How to Tell the Difference Between Psoriasis, Rosacea, and Eczema
Updated: Jun. 22, 2021
When it comes to skin conditions like rosacea, psoriasis, and eczema, they have some similar and some unique symptoms, treatments, and ways to prevent flare-ups. Here's how to tell them apart.
Rosacea vs. psoriasis vs. eczema
Rosacea, eczema, and psoriasis can sometimes look and feel alike. They can include itching, rashes, and redness, which are common symptoms of chronic inflammatory skin conditions.
It’s not always clear what causes them and there is no cure for any of them—although they can go into remission, meaning symptoms disappear for a while but may come back. So, how do you know which one you have?
The differences between each condition go more than skin deep—in terms of specific symptoms, treatment, triggers, and how they impact the overall health of the body.
Here’s a guide to help you identify the differences between rosacea, eczema, and psoriasis.
Rosacea
Rosacea is a chronic condition that mainly targets the face that presents as flushing or redness of the cheeks, nose, forehead, and chin. More than 16 million Americans have rosacea, yet most don’t realize they have it, according to the National Rosacea Society.
The cause of rosacea is unknown, but people who blush or flush easily, have fair skin, and are of European descent seem to be more prone to rosacea.
Over time, the flushing becomes ruddier and appears more often with visible blood vessels. It is typically seen in men and women after 30, yet women are diagnosed with rosacea more often. This could be because women seek treatment more than men, says Pooja Sodha, MD, FAAD, director of cosmetic dermatology at George Washington Medical Faculty Associates, in Washington, D.C.
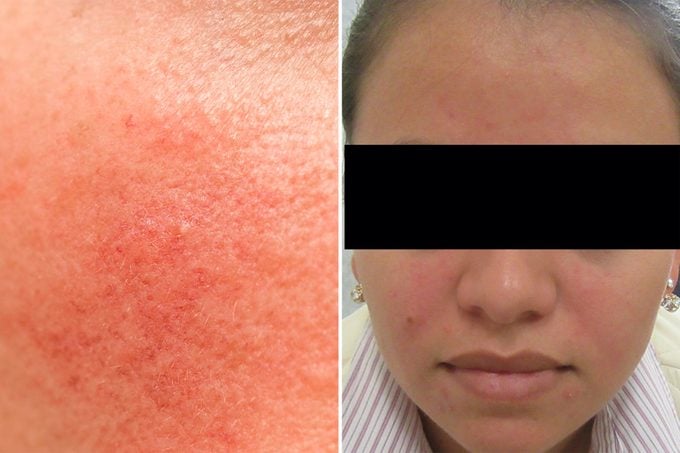
Symptoms of rosacea
Symptoms and their severity vary by individual, but typically, symptoms worsen with age, especially if the condition goes untreated. “Men, in particular, often have more severe cases, Dr. Sodha says.
“Men are more commonly afflicted with a progressive variant affecting the nose, known as phymatous rosacea,” says Dr. Sodha. That’s when the skin on the nose is thicker with irregular lumps and enlarged pores.
People with rosacea shouldn’t ignore or delay seeing their doctor if they have symptoms such as redness, irritation, bloodshot eyes, or watery eyes. “Long-standing untreated symptoms increase the risk of developing eyelid scarring and progressive vision loss from corneal ulcers,” Dr. Sodha cautions.
Common symptoms include:
- Flushing or redness along the nose, cheeks, chin, and forehead that last a few minutes or is persistent
- Rough or scaly skin
- Visible, fine blood vessels
- Stinging and burning
- Itching
- Inflamed red bumps and fluid-filled bumps
- Swelling
- Redness, inflammation, and irritation of the eye and eyelid and/or watery and bloodshot eyes
- Thickening of the skin with irregular lumps and enlarged pores and pimples
Rosacea treatments
While there is no cure for rosacea, it is treatable with medications and proactive measures to control and manage rosacea flare-ups. However, there is no single definitive treatment or course of medications that fits every person who has rosacea.
“Though it is difficult to predict which treatment will be most effective until a trial of the treatment regimen has been initiated, there is an extensive arsenal of options, often aligned with the subtype of therapy,” says Dr. Sodha. “A skin care routine of a very gentle cleanser, soothing moisturizer, and sunscreen should be a part of every treatment regimen.”
Treatments include anti-inflammatory and antimicrobial ointments and pills, and anti-parasite creams. The anti-parasite targets the demodex mite. (They aren’t as scary as they sound. These are mites that live on our hair follicles and are quite common, but they often cause trouble in people with rosacea.)
Retinoids may be prescribed for stubborn cases of pimples and fluid-filled bumps. For rosacea that surrounds the eyes and eyelids, Dr. Sodha recommends warm compresses, neutral baby shampoo, and lubricating eye drops. Vascular laser and pulsed light treatments can minimize redness, pimples, and visible blood vessels.
Finally, it might be wise to check on the status of your body’s microbiome—the collection of naturally occurring microorganisms that live in your gut and elsewhere on the body—as it affects skin health. “Research suggests that rosacea patients have a higher prevalence of small intestine bacterial overgrowth,” says Dr. Sodha.
Rosacea flare-up prevention
In addition to medical therapy, people with rosacea can stay in remission and minimize flare-ups by identifying and avoiding specific triggers. (Triggers include things like food, the weather, cosmetics, stress, illness, medication, and other factors).
However, triggers can be highly individual. What causes a flare-up for one person might not have an impact on another person. It is useful to keep a diary to identify things that prompt a flare-up.
A National Rosacea Society survey of 1,066 rosacea patients found there are some rosacea triggers that are more common than others. The top five from the survey are sun exposure (81 percent), emotional stress (79 percent), hot weather (75 percent), wind (57 percent), and heavy exercise (56 percent).
Psoriasis
“Psoriasis is an immune-mediated inflammatory condition (a dysfunction of the immune system that causes inflammation in the body) that affects the skin and joints driven by environmental exposure and genetic predisposition,” says Dr. Sodha.
The National Psoriasis Foundation reports about 8 million Americans experience psoriasis, and chances are if you have psoriasis you probably have family members who have it too. “There is a tendency to see this condition manifest in families, with more than 45 percent heritability in the first and second-degree relatives,” says Dr. Sodha.
Usually, your body grows new skin cells and sheds them every 30 days. In psoriasis, the immune systems go into overdrive and produce new skin cells every three to four days. But, instead of shedding, the dead skin piles up on the skin’s surface that looks like raised reddish patches with a thick layer of the silvery-white buildup of dead skin cells that looks scaly.
What isn’t visible is the impact psoriasis has beneath the skin, including on the joints of the body. One in three people with psoriasis develop psoriatic arthritis, a disease that causes stiffness, swelling, and pain in the joints and areas surrounding the joints.
Chronic inflammation in psoriasis is associated with other serious conditions such as cardiovascular disease, type 2 diabetes, anxiety, and depression. If you have psoriasis, take action to stay ahead of these conditions by making healthy lifestyle choices and get screened for these conditions.
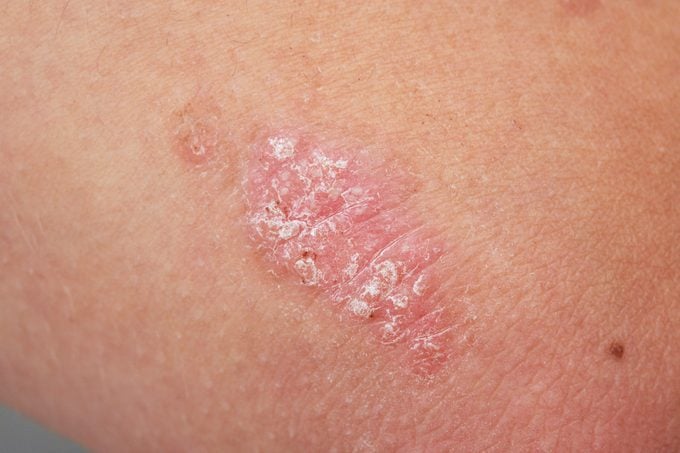
Symptoms of psoriasis
Psoriasis symptoms can happen at any stage of life, but typically they occur between the ages of 15 and 25 and affect people of all ethnicities. The most common symptom are raised reddish patches with a thick layer of silvery buildup of dead scaly skin.
Called plaques, these skin patches affect 80 to 90 percent of people with psoriasis, Dr. Sodha says. The plaques can be few or widespread, and are usually symmetric in pattern. Plaques can appear anywhere on the body, but most often on the elbows, knees, scalp, trunk, and buttocks.
Other symptoms include:
- Itching, burning, and stinging skin
- Shedding skin
- Nail splitting, changes in color, and thickness of nails
- Lesions in the skin folds, such as armpits, genitals, groin, and breast
- Pustules over the plaques, widespread small drop-like lesions and general redness
Psoriasis flare-up prevention
As with rosacea, specific triggers can make psoriasis symptoms feel worse. “The disease can be instigated or worsened by certain medications (classically beta-blockers, lithium, and antimalarial drugs), skin trauma (sunburn, bug bites, vaccinations), infections, pregnancy, and stress,” says Dr. Sodha.
Anything thing jolts your immune system can bring about a painful flare-up. That could be a cold, strep throat, or even an ear infection. And it’s a good time to think about quitting smoking if you’re a smoker.
“Smoking has been shown to be increased in prevalence in those with psoriasis and increases the severity of psoriasis,” says Dr. Sodha.
Psoarisis treatments
There are a lot of options when it comes to treating psoriasis. Everyone responds differently to treatment, so relief or remission may come in the form of a combination of over-the-counter medications with prescription medications or phototherapy.
“Mild to moderate skin limited disease can be treated topically with a combination of steroids, emollients such as Vaseline mixed with salicylic acid, retinoids, and vitamin D. Phototherapy treatment exposes the skin to an artificial UVB light source, according to the National Psoriasis Foundation.
When used regularly, it can slow the growth of affected skin cells. Moderate to severe psoriasis with or without arthritis typically requires systemic treatment in the form of small molecule disease-modifying drugs, such as methotrexate and systemic retinoids or biologics,” says Dr. Sodha.
Biologics are created in a lab to mimic naturally occurring proteins and molecules, and are given as an injection or IV. (Find out how biologics became the psoriasis solution that gave this woman her life back.)
Eczema
Also called atopic dermatitis, eczema is a common allergic skin disease that causes itchy skin. The exact cause of eczema is unknown, but environmental triggers and genes are known factors.
It often starts in early childhood. “Eczema is an inherited skin condition. It is often associated with asthma or allergic rhinitis (hay fever). It is very common, and it has been estimated that over 10 percent of individuals in Western countries are affected,” says Jeffrey Weinberg, MD, associate clinical professor, Mount Sinai, New York.
Exposure to things outside or inside the body, like detergents, pollens, food, and some bacteria, can prompt inflammation and cause eczema symptoms.
A 2017 study published in the Journal of Allergy and Clinical Immunology found that some people with eczema don’t have enough filaggrin, a protein creates a protective barrier on top of the skin to help keep moisture in and bacteria and viruses out.
If your filaggrin is on the fritz, it makes your skin more prone to dryness and infection. According to the American Academy of Allergy, Asthma, and Immunology, a faulty filaggrin is a culprit for moderate to severe eczema in about a third of people of North European and Eastern Asian descent.
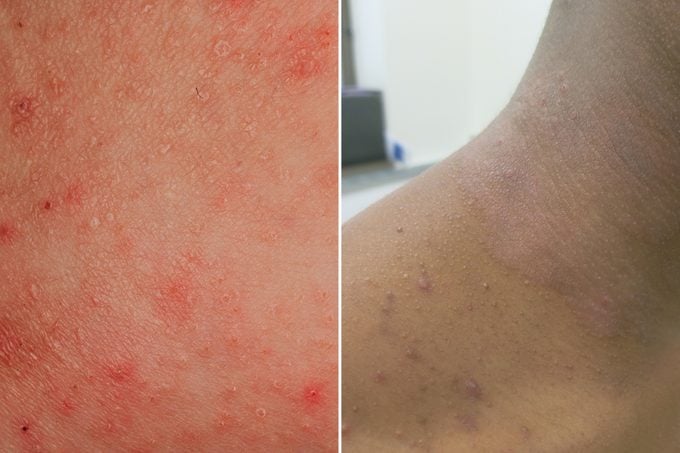
Symptoms of eczema
The main symptom is itchy skin. Where the itch is located will depend on the individual. Children tend to have eczema on their cheeks, elbows, knees, and scalp. In adults eczema typically shows up in the creases of the face and neck, wrists, elbows, knees, and ankles.
Sometimes, itching is so intense, scratching it leaves the skin susceptible to infection. “Chronic eczema can be associated with impaired health as a result of systemic inflammation. People with eczema are at risk of skin infections,” says Dr.Weinberg.
Infections such as staph and herpes can be very serious, as they can spread across the body and should be treated immediately.
Other symptoms include:
- Itchy skin
- Dry skin
- Red or inflamed skin
- Chafed or scaly patches of skin
- Bleeding (from scratching)
- Swelling
- Crusted or oozing skin
Eczema flare-up prevention
What may trigger your eczema may not bother someone else at all. Dr. Weinberg says harsh soaps and environmental allergens, like dust mites, animal dander, and cigarette smoke, are common eczema triggers.
Be mindful of things that cause dry skin, like the cold, dry air of winter and frequent bathing without applying a high-oil content moisturizer afterward.
Be alert of possible irritants such as wool and polyester clothing, and wash new clothes before wearing them. (Remember to use fragrance-free detergent!) Fragrances, household disinfectants, and cleansers, and even the nickel found in jewelry, zippers, and snaps are common triggers.
Eczema treatments
Chronic itching associated with eczema can be unbearable at times, even debilitating. The intensity can be more frustrating than a mosquito bite or poison ivy itch, except the antihistamines that work for those bites don’t help the itching that comes from eczema.
The key to battling itchy, dry skin is moisturizing frequently, says Dr. Weinberg. “Eczema is usually treated with topical medications, including topical corticosteroids and non-steroids,” says Dr. Weinberg. As with psoriasis, biologic agents and phototherapy are also used to treat eczema. Immunosuppressants help control symptoms.
Natural and alternative treatments approved by the National Eczema Foundation include sunflower seed oil, apple cider vinegar, and bathing with colloidal oatmeal. It’s always good practice to discuss any treatment with your doctor before trying it.
How skin conditions may impact mental health
Whether it’s the unrelenting itching or how you feel about the appearance of your skin—or just being mentally exhausted from managing your symptoms—rosacea, psoriasis, and eczema can really impact your mental health.
A 2015 study in Nature Reviews Immunology suggests that when there’s skin inflammation, neuro-connections let the brain know. As a result, you could feel depressed, anxious, tired, and have foggy thinking.
Managing these skin conditions can be grueling and exhausting on your body and your emotional well-being, so don’t put off asking for help.