Keep these STD facts in mind
If you’re aware of these sex myths and other interesting sex facts, you also need to know about STDs, too. Here are some facts from experts that could save your life.

Cases of STDs are at an all-time high
STDs continue to rise in the U.S. Cases of chlamydia, gonorrhea, and syphilis reached an all-time high in the United States in 2018, according to the Sexually Transmitted Disease Surveillance Report released by the Centers for Disease Control and Prevention (CDC). “While the reasons are complex, health officials and researchers agree that the main drivers of the STD increases have been the closure of public health clinics, the lack of funding for STD awareness and prevention efforts, and the loss of state and local health department staff during the 2008 recession that were never replaced,” says Jeffrey Klausner, MD, professor of medicine in the Division of Infectious Diseases and the Program in Global Health at UCLA and member of the Infectious Diseases Society of America’s (IDSA) STD working group. “Additional reasons may include the increased use of social media, apps, and online sites (such as Tinder or Grindr) and the declining fear of AIDS now that AIDS is treatable.” Here are 8 sexual health conditions millennials aren’t talking about, but should be.

Anyone who has sex is at risk for getting HPV
Currently, there are nearly 80 million people infected with the human papillomavirus (HPV) and most (about 9 in 10) will get an HPV infection at some point in their lives, per the CDC. One of the reasons that HPV is so common is that there are more than 100 types of the virus; plus, it can be transmitted by digital, anal, or oral sex, says Dr. Klausner. (Although not all HPV types are sexually transmitted.) HPV can also be passed on by an infected person who has no signs or symptoms, because some people can take years to show symptoms.”While the majority of people who get HPV will clear the virus with their own immune system,” says Dr. Klausner, “having the virus can cause genital warts and cancer.” The HPV vaccine, usually given to children before entering seventh grade, protects against the nine strains of HPV that are mostly strongly linked to cancer and genital warts. According to the CDC, HPV is responsible for about 34,000 cases of cancer each year, including almost all cases of cervical and anal cancer. There are pros and cons to adults being vaccinated. Read on to discover if you should get the HPV vaccine as an adult.
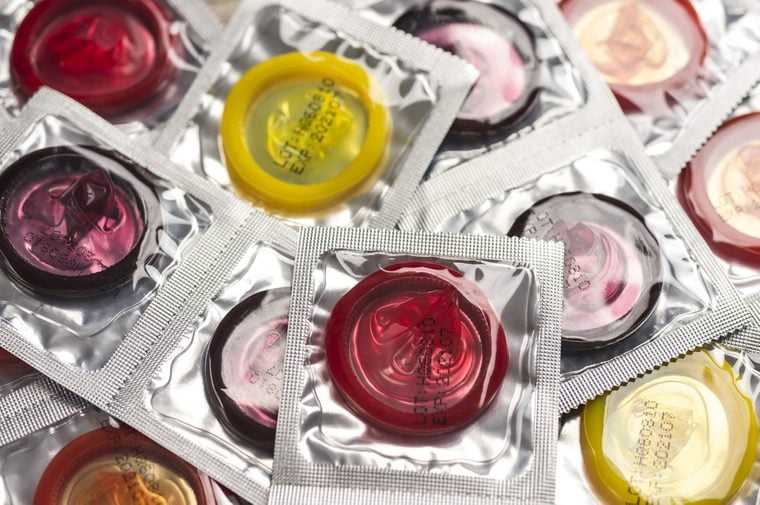
Condoms are not guaranteed to protect you from STDs
Condoms are a mantra for safe sex, but they’re not 100 percent effective when it comes to preventing the spread of STDs. “Condoms are best for retaining fluids and protecting against STDs contracted through genital fluids, such as gonorrhea, chlamydia, and HIV,” says H. Hunter Handsfield, MD, professor emeritus of medicine at the University of Washington Center for AIDS and STD. “But they are less effective in preventing STDs that are passed through skin-to-skin contact, such as syphilis, herpes, and HPV.” Both latex and female condoms are effective in preventing HIV and other STDs when used properly, says Patricia Ferguson, MD, physician consultant at Blue Cross Blue Shield of Michigan, but if the condom does not cover infected areas or sores, it’s likely that disease, most commonly HPV or genital warts, can be transmitted. “The only 100 percent effective method of STD prevention is abstinence,” she says.

You don’t have to have intercourse to get an STD
Often STDs spread due to myths and misconceptions, such as the belief that people can only be infected through sexual intercourse, says Dr. Ferguson. “For example, herpes or genital warts can be spread through skin-to-skin contact with an infected area or sore,” she says. STDs can also be transmitted through oral or anal sex, and researchers in Australia are theorizing that gonorrhea might actually be transmitted by deep kissing as well. Bottom line: “If you decide to have sex, you and your partner should get tested for STDs beforehand and always use protection,” says Dr. Ferguson. (Here are common lies you tell your doctor, and you should just stop.)

You should be tested for STDs annually
If you are young and sexually active, following the guidelines for STD screening is one of the most important steps you can take to protect your health. Young, sexually active people should be screened for STDs once a year, or more often if either partner is high-risk or is changing partners more frequently, says Dr. Handsfield. Testing involves a swab of the genital area or a urine test to detect gonorrhea or chlamydia; blood work is required to test for HIV or syphilis; Pap smears can detect HPV. While the most accurate testing is done in a medical setting, there are home self-tests available. (Here’s what happened when I tried an at-home STDs testing kit.) “If you don’t have access to health care, you can get an over-the-counter test for HIV,” says Dr. Handsfield. Other sources include websites that let you order the test online, visit a test center, and then receive your results via email. You can even get an at-home STD test subscription to test yourself more regularly.

STDs often have no symptoms
There are approximately 20 million new STD infections each year, according to the CDC, and almost half of them occur in people between the ages of 15 to 25. “It’s also true that many STDs don’t come with symptoms,” warns Dr. Ferguson, “even the ones that can do serious damage to your body.” Chlamydia, gonorrhea, HPV, and HIV can all be asymptomatic. “Eighty percent of women with chlamydia carry it with no symptoms and they won’t know unless they get tested, says Dr. Klausner. “Gonorrhea may also not have symptoms about 50 percent of the time: You can have gonorrhea of the throat or of the rectum—be a carrier—and have no idea,” he says. The American Sexual Health Association reports that close to 90 percent of those with genital herpes don’t know they have the infection. These statistics show why it’s important to get tested regularly and be honest with your doctors about your sexual activity, says Dr. Ferguson. “Moreover, be honest with sexual partners and always use protection,” she says. Ladies: having this vaginal condition (that 30 percent of women have and most don’t realize) can double your risk of becoming infected with HIV.

Chlamydia is the most prevalent STD
According to the CDC’s STD Surveillance Report, chlamydia is the most frequently reported STD in the United States, accounting for 1.8 million new cases that year—up 19 percent since 2014. Known as the “silent infection,” chlamydia often is asymptomatic. If left untreated, the condition can cause pelvic inflammatory disease, chronic pelvic pain, infertility, and potentially fatal ectopic pregnancy. Having the infection puts pregnant women at risk of preterm delivery and may increase the likelihood that their infants will develop conjunctivitis and pneumonia.

A new STD that is almost as common as chlamydia
The bacteria Mycoplasma genitalium (MG) is a newer type of STD. It is almost as common as chlamydia, but there is no FDA-approved test yet, and many doctors don’t even know about it, says Dr. Klausner. Like chlamydia, MG often does not have symptoms; if left untreated can cause urethritis, pelvic inflammatory disease, miscarriage, preterm labor, and cervicitis. Symptoms of the condition include lower abdominal pain, pain with intercourse, and vaginal discharge in women and burning with urination and penal discharge in men. The bacteria spreads through sexual intercourse as well as skin-to-skin contact and can be difficult to treat with common antibiotics such as penicillin. Don’t miss these surprising reasons for painful sex.

Untreated STDs increase your risk for HIV
While most STDs are treatable, they can be very dangerous if you ignore them—or if you aren’t even aware you have them, explains Dr. Ferguson. “Sexually transmitted diseases, if left untreated, can increase the chances of getting HIV.” According to the CDC, people who get syphilis, gonorrhea, and herpes are more likely to have HIV or get HIV in the future because the behaviors that put them at risk for one infection—not using condoms, multiple partners, anonymous partners—often put them at risk for other infections. Having a sore or inflammation from an STD also makes it easier to become infected with HIV. Here are additional surprising things most people don’t know about HIV and AIDS.

You can get STDs from oral sex
Engaging in oral sex is another way to contract an STD, says Dr. Ferguson. The most common STDs transmitted this way are gonorrhea, genital herpes, and syphilis; the riskiest type of oral sex is mouth-to-penis oral sex. However, the overall risk is low when compared to vaginal or anal intercourse, and oral sex is not a risk factor for HIV, says Dr. Handsfield. Other potentially dangerous conditions passed through oral sex include hepatitis A and B, E. coli (responsible for food poisoning), and parasites such as giardia. Here are the silent signs you have a parasite.

Zika can be transmitted by having sex
“Zika is not an STD, but it can be transmitted by sex,” says Dr. Klausner. “Men who have been infected have it for 30 days, so they can transmit to another female or male.” Zika, which starts with the infectious bite of a mosquito, often produces no symptoms or very mild symptoms: Most people don’t know they have it. According to the CDC, the disease poses the greatest risk to pregnant women because it can cause a birth defect of the brain called microcephaly, along with pregnancy issues such as miscarriage, stillbirth, and other birth defects. Check out these fast facts you need to know about the Zika virus.

Some forms of STDs are drug-resistant
Gonorrhea is one of the most common sexually transmitted diseases around the world, accounting for more than 78 million estimated cases worldwide and classified as the second most common STD in the United States. In 2017, the World Health Organization reported that gonorrhea has become increasingly more difficult and sometimes impossible to treat with antibiotics. The gonorrhea superbug is a different strain that is common in parts of southeast Asia, explains Dr. Klausner; there are three new antibiotics in development and new tests coming out that will tell doctors how to best treat this STD. Gonorrhea, which can infect the genitals, rectum, and throat, often does not have symptoms and if left untreated it can lead to pelvic inflammatory disease, ectopic pregnancy, infertility, and an increased risk of HIV. Make sure to ask your doctor these essential questions before taking antibiotics.

If you have these symptoms, seek medical attention
Any abnormal discharges from the genitals, burning with urination, pain with intercourse, bleeding after intercourse, lower abdominal pain, rectal bleeding, or throat infections are a signal to get tested—they’re all key signs of STDs, explains Dr. Klausner. However, many STDs are asymptomatic, and you won’t know you have one unless you get screened by your doctor. If you’re active sexually and change partners (or your partner has slept with other people), consider that a reason to be tested. Here are essential things your vaginal discharge can reveal about your health.

Common sense is the best prevention
Ideally, getting vaccinated for HPV, wearing protection, and reducing the number of sexual partners will help lower your risk, according to the CDC. Being prepared is critical, regardless of plans and pledges, says Dr. Handsfield. As with other health risks like smoking and obesity, people understand that having sex comes with a risk and they need to be prepared for it, he says. “When you are out there dating, have common sense: If you have sex with new and unknown partners use condoms.” Read about these things that happen to your body when you stop having sex.
