“My Psoriasis Got So Bad that I Nearly Gave Up”
Updated: Jun. 17, 2021

About 125 million people around the world have psoriasis, a skin condition that can be devastating. Here's one woman's story of surviving the chronic disease that once controlled her life—and learning how to thrive.

For Jennifer Kerner, 35, psoriasis made its unwelcome introduction during middle school. That’s not unusual—people often develop psoriasis between the ages of 15 and 35. Plaque psoriasis, Kerner’s eventual diagnosis, typically starts with patches of unsightly red, scaly skin on the elbows, scalp, or knees. With an autoimmune disease like psoriasis, the body’s own defenses turn on healthy tissue leading to scarring and damage; psoriasis is often linked to other conditions such as type 2 diabetes, cardiovascular disease, and psoriatic arthritis. According to a 2016 study published in the journal American Health & Drug Benefits, the negative mental impact of psoriasis is significant: People who have the condition are at greater risk for depression and suicidal thoughts.
Psoriasis expert Mark Lebwohl, MD, a dermatologist with Mt. Sinai Beth Israel in New York explains: “There’s a huge social impact for patients. I’ve heard of hairdressers turning patients away, as well as blood banks not allowing them to donate. There’s a fear that it’s contagious, and sometimes it even results in job losses and absenteeism.” He says the disease can isolate people: “People with psoriasis are often hermits, living at home with no life. Someone once said, ‘Psoriasis is not fatal, but dealing with it is murder,’ and that’s a great description of it. It’s a devastating disease.”
“Psoriasis gets triggered by inherited genes from both parents, along with a combination of environmental triggers,” he says. “We have phenomenal treatments today for it, but it’s really a matter of access to them, due to cost and insurance restraints.” Some people try home remedies for psoriasis, as well. Here’s how Kerner survived—and found a way to thrive.
What’s setting my skin on fire?
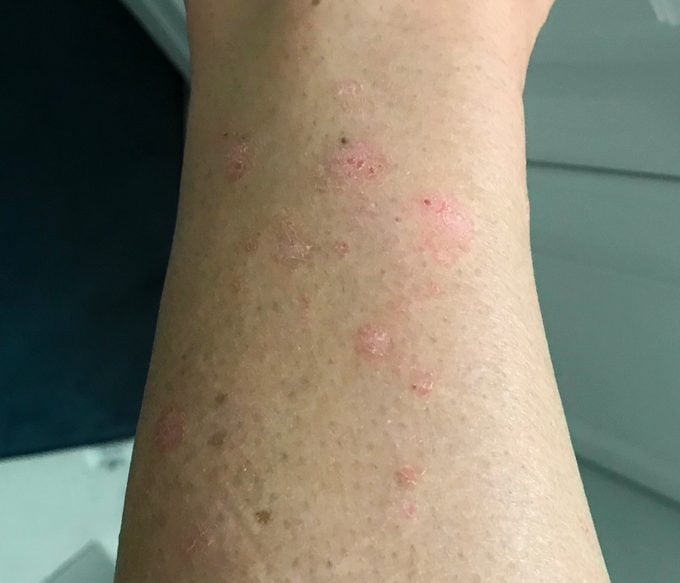
When I was a kid I had skin issues, but it wasn’t until middle school that I began having flare-ups of red, itchy patches of skin on my elbows and knees. I didn’t know what it was or what to do about it. Both of my parents were in the medical field at the time—before retirement, my father was a physician and my mother was a nurse—but no one thought of psoriasis. By high school it became worse—the patches were now more visible. They were on my arms and legs, and to cover them up I would wear long sleeves, turtle-necks, and pants—all the things you shouldn’t do with psoriasis because it overheats the skin and makes it worse. My parents made me an appointment with a dermatologist, who finally made the diagnosis. I was relieved—I had been so scared that it was some terrible disease.
The doctor told me I would need to put the topical ointments all over my body and then wrap it in cellophane in order for it to really work. She also warned me it would stain my clothes and bedsheets—basically anything that touched my skin would discolor. High school is so hard because you’re figuring out life and trying to be excited about college. When you have a disease like psoriasis, you’re self-conscious, but on top of that, it’s just emotionally painful. [Check out these psoriasis treatments.]
Growing up with psoriasis
In college, I continued to have flares while I struggled to maintain my treatment plan. I was afraid to borrow clothes from my friends or even sit on their beds while watching a movie because I knew I would ruin their sheets. People could also be really harsh and cruel with their questions and judgments. They’ve asked if I’m contagious. It looks painful, so I often get asked if it hurts. Sometimes little kids ask if I’ve been burned. Other people are more hurtful, making comments that I must have done something to myself to get a rash like this.
Fighting more than just itchy skin
Psoriasis hasn’t kept me from doing what I want. I love to travel and have been around the world. I’m a competitive equestrian and an endurance athlete, but I do get flare-ups a lot: My triggers have a lot to do with mental or emotional stress, weather changes, and physical stress of clothing rubbing against skin. I have to protect my skin from the sun, but I’ve yet to find a sunscreen that doesn’t also irritate my psoriasis.
Like many people with a psoriatic illness, I also have irritable bowel syndrome, so the flare upsets my gut, and my gut can also trigger a flare. During a flare-up, my tonsils and lymph nodes often swell, and my skin will feel as though I’m covered with fire ants. Fatigue also hits hard. Not everyone experiences psoriasis in the same way, but even mild flares cause skin to swell and make me feel bloated—like my clothes no longer fit. During a flare, I just don’t want to see anyone or touch anyone. It’s an uncomfortable place to be. [Here are the 10 things dermatologists want you to know about scalp psoriasis.]
Finding treatment that works
In high school, I heard about biologic medications, but they were described as a last resort. The doctor told me at the time that it would make me infertile, and increase my susceptibility to infection—and that they’re incredibly expensive. But after years of trying every topical medication available, I was determined to find another option. I went to one doctor, and she was hesitant when I brought up the idea of a biologic. She didn’t want me to be on it for the rest of my life, but she had no other solutions for me. I found another doctor after that. The next doctor listened to my story, and the first words out of his mouth were, “We’re going to put you on a biologic.” I burst into tears at that point, because it was the first time anyone had taken me seriously. I began giving myself biologic injections every two weeks, and I felt like a new person. [Check out these 8 proven treatments for plaque psoriasis.]
I have my free time back
Since starting the biologic medication I feel like my nights, mornings, and weekends are my own again; they used to be my recovery times. At its core, psoriasis is an overactive immune system, and biologics put a monkey wrench in the immune system function. That means I’m more susceptible to infections. And it’s important to know that biologics aren’t a cure, but they do keep my body from going into a flare.
I feel like I’m making up for lost time. I think about all of the marathons and activities I did while sick—and think about how much more I could have enjoyed them, or how much better I could have done. I haven’t had any bad side effects, I’m sleeping better, and I can have most of the foods I want to eat. This is a freedom I haven’t had. [Here are the 7 foods that can make psoriasis worse.]
What I’ve learned
I’m a scientist and consultant [with Booz Allen Hamilton in Washington, DC], so maybe it’s more natural for me to do this, but I record my symptoms meticulously. When you have a chronic illness, it’s up to you to be your biggest advocate. You are the expert on your condition. I take photos of my skin constantly because the law of psoriasis is that as soon as you walk into a doctor’s office, your skin will clear up. I document how it’s affecting my daily life as well. I’ve lived in six different states, so it’s important that I have all of the information with me. For parents of children with psoriasis, they’ll have to do the tracking while also teaching their child to be their own advocate: At the end of the day, encourage them to take an inventory of how their skin is doing. When you ask, “How was school today?” also ask, “How’s your skin feeling?” and then record that information for them. You can explain to them that not all of their friends have this, but they do, and it’s going to be okay.
There is a way to live with psoriasis
In high school, I felt like a monster, and my immediate thought was that there’s no cure. And psoriasis is such a struggle because a lot of people don’t realize how disruptive this disease is to daily life—there have been so many doctors that didn’t believe me. But I didn’t give in and I didn’t give up. I want to inspire others to do the same because now I’m enjoying everything so much more. [Learn more about this disease at the National Psoriasis Foundation. Kerner is running a 50K as part of the Marine Corps Marathon to raise money for psoriasis research—learn more.]

















