
Type 2 diabetes complications: Serious, but preventable
With type 2 diabetes, you no doubt know about worst-case scenarios if you don’t manage your disease. But those outcomes are rare—and very preventable. “Just because you have diabetes doesn’t mean you will lose your sight or your kidneys or your legs,” says Aaron Cypess, MD, PhD, an investigator at the National Institute of Diabetes and Digestive and Kidney Diseases at the National Institutes of Health. “None of these things has to happen. You can stop or reverse the progression and get back your quality of life.”
But what’s equally important is learning about the type 2 diabetes complications that can happen when diabetes isn’t controlled.
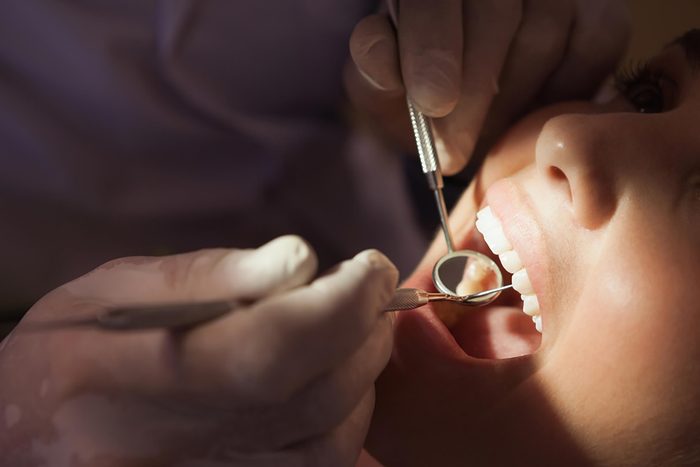
You can get more cavities and gum infections
People with diabetes don’t have as much saliva, which can lead to dry mouth and a greater risk of cavities and gum disease, says George L. King, MD, research director at Joslin Diabetes Center, a professor of medicine at Harvard Medical School, and author of The Diabetes Reset. And you need normal blood sugar to maintain proper oral health, says Dr. Cypess. “It’s very important for people with diabetes to have regular evaluations of their teeth and gums, or else they could lose them. People with diabetes need to be more vigilant about brushing, flossing, and seeing a dentist than a person ordinarily would be.” (Here are some things your dentist wishes you would do differently.)

You can get more urinary tract infections
People with type 2 diabetes are more likely to get urinary tract infections than people without diabetes. Those infections are also likely to be more severe and have worse outcomes, including the chance that they’ll lead to hospitalization, according to a study published in 2015 in Diabetes, Metabolic Syndrome and Obesity.
Sugar in the urine becomes a breeding ground for bacteria. Diabetes also contributes to nerve damage in the bladder, which can allow urine to pool—and bacteria to grow. Urinary tract infections are treated with antibiotics.

Your sexual function may be affected
Diabetes in both men and women can detract from intimacy. According to figures from Joslin Diabetes Center, more than 50 percent of men with type 2 diabetes experience erectile dysfunction; about 30 percent of men whose diabetes is well controlled do. “An erection requires good, healthy blood vessels, which get damaged in diabetes patients,” says Dr. Cypess. (These are the most common nine signs of diabetes in men.)
About 35 percent of women with diabetes may experience sexual dysfunction, including lack of desire, pain or discomfort, and inability to orgasm. High blood sugar can damage the blood vessels and nerves that make intercourse enjoyable, according to the National Institute of Diabetes and Digestive and Kidney Diseases. Here are some tips for a healthy sex life if you have diabetes.

Your memory and mental sharpness can suffer
Numerous studies suggest a link between type 2 diabetes and an increased risk of cognitive issues, including dementia. One study published in 2013 in the Journal of Diabetes Investigation found that people with diabetes were up to 73 percent more likely to develop dementia than those who didn’t have diabetes. Insulin may play a part in memory and learning. Diabetes can also damage blood vessels in the brain, which can affect blood flow and nutrient delivery to cells and contribute to a condition known as vascular dementia. (These are the life-saving lessons one woman learned from her father’s type 1 diabetes.

You can be more likely to get depression
Rates of depression are two to three times higher in people with diabetes than in those without the disease, says Dr. King. Scientists suspect that diabetes can contribute to depression and that depression can contribute to diabetes risk—a two-way street. Feeling depression-like symptoms are also a silent sign you have diabetes. Brain scan studies have shown that certain parts of the brain are particularly affected by changes in glucose levels, which could affect depression risk.

You feel indigestion, nauseous, or very full after meals
Diabetes can affect the function of the vagus nerve, which controls how food moves through your digestive tract, according to the American Diabetes Association. When this nerve doesn’t work properly, food takes longer to leave your stomach, which can lead to a host of uncomfortable type 2 diabetes complications, such as heartburn, nausea, and vomiting, bloating, feeling full after meals, and lack of appetite. If you have gastroparesis—a condition where your stomach can’t empty properly—your doctor might recommend eating-habit tweaks such as having smaller meals or avoiding high-fat or high-fiber foods. You might also need to change or adjust your medications, including the timing and dosage of insulin. (Check this list of foods for people with diabetes.)

Your eyesight can deteriorate
In the short term, fluctuations in glucose levels can cause the lens of the eye to swell, which can make your vision blurry, says Dr. King. In fact, when patients are first treated for diabetes, their vision may even seem to get worse—which is totally normal—because as their blood sugar levels drop, the lens can change shape. But the eye will adjust within a few weeks.
However, over time, diabetes raises the risk of far more serious problems, including a cluster of issues known as diabetic eye disease: diabetic retinopathy (damage to blood vessels in the back of the eye); cataracts (clouding of the lens); and glaucoma (fluid in the eye that damages the optic nerve and causes vision loss). The National Eye Institute recommends that people with diabetes get a comprehensive eye exam every year to catch these problems as early as possible—when they are more treatable. These 30 simple habits help protect your eyes.
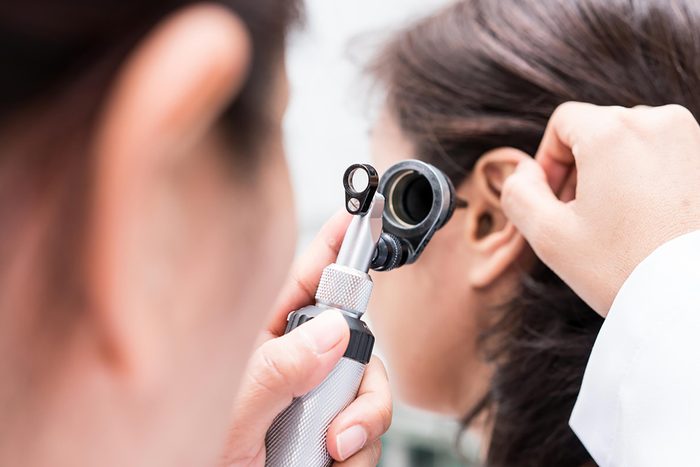
You can get ringing in your ears
Nerves in the ear can be damaged in people with diabetes, which can lead to ringing, or tinnitus, according to Dr. King. Managing blood glucose levels can improve symptoms.

You’re more prone to sleep apnea
People with diabetes are more likely to have sleep apnea. Being overweight or obese increases your risk for both sleep apnea and diabetes. There is also a newer theory that suggests that the connection between sleep apnea and diabetes may have to do with insulin resistance, says Dr. King. For example, thin people who are insulin resistant also are more likely to get sleep apnea. There is also evidence that the reverse is true: people with sleep apnea have an increased risk of excessive cortisol due to lack of adequate sleep. This cortisol rise causes insulin resistance. Sleep apnea, a condition in which you repeatedly stop and start breathing throughout the night, can raise the risk of many other serious problems, including high blood pressure. Proper treatment, commonly with a mask you wear that helps keep your airway open when you’re asleep, can make a big difference.
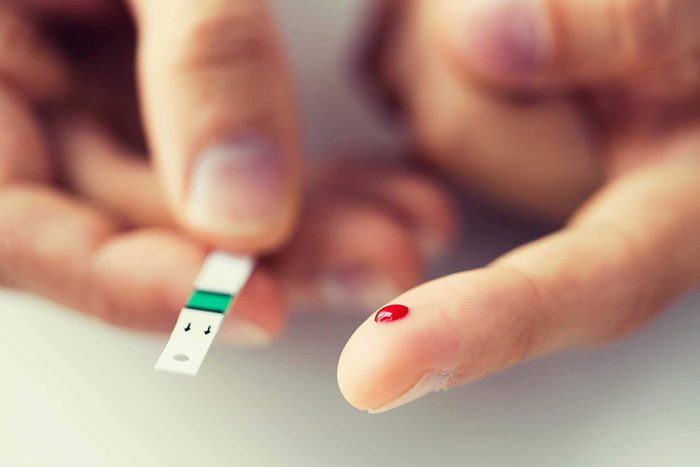
You can get fatty liver
This is another example of “which came first?” This build-up of fat in the liver may contribute to diabetes risk—and people with diabetes may also be more likely to deposit fat in the liver. Either way, the connection is striking: about 70 percent of people with diabetes have fat in the liver, according to a study published in 2018 in the Indian Journal of Endocrinology and Metabolism. An accumulation of fat makes it harder to control blood glucose levels.
Fatty liver often has no symptoms but causes inflammation and scarring that over time can prevent the liver from working properly. Inflammation in the liver is called hepatitis and the scarring is called cirrhosis. Slimming down—losing even just 5 percent of body weight—and reducing carb intake can dramatically improve fatty liver.

You can have foot problems
Type 2 diabetes complications often include foot problems, but simple routine steps can help. Damaged nerves in the feet can cause you to lose sensation in your feet, so you’re less likely to feel pain, heat, cold—or, say, a blister from a new shoe, according to the American Diabetes Association. Since you can’t feel these early warning signs, feet can more easily become infected; what’s more, high levels of glucose in the blood and impaired blood vessel scan make the infections slower to heal. (In very severe cases, bad infections just keep getting worse, causing skin tissue to die. This is what leads to the need for amputations).
But simply looking at your feet every day can ensure this never happens. Examine your feet every day for redness, swelling, ingrown toenails, or any areas of discoloration and tell your doctor if you find anything. And be sure to check out these recommended slippers for men with diabetes.
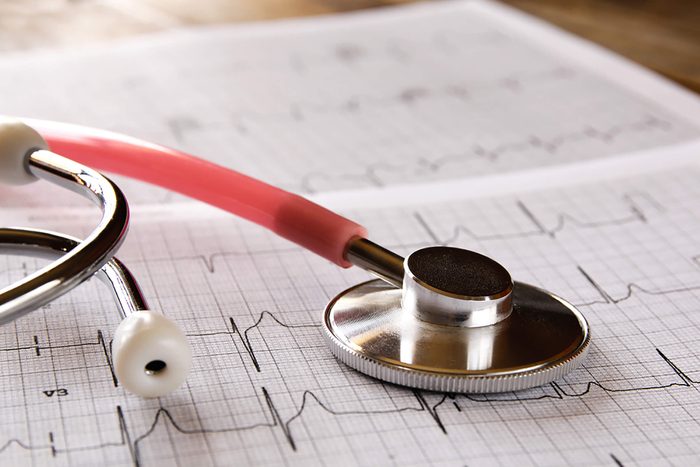
Your heart has to work overtime
The risk of heart disease is two to three times higher in people with diabetes, making it the strongest risk factor for heart trouble, according to the Joslin Diabetes Center. A cluster of issues is in play: Blood vessels in diabetes patients—already impaired—are more vulnerable to wear-and-tear from other risks like smoking, high cholesterol, and high blood pressure. (And according to Joslin, 90 percent of diabetes patients have one or more of these additional risk factors). Diabetes patients also have increased low-grade inflammation in the lining of their arteries, which can lead to the stiffness that precipitates heart disease.
Fortunately, many of the same good lifestyle habits can help prevent both diabetes and heart disease. Even if you’ve heard them before, these big ones bear repeating: Stop smoking, lose weight if you need to, maintain healthy blood pressure and blood fats/cholesterol, get physical activity, and keep blood glucose levels in check. There are certain classes of medications: statins, PSK9 inhibitors, SGLT2 inhibitors, and GLP-1 agonists that have been shown to reduce the risk of heart disease, too.
Up next: Don’t miss these simple tricks for living well with diabetes—from people who have it.
