Get Hives for No Reason? What to Know About Idiopathic Urticaria
Updated: Jul. 15, 2021
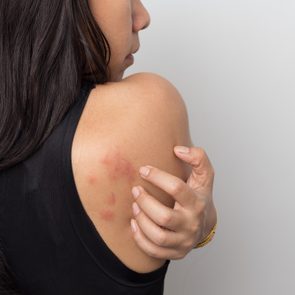
Most cases of hives, or urticaria, have no known cause. However, if they persist for weeks it could be chronic idiopathic urticaria.
Why do you break out in hives?
Up to 20 percent of people experience hives, also known as urticaria, at some point in their lives.
There is an endless list of causes, from ultraviolet rays to seafood to intestinal parasites and even cold temperatures can cause hives.
When you know the cause, it can be helpful; you might be able to avoid the trigger and avoid future outbreaks, even if means giving up strawberries or (worse) chocolate.
The unfortunate truth is that most urticaria cases are “idiopathic,” meaning they have no known cause, says John E. Wolf Jr., MD, a spokesperson for the American Academy of Dermatology.
That means you can’t take steps to avoid them, but take heart. You don’t necessarily need to know the cause to treat the hives.
What is urticaria?
While the official medical term is urticaria, people often refer to having hives, wheals, welts, or lesions.
“I like to think of it as a rash or a skin rupture that comes on suddenly and is very itchy,” says Dr. Wolf, who is also chairman of the Department of Dermatology at Baylor College of Medicine in Houston.
“It’s considered a reaction,” he says. “Maybe an allergic one or maybe not necessarily truly allergic.”
Symptoms of urticaria
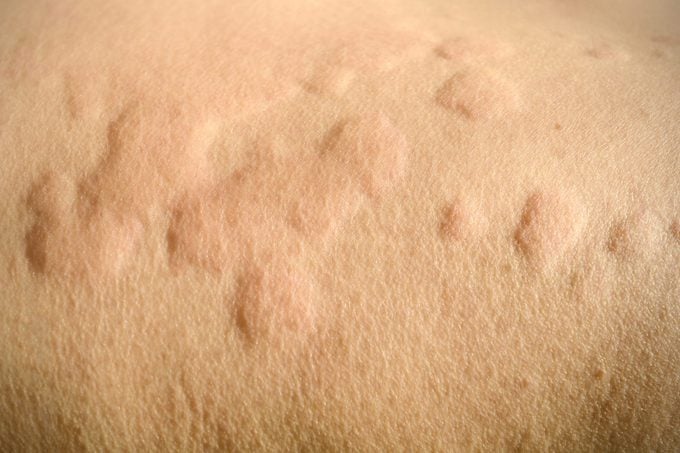
Typically, the hives or welts appear as raised bumps or areas on the skin. They often have a white center and a red circle on the periphery, although if you have dark skin, the hives may be the same color as surrounding skin. The raised areas can be small or large and the surface is smooth.
“Fluid under the skin has pushed the skin up so there’s no real change in the texture of the skin,” says Dr. Wolf.
They can also change shape and move around your body.
“Oftentimes patients will say they feel like it’s traveling to different spots,” notes Heather Holahan, MD, an assistant professor of dermatology at the University of North Carolina School of Medicine in Chapel Hill.
At the very least, the hives are uncomfortable. “They can keep you awake at night and scratching during the daytime, and it’s stressful,” says Dr. Wolf.
Acute versus chronic urticaria
While hives may appear suddenly and seemingly out of nowhere, they may not go away quickly.
If you have hives for six weeks or more, it’s considered chronic. Anything less than that is acute, and many of those cases will disappear totally in as little as a day or a few days.
About 70 percent of urticaria cases are acute, and only one-third are chronic. Even the chronic cases will eventually go away, but it could take years.
For some people, hives are there day and night without stopping. For other people, the hives go away for a week or two then come back.
“It will vary from patient to patient,” says Dr. Wolf. “But two to five years, even if it comes and goes, is a long time.”
The biology of urticaria
Regardless of the cause, the basic biological process in your body leading to hives is the same.
A trigger (known or unknown) spurs the release of immune-system compounds called histamines, which then attach to certain receptors on the surface of blood vessels, prompting them to leak fluid.
“The fluid will accumulate in the skin, push up, and cause the formation of a wheal,” explains Dr. Wolf.
In effect, hives are an autoimmune reaction (when your immune system mistakenly attacks your own body), and many people with urticaria also have other immune problems.
(Here’s why you have hives on your face.)
Causes of non-idiopathic urticaria
Before determining that a case of urticaria is idiopathic, doctors will thumb through all the known causes.
Allergies to foods like peanuts, eggs, berries, and shellfish, among others, are a frequent trigger. So are latex, pollen, and pet dander allergies, as well as infections, temperature changes, and even exercise.
Sometimes the cause is as simple as a medication you’re taking. It could be aspirin, ibuprofen, penicillin, or another antibiotic, or even a contrast dye used for imaging tests.
Although stressors may not actually cause hives, they can certainly make them worse, says Dr. Wolf.
Diagnosing idiopathic urticaria
Doctors will dig deeply trying to diagnose unexplained cases of urticaria, even though the investigation more than likely will not reveal anything.
“We take a careful history, looking at what people are eating or consuming. Did it come after taking a vitamin supplement? People often don’t think about over-the-counter medications,” says Dr. Wolf. “Did it happen after eating shrimp or something more unusual like kelp, which contains iodine?”
A specialist (usually an allergist or dermatologist) will then do skin, blood, or urine tests to hunt for causes.
“I order very basic labs,” says Dr. Holahan. “A lot of the time, it’s just to see if you have another condition, like thyroid disease or anemia.”
Lupus and liver disease can also cause hives.
Ultimately a diagnosis of chronic idiopathic urticaria is a diagnosis of exclusion, meaning you simply rule out other things that may be causing it. A biopsy can help in this process, even if it doesn’t point to a precise cause.
“You’re hoping you’re going to hit a cause but, in most cases, you’ve [just] ruled everything out,” says Dr. Wolf.

Treating urticaria
“Most cases of urticaria, both acute and chronic, are idiopathic, so frequently we treat it without knowing the cause,” says Dr. Wolf.
To get rid of hives, your doctor will typically start you on antihistamines, which work by blocking the histamines that are responsible for the symptoms.
There are two main types of antihistamines, and doctors typically start with H1 antihistamines, which block H1 receptors.
These include Benadryl, Zyrtec, and Allegra. Heartburn medications like Pepcid, Tagamet, and Zantac also block H1 receptors.
If these don’t work, clinicians may move on to H2 antihistamines, perhaps adding them to the H1 antihistamines. Drugs in this class include Zantac.
Drowsy and nondrowsy meds
Some drugs (like Benadryl) are more likely to make you drowsy than others (such as Allegra and Claritin). But nothing is completely nonsedating, says Dr. Wolf.
So if you’re taking an antihistamine, be careful when you drive or operate heavy machinery.
“For chronic urticaria, the patient may be taking the drug for years,” says Dr. Wolf. “That’s a big deal, so you want to go, if possible, to nonsedating antihistamines.”
(Learn whether allergies can make you tired.)
Additional medications for treating hives
While most cases of chronic idiopathic urticaria can be controlled with antihistamines, a few require other drugs, such as corticosteroids or the asthma medication Xolair.
Epinephrine is brought in to treat rare emergency reactions, often in the form of an EpiPen.
Lifestyle measures
People who have discomfort even with medication can try cool compresses or tepid baths with oatmeal for hives relief. Hot showers or baths aren’t recommended. In fact, heat should be avoided in general.
“If you’re having an outbreak, try not to get overheated,” says Dr. Wolf. “If the temperature is high, stay inside in air conditioning and don’t exercise heavily.”
Some people have luck with anti-itch creams or lotions like calamine lotion, but you should avoid topical antihistamines. “People frequently become allergic to them, and then they can’t use the pills,” says Dr. Wolf.
(Here’s what itchy skin can reveal about your health.)
When to call a doctor
Urticaria has been associated with rare but severe anaphylactic reactions. This is when an allergic reaction sends you into shock, constricts your airways, and prevents you from breathing.
“If you have swelling of your lips or tongue or mucus membranes, go immediately to an emergency room,” says Dr. Wolf.
Anaphylactic reactions are treated with epinephrine, also known as adrenaline. (An EpiPen is an autoinjector that delivers epinephrine in an emergency.) This stops the overblown immune reaction and can save your life.
Next, read about one woman’s experience with adult-onset asthma allergies.