What to Expect When You Get a Mole Removed
Updated: Jun. 30, 2022
After having a few moles removed, I was surprised by how long the scars took to heal. Here's what I learned about smoother—and faster—recovery
Our editors and experts handpick every product we feature. We may earn a commission from your purchases.

A couple of years ago, I had three moles removed. My trusted dermatologist told me they looked suspicious in my yearly skin exam, and so he wanted to remove and biopsy them. I’m three-quarters Italian and tan easily in the summer, but my grandpa did have melanoma (they caught it early, thankfully).
As a health writer, I know that having a family history increases your risk of melanoma. Furthermore, catching it early is key to prevent it from spreading, and it also increases your chances of successfully treating it, according to the Skin Cancer Foundation. So, if my doctor tells me something on my skin looks suspicious, I’d rather be safe than sorry.
I did have some concerns about scarring—two of the moles were on my ribcage right under my breasts, and the third was in my cleavage. My doctor reassured me that as long as I was diligent about wound care, it shouldn’t be so bad. At my next appointment, he shaved them off.
But, despite my tending to my wounds every single day without fail, the scars were pretty noticeable months after they healed. It looked like someone scooped out small chunks of my skin because, well, that’s essentially what had happened. The scars on my ribcage are noticeable in a bikini. The scar in my cleavage was really visible in my wedding dress. If I had expected that scar, I probably would have waited to have it removed until after my wedding. I know that some scarring is simply the cost of doing business. But, I really wish I had known more about what to expect when I said yes to having my moles removed. Now, a few years later, the scars have smoothed out a bit, but they’re still noticeable, discolored indentations in my skin.
To figure out if my experience was normal, I asked a few dermatologists to explain the typical mole removal process and what people might want to know beforehand.
Two main options for mole removal
When dermatologists remove biopsy moles, they can do it one of two ways, says Amanda Wendel, MD, dermatologist at Northwestern Medicine in St. Charles, Illinois. One option is a shave excision, which is what I had. The doctor will use a razor-like tool to basically shave off the mole and some of the skin around it.
The other option is called a punch biopsy and is often used when the mole goes deeper into the skin, according to the National Cancer Institute. A circular tool with a blade is pressed into the skin around the mole to cut it out. Since the cut usually goes pretty deep, your doctor will then put in a few stitches.
Which one is best depends on factors like the shape of the mole, the size of the mole, and both your and your doctor’s preference, Dr. Wendel says.
Mole removal should be painless
A lot of people think that mole removal is going to be a painful procedure, says Susan Y. Chon, MD, dermatologist at The University of Texas’s MD Anderson Cancer Center in Houston. “The thought of having a biopsy is so stressful and the truth is, it’s quite painless,” she says. “It’s a very tolerable and non-invasive procedure. It’s done very quickly and very effectively.”
Your doctor will use a tiny needle to inject an anesthetic into the area, which numbs you instantly. “People are always shocked that it gets numb so fast,” says Dr. Chon. Personally, I don’t do well with needles, but I’d agree that the numbing part was quick and painless, and all I felt during the removal was some pressure.
Wound care for proper healing
“Either with or without stitches, we want the wound to stay moist and covered,” Dr. Wendel says. “Moisture helps it heal. We want new skin cells to migrate easily and quickly [to the site of the wound], and a moist environment can help with that.” Moisture helps prevent scabbing, which can essentially act as a barrier and makes it harder for new skin cells to migrate to the area and heal the wound. Covering the wound with a bandage will protect it from dirt and debris that can cause infection, Dr. Wendel says. That’s why my doctor had me apply an ointment and change the bandage a few times each day.
Dr. Chon also notes that it’s important to avoid submerging the area in water (swimming or taking a bath) until the wound is healed. On that note, it’s a good idea to time any mole removals for when you don’t have an upcoming vacation planned, she says. Traveling itself makes it harder to keep up with proper wound care, and spending time in the sun can further damage the area and hinder healing. My doctor specifically asked me if I had any beach vacations planned for the near future (I did). We waited a few weeks until I got back to take off my moles.
Your dermatologist will also ask you to limit your activity to prevent pulling and tension, especially if you’ve had stitches, Dr. Wendel says. “Depending on where the spot is, we don’t want any heavy physical activity for at least two weeks.” After my biopsies, I had to avoid movements that required me to lay down on my stomach or really twist or bend my torso, but was able to do pretty much everything else.
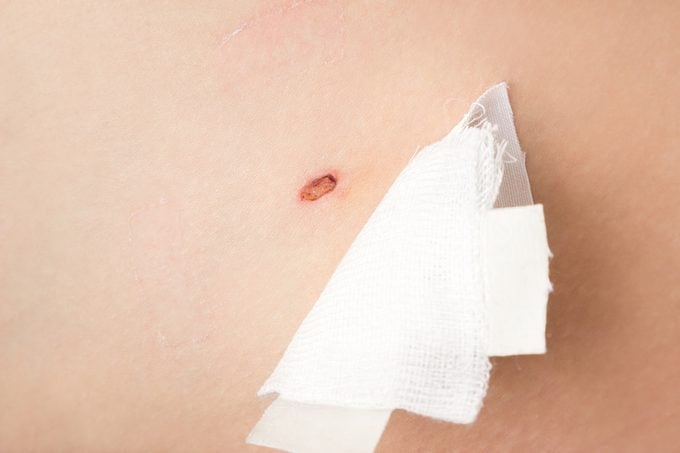
The ups and downs of the healing process
I’m a very compliant patient, so I was pretty annoyed that my wounds weren’t healing perfectly. Apparently, being young is a disadvantage when it comes to mole removal scars.
“It is true that people do heal differently and some of that has to do with the age of the patient,” Dr. Wendel says. Younger people actually tend to scar more, she says, because having tighter, more elastic skin makes scarring more noticeable. (Who knew?!)
Some areas of the body also tend to scar more than others—usually, anywhere the skin is tighter or where there’s a lot of movement and pulling on the wound. “The shoulders and upper back are probably the worst,” Dr. Wendel says. The abdomen can also be a bad area, she adds. Keloid scars—raised and bumpy—are more common on the chest and upper back, says Dr. Chon. In contrast to my slightly concave scars, keloid scars occur thanks to an overgrowth of collagen during the healing process.
Also, some people are just genetically prone to scarring more, Dr. Wendel says. Sometimes there isn’t much of an explanation beyond that.
How to minimize scarring
“It’s impossible to do scarless surgery, even for a plastic surgeon,” Dr. Wendel says. “But there are a few things you can do to help improve it.” That is, beyond taking good care of the wound and helping it heal as quickly as thoroughly as possible.
Dr. Chon says that the type of removal I had, a shave excision, can sometimes leave a permanent depression in the skin, especially if your doctor ends up having to shave a little deeper than they had anticipated to get all of the mole. Scarring can still happen with a punch excision, but it can be a little less noticeable. Stitching the two sides of the wound together makes the scar smaller and flatter.
Once the wound is much healed, gently massaging the area may help break up the scar tissue, says Dr. Wendel. She recommends using ointment, like Vaseline or Aquaphor, and gently rubbing twice a day for two to three minutes each time. And don’t forget to keep the scar protected with sunscreen to help with any increased pigment.
“Sometimes we also recommend using silicone-based products or cortisone-based products to help with scars,” Dr. Wendel adds. You can find these over-the-counter—like this Cica-Care Silicone Gel Adhesive Sheet—but it’s best to ask your dermatologist about what they recommend for the specific type of scar you have.
Dr. Wendel also makes an important note: It can take a couple of years for a scar to fully mature. “Don’t pass final judgment on the appearance of a scar for two to three years,” she suggests. At that point, if you’re still not happy with how it looks, you can explore cosmetic treatments like lasers for redness and discoloration and certain injections that may help flatten the scar.
While I’m not thrilled about my scars at my 2+ year mark, I don’t regret having my moles removed. Now that I know what to expect, I’ll be more prepared for any biopsies I need in the future.















