9 Ways to Get Rid of Hives Fast According to Experts
Updated: Mar. 16, 2022
Soothe itchy skin and ease discomfort with these expert-recommended methods for treating hives—from home remedies to prescription meds.
Dealing with hives
Suddenly afflicted by mysterious red bumps on your body? It can be hard to know just what they are, but a common culprit is hives.
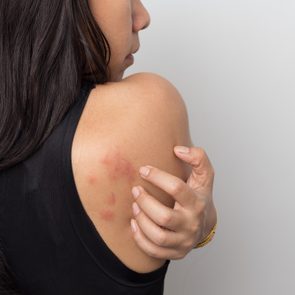
“Hives are a pale red, raised, itchy rash that occurs when your immune system is activated by something in your skin,” says Flora Waples, MD, medical director of Restor Medical Spa in Denver. They may look like raised bumps or welts.
Even though hives are extremely common and can be triggered by what you might think are benign events (like wearing too-tight workout clothing), they can be alarming the first time they occur.
And they’re especially worrisome if they keep flaring up and disappearing over and over, which may be a sign of something more serious, like an autoimmune disorder.
We spoke with dermatologists about the things that cause hives and, more important, how to get rid of them fast.
What are hives?
If you’ve had hives before, you know how irritating they can be. And you probably understand why many people add embarrassment to the list of side effects.
Officially known as urticaria, hives are red, itchy, angry welts that appear on the skin anywhere on the body, explains Annie Gonzalez, MD, a dermatologist with Riverchase Dermatology in Miami.
“They can be small or large,” she says. “They are usually pink, flesh-colored, or red, and in some cases, they can sting and swell.”
While they may have a similar appearance to a rash, there are differences. Hives are frequently raised, may be colors other than red, and are often itchy, especially because they’re commonly an allergic reaction.
Hives are extremely common, says Kelly Bickle, MD, a dermatologist in Santa Monica. “Twenty-three percent of adults experience at least one episode of acute urticaria in their lifetime.”
What causes hives?
The causes of hives are varied, but a common trigger is allergies.
“Hives are typically caused by an allergic reaction to something that you have come into contact with or ingested,” explains Dr. Gonzalez.
In response to this foreign invader, your immune system mounts an attack. Your body releases histamine into your blood, and that can cause hives in some people.
What exactly are these “foreign invaders”?
“If you want to get technical, anything that activates your immune system can cause hives, so depending on your personal immune systems like and dislikes, hives can be caused by literally any molecule in existence,” says Dr. Waples. “That being said, some are much more common than others.”
She cites bug bites, contact with a food or substance that you are allergic to, and medications as common triggers. Pollen and pet dander are also common culprits.
Stress can also trigger hives, according to Jennifer Segal, MD, founder of Metropolitan Dermatology Institute in Houston.
In fact, research points to a solid link between stress and hives. A small study published in 2018 in Advances in Dermatology and Allergology found that women experiencing chronic hives also reported much higher levels of stress.
Of course, that doesn’t mean stress directly causes hives. Further research is needed before scientists can say that for sure.

How to treat hives
There are many ways to treat hives, says Dr. Waples, and luckily many treatments work quickly.
“Most hives go away within 15 minutes of application of medications,” she says. “But they can frequently come back in crops, every four to six hours, and this can sometimes go on for a couple of days while you are working whatever the offending substance was out of your body.”
Use a cold compress
If you’re experiencing a flare-up, try using a cold compress on the affected areas, says Dr. Gonzalez. It may alleviate symptoms like inflammation and itching.
Just skip this remedy if your hives are caused by an extreme drop in temperature, a condition called cold urticaria.
Lower the thermostat
Keep the temperature in your house cool, if possible. Extreme temperatures may trigger hives, so aim for a middle-of-the-road cool temp.
Take a lukewarm bath
Baths are more than just fantastic stress relievers; they’re also great at reducing the severity of your hives.
Dr. Gonzalez recommends taking a lukewarm bath with an anti-itch solution, such as colloidal oatmeal, which is known to soothe skin.
Wear lightweight clothing
One of the most common causes of hives is friction against the skin.
This can occur when you’re wearing heavy clothing, too-tight clothing, or compressive gear, such as workout clothes.
If you find that you’re constantly breaking out in hives when wearing certain types of clothing, consider swapping the offending items for lightweight, breathable clothes, says Dr. Gonzalez.
Avoid the sun
Sunlight is a known trigger for hives. Interestingly, while heat can cause hives, that’s not necessarily the case with sunlight-induced urticaria. The rays themselves cause hives to flare up.
If you’re prone to hives or have noticed previous bouts with sunbathing or extended sun exposure, cover up with loose-fitting sun-protective clothing or stick to shady areas.
Whenever possible, says Dr. Gonzalez, avoid exposure to direct sunlight.
Use calamine lotion
It might trigger unpleasant images of childhood, but calamine lotion is a first aid staple for a reason: it really works. Applying calamine lotion to your hives can help provide relief, says Dr. Gonzalez.
(These are the best natural remedies for rashes and irritation.)
Take Benadryl
While Benadryl (otherwise known as diphenhydramine) is the most well-known and often-cited antihistamine, any antihistamine (including Zyrtec, Claritin, and Allegra) will work to help counteract hives.
“Oral antihistamines are the cornerstone of treating hives and are most effective when taken continuously,” says Dr. Segal.
Topical antihistamines are typically less effective than oral antihistamines, she says.
Try topical or oral steroids
Topical steroids can help for short-term relief but are not recommended long term because they can thin the skin over time, says Dr. Segal.
“Oral steroids can be effective but should really only be used in the setting of curbing an acute severe hive reaction, and then in combination with antihistamines, due to the potential for a flare once the steroids wear off,” she says.
Dr. Waples also cites 1 percent hydrocortisone, a topical corticosteroid, as a popular option for treating hives.
Treating chronic hives
When hives become a long-term daily occurrence, they’re considered chronic hives.
“When new outbreaks occur approximately every day for six weeks or more, it’s considered chronic,” Dr. Gonzalez says.
People who get chronic hives tend to be between the ages of 20 and 40. The good news is that chronic hives are not very common. Only 1 percent of the population experiences them.
The disturbing news is that chronic hives are often a result of an underlying illness, like lupus or a thyroid disorder.
You’ll need to see your doctor for treatment. Chances are, you’ll need an allergy and/or autoimmune workup, which will help identify potential root causes.
Take prescription medication
“If you’re experiencing severe or chronic hives, prescription medication may be necessary,” says Dr. Gonzalez. “Talk to your doctor about your symptoms and how you can best find relief.”
She recommends a variety of options, including the oral corticosteroid prednisone (Deltasone) and the antibiotic dapsone (Aczone), which is available topically and as an oral medication.
There are also leukotriene receptor agonists, nonsteroidal drugs that can be taken orally.
Modify your lifestyle to get rid of hives
Researchers are still trying to determine whether stress can directly cause hives. But most agree that stress can play some role in hives.
“The reason stress can trigger hives is that chemical changes occur in the body in response to stress,” Dr. Gonzalez says. “These changes cause the blood vessels to leak and expand, leading to swollen and red skin patches—hives.”
Her advice is simple: “Do what you can to minimize stress in your life.”
Consider stress-reduction techniques, like:
When should you see a doctor?
While hives are common, in rare cases they can become extremely serious and warrant immediate medical attention.
Chronic hives in particular warrant a trip to the doctor to figure out the root cause, says Dr. Bickle. But she warns that this may be a long, difficult road.
“It can sometimes be hard to determine the cause of chronic urticaria, which can make it challenging to treat,” she says. “Treating the causative agent, if it can be identified, is the most appropriate way to treat.”
If the cause can’t be determined or if exposure is unavoidable, “then nonsedating antihistamines and new medications called biologics, including omalizumab, can help,” she says.
Even if they’re not chronic, hives that continue to worsen need medical attention, so get yourself to a doctor. A medical professional can prescribe oral steroids and/or an EpiPen to resolve your reaction, says Dr. Waples.
If your lips or tongue begin to swell or if you have difficulty breathing, seek emergency care immediately.
Next, these are the skin problems that could be a sign of disease.