7 Eczema Types: What to Know About the Symptoms, Causes, and Treatments
Updated: Mar. 08, 2022
If you have itchy skin, redness, and a rash, you may have eczema. Here's what to know about the seven eczema types, and how to treat them.
On This Page
What are the 7 different eczema types?
If you start to experience itchy skin, redness, and a rash-like appearance, you may have eczema, an umbrella term for a group of skin conditions. These hallmark symptoms are common in all seven eczema types: atopic dermatitis, contact dermatitis, dyshidrotic eczema, nummular eczema, neurodermatitis, seborrheic dermatitis, and stasis dermatitis.
So, how can you tell one type of eczema from the other? Here’s what you need to know about their symptoms, causes, and treatment options.
Atopic dermatitis
Atopic dermatitis is the most common type of eczema. It’s a chronic skin condition that causes mild to severe itching, burning, and irritation. It often runs in families and is frequently linked to asthma and hay fever.
According to a 2016 study led by the Allergy and Asthma Foundation of America and the National Eczema Association, atopic dermatitis occurs in 7.3 percent of adults in the U.S. For about 40 percent of the people who have it, atopic dermatitis is more than just occasional itchy skin; their symptoms range from moderate to severe.
“Atopic dermatitis can be very difficult for patients and their family members to live with because it is chronic and requires routine regular maintenance measures, some of which can be time-consuming for patients and the family members helping with their treatment,” says Richard Browning, MD, a dermatologist at UCHealth Dermatology Clinic, Cherry Creek in Colorado.
Symptoms
Itching is the main symptom of atopic dermatitis. You can get rashes anywhere on your body, but many people develop rashes inside their elbows or behind their knees. Babies tend to get rashes on their scalp and cheeks.
It’s important not to scratch your skin, especially if you have small bumps, because they can leak fluid. Scratching your skin may also lead to an infection.

Treatment
“Mild cases may be managed with frequent thick moisturizing and use of topical medications, while more severe cases can require the same in addition to phototherapy or systemic medications,” says Dr. Browning. “Corticosteroids are the mainstay of topical treatments for acute cases. Calcineurin inhibitors, such as pimecrolimus and tacrolimus, can offer a non-steroid option for longer-term management of troublesome areas.” These inhibitors work to suppress the immune system to ease skin inflammation.
Home remedies
A thick, greasy moisturizer, such as Vaseline, is an inexpensive, safe, and effective way to help keep skin moist, but it should be applied multiple times a day to improve the skin barrier Dr. Browning says. The skin barrier consists of the outermost layers of skin cells that protect it from the environment.
A dermatologist may recommend wet wraps and diluted bleach baths. Make wet wraps by dampening a cloth or gauze in warm water and wrapping the affected area. Then wrap a dry later of cloth over the wet layer and wear loose clothing over the wraps. In severe cases of atopic eczema, wet wraps can be done two to three times a day and sometimes left on overnight.
Bleach baths might sound scary and counterintuitive to keep skin moist, but bleach can actually reduce inflammation and fight off harmful bacteria.
“The concentration when mixed appropriately in the bathtub (1/2 to 1 cup of bleach for the entire filled bathtub) is similar to that of chlorinated pool water,” Dr. Browning says. “It is safe for the skin but a high enough concentration to help reduce the amount of Staphylococcus aureus bacteria on the skin, which can often cause flares of eczema and infections of open areas.”
Be sure to consult with your dermatologist before doing wet wraps or bleach baths at home.
What to watch for
When atopic dermatitis gets out of control, serious complications can occur. You may get bacterial or viral skin infections that can spread over large parts of the body. When atopic dermatitis isn’t well controlled, it can lead to nighttime scratching, poor sleep, learning difficulties, and behavior problems. Severe cases can even lead to growth problems over time.
“It is incredibly important to seek care from a dermatologist who can help establish best practices to keep it as well controlled as possible,” says Dr. Browning.
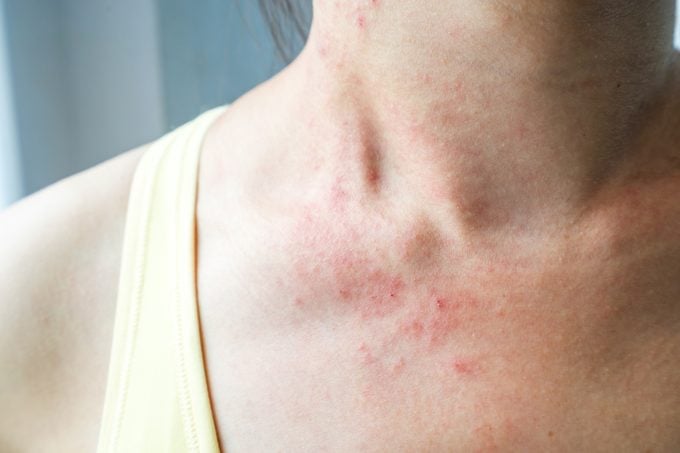
Contact dermatitis
Contact dermatitis isn’t a chronic condition like atopic dermatitis. It happens as a result of skin making contact with a substance that causes a reaction. There are two types of contact dermatitis: irritant and allergic.
Irritant contact dermatitis is far more common, Dr. Browning says, with four out of five cases treated for irritant exposure. Common irritants are solvents, detergents, make-up, nickel-containing items such as jewelry, scissors, and zippers.
Allergic contact dermatitis is a delayed reaction that appears as a rash after you are exposed to something that triggers an allergy.
Symptoms
Exposure to certain irritants might first cause pain and then later trigger itchy, red, dry, or scaly skin. Allergic reactions are a different beast.
According to the American Academy of Dermatology, more than 3,600 substances can cause an allergic reaction. If you’ve ever had poison ivy or experienced a rash after wearing jewelry made of nickel, you probably had allergic contact dermatitis.
Surprisingly, the substance may be something you touched without problems in the past but now causes an allergic reaction. Most often, the immune response from allergic dermatitis typically shows up a day or two or even weeks after exposure with an itchy, inflamed rash, that might burn or sting and ooze.
Treatment
It’s best to avoid exposure to irritants or allergens. Treatment involves anti-inflammatory medications to soothe and relieve itching and inflamed skin. If an allergen is suspected as the cause of contact dermatitis, a dermatologist can perform patch testing to determine the culprit Dr. Browning says.
Allergic contact dermatitis can be pretty miserable, too, affecting large body surfaces with itching and burning.
“Serious complications include full body rash, called erythroderma (when more than 90 percent of the skin is inflamed), which could require hospitalization,” says Dr. Browning. “It is very frustrating for patients who are trying to determine and avoid suspected allergens because some causative allergens are found in a large number of routine body products including shampoos, conditioners, soaps, etc.,” adds Dr. Browning.
In severe cases of irritant and allergic contact dermatitis, systemic medications may be needed.
Home remedies
As with all types of eczema, moisturizing, and gentle skin care is critical.
With the pandemic still looming, you may have noticed your hands are in rougher shape than usual. The hands are commonly affected in irritant hand dermatitis, and frequent handwashing or hand sanitizers strips the moisture barrier from our skin. “I recommend an application of a barrier moisturizer after every use of hand sanitizer or handwashing,” adds Dr. Browning.
Nummular eczema
As with other eczema types, nummular eczema is a persistent skin condition that appears as an itchy and inflamed rash.
Symptoms
It can be mistaken for psoriasis, ringworm, or a fungal infection, but nummular eczema does have a distinguishing feature: patches of multiple coin-shaped lesions. The lesions sting or burn, ooze liquid, and become crusty and then scaly.
About one in 500 people will be affected by nummular eczema during their lifetime Dr. Browning says, but males are more prone to developing it. Researchers aren’t sure what causes nummular eczema, but it tends to be triggered by extremely dry or sensitive skin, or when the skin is injured, such as a scrape, chemical burn, or insect bite.
Everyday things that irritate nummular eczema include soaps, wool, detergents, and fabric softeners (liquid and sheets), and it tends to be more common in winter months. People with problematic swelling or poor circulation in the legs can be more prone to nummular eczema.
Treatment
“Treatment includes routine use of thick moisturizers, avoidance of skin drying behaviors like long hot baths/showers, and working with a dermatologist to determine if topical medicines, antibiotics, or other therapies may be needed,” says Dr. Browning.
Home remedies
Again, moisturizing is essential. Vaseline or other thick emollients are ideal and should be applied multiple times daily. “Wet wraps or dilute bleach baths may also be recommended as part of a treatment regimen,” adds Dr. Browning.
What to watch for
Bacterial infections are not uncommon and can make any type of eczema more resistant to treatment if not recognized and appropriately treated.
“Like atopic dermatitis, patches of nummular eczema are often infected with Staphylococcus aureus (staph infection), which needs to be treated along with the skin inflammation to clear the condition,” Dr. Browning says. “In these cases, until the skin infection is treated, the eczema lesions are usually less responsive than normal to the topical medicines.”
Stasis dermatitis
Also referred to as venous eczema, stasis dermatitis is associated with poor circulation in the legs. It commonly occurs in older people as the valves in the legs get weaker with time and have a hard time pumping blood back up to the heart. This causes water and blood cells to collect in the lower legs.
Symptoms
Stasis eczema is most commonly found in the lower legs and feet, usually in people 50 years of age and older.
“The prevalence has been reported to be as high as 20 percent or more and may likely even be underdiagnosed,” adds Dr. Browning.
Swelling in the lower legs, ankles, and feet is one of the main symptoms. You may also have itching, scaling, dryness, and aching pain—especially after long periods of sitting or standing.
Symptoms can include orange-colored speckles sometimes called cayenned pepper spots, which develop when pressure causes capillaries under the skin to burst, according to the National Eczema Association. if left untreated, ulcers can form on the lower legs and tops of feet. They can bleed and leave scars after they’ve healed.
Treatment
If the skin is inflamed because fluid has leaded from ineffective veins, then it’s important to use topical prescription medication as well as using home treatments, says Dr. Browning.
Home remedies
Treatment is focused on easing swelling in the lower legs which can be achieved with compression stockings and other edema control measures. Elevating the legs above the heart whenever possible helps the blood move and return to the heart.
Be sure to check in with your doctor first. People with congestive heart failure, for example, can be sensitive to fluid shifts like this.
What to watch for
Poor circulation can impede the healing of severe skin breakdowns and ulcerations. Prolonged uncontrolled stasis dermatitis can also lead to permanent skin changes and scarring.
“I commonly hear patients with stasis dermatitis state they have been applying a triple antibiotic ointment to the affected areas because they fear it is an infection. Unfortunately, this commonly causes allergic contact dermatitis in addition to the underlying stasis dermatitis. This explains why so many dermatologists recommend Vaseline ointment as an at-home strategy while scheduling for an appointment with a dermatologist as it does not have the risk of developing a contact allergy,” says Dr. Browning.
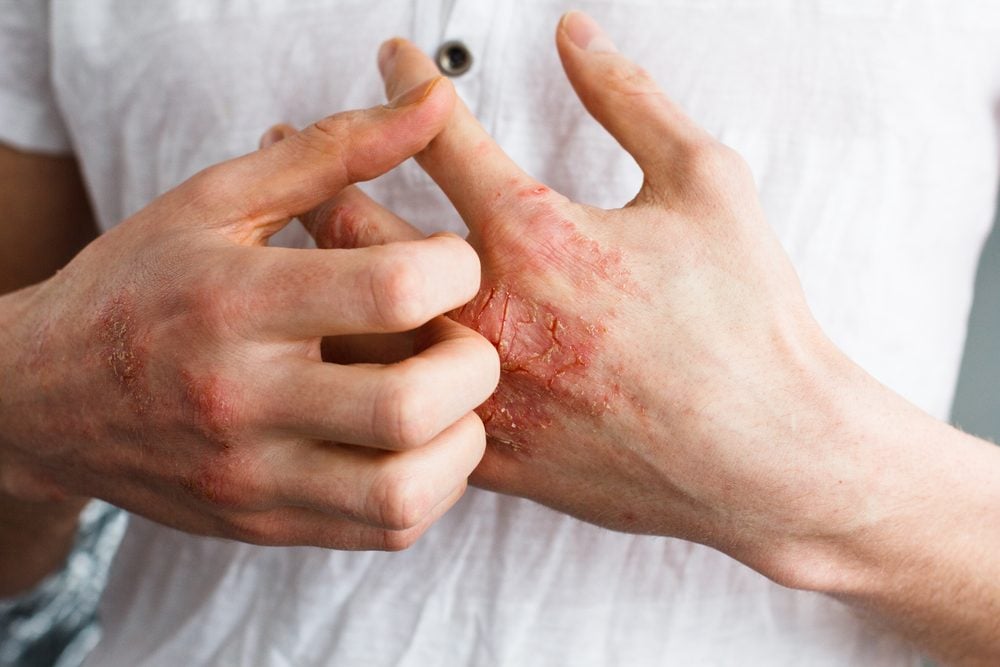
Dyshidrotic eczema
Pronounced dis-hi-drah-tic, this type of eczema mainly affects the hands, fingers, and feet with small blisters and dry, itchy skin. It’s quite common and associated with chronic recurrences, but symptoms are controllable.
Symptoms
Blisters only happen on the hands and feet and may start with a rash, itching, or burning first. As blisters start to heal and skin dries, it may turn red and peel. This leaves it dry and tender and can cause it to crack.
You might not be able to control some eczema triggers, such as the weather and temperature, infection, and underlying hand eczema, but other triggers such as allergies to nickel, cobalt, and chromium are easier to avoid. Excessive sweating of the hands and feet and stress are the most well-known triggers. There are prescription medicines to help with excessive sweating, and if you can learn coping skills to reduce worry and anxiety, you might avoid some flare-ups.
Complications can include bacterial infections if you don’t keep your eczema under control.
Treatment
“Treatment is based on severity,” says Pooja Sodha, MD, FAAD, director of cosmetic dermatology at George Washington Medical Faculty Associates, in Washington, D.C. “Cornerstone of treatment is topical steroids and avoidance of triggers. Phototherapy can be used to address severe recalcitrant (stubborn) cases. Oral corticosteroids can help to achieve faster control in severe flares. Botulinum toxin can be used to treat cases with underlying hyperhidrosis (excessive sweating), and oral antihistamines can help improve the itch,” says Dr. Sodha.
If you’re still scratching more than you are sleeping, be sure to check in with your dermatologist to find out what medicines or therapy could help with nighttime itching.
Home remedies
When your hands have blisters and itchy dry skin, it makes everyday life challenging. Walking and simple chores such as washing dishes can be a nightmare if dyshidrosis isn’t under control. Wear cotton gloves under waterproof ones when working with water and moisture-wicking socks to keep your feet dry.
As with other forms of eczema, there are things you can do at home to treat and soothe the itching and inflammation and help repair the skin barrier.
Dr. Sodha suggests gentle cleansers and applying thick emollients, such as Vaseline. Make it a part of your routine by using it after each handwashing and bathing. Repairing and replenishing the skin barrier helps prevent the skin from drying out and reduces flare-ups.
Neurodermatitis
This type of eczema affects up 12 percent of the total population, and women are scratching more than men with neurodermatitis—also called lichen simplex chronicus. Characterized by intense itching, the constant scratching can irritate nerve endings in the skin.
Symptoms
It initially appears as other forms of eczema, but as the itch-scratch cycle intensifies, the end-stage manifestation of chronic scratching results in a “lichenified” (tough or leathery skin) appearance and may develop pigment variations such as darkening or lightening, says Dr. Sodha. The itch, which can be intense, can occur anywhere on the body, including the genitals and the face, frequently strikes at night.
Previous research, including a study published in the British Journal of Dermatology, shows the reason for this type of neurodermatitis itch could have to do with one of its significant triggers—stress. Neurodermatitis is often initiated during extreme stress, anxiety, or emotional trauma. Anxiety and itching seem to kick into high gear as you try to relax or sleep.
Treatment
To soothe itching and reduce inflammation, topical steroids might be suggested for the acute stage, but only briefly as they can have a skin-thinning effect if used too long. Non-steroidal options such as topical calcineurin inhibitors, minimize this risk. They’re also safe to use on sensitive, thin skin such as the face, neck, and genital region, Dr. Browning says. More stubborn cases with bacterial infections might require systemic antibiotics.
Home remedies
When neurodermatitis is robbing you of sleep, establish a nighttime routine that includes a relaxing technique. To keep yourself from scratching in the middle of the night, cover trouble spots with topical creams recommended by your dermatologist. Make sure you cover the areas with socks, gloves, bandages, or gauze. Layering ointment with a cloth keeps fingers from scratching the skin and helps the medicine penetrate the skin. As always, use Vaseline and gentle cleansers and avoid known triggers.
Seborrheic dermatitis
“Seborrheic dermatitis is an inflammatory rash caused by our body’s immune response to an overgrowth of normal yeast called Malassezia that lives on human skin. Roughly 10 percent of the population will experience this at some time during their lives,” says Dr. Browning.
Symptoms
This inflammatory rash is found on parts of the skin that tend to get oily, like the sides of the nose, mid-chest, upper back, armpits, groin area, eyebrows, and eyelids. You’re likely most familiar with the mild form of it when it appears as dandruff on the scalp. There’s usually some redness, swelling, flakiness, and greasy scaling on the affected areas.
Treatment
Because yeast overgrowth is the offender, seborrheic dermatitis calls for a different kind of treatment than the other eczemas. At first, over-the-counter hydrocortisone might be used for mild cases, but prescription strength may be necessary in more serious situations.
“I often educate my patients that we will utilize a prescription-strength version of hydrocortisone or a similar alternative to get clearance of the rash, but once clear, maintaining clearance in this often chronic condition is safer with use of antifungals like ketoconazole,” says Dr. Browning. This is available in shampoo and cream forms.
Seborrheic dermatitis often lasts for years, yet it may come and go due to dry and cold weather, stress, and hormonal changes. The risk for developing seborrheic dermatitis increases in people with HIV (human immunodeficiency virus) or who have a suppressed immune system for other reasons, as well as those with a history of neurological diseases like stroke or Parkinson’s disease, Dr. Browning says.
Tips for managing eczema
Dr. Browning explains to his patients that eczema is often a chronic condition that waxes and wanes. Emotional and physical triggers can set it off, so it’s key to be mindful of what those triggers are for you.
And eczema isn’t just a condition that affects your skin. Managing and coping with eczema can take a toll on your mental health too. “The chronicity of the itch-scratch cycle can lead to significant psychosocial impairment—negative moods, poor social skills, sleep disturbances, and sexual dysfunction. For this reason, treatment is so vital,” says Dr. Sodha. Here are a few more self-care tips to help you cope at home:
- Keep your fingernails short to protect your skin from damage and infections.
- Use a humidifier to add moisture to the air whenever heat or cool your home.
- Wear loose and moisture-wicking clothing if you’re prone to sweating.
- Stash creams and gels in the fridge for cooling relief of inflamed skin.
- Moisturize daily after bathing and apply moisturizer more frequently when seasonal weather dries out the skin.
- Remove rings or snug-fitting bracelets while cleaning and washing your hands to keep irritants from getting trapped beneath.
- Wash new clothes in an eczema-friendly detergent before wearing them.
Additional resources
For more help and information on the different eczema types, consider these resources: