How to Know When High Blood Pressure Is an Emergency
Updated: Oct. 10, 2022
If you have high blood pressure and haven't been great about taking your medication as directed, you may be at risk for sky-high blood pressure and damage to your organs. Here are the symptoms of a high blood pressure emergency and what to do.
A silent killer
High blood pressure produces no signs, and yet it can dramatically increase the risk for heart attack and stroke. No wonder it’s often called the silent killer.
When blood pressure creeps up so high that it causes potentially life-threatening symptoms, it may be a type of high blood pressure crisis known as a hypertensive emergency, says Stephen J. Huot, MD, PhD, professor, associate dean, and director of graduate medical education at Yale School of Medicine/Yale New Haven Hospital.
Not surprisingly, it can warrant a 911 call or a trip to the emergency room.
What is a high blood pressure emergency?
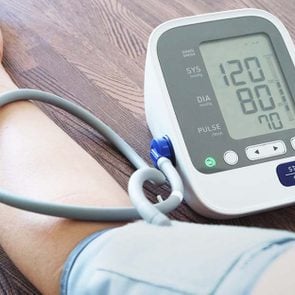
The answer can be found in two numbers. Systolic blood pressure, the upper number in a blood pressure measurement, refers to how much pressure your blood is exerting against your artery walls when the heart beats. Diastolic blood pressure, the lower number, indicates how much pressure your blood is exerting against your artery walls when the heart is resting between beats. A blood pressure of less than 120/80 mm Hg is considered normal.
If your blood pressure is 180/120 millimeters of mercury (mm Hg) or higher and you have chest pain, back pain, numbness or weakness, or a change in vision, you may be experiencing a hypertensive emergency. (Find out what high blood pressure can feel like and get ahead of your numbers.)
These symptoms suggest you may be experiencing what’s called end-organ damage, Dr. Huot says. “Untreated high blood pressure negatively impacts blood vessels in critical areas of the body such as the brain, heart, kidneys, and the aorta, which is the main blood vessel that carries blood away from your heart to the rest of your body.”
End-organ damage takes many forms including stroke, heart attack, and kidney failure. It’s not just the blood pressure numbers that indicate the emergency and risk, it’s the symptoms of end-organ damage, he says.
Other signs of end-organ damage due to a high blood pressure emergency can be:
- Passing out
- Memory loss
- Damage to the eyes
- Rupture of the aorta, the body’s main artery
- Crushing chest pain (angina)
- Fluid build-up in the lungs
- Preeclampsia, a serious pregnancy complication
In these emergency situations you need to get help immediately, Dr. Huot says.
High blood pressure emergencies may also travel with other symptoms that do not indicate end-organ damage—yet. These include:
- Severe headache
- Shortness of breath
- Nosebleeds
- Severe anxiety
Are you at risk for a high blood pressure emergency?
Nearly half of adults in the U.S. have high blood pressure—meaning, greater than 130/80 mm Hg—or are taking medication to control hypertension, placing them at greater risk for a high blood pressure emergency. (Only about one in four adults with high blood pressure have their condition under control.)
Men are at greater risk than women for a high blood pressure emergency. Other risk factors for a hypertensive emergency include advancing age, diabetes, high blood cholesterol levels, and/or chronic kidney disease, according to research presented at the 2020 meeting of the American Heart Association. Medication interactions may also cause a hypertensive emergency, Dr. Huot explains.
In many instances, these emergencies occur when someone stops taking their blood pressure medication. “Most people who experience a hypertensive emergency have known that they have high blood pressure in the past, but they fall off their medication management wagon and their blood pressure progresses,” Dr. Huot says. “It’s not out of the blue.”
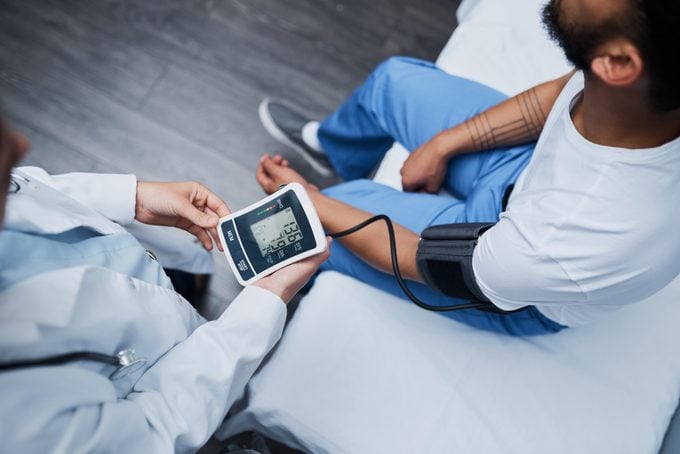
Treating and preventing a high blood pressure emergency
High blood pressure emergencies are treated with intravenous blood pressure-lowering medication and hospitalization, in addition to treating any end-organ damage that has already occurred, says Dr. Huot.
If you experience dangerously high blood pressure along with symptoms that suggest end-organ damage, it is an emergency.
“Start with calling your physician’s office and if you’re unable to reach the doctor, go to the emergency room for immediate evaluation and treatment, ” says Guy L. Mintz, MD, director of cardiovascular health and lipidology at Northwell Health’s Sandra Atlas Bass Heart Hospital in Manhasset, New York. “An ambulance is not required unless the patient feels that they are having a stroke or heart attack, chest pain, or shortness of breath.”
High blood pressure emergencies can be prevented, Dr. Mintz says.
Regular medical check-ups—especially in people with other risk factors—along with home blood pressuring monitoring, at least half an hour of aerobic exercise most days of the week, proper diet with no added salt, and maintaining an ideal weight can all work together to stave off an emergency, he says. (And if you’re feeling under the weather, make sure you know cold medicine and high blood pressure interact.)
What is hypertension urgency?
A hypertensive crisis is divided into two camps: urgent and emergency.
In an urgent hypertensive crisis, your blood pressure is extremely high, but there doesn’t seem to be symptoms suggesting damage to your organs. “The distinction is not the level of blood pressure but whether there is evidence of end-organ damage,” says Dr. Mintz. (This is what it’s like to have a hypertensive crisis.)
With hypertensive urgency, your blood pressure is 180/120 or greater. But there is no evidence of end-organ damage—yet. Consider it a really loud warning call, Dr. Huot says.
The American Heart Association suggests waiting about five minutes and taking blood pressure again if your numbers are 180/120 or greater with no symptoms. If the second reading is just as high, check in with your doctor.
“We want to intervene before it progresses to damaged blood vessels and causes an emergency,” Dr. Huot says. Treatment likely entails getting back on medications or starting new ones, he says. “We also do closer follow-up, as opposed to routine follow-up, which we would do if blood pressure is just a little elevated,” he says. There is usually no need for hospitalization with an urgent hypertensive crisis. (Here’s what to do if you have a high blood pressure headache.)
Unlike an emergency high blood pressure crisis, those that are considered urgent may travel with other symptoms that do not indicate damage to your organs.
The last word
High blood pressure is a major risk factor for heart attack and stroke. Lifestyle changes such as eating a low-salt diet, maintaining a healthy weight, and getting regular physical activity are often recommended first.
Medication is also available to get your numbers where they need to be. Make sure you know your blood pressure levels and are doing everything that you can to keep them in the safe zone. Even slightly high blood pressure can be dangerous.
Next, these are the 31 things you should do right now to avoid high blood pressure.