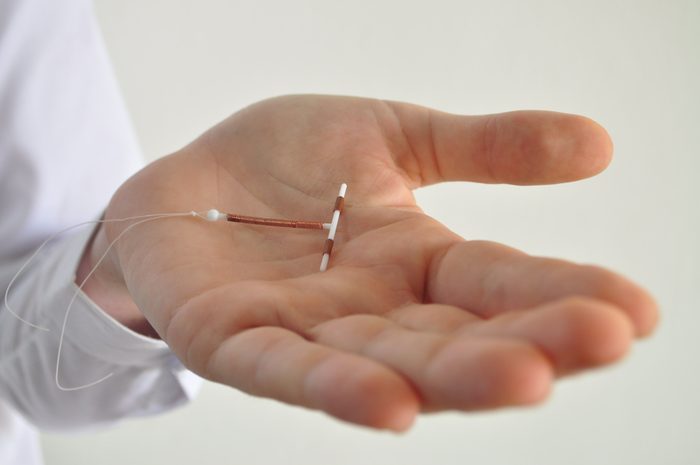
Why choose an IUD?
The birth control pill is an easy and popular contraceptive option, but the Centers for Disease Control and Prevention (CDC) says that the IUD (intrauterine device) is the next most common form of birth control. If you’re considering switching your birth control, here’s what doctors want you to know about using an IUD.

You don’t plan on getting pregnant in the near future
An IUD—which your ob-gyn can insert into your uterus in about five minutes—blocks contraception for many years. The hormone-free copper IUD called ParaGard is effective for up to 10 years. Hormonal IUDs Mirena and Skyla, which release low levels of progestin into the uterus, are effective for up to five years and three years, respectively. “The American College of Obstetricians and Gynecologists recommends long-acting reversible contraception, such as IUDs and implants, as a first line contraceptive option of women of all ages, even women who haven’t had babies, adolescents, and women over 40, because they are so safe, effective, and convenient,” says Petra Casey, MD, director of the Complex Contraception Clinic at Mayo Clinic. “But if you want to get pregnant in the next six to 12 months, an IUD is not a good option for you.”

You forget to take your pill consistently
Some women don’t want to worry about popping a pill every day or they just forget to take it, which can decrease its effectiveness. “You have to keep your serum level of hormones consistent to suppress ovulation, which is the primary mechanism of action of the pills,” Dr. Casey says. According to Dalia Davood, MD, of Advocate Lutheran General Hospital in Illinois, having an IUD eliminates the need to remember to take a pill in the midst of everything going on in life. It’s still critical to practice safe sex, however, as IUDs do not protect against sexually transmitted infections.

You want the most effective birth control possible
Human error often gets in the way of successful birth control, but there’s significantly less failure with an IUD that’s placed properly. According to Dr. Casey, a woman can expect the efficacy of her birth control to go from 95 percent on the pill to 99.9 percent with an IUD. “If a woman wants to have birth control put in and then just forget about it for years, that’s a good reason to switch to an IUD,” she says. (Here’s how to know if you’re using the wrong birth control.)

You have super-heavy periods
If you’ve tried using the pill to lighten your heavy periods and it didn’t really work, consider switching to the Mirena IUD, which is an approved treatment for heavy periods. “With the Mirena IUD, up to 70 percent of women decrease the amount of bleeding with their cycles and some women have no cycles at all within the first year or two,” Dr. Davood says. Keep in mind that while the Mirena IUD could decrease menstrual bleeding, the copper IUD sometimes can increase it.
You can’t take the pill
An IUD is a good alternative for women who have an underlying condition that makes birth control pills off limits. The pill may not be appropriate for you if you have a family history of blood clots, if you’ve had a blood clot, if you’re prone to migraine headaches, or if you have diabetes or a risk of heart disease, or if you’re a smoker over 35. When it comes to migraines, women who experience aura—verbal, motor, or auditory symptoms that indicate a migraine is coming—probably should not be on the pill and would be a good candidate for an IUD, according to Bridgette Blazek, MD, an obstetrician-gynecologist with Advocate Medical Group.

You’re not into taking hormones
Some women prefer to skip hormonal contraceptives or tend to have side effects from the hormones in birth control pills (and/or the hormonal ring and the patch). “Most patients can tolerate taking hormonal therapy just fine, but some are sensitive and feel that it’s not right for them and that’s OK,” Dr. Blazek says. “There are other options.”
Namely a copper IUD, which has no hormones and instead works by damaging or killing sperm and making cervical mucus thick and sticky, so sperm can’t get through. Even the hormonal IUDs use only one type of hormone—progesterone—versus two (estrogen and progesterone) in the pill. “So you may have fewer side effects using IUDs because of the type of hormone or non-hormone that’s in it,” Dr. Davood says. Make sure you’re not pregnant before getting an IUD inserted, and once it’s in place, check after each menstrual cycle that it’s still in the right position—you can feel for the one-inch string that hangs down, much like a tampon string. If you can’t find the string, call your doctor to get it checked.
Next, check out the contraception myths that could put your health at risk.