High Blood Pressure Headaches: What They Are and How to Treat Them
Updated: Oct. 10, 2022
When blood pressure rises to dangerous levels, headaches can occur, and this may be a sign of a medical emergency. Here are the causes, what they feel like, and what to do about high blood pressure headaches.
Understanding high blood pressure headaches
If you are one of the millions of people who live with high blood pressure, you were probably surprised when your doctor told you that your numbers were higher than they should be—especially because you feel fine.
High blood pressure doesn’t typically cause symptoms. However, some people may have headaches—especially if their blood pressure skyrockets into the danger zone—a condition known as high blood pressure emergency or urgency.
Here’s what you need to know about a high blood pressure headache, what other symptoms may occur, and when to call 911.
Blood pressure: How high is too high?
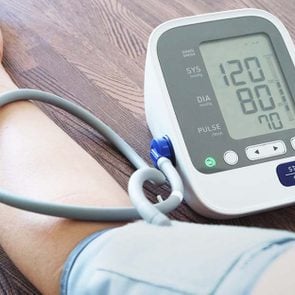
Systolic blood pressure is the upper number in a blood pressure measurement. It refers to how much pressure your blood is exerting against your artery walls when your heart beats. The lower number, diastolic pressure, refers to how much pressure your blood is exerting against your artery walls when your heart is resting between beats. A blood pressure of less than 120/80 mm Hg is considered normal.
Nearly half of adults in the U.S. have high blood pressure—meaning greater than 130/80 mm Hg—according to the American Heart Association (AHA). When untreated, high blood pressure increases the risk for heart attack, stroke, and other complications by damaging blood vessels throughout your body.
“In most cases, high blood pressure does not cause headaches, nosebleeds, or any other symptoms,” stresses Salim Virani, MD, professor, sections of cardiology and cardiovascular research, Baylor College of Medicine, Houston.
“If you are waiting for symptoms to tell you that you have high blood pressure, you have missed the boat,” he says. “Waiting for symptoms is actually a very big mistake. We need to pick up high blood pressure in the absence of symptoms.” This gives doctors the best opportunity to treat high blood pressure and avoid complications.
If you have high blood pressure, you have to take your medicine every day, even if you feel fine. Don’t wait for symptoms to take your medication, says Dr. Virani. (These are the 31 things you should do right now to avoid high blood pressure.)

High blood pressure crisis and headaches
If your blood pressure is 180/120 mm Hg or higher and you have chest pain, back pain, or vision changes, you may be having a hypertensive emergency.
These are signs of end-organ damage and you should call 911 or get to the emergency room, the AHA warns.
A high blood pressure crisis may cause other symptoms too, including:
“A hypertensive headache is acute in onset, occurs on both sides of the head, tends to pulsate and resolves once blood pressure is normalized,” says Brian M. Grosberg, MD, director of the Hartford Healthcare Headache Center, Ayer Neuroscience Institute, and professor of neurology at the University of Connecticut School of Medicine.
These headaches are typically treated with blood pressure-lowering medication either in the hospital given intravenously or taken at home, depending on whether there is evidence of end-organ damage. (Find out what it’s like to have a hypertensive crisis from someone who survived one.)
High blood pressure and recurring headaches
If you have recurring headaches, schedule an appointment with your doctor or a headache specialist to determine what’s causing them and whether they are related to your blood pressure. High blood pressure is usually not the cause of a recurring headache, Dr. Grosberg says. (Here are surprising headache causes you didn’t know about.)
High blood pressure and migraines
There may be a link between high blood pressure and migraine headache. “This is likely complex and multifactorial,” says Dr. Grosberg. “With migraine, we do know that stiffening and other changes that occur in blood vessels in the brain can contribute to high blood pressure too, but this link needs further exploration.”
You can have migraine headache and high blood pressure at the same time and this doesn’t mean they are directly related, he explains. “The two conditions can coexist.”
If your high blood pressure is not well controlled, you should not take migraine drugs known as triptans, Dr. Grosberg warns. “These have effects on the blood vessels so one wouldn’t want to use these medications in people with poorly controlled blood pressure.”
Other over-the-counter or prescription medications may also increase blood pressure, he says. This list includes non-steroidal anti-inflammatory medications (NSAIDs), which cause your body to retain fluid, decreasing kidney function, and raising blood pressure. Pain relievers that contain caffeine—a stimulant—may also raise blood pressure levels, he says.
Blood pressure meds and headaches
It’s possible that your blood pressure medications may play a role in causing headaches, says Dr. Grosberg. Headache is a common side effect of some antihypertensive drugs such as angiotensin-
Some blood pressure medications such as beta-blockers and calcium channel blockers may reduce headache frequency, independent of their effects on lowering blood pressure. “These are sometimes used for headache prevention,” he says.
He adds: “We don’t use these medications for headaches with the thought that they will get blood pressure under control. The idea is, ‘Let’s use them for headaches and it may have an added benefit on blood pressure.'”
Preeclampsia and headaches
Headaches may be a sign of preeclampsia, or high blood pressure during pregnancy, and this should also be evaluated, according to Dr. Grosberg.
How to manage headaches and high blood pressure
If you have a migraine or another type of chronic headache and high blood pressure, a non-drug approach may be worth a try, says Dr. Grosberg. These may include biofeedback, eating a low-salt diet, and/or weight loss, he suggests.
Biofeedback involves placing sensors on the body to measure head pain to help you learn how to control it. It may provide as much relief as some prescription headache medications, according to the American Migraine Foundation.
The last word
If you have headaches and high blood pressure, see a doctor to help learn the exact cause. Taking steps to lower blood pressure such as eating a low-salt diet, exercising regularly, maintaining a normal weight, and/or taking medication can all help keep blood pressure in the healthy range. Your doctor will also be able to give you advice on the best way to treat your headaches if you also have high blood pressure.
If your blood pressure is 180/120 mm Hg or higher and you have headaches, wait five minutes and retest. If your reading remains that high, call your doctor. If you also have chest pain, numbness, or other symptoms, call 911.
Next, here are the best heart-healthy products to buy.