Many people don’t bother to peek inside the bag after picking up a prescription, let alone look inside the bottle or box. But we all should, according to experts on medication-dispensing errors.
Medication mix-ups occur in about one in every 100 prescriptions, says Michael T. Rupp, PhD, FAPhA, a professor of pharmacy at Midwestern University in Glendale, Arizona, citing a 2017 report in BMJ Quality Improvement Reports.
Serious mistakes that could hurt patients are estimated to happen much less often, in about one in every 1,000 prescriptions, according to same report. While they’re rare, cases where a pharmacy employee accidentally swaps one drug for an incorrect pill that may resemble the prescribed one, or that may have a name that sounds similar, have had devastating consequences, including permanent disability and death. This type of medication mixup could also happen in other healthcare settings—not only at the pharmacy.
“When we consider that about 4 billion prescriptions are dispensed every year, even this apparently small incidence rate can have a very large public health impact,” says Rupp.
By law, pharmacists must assess whether a prescribed drug is appropriate for a patient and not likely to cause harm, a safeguard known as prospective drug utilization review. If the pharmacist does find a problem, he or she is required to check back with the prescriber to correct or resolve it. Pharmacists are also required to offer medication counseling to patients.
Most liability claims against pharmacists are due to the wrong drug or the wrong dose being dispensed, or a drug being dispensed to the wrong person, according to the Healthcare Providers Service Organization. Pharmacies take extra precautions and implement safety protocols when dispensing sound-alike and look-alike drugs, and failure to perform safety checks is a leading cause of medical errors. It’s not necessarily that pharmacists are failing to make these extra checks; other issues could lead to mistakes including the fact that some pharmacies have too-few staffers and pharmacists have other non-dispensing responsibilities.
Despite these efforts, mistakes are still made, which is why Dr. Rupp and other experts advise consumers to do their own prescription safety checks. Here are some examples of pills that look or sound alike.
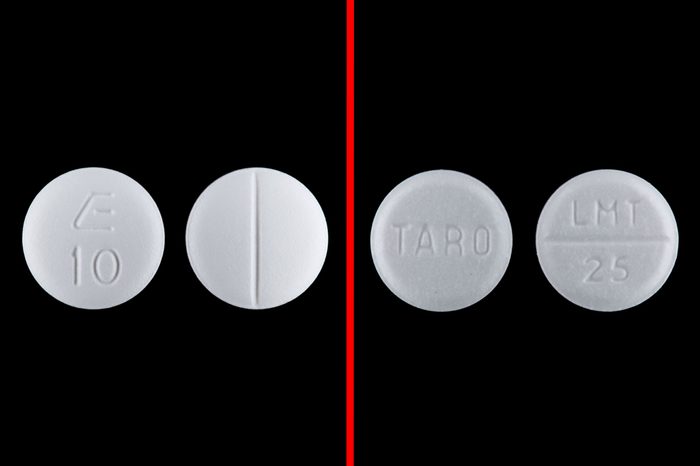
Labetalol/lamotrigine
More than a dozen cases of patients getting labetalol, a blood pressure-lowering medication, instead of the seizure and bipolar disorder drug lamotrigine (or vice versa), have been reported to the U.S. Food and Drug Administration and the Institute for Safe Medication Practices (ISMP), a non-profit watchdog.
Taking labetalol instead of lamotrigine can lead to breakthrough seizures, an abnormally slow heart rate, and decreased blood pressure while doing the opposite can lead to uncontrolled high blood pressure and rare, but life-threatening skin conditions known as Stevens-Johnson syndrome and toxic epidermal necrolysis, which can cause rash, peeling, and sores on mucous membranes.
Three of the cases reported to the FDA and the ISMP involved pregnant women who accidentally took lamotrigine instead of labetalol for high blood pressure. Untreated hypertension in pregnancy is particularly risky, because it can slow the growth of the fetus and can cause heart disease, kidney failure, seizures, and stroke in the pregnant woman.

Methylphenidate/methadone
Several cases of patients receiving methadone instead of methylphenidate have been reported to the ISMP and the FDA. Methylphenidate is a stimulant prescribed for treating attention deficit hyperactivity disorder (ADHD), while methadone is an opiate people use to wean from dependence on opioids, including prescription opioid medications and substances such as heroin. In addition to sharing the “meth” prefix, both drugs are dispensed in 10 milligram tablets, and are available from the same manufacturer. Because their names are so close, they may be stored next to each other or listed together on computer screens.
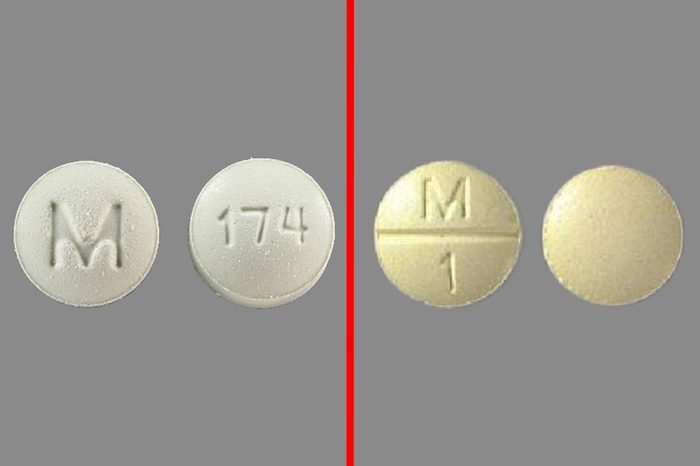
Metolazone/methotrexate
Methotrexate, a chemotherapy drug also used at lower doses to treat autoimmune conditions like rheumatoid arthritis, and metolazone, a diuretic that increases the amount of urine produced to get rid of excess water, can be mixed up because they look and sound alike. Both drug names start with “m-e-t” and have overlapping strengths of 2.5, 5, and 10 mg, according to the ISMP.
In a 2017 Missouri case reported in Pharmacy Times, transcribing errors made by a pharmacy technician led to a woman receiving methotrexate instead of metolazone. The patient took the accidentally dispensed drug once a day, as had been prescribed for the metolazone, and died less than a month later. The confusion between these two drugs can be life-threatening.
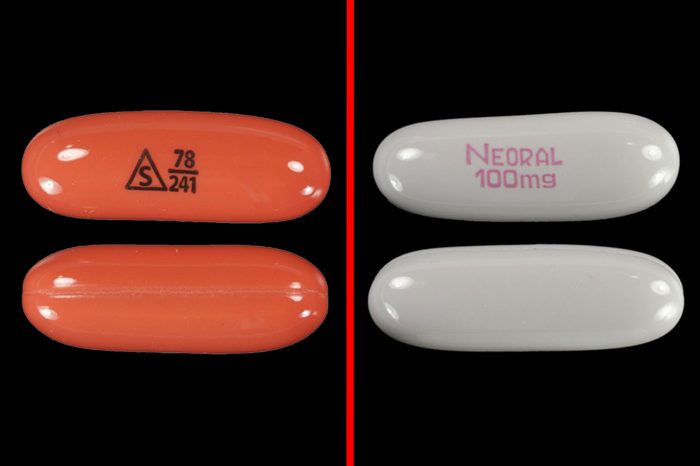
Sandimmune/Neoral
Sandimmune and Neoral are two different formulations of cyclosporine, and both are used for immune suppression after organ transplants. But less Sandimmune (non-modified cyclosporine) reaches the blood than Neoral (modified cyclosporine, also sold as Gengraf), so the body has a harder time absorbing the drug.
The ISMP first warned about the difference two decades ago, noting that the drug’s maker, Novartis, had found a quarter of cyclosporine prescriptions didn’t specify which form should be dispensed, and just 22 percent of the non-specific prescriptions were clarified. Taking the drug in the wrong form could lead to inadequate immunosuppression, and potentially loss of the donated organ.
In 2018, the ISMP still received reports of people who were prescribed Neoral or Gengraf but received Sandimmune.

Hydroxyzine/Hydralizine
These two drugs are commonly prescribed, and frequently mixed up, according to the ISMP, which has been warning about the potential for confusion for more than a decade.
Hydroxyzine (Vistaril, Atarax) is a medication for allergy symptoms like itching and rash, and may also be prescribed for anxiety and nausea. Hydralazine (Apresoline) is a blood pressure drug. In addition to sharing the first four letters of their generic names, the two medications are often stored side by side, and listed next to each other on computer screens, the ISMP notes.
In a recently reported case by the National Community Pharmacists Association, a young man went to the emergency room with an aching head, numb arms and legs, and difficulty breathing, which occurred after he started taking what he thought was hydroxyzine but turned out to be hydralazine. He was discharged with the right prescription.

Chlorpromazine/chlorpropamide
Chlorpromazine is used to treat schizophrenia and bipolar disorder, and chlorpropamide is used to treat type 2 diabetes. In a 2015 case report published in Mental Health Clinician, University of Oklahoma researchers noted that chlorpropamide instead of chlorpromazine was dispensed to a young man with schizophrenia, leading to worsening anxiety, confusion, and extreme sweating. After two weeks, he was switched to the right drug, and his anxiety improved.
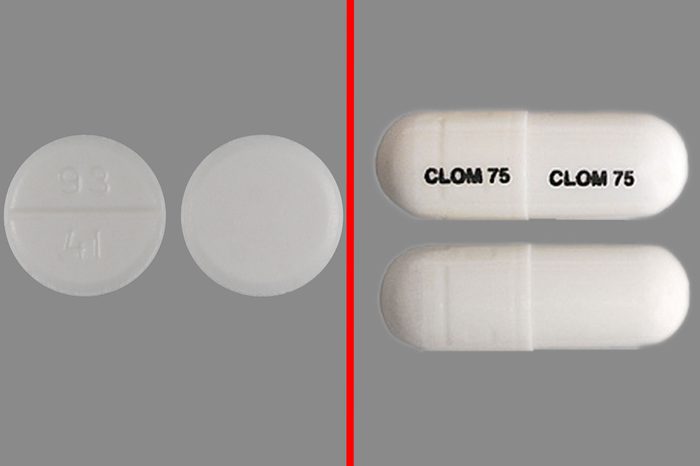
Clomiphene/Clomipramine
Clomiphene is a drug for treating infertility that stimulates the ovary to release eggs. Clomipramine is used to treat depression, obsessive compulsive disorder, and panic disorder. In a 2016 article in the Indian Journal of Psychiatry, a 35-year-old male with obsessive compulsive disorder received a prescription of clomipramine 100 mg/day in divided doses, and then 150 mg/day at 1-month follow-up, because he wasn’t improving. Following an examination of the pill strips, it was found the patient received a prescription of six tablets of clomiphene citrate (25 mg, each) daily, and not clomipramine, as advised. Fortunately, the patient did not have any adverse consequences.
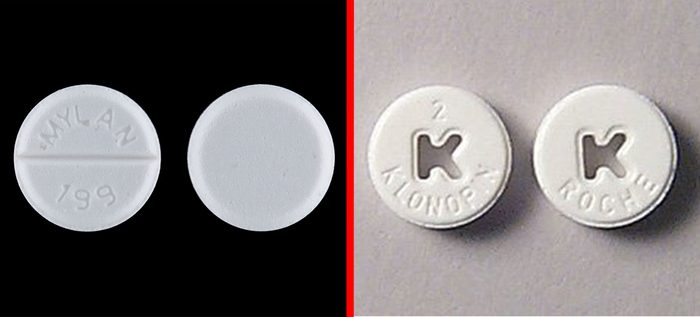
Clonidine/Klonopin
Clonidine (brand name Catapres), which is used to treat high blood pressure and ADHD, frequently gets mixed up with Klonopin (generic name clonazepam), a potentially addicting drug for treating seizures and panic disorder, according to the ISMP. Both drugs may also be prescribed for treating anxiety. (Here are 10 ways to safely use prescription drugs.)

Risperidone/Ropinirole
The FDA first warned the public about the risk of risperidone/ropinirole mixups in 2011, after the agency and the ISMP received more than 200 reports. Risperidone (Risperdal) is used to treat bipolar disorder and schizophrenia, and ropinirole (Requip) is for treating Parkinson’s disease and restless legs syndrome.
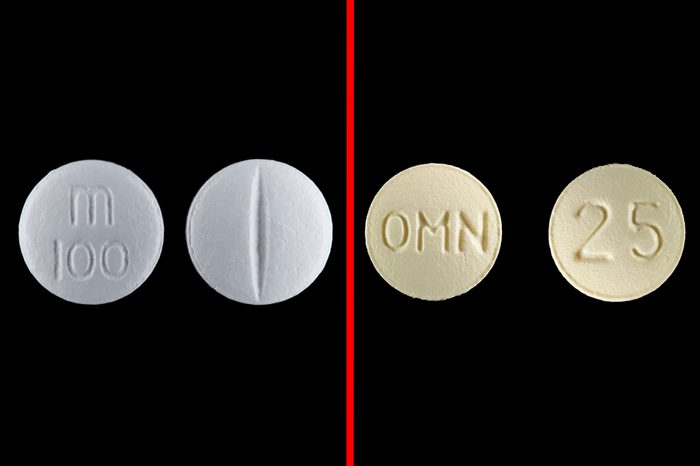
Toprol/Topamax
Toprol-XL (generic name metoprolol succinate) treats high blood pressure, chest pain, and heart failure. Topamax (topiramate) is used to treat and control seizures, and may also be prescribed for preventing migraine. Toprol-XL also gets confused with another seizure drug, Tegretol (carbamazepine). Patients mistakenly given Toprol-XL can develop an abnormally slow heart rate and a possible decrease in blood pressure, while those who stop the medication due to a mixup can see their blood pressure increase. The maker of Toprol-XL, AstraZeneca, along with the FDA, released a warning about the mixups in 2005.
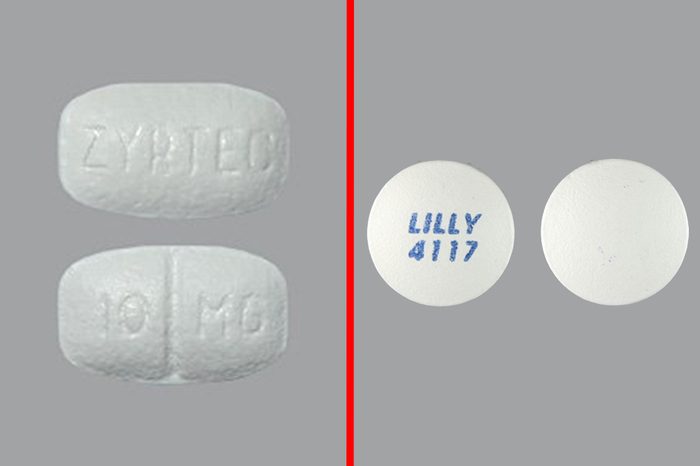
Zyrtec/Zyprexa
Zyrtec, an allergy medication, and Zyprexa which treats bipolar disorder, depression, and schizophrenia, could be confused with one another. The ISMP published its first alert on Zyrtec/Zyprexa mixups in 1996. The maker of Zyprexa, Eli Lilly and Co., issued a warning about the mixups in 2005, and changed its labeling in an attempt to reduce confusion. In 2009, the FDA issued its own warning to doctors and pharmacists about mixing up the drugs. One patient whose schizophrenia was kept under control by Zyprexa relapsed after she was mistakenly given Zyrtec. (Zyrtec has been available without a prescription since 2008.)
