: blanching. Press the hive and it’ll turn paler in the center.
While most cases of urticaria are not serious, some people might experience angioedema, a type of swelling of tissue deep under the skin. This may be associated with hives, but it can also be mistaken for hives.
If you notice angioedema symptoms—like swelling of your eyelids or mouth, hands, feet, or throat—seek emergency care. It can be a sign of a more dangerous allergic reaction known as anaphylaxis.
If you have hives along with wheezing, shortness of breath, difficulty swallowing, or fever, you should seek immediate medical attention as this is a medical emergency. Go to your nearest emergency center or call 911.
How long do hives last?
Signs of hives might subside within 24 hours, but the swollen bumps may pop up somewhere else on the body.
Generally, urticaria is broken up into two categories, the short-lived acute hives and long-term chronic hives.
- Acute hives: Hives that lasts less than six weeks. It may last just a few minutes.
- Chronic hives: Hives that last more than six weeks.
How are hives diagnosed?
If you have hives, the itching alone may get you into the doctor’s office, pronto.
Sometimes the cause is easy to catch—you’re allergic to shellfish, and you accidentally ate shrimp. Other times, you’ll need to answer some questions from your doctor to determine what triggered the outbreak.
A physician will look at the hives and ask about your health history, says Dr. Cohen.
The trigger for chronic hives can be particularly tough to uncover, according to the ACAAI, so your doctor may conduct additional tests. For instance, you may get allergy tests, blood work, or urine tests to get to the bottom of what caused your reaction.
You may need to keep a food diary to see if there’s a link between what you eat and your hives.
(Here’s what you need to know about at-home allergy tests.)
Treatments for hives
Hives often go away on their own, but there are also treatments to speed up the process.
“The most common treatments for hives are medications called antihistamines, the same medications people take for seasonal allergies,” says Dr. Cohen.
Antihistamines work by blocking histamine, a chemical in the body that produces an allergic reaction. As a result, they can reduce itching. There are many available over the counter (think Benadryl and Claritin), and your doctor will suggest the best for your condition.
Be aware that certain antihistamines can cause sleepiness, so if you’re taking the med during the day, be sure to get a nondrowsy version.
This treatment method is effective most of the time, but for some people who develop hives regularly for no reason, it may not work.
“For some of these people, antihistamines do not control the problem, and other medications such as pills or injections may be needed,” he says.
Prescription pills may include corticosteroids like prednisone, but this is a short-term treatment. Allergy shots (like omalizumab) may also be an option if you have chronic hives.
The antibiotic dapsone can also relieve redness and swelling. And if your reaction includes severe or life-threatening swelling in your tongue or lips, or if you have trouble breathing, your doctor may give you epinephrine (EpiPen).
If you know the trigger of your hives, one treatment is a no-brainer: “avoiding the trigger if it is known,” Dr. Cohen says.
(Here are the best natural home remedies for rashes.)
How to prevent hives
Preventing hives requires some thought and precautions.
If you’re aware of an allergy that causes hives, avoiding what you’re allergic to is an obvious fix. If environmental triggers (a change in body temp, for instance) lead to hives, try to minimize those as much as possible.
Since bacterial infections and other illnesses may trigger hives, maintaining your health, in general, is a good recipe for avoiding hives, too.
And when in doubt, call your doctor to determine the trigger and find treatment.
Next, learn about dermatographic urticaria, a condition known as skin writing.





















