Your body’s defense system
A normal body temperature is 98.6 degrees Fahrenheit; when it hits 100.4 or above, you have a fever. Many times, a fever can be a sign that your immune system is functioning well. Your body heats up because it senses a foreign invader: “Bacterial, viral, or something else that’s not supposed to be there,” says Deborah Nunziato-Ghobashy, DO, a family medicine physician at Scarsdale Medical Group.
“The hypothalamus in the brain controls your body temperature and raises it to kill off anything that could be invading your body,” she says. “All those bacteria and viruses prefer a cozy 98.6-degree environment to keep on replicating. Once it’s higher, it’s too hot for them and they start to die off.”
But what about those times your fever is a red flag for something more serious? Here’s what you should look for.

Persistent fever
A fever is usually a sign that your immune system is busy at work fighting off an illness. But if you’re still running a temperature after three days, you should see your doctor.
“A fever with no obvious origin that persists despite the appropriate use of traditional fever-lowering agents—like acetaminophen, naproxen, ibuprofen, or aspirin—is concerning,” says Gary LeRoy, MD, a family physician in Dayton, Ohio and president of the American Academy of Family Physicians.
That’s especially true if you’ve been exposed to the coronavirus (fever is the most common symptom of coronavirus). A study published in The New England Journal of Medicine found that 44 percent of almost 1100 patients hospitalized with coronavirus in China had a fever when they first arrived at a healthcare facility.
“A persistent fever of 100.4 degrees or higher associated with a history of possible Covid-19 exposure should raise suspicion,” says Dr. LeRoy. “An episode of sudden confusion, agitation, or mental status changes in a young to middle-aged adult is also concerning.”
Other physical signs requiring urgent attention, he says, are fevers accompanied by:
- Trouble breathing
- Persistent pain or pressure in the chest
- Inability to wake or stay awake
- Bluish lips or face
- Rapid pulse/heartbeat

Pain on the lower right side of your belly
If you have a fever and you experience abdominal pain that starts around the belly button, but within two hours moves to the right lower quadrant of the abdomen and becomes severe, those are signs you have appendicitis, says Dr. Nunziato-Ghobashy.
In a study published in JAMA, fever was the single biggest red flag associated with appendicitis in children with abdominal pain. Not only did the researchers find that a fever increased the likelihood of appendicitis, but its absence was associated with a decreased chance of appendicitis. The condition is typically confirmed with a CT scan and doctors will perform surgery to remove the appendix. If surgery is not performed quickly enough, the appendix can burst and cause infection and even death.
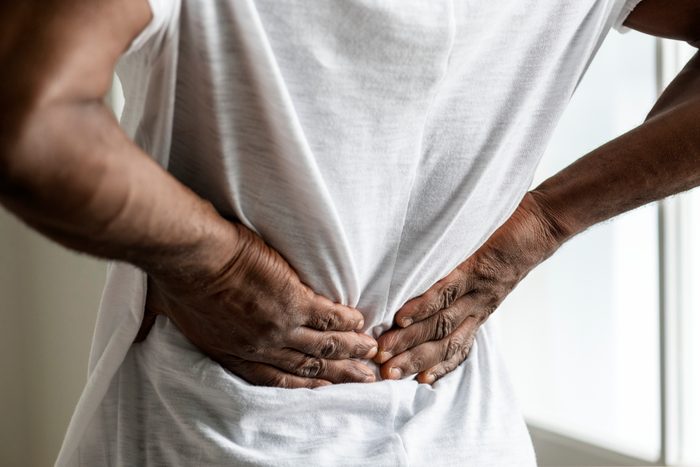
Low back pain and blood in the urine
If you have a fever accompanied by burning pain when you urinate, lower back pain, pelvic pain, blood in the urine, or urine that looks cloudy or smells funny, you may have a urinary tract infection (UTI), says Dr. Nunziato-Ghobashy.
When this type of infection gets more advanced, you’ll end up with a fever. Your doctor can take a urine sample to look for white blood cells, red blood cells, or bacteria—all signs of a UTI. Patients typically get medication for the pain as well as an antibiotic to eliminate the infection.

Sore throat
Strep throat is a bacterial infection that’s more common in children than adults. In addition to an intensely sore throat along with a fever, symptoms can include tiny red spots on the roof of the mouth and swollen lymph nodes in the front of the neck, as well as red and swollen tonsils, which are classic signs of tonsillitis.
Until recently, scientists were puzzled by the fact that strep throat is so highly prevalent in kids, and yet not all kids develop tonsillitis. A study published in 2019, in Science Translational Medicine, however, sheds light on the long-standing mystery. Turns out that kids who have repeated bouts of tonsillitis have fewer of the antibodies that protect against strep throat.
Your doctor can do a quick strep test to see if a type of bacteria called group A strep are causing your or your kid’s sore throat. If the test is positive, “you’ll need to be treated with antibiotics,” says Dr. Nunziato-Ghobashy. If left untreated, strep throat can also lead to rheumatic heart disease.
Be sure to finish all the medication, even after your throat feels better, she adds. “Lingering strep bacteria can cause pericarditis, an infection of the heart valves, which is very serious.”
Digestive disorder
Irritable bowel syndrome (IBS), Crohn’s disease, ulcerative colitis, and celiac disease are all very different digestive ailments, but all can trigger an inflammatory response in the body—and that can raise your temperature.
“Sometimes fever is the first sign,” says Dr. Nunziato-Ghobashy. And if you alternate between constipation and diarrhea—common among people with these conditions—the body can react to symptoms of dehydration and raise your temperature, she explains.
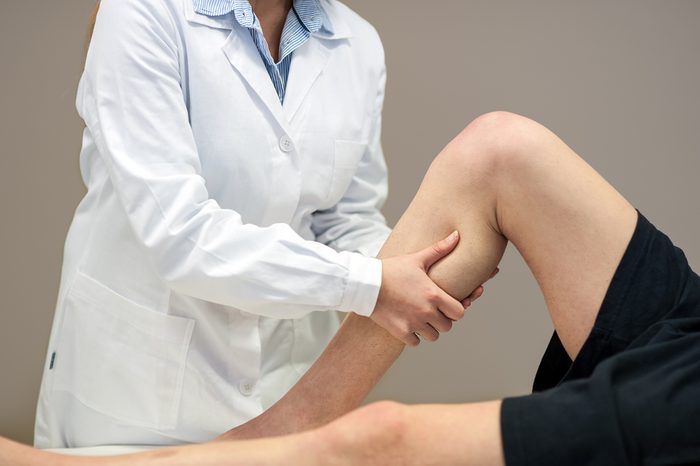
Blood clot
Abnormal blood clotting—which prevents blood flow—is among the more dangerous symptoms to emerge in patients with severe Covid-19. But how exactly the coronavirus triggers the formation of blood clots is still a mystery.
One study, published in the journal Blood, suggests that changes in blood platelets triggered by Covid-19 may be to blame, possibly because that contributes to the onset of heart attacks, strokes, and other serious complications. The researchers found that inflammatory proteins produced during infection significantly altered the function of platelets, making them more prone to form potentially deadly blood clots in the lungs, as well as deep vein thromboses in the legs.
Whether caused by Covid-19 or not, “a deep venous thrombosis (DVT) is a serious medical condition that requires immediate care,” says Dr. LeRoy. “One of the signs of a DVT that is likely not present in Covid-19 would be a swollen, red, possibly tender leg where the blood clot had formed. Blood clots can sheer off and float to the lungs causing a pulmonary embolism—a clot trapped in a major lung vessel—which may cause severe chest pain along with trouble breathing. This can be life threatening and needs immediate medical attention.”
A doctor will do a physical exam to check for swelling, and may also order an ultrasound of the leg to see if there’s a DVT.

Joint pain
Not to be confused with the more common osteoarthritis—which occurs when the cartilage protecting your joints wears down over time—rheumatoid arthritis is a chronic autoimmune condition that affects different parts of the body. In most cases, symptoms come on gradually, and weeks or months may pass before you feel the need to seek medical care. In addition to a low-grade fever, early symptoms include fatigue, muscle pain, weight loss, and numbness and tingling in the hands.
“Arthritis, especially rheumatoid arthritis, can raise inflammatory markers in the body and cause you to have fever,” says Dr. Nunziato-Ghobashy. “Sometimes a fever that seems to have an unknown origin can be triggered by arthritis.” You may also have joint pain and body aches. Typically the pain will be felt on both sides of the body and is worse in the morning. It will often be accompanied by insomnia.
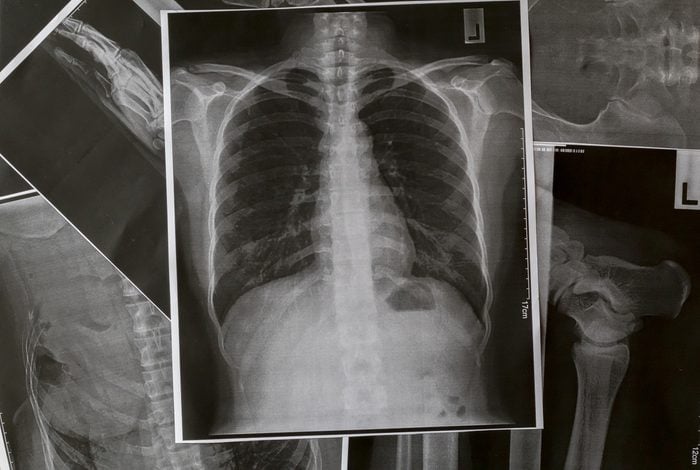
Breathlessness, exhaustion
Pneumonia inflames your lungs’ air sacs, which may then fill up with fluid or pus. The infection can be viral or bacterial. In addition to fever and chills, symptoms can include cough with mucus, chest pain, and shortness of breath. Always see a doctor if you suspect you or someone you are caring for has pneumonia, especially if they’re in a high-risk group: children 2 or younger, adults 65 or older, people with a chronic health condition or weakened immune system, and those who’ve been exposed to Covid-19.
“Fever, cough, and shortness of breath accompany both Covid-19 and pneumonia,” says Dr. LeRoy. “You should see your family physician if you have these three symptoms, regardless of exposure to Covid-19. When in doubt, check it out.”

Swollen neck, fatigue
Fever, fatigue, swollen lymph nodes in the neck, sore throat, and an enlarged spleen are the hallmark symptoms of Epstein-Barr virus, also known as mononucleosis. Common among children and adolescents, less so among adults, it usually resolves in two to four weeks but the effects can last for months, according to the Centers for Disease Control and Prevention. Your doctor can confirm the diagnosis with a blood test; treatment includes rest, drinking plenty of fluids, and taking OTC medications for pain and fever.
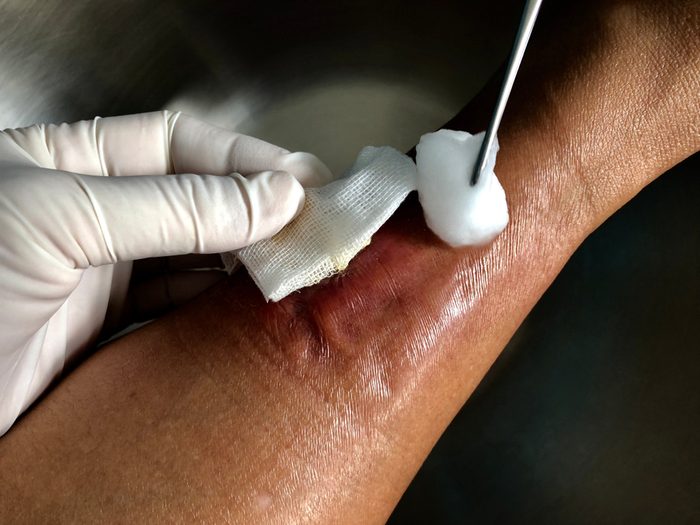
Skin infection
Cellulitis is a common—and serious—bacterial skin infection that often appears on the lower legs but can turn up anywhere on the body or face. It occurs when bacteria infect a break or crack in the skin; at first, you’ll see a swollen, red patch on the skin that is warm and painful to the touch. You may also get a fever, red spots, skin dimpling, and blisters. Patients with a history of cellulitis, particularly of the lower limbs, have an estimated recurrence rate of eight to 20 percent, according to a study published in 2018 in Clinical Medicine.
“The infection can spread quickly if not caught in time,” says Dr. Nunziato-Ghobashy. Seek emergency care if you notice signs of cellulitis. The good news about that infection: it isn’t contagious.

The stomach flu
With gastroenteritis—commonly called the stomach flu although it’s unrelated to influenza—your digestive tract is irritated and inflamed, typically because of a virus, says David Greenwald, MD, professor of medicine and gastroenterology at the Icahn School of Medicine at Mount Sinai and director of clinical gastroenterology and endoscopy at Mount Sinai Hospital in New York City. “Signs and symptoms often include nausea, vomiting and diarrhea, as well as a low-grade fever is common.”
Symptoms typically last from two to 10 days and go away by themselves. But “more serious illness may be indicated by blood in the stool or in the vomit, unremitting or high—meaning greater than 102-degree—fever, and severe weakness or dizziness on standing, that might indicate dehydration.” In that case, you should see a doctor right away. Infants, older adults, and people with compromised immune systems are at particular risk for severe dehydration.

Cancer
Fever is not uncommon in people who have cancer, according to the American Cancer Society, but it more often happens after cancer has spread from where it started. Almost all people with cancer will have fever at some time, especially if the cancer or its treatment affects the immune system, making it harder for the body to fight infection.
Although rare, fever may be an early sign of some cancers, including lymphoma, leukemia, and kidney and liver cancers. “They cause an inflammatory response in the body,” says Dr. Nunziato-Ghobashy. “If you can’t find a reason for your fever, it’s important to have somebody look to see professionally whether there is a reason.” (Here’s what you can do to prevent cancer.)
