Can Stress Cause Hives? 8 Things to Know About Stress Hives
Updated: Jul. 06, 2021
Yes, there's such a thing as a stress rash or hives. Find out more about stress hives and what to do if you have them.
Stress and hives
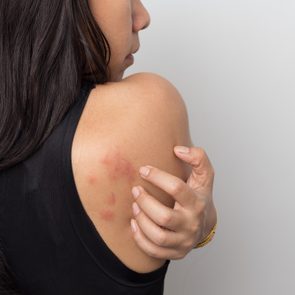
Pounding heartbeat, shortness of breath, headaches, stomachaches—stress can certainly take a toll on the body. Here’s another symptom to add to that list: hives.
That’s right: these raised welts can appear on the skin’s surface when we’re stressed out.
“Hives are an immunologically mediated skin reaction that can occur from different stimuli, such as medications, chemicals, foods, viral infections, temperature extremes, and stress,” explains Jeffrey Fromowitz, MD, a board-certified dermatologist in Boca Raton, Florida.
For some people, that stress manifests on the skin in the form of acne, dryness, rashes—and, yes, hives.
If you think stress is all in your head, think again.
A 2014 study published in Inflammation & Allergy Drug Targets found a tangible brain-skin connection, with physiological stress linked to multiple skin diseases.
So let’s take a look at the link between hives and stress, including what causes hives, how to treat them, and how to (hopefully) prevent them from striking again.
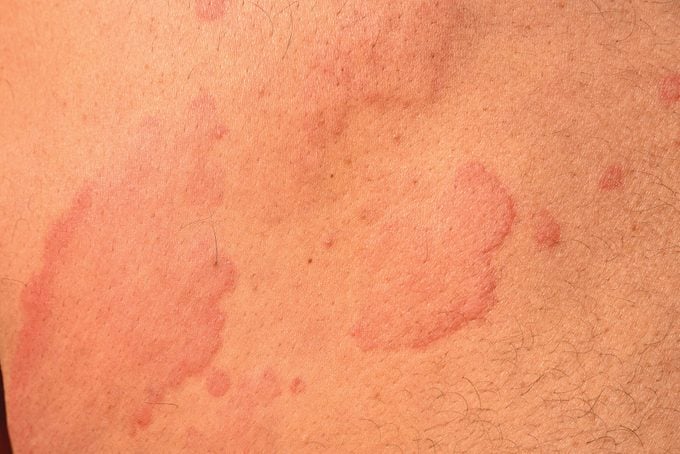
What causes hives?
Hives are an immune system-related skin reaction. You come into contact with something and however benign it may be, your body thinks it’s a foreign invader. The immune system sets off a reaction. The result: hives.
There are a lot of potential triggers: food, medication, exercise, temperature changes, an insect bite or sting, or even a viral, bacterial, or parasitic infection.
“Hives are very common, and there are numerous potential causes,” says Dr. Maguiness. “In many people, in particular children, hives might arise in the skin after an infection of some kind, typically a viral infection. However, we are not always able to identify the exact cause or trigger.”
Pinpointing the cause of hives it harder when hives are long lasting. “Many cases of chronic hives end up being idiopathic, meaning there is no identifiable cause,” says Dr. Fromowitz.
There are different types of hives. They can be caused by an allergic reaction, spontaneous (without explanation), autoimmune (where your immune system mistakes your own tissue as an invader), physical (caused by cold, pressure, exercise, sunlight, or physical activity), or even a light touch on the skin, known as skin writing or dermatographic urticaria.
Autoimmune hives
Autoimmune-induced hives are often chronic, explains Joseph Del Priore, DO, board-certified dermatologist at Huntington Hospital in Pasadena, California.
“Autoimmune conditions such as systemic lupus, rheumatoid arthritis, Sjogren’s [syndrome], and autoimmune thyroid disease can present with hives that continue to recur usually longer than six weeks,” says Dr. Del Priore. “They usually have an autoimmune component that activates the specialized cells in your skin, causing the release of the hive-causing mediators.”
The link between hives and stress
Officially known as urticaria, hives are itchy, red, swollen areas of skin that are caused by histamine release, explains pediatric dermatologist Sheilagh Maguiness, MD, an associate professor in the Department of Dermatology at the University of Minnesota Medical School and cofounder of Stryke Club skin care line for boys.
While a variety of things can cause hives, anecdotally, many people report a link between those distinctive red welts and stress.
It makes sense, says Dr. Maguiness, because stress has tangible effects on your body and often manifests physically.
“Stress can definitely play a role in any skin disease, including hives,” she says. “Stress truly never makes anything better and can lead to worsening the hives in some cases.”
The connection goes beyond anecdotes. A 2018 study found a link between stress and hives, noting that women with chronic hives demonstrated significantly higher stress levels.
(Learn the different types of stress—and how to ease them.)
Hives and stress: correlation or causation?
Though science has suggested a link between hives and stress, it’s less clear whether stress causes hives.
It comes down to the tricky difference between correlation and causation. Correlation is a relationship, but it’s not necessarily cause and effect, like causation is.
For instance, you might say there’s a correlation between exercising in older age and longevity. But does it mean that exercising causes older adults to live longer? Not necessarily. There’s a good chance that sick or less-healthy older adults (who are more likely to die) are less able to exercise than their healthier peers.
The same reasoning applies to stress and hives. Until research proves otherwise, we can’t say that our bodies’ stress response directly leads to hives.
“Although stress can make all skin problems worse, it is not known to be a direct cause of hives,” says Dr. Del Priore.
(These are the weird symptoms linked to stress.)
How long do hives last?
Hives can be annoying and even painful, but thankfully, they don’t always last long. Often an outbreak of hives will dissipate within hours.
“Each individual hive lesion should only last a few hours, such that if you drew a ring around it, the hive would have moved, changed shape, or resolved in the span of 24 hours,” says Dr. Maguiness.
But just because the hives fade quickly doesn’t mean you’re out of the woods.
“You can keep getting new crops of hives for several days to weeks,” she says.
Hives generally fall into one of two categories: acute or chronic.
Acute hives typically last 24 hours or less in one location, says Dr. Fromowitz.
“A hive that persists in the same spot for longer than 24 hours may indicate something else is going on,” he says, “for example, a condition called urticarial vasculitis which, while immunologically mediated like hives, represents inflammation in the blood vessel walls.”
An acute hives outbreak won’t last longer than six weeks, max.
“If the recurring hives last more than six weeks, then we classify it as chronic urticaria,” says Dr. Del Priore. “This requires a further investigation into the cause, with a thorough look into the patient’s history and a physical exam.”
Usually, a doctor will order blood work to look into autoimmune causes and a food or medication allergy workup to determine if those may have triggered your chronic hives.
(Here’s everything you need to know about dermatographic urticaria.)

How to manage stress to avoid hives
If feeling stressed out wreaks havoc on your body, it stands to reason that keeping stress in check will automatically prevent hives, right? Not necessarily.
Sometimes hives worsen stress.
“For some individuals, stress may exacerbate hives,” Dr. Fromowitz says. “For example, being itchy and having a rash may further exacerbate the stress one is feeling and perpetuate scratching, and more hives will form.”
However, because hives happen for a variety of reasons and can be triggered by causes like sunlight, friction, cold, or autoimmune disorders, it’s possible to feel relaxed, calm, and stress free yet still experience an outbreak.
Still, stress reduction is always a good idea. It benefits both your mind and body.
“Stress is detrimental on your skin, and it is well known that skin problems improve with stress reduction,” says Dr. Del Priore.
“I recommend stress-reducing activities, like increasing exercise, giving yourself time to think alone, meditating quietly, and reducing phone or work-related activities when outside the office,” he adds.
It’s not guaranteed that keeping stress in check will prevent hives, but it doesn’t hurt (and only can help your quality of life) to try.
How to tell when a reaction is serious
While hives are annoying and unsightly, they’re not necessarily dangerous … unless they exhibit a few telltale symptoms.
“If you experience a few red, itchy hives on the skin, it is usually not serious,” says Dr. Maguiness. “However, if you start to notice lip or facial swelling; an itchy, swollen throat; and/or difficulty breathing, this could indicate a more concerning anaphylactic reaction and is a true emergency.”
Any facial swelling stemming from hives could obstruct breathing and be potentially life-threatening, says Peterson Pierre, MD, a board-certified dermatologist in Westlake Village, California, and owner of Pierre Skin Care Institute.
“If you experience such symptoms, you should go to the emergency room immediately,” he advises.
Treatment options for hives
So the dreaded has happened and you’ve had a hives outbreak. Are you doomed to 24 hours (or longer) of itchy, painful welts? Absolutely not, say doctors.
“There are very effective treatments for hives,” says Dr. Maguiness.
Antihistamines are the first line of treatment
“Regular use of nonsedating antihistamines—fexofenadine, cetirizine—will usually do the trick,” she says. “Additional antihistamines, like diphenhydramine [Benadryl], are sedating and can be used at night in addition to the nonsedating antihistamines, depending on the severity of the hives.”
Dr. Del Priore notes that immunosuppressants are also used, but he cautions that they have a higher potential for more serious side effects.
He recommends other, promising medical alternatives.
“Newer biologic injectable medications, like Xolair, have been helpful as well in improving idiopathic chronic urticaria,” he says.
Can you prevent hives?
If you want to prevent hives from cropping up again, you need to know why you got them in the first place.
“The first thing to do is to try to determine the cause of the hives so that it can be avoided,” says Dr. Fromowitz.
Always get hives after sun exposure? Do your best to cover up and stay cool in the shade.
Notice an outbreak of hives after a particularly grueling workout? Consider taking it easier, or see if your workout clothes are causing friction.
If you determine a certain food, medication, or allergen causes hives, find ways to avoid the trigger.
“Next, avoid scratching,” says Dr. Fromowitz. “Try applying a cool compress, as this will decrease the itch sensation and help the hive resolve. Also, start by taking an over-the-counter antihistamine such as Allegra, Zyrtec, or Benadryl.”
Although you may be tempted to take an a nonsteroidal anti-inflammatory drug (NSAID) such as ibuprofen or aspirin to help relieve discomfort, Dr. Fromowitz recommends steering clear since they may worsen hives.
Another tip: stay away from harsh, tight-fitting fabrics and hot water, which can aggravate hives.
You’ve probably noticed that stress reduction isn’t on the experts’ list of ways to prevent hives. “Managing stress can certainly be helpful but will probably be insufficient to make your hives go away,” he says.
That said, lowering stress is good for your all-around health. So go ahead and do those stress-reduction techniques. Just be sure to follow your doctor’s other treatment instructions too.
Next, here’s how to save your own life in a medical emergency.