How to tell it’s eczema
Eczema is a skin condition where the skin barrier is not functioning as well as it should be. The immune system in the skin is also not working optimally, so people with eczema are more likely to develop skin infections. To tell if you have eczema, you need to know your symptoms. “Your skin becomes dry, itchy, and easily irritated, and there can be a rash with skin that is scaly and thickened,” explains Jeffrey Benabio, MD, a dermatologist with Kaiser Permanente in San Diego. People tend to get the rash on certain parts of the body depending on their age. Common sites for babies include the scalp and face (especially the cheeks), the front of the knees, and the back of the elbows. In children, common areas include the neck, wrists, legs, ankles, the creases of elbows or knees, and between the buttocks. In adults, the rash often appears on the inside of elbows and knees and on the nape of the neck, sometimes accompanied by a yellowish to light brown crust or pus-filled blisters. Localization on the hands or feet, known as dyshidrotic eczema, is also common.
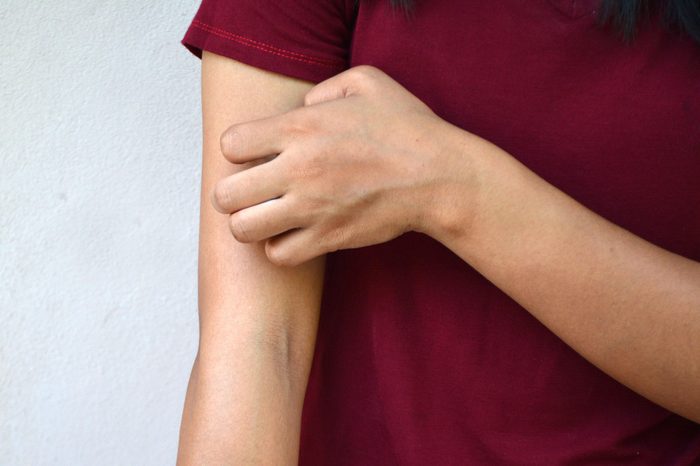
Scratching makes eczema worse
Anyone who’s ever had poison ivy or a mosquito bite knows how powerful the urge to scratch can be, but especially with eczema, it can lead to a vicious itch-scratch cycle. “The initial itch prompts the patient to scratch, which provides transient relief,” explains Steven Q. Wang, MD, director of dermatology and dermatologic surgery at Memorial Sloan Kettering Cancer Center in Basking Ridge, New Jersey. “However, the scratching motion creates micro-tears in the skin barrier and triggers inflammation, which leads to more itch.” Here are home remedies for eczema worth trying.

Eczema is not just skin-deep
You may see signs of eczema only on the skin, but it can cause other troubles in the body as well. In a 2015 study in the Annals of Nutrition and Metabolism, researchers found that people with atopic dermatitis, the most common type of eczema, are more likely to develop asthma and sensitivities or allergies to foods and airborne allergens. For example, some 50 percent of children with eczema are sensitive to cow’s milk protein. Then there are issues of not being able to fully flex parts of the body that are stricken by the rash—and of course the embarrassment some people feel at always having a rash on their body. “It is important to know that eczema is not only a skin condition,” Dr. Wang says. “It impacts sleep, concentration, and overall well-being.” (Check out the other surprising signs of disease your skin can reveal.)

You’ll need to read ingredient labels
You don’t want to just put any old soap or cream on skin that’s already inflamed. According to Alejandra Vivas, MD, a dermatologist in Hollywood, Florida, you’ll need to stick to a skincare regimen for sensitive skin, and use the right products, along with topical steroids and other appropriate treatments. Here’s what you definitely don’t want in any skincare products, according to the National Eczema Association: glycolic acid, salicylic acid, or retinol; products with the preservatives methylparaben or butylparaben, which can exacerbate inflammation; and any products with fragrance, which can trigger flare-ups. (See how changes in the weather can affect your skin as well.)

Your skin is desperate for hydration
Eczema is a condition of excessive dryness, so it needs major moisturizing. Dr. Vivas recommends moisturizing several times a day to keep skin hydrated, especially after showering, while skin is still damp. “That’s when you’ll get maximum absorption,” she says. Dr. Vivas recommends ointment-like formulas such as Aquaphor Advanced Therapy Healing Ointment and Avene XeraCalm A.D Lipid-Replenishing Cream, a new product proven to significantly calm itch, decrease dryness, and help rebuild the skin natural barrier. Dr. Wang recommends his own product, Dr. Wang Herbal Skincare Eczema Ointment Natural Repair, which he says can bring soothing relief for intense itch within an average of six minutes. To preserve skin moisture, don’t spend too much time in the shower (and feel free to skip the daily dip), as it can dry out your already dry skin. “To avoid a flare-up, take one five- to 10-minute bath or shower daily in lukewarm water,” Dr. Vivas suggests. “And avoid scrubbing and unnecessary use of soap.” In fact, skip bar soap altogether in favor of a sensitive skin formula like CeraVe Eczema Soothing Body Wash. (Here are dermatologists’ rules for using moisturizer.)

You’ll want to switch up your laundry soap
If you have eczema, your skin is so hypersensitive that even the laundry detergent you use can trigger a flare-up. Dr. Vivas recommends choosing hypoallergenic detergents such as Tide Free or All Free and Clear, which are free of dyes, fragrances, and irritating residues and still manage to get your clothes clean. “Fabric softeners including dryer sheets should be avoided,” she adds, as they’re chock-full of irritating fragrances and other chemicals. Don’t be surprised if some of your clothing, especially pieces manufactured with dark dye, also exacerbates your eczema.

You’re surrounded by triggers
Many everyday items are known to make your eczema worse, and you’ll want to avoid them as much as possible. “Harsh soaps, shampoos, and cleaning products such as dish soap can make your eczema flare,” says Janet Prystowsky, MD, a dermatologist in New York City. “Allergens like pollen, mold, and pets can also cause flare ups.” Stress can also worsen eczema, as can skin infections, certain temperature and humidity situations and fluctuations, dietary allergies, and hormonal changes. “Some common food allergies associated with eczema include milk, eggs, wheat, fish, and nuts,” Dr. Prystowsky says, “however, not everyone who has eczema will be triggered by a food allergy.” (Check out the weird things that make your allergies worse.)

Genetics can play a role
If you or a member of your family has eczema, others may develop it too, as the condition seems to have a genetic component. In identical twins, 77 percent will both have eczema, but it affects both fraternal twins only 15 percent of the time, according to a 2015 study in the Journal of Allergy. Another indication that eczema is genetic is the fact that people with celiac disease (an inability to digest gluten properly) are three times more likely to have eczema; and relatives of people with celiac disease are twice as likely to have eczema.
You don’t have to suffer from eczema alone
Two large clinical trials that looked at a relatively new eczema drug, dupilumab, found that it helped ease test subjects’ eczema-related itching within two weeks and cleared it entirely within a few months, according to a study published in 2016 in the New England Journal of Medicine. The drug works by blocking two molecules of the immune system that are overproduced in patients with eczema and other allergic diseases. It was first approved by the FDA in March 2017, and approved for eczema in 2019. There are also other options to control the symptoms. Your dermatologist might prescribe topical creams and ointments that minimize the inflammation, and other topical creams and ointments that help repair the skin barrier defects that let water out and allow chemicals to come in. You might also be prescribed antibiotics to address any bacterial overgrowth (staph infection), according to Fayne Frey, MD, a dermatologist and dermatological surgeon in West Nyack, New York. Anti-itch medications can also help; your doctor may recommend antihistamines to relieve the itch or a prescription corticosteroid like prednisone to relieve inflammation.
