Allergy advice you can ignore
Home remedies and tips for dealing with allergy symptoms are one thing, but don’t fall for these allergy myths and all-around poor advice that experts loathe.

“It’s fine, my dog is hypoallergenic”
“Unfortunately, there is no such thing as a truly hypoallergenic dog or cat. It’s not the fur people are allergic to but the allergens that are released in saliva, sebaceous glands, and perianal glands. It is true, however, that some breeds are more bothersome for allergy sufferers than others.” —Bryan Martin, MD, president of the American College of Allergy, Asthma and Immunology. Besides hypoallergenic pets, these are the 20 things you never knew you could be allergic to.

“I can’t get vaccines, I’m allergic to eggs”
“Egg embryos are used to grow viruses for vaccines such as the flu so you may have heard that you shouldn’t get vaccinated if you’re allergic to eggs. But there is now a vaccine approved for adults that is completely safe for people with egg allergies. It’s important to get vaccinated as it can help prevent serious illness.” —Bryan Martin, MD

“Pass on the bread basket, I have a gluten allergy”
“You can have a gluten intolerance, but it’s extremely rare to have a true gluten allergy. Many people self-label as having gluten allergy and avoid gluten without any medical indication this is true or necessary.” —Bryan Martin, MD

“Seasonal allergies are just seasonal—so this has to stop soon, right?”
“While some allergies are seasonal, it really depends on what a person is allergic to. Pollen allergies are seasonal—for example, tree pollen allergies peak in early spring, grass pollen soars in late spring, and ragweed pollen is highest in summertime. Unfortunately, many people have the pollen allergy “triple threat” and have reactions to all three pollen types. Some types of allergies go year-round. I always recommend that my patients try to identify the times of the year their symptoms tend to occur, so they can take measures to decrease or even prevent those annoying allergy symptoms.” —Rob Danoff, DO, family physician and program director of the Family Medicine/Emergency Medicine Residency Programs at Aria Health. These are the 9 things allergists do to control their own allergies.

“Allergy pills work best”
“Depending on the type of allergies and symptoms experienced, allergy products applied directly inside the nose may have better results than oral medications. Nasal steroids, for example, are often the most effective maintenance treatment for patients with allergic rhinitis and are particularly helpful when patients have nasal congestion. However, you must use nasal steroids properly to get the best effect.” —Skye McKennon, PharmD, clinical assistant professor at the University of Utah College of Pharmacy. Beware of these signs your allergy medicine isn’t working.

“I swell up like a blimp when I get a mosquito bite, I must be allergic”
“While allergic reactions can occur with stinging insects like yellow jackets, hornets, honey bees, wasps, and fire ants, they do not occur with biting insects such as mosquitoes or chiggers. Mosquito bites cause local swellings (hives) that are itchy but they are not allergic reactions. Use topical calamine or hydrocortisone ointment for itchiness and use mosquito nets and insect repellents to prevent bites.” —Chitra Dinakar, MD, director of FARE Center of Excellence at Children’s Mercy, Kansas City. These are the 13 skin-allergy myths you need to stop believing.

“My nose won’t quit running, my allergies are terrible”
“Many patients may not actually have allergies, as identified on blood or skin tests. Having a deviated septum is very common and patients with a deviated septum may have symptoms similar to allergies, such as nasal congestion, post-nasal drip, or sinus infections.” —Houtan Chaboki, MD, board-certified facial plastic surgeon, George Washington Medical Faculty Associates

“I’m allergic to artificial dyes”
“Controversy exists regarding evidence for artificial coloring and behavioral changes in children, as well as dyes causing chronic urticaria and asthma but there is no scientific evidence to support a link between exposure to artificial coloring and allergies.” —Bryan Martin, MD

“Dairy makes me all congested, I must be allergic”
“Many people will stop eating dairy foods, especially milk, thinking it is responsible for their nasal or sinus congestion and will assume they’re allergic to dairy. While it’s true that some people do have a real milk allergy, it is rare and must be confirmed by a test. It’s more common to see patients allergic to soy milk, which they use as a replacement for dairy.” —Murray Grossan, MD, author of The Whole Body Approach to Allergy and Sinus Relief.
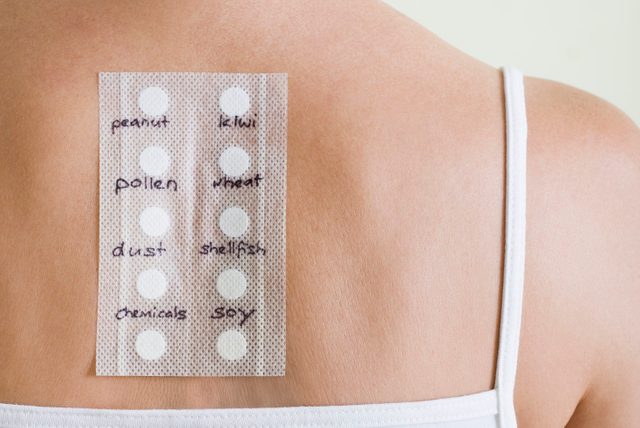
“I know all my allergies, I did one of those at-home kits”
“At-home blood allergy tests might be able to reveal sensitization, but being sensitized to a certain allergen, like milk, doesn’t mean you’re actually allergic to it. These sort of at-home screening tests are not reliable and can often lead to misinterpretation, diagnostic confusion, and unnecessary dietary elimination.” —Bryan Martin, MD

“Children shouldn’t have foods like peanut butter before age one”
“Many people believe that highly allergenic foods shouldn’t be given to babies but for most children, there is no evidence to support avoidance once they are past four to six months of age. New evidence emerging on peanut allergy shows that early introduction of highly allergenic foods may actually promote tolerance and reduce the likelihood of an allergy.” —Bryan Martin, MD. (You might also be interested in learning these myths about food allergies.)

“Allergies aren’t my real problem”
“There’s a common notion that allergic reactions only cause symptoms like itching, wheezing, sneezing, swelling, or diarrhea and that they can be measured with a simple blood test or scratch test. I explain to my patients that there are at least four different types of allergies and three of them don’t show up on standard allergy tests. Allergies can cause a very wide range of chronic symptoms, especially if the symptoms fluctuate in response to environmental changes or eating.” —Leo Galland, MD, author of The Allergy Solution. These are the 11 common triggers of spring allergies.

“Allergies aren’t a real illness”
“Eczema or seasonal allergies can be very mild but they can also be symptoms of a genetic allergic condition that, with asthma, is called atopy. When you have eczema, allergies, and asthma together, this can lead to heightened immune responses to common allergens like pollen and food. This needs to be treated and managed or it can cause serious problems.” —Murray Grossan, MD

“Allergies are purely physical”
“Allergies are very real and in some cases, potentially life-threatening. They are rooted in heredity and the environment. But the mind does play a role: Mental stress can precipitate or enhance allergic reactions and relaxation techniques can moderate them. A person who is strongly allergic to roses, for example, may react to the sight of a plastic rose, demonstrating the involvement of the mind and the brain, but this relationship is not well understood.” —Morton Tavel, MD, clinical professor emeritus of medicine, Indiana University School of Medicine, and author of Health Tips, Myths and Tricks: A Physician’s Advice. Here’s how to know if your symptoms are allergies or another medical condition.
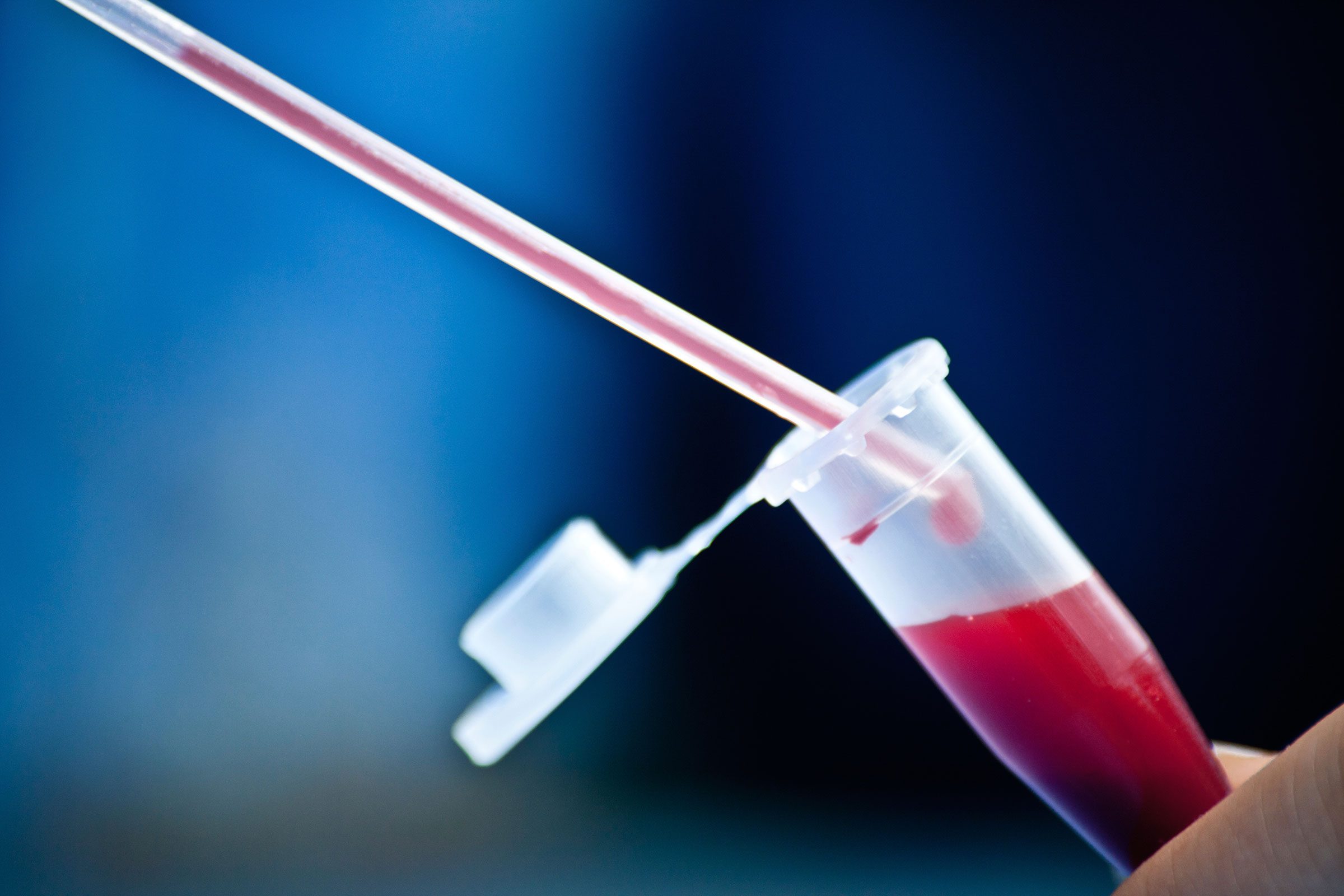
“All I need is a blood test to screen for allergies”
“Allergen-specific serum testing (for IgE) is not a reliable screen for allergy and often leads to misinterpretation and false-positive results which in turn lead to diagnostic confusion and unnecessarily eliminating foods from a diet. A negative test provides more useful information, providing evidence against such an allergy, but it also is not a failsafe.” —Morton Tavel, MD

“There’s nothing I can do personally to prevent an allergy attack”
“Most people don’t realize that hair sprays and gels act like a sticky paste. Pollen floating near you will often get stuck in your hair, so you will end up being a pollen magnet bringing your personal pollen with you wherever you go. That in turn, may make your allergy symptoms worse.” —Rob Danoff, DO
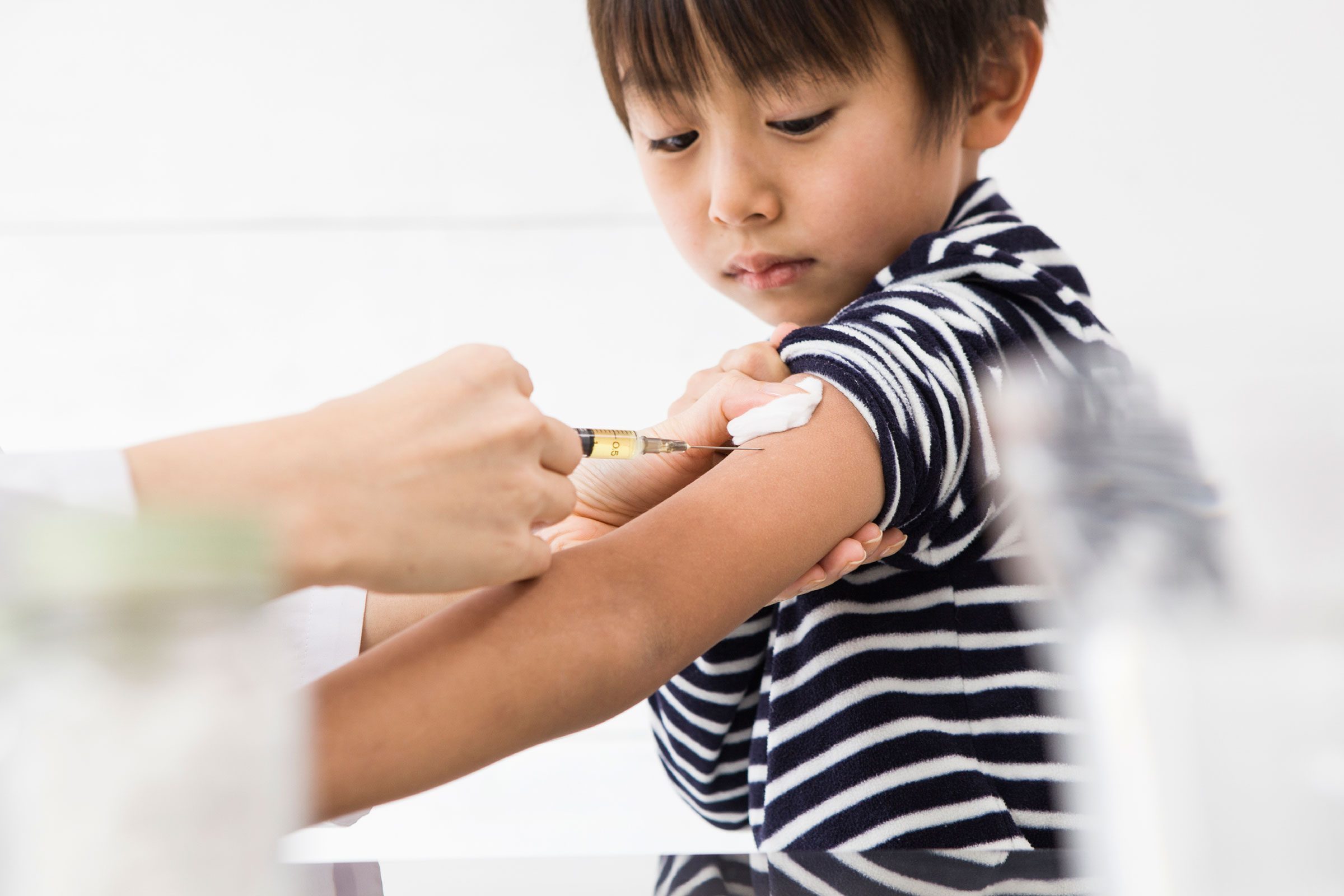
“My kid will outgrow her allergy”
“Children are ten times more likely than adults to have food allergies but while many children may outgrow them, others will not. Some researchers believe that as a person’s gastrointestinal system develops, it gets better at blocking the absorption of components that trigger food allergies. Over time, children typically outgrow allergies to cow’s milk, eggs, wheat, and soybean products. Allergies to peanuts, tree nuts, fish, and shellfish, however, are more likely to be lifelong. And some children will outgrow one allergy only to develop another.” —Morton Tavel, MD. This is why your kids should never use your allergy medication.

“I can’t get a CT scan, I’m allergic to shellfish”
“Radiologists and cardiologists often use iodinated contrast during CT scans and other procedures for better imaging. Since shellfish contain iodine, many physicians have linked a contrast reaction to a shellfish allergy. However, this is false, and a shellfish allergy has nothing to do with the reaction. In fact, iodine is not and cannot be an allergen as it is found naturally in the human body.” —Bryan Martin, MD

“I’m allergic to penicillin”
“Adverse reactions to antibiotics are very common, but true allergic reactions are rare. Approximately 10 percent of people in general say they are allergic to penicillin, but fewer than 10 percent of those will have a positive skin test or any symptoms if challenged. Labeling someone allergic to this antibiotic makes them more likely to receive less effective, more toxic, and costlier antibiotic alternatives. Thus efforts should be made to clear patients from retaining this label, if falsely applied.” —Morton Tavel, MD. These are the allergies of all types that are on the rise.

“What’s the big deal? It’s just an allergy”
“Although it rarely happens, allergies can kill. Some people have such an extreme sensitivity to a particular substance that the allergen can trigger an episode known as anaphylactic shock—a sudden, potentially fatal reaction that lowers blood pressure, swells the tongue, throat, or airways, making it difficult to breathe. Such a reaction requires immediate medical attention. Anaphylactic shock is most often triggered by a food or drug, but it can also result from an insect sting or injections of various medical agents. People with a history of severe allergic reactions should always carry a pre-loaded syringe of epinephrine (like an Epi-pen), which can be administered in an emergency.” —Morton Tavel, MD

“Natural or organic foods can’t cause allergic reactions”
“Limiting your diet to ‘all-natural’ or organic food is no guarantee that you’ll avoid allergies. In fact, some of the most allergenic foods are ‘natural’ unprocessed foods including cow’s milk, eggs, peanuts, wheat, soybeans, fish, shellfish, and tree nuts. Combined, these foods account for up to 90 percent of all ingested allergic reactions. Allergies are caused not by chemicals related to growing the food, but by proteins in the food itself.”—Morton Tavel, MD. Learn more about the 7 most common food allergy culprits.

“Seasonal and food allergies are unrelated”
“There is a condition called oral allergy syndrome (OAS) that may affect between 50 to 75 percent of seasonal allergy sufferers, where airborne allergens may sensitize you to those in food. For example, the proteins in certain fruits such as peaches and apples are similar to the proteins from Birch tree pollen so you may have a reaction to both the tree pollen and eating raw peaches and apples, although the symptoms differ. Those with OAS may experience a tingling or itchy throat, or swollen lips. In some more severe cases, some may experience wheezing and have trouble breathing. If you notice any of these symptoms when eating certain fruits and vegetables, please speak with your physician.” —Rob Danoff, DO

“Moving to Arizona (or Antarctica) will cure my allergies”
“For allergy sufferers, there simply is no safe haven. While desert regions have no maple trees or ragweed, they do have plenty of other plants that produce pollen, including sagebrush and cottonwood, ash, and olive trees. Relocating to such a region may offer relief for a few months, but a fresh crop of allergies to local plants is likely to develop before long.” —Morton Tavel, MD. If you’re suffering, these are the 10 new allergy solutions you haven’t heard of yet.

“Hay fever is giving me an actual fever”
“Fevers do not occur due to seasonal allergies because symptoms are not caused by a virus or bacteria, rather by an allergen. If you are presenting a low-grade fever, it’s likely that you have a cold caused by a virus.” —Rob Danoff, DO

“I can’t eat ice cream, I’m allergic to milk”
“When adults react adversely to milk—usually in the form of cramps, gas, and diarrhea—it’s often mistaken for an allergic reaction. In reality it’s usually a condition known as lactose intolerance, an inherited trait caused by the body’s lack of lactase, an enzyme needed to digest milk products. True milk allergy is only common among infants and is usually outgrown in adulthood.” —Morton Tavel, MD

“Allergy tests don’t work on kids younger than two or on elderly people”
“Allergy tests are valid at any age. Younger kids are less likely to have allergies, so the tests are more often negative, but they are valid.” —Jay Portnoy, MD, Division Director, Allergy/Asthma/Immunology at Children’s Mercy Kansas City

“Ugh, it smells like mold. I better leave before my allergies act up”
“Mold is everywhere and can cause real problems in susceptible persons, but it rarely causes allergies unless ingested in large quantities. Most health problems attributed to mold exposure are exaggerated, with no scientific basis or supportive evidence. You don’t need fancy air purifiers or other detoxification equipment.” —Morton Tavel, MD. These are the 11 common things you do that make your allergies worst.

“Alternative therapies are just voodoo”
“There are several complementary and alternative therapies patients can use to help relieve allergies. Saline nasal rinses can effectively moisturize and clean the nasal passages. They can actually help other medicines for allergies (like nasal steroids) work better if used immediately before. Another effective therapy comes from the plant butterbur. Butterbur has been shown to be comparable to antihistamines such as cetirizine (Zyrtec) and fexofenadine (Allegra) for some patients with allergies. If you want to use butterbur be sure to seek a professional’s advice in selecting a product—some formulations contain pyrrolizidine alkaloids which can lead to liver injury.” —Skye McKennon, PharmD (These are the neti pot safety tips you need to know before using one.)
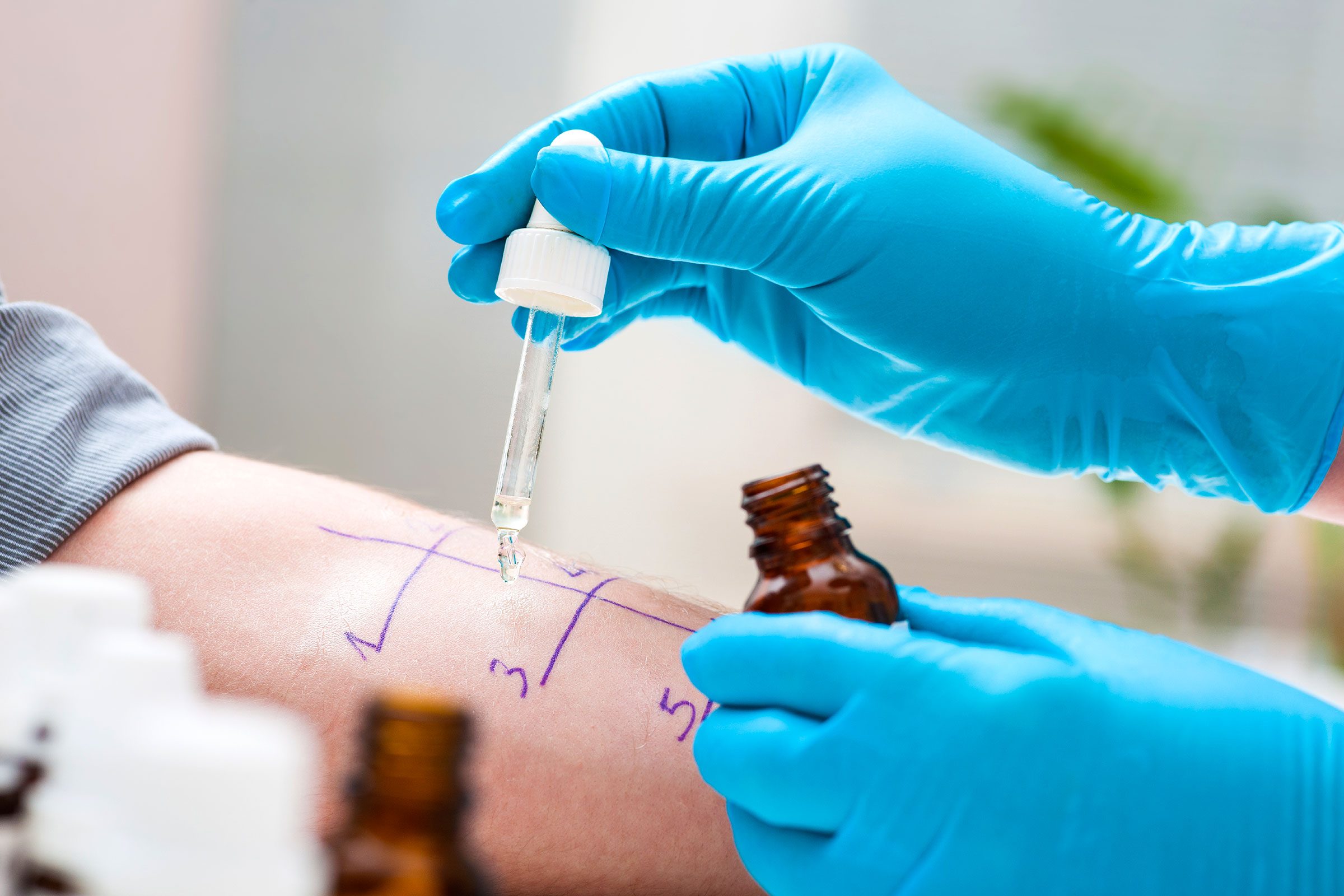
“Scratch tests aren’t reliable”
“Skin testing is reliable at any age. A positive result—a red, raised area called a wheal—means you reacted to a substance in a potentially allergic way. Such a positive result means the symptoms you are having are likely due to exposure to that substance. In general, the stronger the response, the greater the chance of allergy to that given substance. It is possible to get a false positive or false negative. In general, allergy skin tests are most reliable for diagnosing allergies to airborne substances, such as pollen, pet dander, and dust mites. Skin testing may help diagnose food allergies but because food allergies can be complex, you may need additional tests or procedures.” —Morton Tavel, MD. Next, check out the 13 ways doctors allergy-proof their homes.