5 Studies That Show Racism in Health Care is Real
Updated: Sep. 21, 2020
Is there racism in health care settings? There are extensive studies on the matter. Here's what the scientific data say.
Racism manifests itself in many ways, and one place it occurs is in health care settings. “Health is not created within the health sector,” says Camara Phyllis Jones, MD, an adjunct associate professor of community health and preventative medicine at Morehouse School of Medicine in Atlanta, “and the conditions of our lives are making some people and communities sicker than others in the first place.”
Blacks are 3.5 times more likely to die of Covid-19 than whites, according to a May 2020 analysis on MedRxiv, a preprinted server where scientific articles are posted prior to being peer-reviewed. Black mothers’ maternal mortality rate is four to five times that of white mothers, according to the Centers for Disease Control and Prevention (CDC). Even Black infants have more than twice the infant mortality rate of white infants. Black and Indigenous persons of color (BIPOC) are also diagnosed with asthma, diabetes, and obesity at disproportionately higher rates than whites. This is what one doctor is doing to save his black diabetic patients’ limbs.
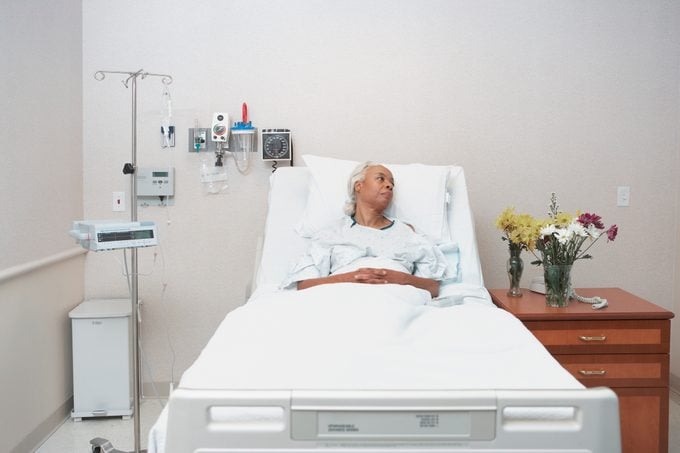
Racism in health care
Dr. Jones, who has spent her career studying the intersection of health and race, says longstanding socioeconomic factors underpin the health inequities of minorities like access to green space, healthy drinking water, and quality health care. Once Black people enter a health care setting, they have to contend with clinicians’ racial bias too. (Racism is an issue for Black medical professionals, too.) She points to the Institute of Medicine’s (IOM) landmark 2002 report, Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care, which analyzed 100 race-related health care studies and found that minorities, “are less likely than whites to receive needed services, including clinically necessary procedures.”
“This was not a study,” says Dr. Jones. “This was a wake-up call. Shame on us that we are still talking about the same thing 18 years later.” Since then, there has been no shortage of studies that paint a bleak picture when it comes to racism in health care.
Denying Black pain
Blacks have thicker skin, experience less pain, and have blood that clots more quickly than whites. Those are just a few of the fantastical falsehoods that about half of white medical students and first-year residents believed in a jaw-dropping 2016 study published in the Proceedings of the National Academies of Sciences. “About 50 percent reported that at least one of the false belief items was possibly, probably, or definitely true,” the report said.
“The most eye-opening [aspect of the study] was the extent to which people with medical training endorsed some of these false beliefs,” says lead researcher Kelly Hoffman, a behavioral scientist at the University of Virginia, department of psychology, in Charlottesville. The study found that the greater the false beliefs about Black bodies, the greater the racial bias in their pain treatment recommendations.
Hoffman says that her studies found white-bias was rooted in super-humanizing Blacks or the attribution of hardships of Black life as making people “tougher” in the face of pain. “What we need to do about it,” says Jones, “is have anti-racism training as the core part of the first-year curriculum in all medical schools. We can’t even let them get to the second year [without it.]” (Here are the things you can do to combat racism.)
Dismal Black maternal and infant mortality rates
In 2018, Wisconsin earned the grim distinction of having the highest national average of infant mortality rates for Black babies, before the age of one. Now, when it comes to the maternal mortality rate, Black mothers are more likely to die than their white counterparts from pregnancy-related causes, according to the CDC. Specifically, for every 100,000 live births, Black mothers have a 37.1 death rate, according to a January 2020 CDC National Vital Statistics Report. That’s nearly 40 percent higher than white women’s at 14.7.
Medical students subjected to racial bias
Medical school evaluations, or Medical Student Performance Evaluation (MSPE), are letters of recommendations that help students land their residency—a rite of passage for any doctor in training—which is why the language used to describe students in the evaluation is crucial. But a groundbreaking 2019 study published in the Journal of General Internal Medicine by researchers at the University of California, San Francisco, and Brown University, discovered that professors used different adjectives to describe underrepresented minority (URM) groups, like BIPOC.
Instead of describing core competencies, as they did with their white counterparts, professors often used words to describe personal attributes like “pleasant,” “open,” and “nice.” Even the study’s senior author Urmimala Sarkar, MD, a professor of medicine at UCSF in the division of general internal medicine, was shocked at her findings. “There shouldn’t be systematic differences based on gender or URM status in a sample this big.”

Few BIPOC in hospital C-suites
In 2015, the American Hospital Association launched the #123forEquity initiative, which asked signees at 1,500 out of 5,000 hospitals to increase diversity in leadership roles in the C-suites, which refers to the executive-level managers within a company, like a hospital. How did the AHA’s Institute for Diversity and Health Equity do with that? Unfortunately, not much has changed, according to its 2015 Benchmarking Survey, which looked at data from 2011 to 2015 on hospitals’ efforts to actively work on health care disparities and improve diversity in management.
The percentage of minority CEOs held at a paltry 9 percent, which is the same percentage as it was back in 2011, while the percentage of COO’s, CFO’s, and Chief Medical Officers and Chief Nursing Officers, all saw declines during the same period.
As serious as a heart attack
Black people who rush to a hospital’s emergency room with a chief complaint of chest pain, or, even worse, a heart attack in progress, may be met with skepticism. In a 2007 study, published in the Journal of General Internal Medicine, researchers studied the responses of 287 emergency medicine residents at four medical centers in Atlanta and Boston.
They discovered their racial bias towards Black patients negatively affected their proposed treatment of thrombolysis, or the treatment to dissolve blood clots, which improves blood flow through blood vessels. While “Physicians reported no explicit preference for white versus Black patients or differences in perceived cooperativeness,” the researcher’s racism-gauging Implicit Association Test showed that the bias against Blacks was measurable.
How can Blacks fight back against this bias? “They need to have an advocate with them all the time,” says Dr. Jones.
How to reduce racism in health care for BIPOC patients
With the Trump administration asking the Supreme Court to overturn the Affordable Care Act (ACA)—in the midst of the Covid-19 pandemic and historically high unemployment rates, no less—the death knell may soon sound for the 10-year-old health law, which would, in turn, wipe out health care for 23 million Americans. The move would devastate BIPOC, who, according to a 2019 report by Kaiser Family Foundation, “experienced improvements in the largest number of the examined measures related to coverage, access, and use.”
Still, despite the ACA, disparity remained between BIPOC and whites. Access to health care is a major hurdle for minorities, says Dr. Jones, who calls “limited differential access to the health care system through insurance, through lack of providers, through proximity, through language, [and] access,” the foundation of health disparities.
Dr. Jones says she’s not optimistic about the state of health care for BIPOC 20 years from now. “I fear that we will have a very fractured system where a lot of people are still falling through the cracks,” she says, adding that hospitals and health care workers need to take a long, hard look at their raw data and make a continuous effort to improve outcomes for black and brown patients.
“We must examine our hospital practices and even individual provider practices for differential treatment, prescribing practices, even differential assignment of patients into the teaching ward of a hospital. Ethnicity, language, zip code, immigration status, incarceration status. We need to routinely analyze those data, publicize those analyses, and then routinely discuss what it means. Over time, we need to have those data, so we can identify those problems and correct them.”



