Can Stress Cause High Blood Pressure? What Heart Doctors Need You to Know
Updated: Oct. 10, 2022
High levels of stress can lead to an increase in heart rate and blood pressure. Here's how to reduce stress to protect your heart health.
Can stress cause high blood pressure?
Stress—and often how you cope with it—can make so many things worse, including your blood pressure.
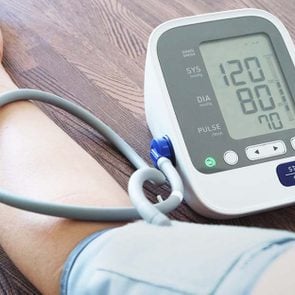
A major risk factor for heart disease and stroke, high blood pressure stage 1 is defined as an upper or systolic blood pressure reading of 130-139 systolic millimeters of mercury (mm/ Hg) and a lower or diastolic pressure reading of 80-89 mm Hg. Systolic blood pressure is the pressure when your heart beats while pumping blood, and diastolic blood pressure is the pressure when your heart is at rest between beats. A blood pressure of less than 120/80 mm Hg is considered normal.
Stage 2 is when blood pressure consistently ranges at 140/90 mm Hg or higher. This is when doctors are likely to suggest medication and lifestyle changes, according to the American Heart Association.
Untreated, high blood pressure can set the stage for heart attack, stroke, and other complications by damaging blood vessels throughout your body. Stress can have both direct and indirect effects on blood pressure levels, explains Vijay Nambi, MD, associate professor of medicine, Baylor College of Medicine, Houston.
Here’s what you need to know about stress and how it affects your heart rate and blood pressure.
Types of stress and your high blood pressure
Stress triggers your body’s fight-or-flight response, and this is a good thing when you are faced with an immediate threat or scare, says Dr. Nambi.
“If something scares me and jumps in front of me, my blood pressure should go up,” he says. In these cases, stress stimulates your sympathetic nervous system which releases the stress hormones adrenaline and cortisol that can increase heart rate and blood pressure.
This is exactly what is supposed to happen to help you avoid harm, he notes.
Chronic stress
Chronic stress—whether related to work, finances, personal relationships, or life in general—is another story altogether. Researchers are still trying to unravel how chronic stress directly impacts blood pressure. What they do know is that that stress gets in the way of making healthy choices, which will have indirect effects on your blood pressure.
When you are stressed, you are less likely to do the things that you know are good for you. This includes following a healthy diet and exercising regularly, says Stephen J. Huot, MD, professor of medicine (nephrology), associate dean and director of graduate medical education, Yale School of Medicine/Yale New Haven Hospital.
Effects of chronic stress
“High blood pressure damages the blood vessels every time it happens, and if stress is causing you to eat poorly, gain weight, not exercise, or take medications for your blood pressure, this contributes to poor blood pressure management over time,” says Dr. Huot. (Beware of these weird stress symptoms.)
You may cope with chronic stress by drinking more alcohol, smoking, or using illicit drugs, all of which can negatively affect blood pressure and your health in general, he says.
“If people are under stress, they are at risk of not being able to comply with lifestyle recommendations as well as the medication regimens that they are on,” agrees Salim Virani, MD, PhD, professor, sections of cardiology and cardiovascular research, Baylor College of Medicine, Houston.
“Chronic stress can lead to anxiety and depression and those carry a worse prognosis if you have heart disease,” he says. This is why stress management is an important part of counseling after a heart attack or stroke, he says.
When you are stressed out, you may have trouble falling or staying asleep. Sleep loss—even just one bad night—may cause a spike in blood pressure that night and the following day, according to a 2019 study in Psychosomatic Medicine. And if you already have high blood pressure, poor sleep plus work stress is a recipe for disaster.
This combination can increase your chances of dying from heart disease, a 2019 study of nearly 2,000 people with high blood pressure suggests. People in the study who had just work stress or just sleep loss had a two times higher risk of dying from heart disease than those with no stress or healthy sleep. Participants with both work stress and sleep loss had an even greater risk of cardiovascular death. The findings appear in the European Journal of Preventive Cardiology.
Coping with stress
You are not powerless in the face of stress even though it sometimes feels that way. Reducing stress starts by doing the following, according to our experts:
Identifying what is stressing you out
There are some stressors that you can change and some things you can’t.
“If it is a stressful work situation, is it changeable? If it a stressful life situation, is that changeable? Try to learn more about what the stressor is and what is behind it,” Dr. Huot says.
If you can make changes such as finding a new job, it will likely help reduce your stress load, but sometimes you have to change how you cope with the stress instead because not everything is modifiable.
De-stressing daily
There are many relaxation techniques that can help put the brakes on chronic stress when practiced regularly. Find one that works for you and fits into your lifestyle, Dr. Nambi suggests.
“It could be more time spent with family, meditation, exercise, yoga or deep breathing,” he says. (Here are some recommendations of exercises for high blood pressure.)
“Structured breathing can calm down the nervous system and can be helpful,” Dr. Huot adds. “Exercise, for sure, produces physiologic changes that help us feel better and if we feel better, we cope better.” There are many apps and videos available to teach you relaxation techniques.
Knowing your numbers
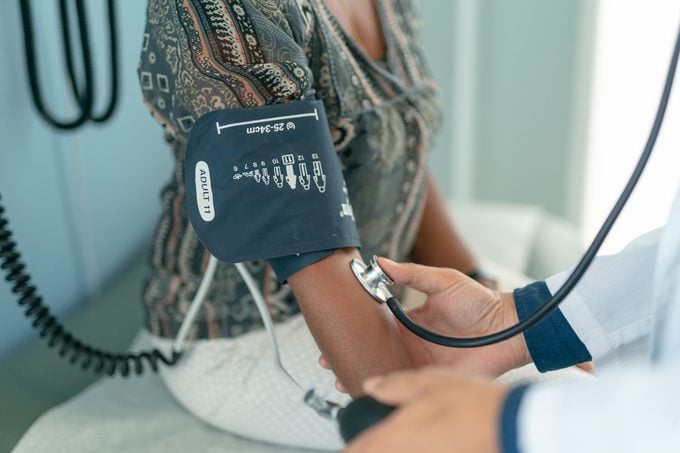
Get your blood pressure measured by your doctor once a year, says Guy L. Mintz, MD, director of cardiovascular health and lipidology, Northwell Health’s Sandra Atlas Bass Heart Hospital, Manhasset, New York.
“Patients with a family history of hypertension should be evaluated more often,” he says. “Patients can evaluate their own blood pressure at home with a good home blood pressure monitor.”
Physicians also have the ability to order a 24-hour blood pressure monitor which measures blood pressure hourly, he says.
Taking good care of your self
Eating a healthy low-salt diet, engaging in regular physical activity, maintaining a normal weight, getting regular high-quality sleep, and taking medication if needed, can all help keep your blood pressure healthy and stave off any long-term complications, Dr. Mintz says.
The last word
Stress is one of many factors that can affect your blood pressure. “It can contribute to it, but it is unlikely to be the only reason,” Dr. Huot says. “You may still need to make lifestyle changes or take medication even if you reduce stress,” he says.
Next, find out thesurprising benefits of stress.