Does Sunlight Give You Hives? 5 Things to Know About Solar Urticaria
Updated: Mar. 08, 2022
Turns out you can be allergic to sunlight. Known as solar urticaria, these are the causes, symptoms, and treatments of hives from the sun.
Solar urticaria: when the sun causes hives
The sun gives life and light, but we’ve also listened for years to warnings about the dangers of ultraviolet (UV) light.
Most of us know about the raised risk of skin cancer from exposure to UV rays, but there’s another, less-common, side effect of sun exposure: solar urticaria, or hives caused by the sun.
“Solar urticaria is a very rare form of hives, which happens when you get exposed to natural or artificial ultraviolet rays,” explains Anthony Rossi, MD, an assistant attending physician at Memorial Sloan Kettering Cancer Center in New York City.
Although hives are common, the itchy red welts of solar urticaria are not. Here’s everything you need to know about solar urticaria causes, what it is, how to treat it, and how to prevent it from flaring up.
What exactly is solar urticaria?
Think of solar urticaria as an allergy to ultraviolet rays.
The condition, which erupts whenever there’s skin exposure to certain wavelengths of UV rays, can be “incredibly life altering,” says Alison Ehrlich, MD, a dermatologist in private practice in Washington, D.C.
“Imagine being super itchy every time you go out in the sun. It has a huge impact on quality of life,” she says.
Fortunately, solar urticaria is rare, representing less than 1 percent of all people who develop hives. The condition typically develops in your 30s, but it can show up any time, from infancy to old age, and affects females more than males.
About 15 percent of cases resolve on their own after five years, and 25 percent resolve after 10 years.
(Stress is another surprising cause of hives. Here’s why it happens.)
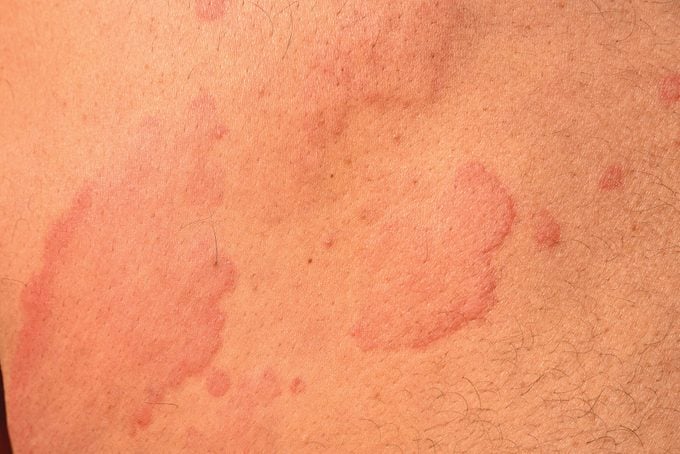
Symptoms appear with sun or artificial light exposure
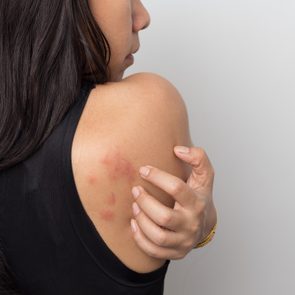
Hives on areas of your skin that have been exposed to UV rays are the main symptom of solar urticaria.
Your face and the tops of your hands may be spared simply because they’re already “hardened,” or used to the sun.
“You get these raised, pink welts that can look circular and can feel like they’re moving around your body,” says Heather Holahan, MD, assistant professor of dermatology at the University of North Carolina School of Medicine in Chapel Hill.
The hives can itch, burn, and sting and appear very quickly—about 10 to 15 minutes after the exposure. Symptoms usually disappear in one to two hours, but they can last as long as 24 hours. Happily, they leave no permanent marks or scars.
Contrast this with sunburns or hives related to a sunscreen allergy, which show up hours later and can take longer to resolve. (Here’s how to tell the difference between hives and rash.)
Although solar urticaria symptoms are usually mild, they can become extreme.
“There can be severe reactions, like fainting, bronchospasm [where your airways react and close], and even anaphylaxis,” says Dr. Rossi.
Anaphylactic shock, which can be life threatening, is uncommon with solar urticaria.
Is solar urticaria an allergic reaction?
Solar urticaria is triggered when your skin comes into contact with UV light, usually UVA light and visible light.
“We don’t know exactly why it happens, but it could be that a protein in our skin changes when the sun hits it, and our body thinks it’s an allergen,” says Dr. Holahan.
After that, your body spirals into the familiar cascade common to most allergies: mast cells from your body’s immune system release chemicals called histamines, which cause the itchy, red welts.
As many as 16 percent of people with solar urticaria also have other forms of chronic urticaria, says Dr. Ehrlich.

How do you treat and prevent solar urticaria?
As with any allergic reaction, monitoring symptoms is essential. Here’s what to do to prevent and treat these hives.
Prevention
With any type of hives, avoiding the trigger will prevent outbreaks. While it’s not possible to avoid sunlight entirely—nor do you want to, as it’s an important source of vitamin D—there are things you can do.
Wear sun-protective clothing, including wide-brimmed sun hats and gloves, when you drive (UV light can travel through window glass.)
Opt for closed-shoes over sandals, and avoid direct sunlight between 10 a.m. and 3 p.m. You can also apply protective film over your windows.
Wear sunscreen, something everyone should do, regardless of whether they have an allergy. But don’t choose just any sunscreen. “Look for sunscreen with zinc or titanium dioxide,” says Dr. Holahan.
Treatment
Some people benefit from a procedure called phototherapy, also known as UV hardening. Exposure to incrementally higher levels of UV rays trains your skin so eventually it won’t react to the allergen.
“You induce tolerance,” explains Dr. Rossi. “The immune system gets gradually more tolerant to UV exposure.”
The process is cumbersome, though, and requires visits to the doctor’s office two to four times a week, says Dr. Holahan.
Some solar urticaria cases are trigger by a drug—oral contraceptives, for instance, or the heart medication atorvastatin. Stopping the medication will often resolve the hives, says Dr. Ehrlich.
Drugs can also help treat hives. These include antihistamines like Allegra or Zyrtec and the anti-inflammatory asthma drug Xolair.
Less commonly, doctors will prescribe steroids or an antimalarial like hydroxychloroquine. While Hydroxychloroquine doesn’t treat or prevent Covid-19, it is used for many different skin conditions, says Dr. Holahan.
Next, check out what happens to your body in extreme temperatures.